 With peak allergy season around the corner, now is a good time to take a step back and reevaluate how we treat patients with ocular allergies. Epidemiological research shows an increase in the prevalence of all types of allergic reactions over the past three decades.1 Potential causes of this phenomenon include increased industrialization and pollution. Although the estimated number of patients varies, at least 20% of the general population suffers from allergic conjunctivitis at some point in the year.2
With peak allergy season around the corner, now is a good time to take a step back and reevaluate how we treat patients with ocular allergies. Epidemiological research shows an increase in the prevalence of all types of allergic reactions over the past three decades.1 Potential causes of this phenomenon include increased industrialization and pollution. Although the estimated number of patients varies, at least 20% of the general population suffers from allergic conjunctivitis at some point in the year.2
Early diagnosis and treatment of the signs and symptoms of allergic conjunctivitis can help patients more comfortably wear their lenses and help bring back dropouts. Whether your patient has previously worn contact lenses and discontinued wear due to allergies, is a first-time contact lenses wearer or is currently suffering allergy-related discomfort due to allergies, educating and treating patients is critical. It is important to start with the basics: Understand the chronic nature of their condition, learn how it affects their eyes, explain how they are not alone in this problem and discuss strategies to best treat their condition.
Ocular Allergy
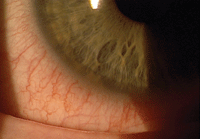
1. Conjunctival chemosis and injections associated with SAC.
While we typically see a spike in office visits for allergic conjunctivitis during the high pollen seasons, remember that many patients suffer from year-round allergies, such as mold and pet dander. Seasonal (SAC) and perennial (PAC) allergic conjunctivitis are the two most common forms of ocular allergy. Both are classified as type 1 or immediate hypersensitivity reaction: SAC typically involves an acute reaction to seasonal allergens, but may present as a chronic irritation in some patients, while PAC is typically a chronic condition caused by household allergens that are always present, but may present as an acute reaction in some situations. Seasonal pollens may exacerbate PAC.
Develop a Protocol
You can actively help relieve your patients’ symptoms by developing a comprehensive ocular allergy treatment protocol. In order to maximize new contact lens fits and prevent lens dropouts when treating patients with allergies, it is essential to collect a detailed history. Some questions to ask include:
• What is your occupational environment?
• When are your allergies the worst? Is it a seasonal issue?
• Are you on any systemic medications?
Our role is to assess symptom severity so we can provide the best treatment options. For example, would any systemic medications complicate the contact lens fitting process? Once we have determined the best treatment, it is our job to help our patients understand the plan we have recommended. This includes discussing how over-the-counter medications may help or hinder ocular relief. Keep in mind though that patients who are suffering from allergic conjunctivitis that is persistent enough to bring them into our office have likely already tried multiple OTC products and are now looking to us for quick, long-lasting and complete relief.
Remain Proactive

Tarsal plate seen with NaFl.
Take extra care with patients who may be asymptomatic at their visit. Start by learning more about the times when they do suffer from allergic conjunctivitis and then provide them the proper therapeutics, optimized contact lenses and a pre-scheduled visit plan before their symptoms start. This proactive approach will help minimize the negative impact of allergic conjunctivitis on successful contact lens wear.
Look for possible mild eyelid edema and conjunctival redness or chemosis during the physical exam (figure 1). Eversion of the upper eyelids may reveal the presence of papillae or other complicating factors; these can be seen more easily with the use of sodium fluourescein viewing in a cobalt blue light and wratten #12 filter (figure 2).
A Treatment Plan
Consider using a simple two-tiered approach when addressing lens wearers with ocular allergies: Treat it first, then fit it second.
1. Treat it. Create an effective treatment protocol for your patient. Here is a general list of allergy medications to include:
• Mast cell stabilizers. Mast cell stabilizers prevent the release of histamine and inhibit eosinophil migration into tissues, which cause allergy symptoms. Mast cell stabilizers must be taken prior to allergen exposure and typically do not provide immediate symptom relief. Common mast cell stabilizing medications include Alamast (pemirolast potassium, Vistakon), Crolom (cromolyn sodium 4%, Bausch + Lomb), Alomide (lodoxamide tromethamine, Alcon) and Alocril (nedocromil sodium 2.0%, Allergan).
• Combination mast-cell stabilizers/antihistamines. These combination agents offer the benefits of a dual mechanism of action in one drop. They provide relief from itching by their antihistaminic activity and protect against future allergen encounters by reducing mast-cell degranulation.
Medication in this category include: Optivar (azelastine hydrochloride 0.05%, Meda), Elestat (epinastine hydrochloride 0.05%, Allergan), Zaditor (ketotifen fumarate ophthalmic solution 0.025%, Novartis), Patanol (olopatadine hydrochloride 0.1%, Alcon) Alaway (ketotifen fumarate 0.025%, Bausch + Lomb).
Since Zaditor (Novartis) went over-the-counter in 2006, ketotifen fumarate—the active ingredient in Zaditor—is the most common compound in OTC allergy eyedrops.
Bepreve (bepotastine besilate 1.5%, Ista Pharmaceuticals) is a highly specific H1 histamine receptor antagonist and is dosed b.i.d. Pataday (olopatadine hydrochloride 0.2%, Alcon) has a higher concentration of olopatadine than Patanol and is approved for once a day dosing. The recently launched Lastacaft (alcaftadine ophthalmic solution 0.25%, Allergan) also offers a once-a-day dosing regimen.
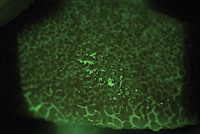
Tarsal plate seen with a Wratten filter.
• Topical steroids. A mild topical steroid may also be an option for patients who require topical treatment for their ocular allergy symptoms. Typically, steroids are used when a patient requires immediate relief. Alrex (loteprednol etabonate 0.2%, Bausch + Lomb) or Lotemax (loteprednol etabonate 0.5%, Bausch + Lomb) are commonly prescribed steroids for acute allergic conjunctivitis. These products are typically dosed four times a day, so it may be difficult to wear contact lenses until the steroid treatment is complete. If you choose to dose steroids twice a day, patients should wait 15 minutes after the drops to insert the lens.3
2. Fit It. One viable option for allergy sufferers is to switch to daily disposable contact lenses. Patients who use this modality typically have minimal issues with lens deposits and cleaning compliance. In fact, one study showed that patients with ocular allergies experienced a significant increase in comfort when fit with daily disposables.4
We are fortunate to have a wide range of daily disposable and toric options for our patients. But for some, the parameters required may be outside of the range available. Educate your patients about the importance of rubbing and rinsing their lenses. If this does not significantly improve symptoms, consider a hydrogen peroxide system with a rub and rinse step. You may also recommend a shorter replacement schedule; this may be more beneficial, albeit costly, to the patient.
A sound treatment protocol will help you more effectively treat patients who present with various allergy-related complaints. By proactively managing ocular allergies in your practice, you will not only provide your patients with relief and minimize contact lens dropouts, but also help grow the medical arm of your practice.
1. Asthma and Allergy Foundation of America. Available at:
www.aafa.org (accessed January 2012.)
2. Bielory L, Katelaris CH, Lightman S, et al. Treating the ocular component of allergic rhinoconjunctivitis and related eye disorders. Med Gen Med. 2007 Aug;9(3):35.
3. Miller J. Step up your ocular allergy care. Rev Optom. 2010 Apr;147(4):33-41.
4. Stiegemeier M, Thomas S. Seasonal allergy relief with daily disposable lenses. CL Spectrum. 2001 Apr;16(4):24-8.


