The tear film is a unique fluid in the body, with multiple functions that include protecting the cornea and ocular surfaces from infection, providing key nutrients and oxygen to the avascular cornea, carrying away debris and cellular waste and maintaining a clear fluid to wet and lubricate the ocular surfaces.1-4 We are just beginning to appreciate the magnitude of the role of the lipid layer and the tear film in providing a planar film of nanometer specifications for clarity of vision.
 The tears and lipid layer are dynamic, not uniform, and change in thickness with and between each blink. Eugene Wolff, M.D., the renowned English ophthalmologist and author of “The Anatomy of the Eye and Orbit,” was the first to propose a three-layered fluid comprising a lipid layer over an aqueous layer, with a mucin layer anchored to the corneal surface.5,6 It is this dynamic, metastable mixture of ingredients that makes the tear unique, reforming after each blink.
The tears and lipid layer are dynamic, not uniform, and change in thickness with and between each blink. Eugene Wolff, M.D., the renowned English ophthalmologist and author of “The Anatomy of the Eye and Orbit,” was the first to propose a three-layered fluid comprising a lipid layer over an aqueous layer, with a mucin layer anchored to the corneal surface.5,6 It is this dynamic, metastable mixture of ingredients that makes the tear unique, reforming after each blink.
We have since further developed our understanding of the tear film, evolving from the three-layer system of Dr. Wolff to a more complex understanding of as many as six layers, and a mix of additional ingredients.7
The Lipid Layer and Dry Eye
We went from an aqueous and mucin model of dry eye to understanding the critical impact of the lipid layer. As recently as 2007, the Dry Eye Workshop Report emphasized the causative mechanisms and roles of tear hyperosmolality and inflammation, minimizing the role of the meibomian glands and the lipid layer.8 Treatments revolved around the use of demulcents, emulsifiers and viscosity agents in over-the-counter products, with emollients comprised of lanolin, mineral oil, petrolatum and waxes used in ointments.9 Restasis (cyclosporine, Allergan) is the only prescription drug reported to increase the production of the aqueous portion of the tears.10 The obstruction of the meibomian gland ducts leads to disturbances in the production of lipids for the tear film’s lipid layer, a process first described and named meibomian gland dysfunction (MGD) in 1980 by Dr. Korb and Antonio Henriquez, M.D., Ph.D.11
In 2011, The International Workshop on Meibomian Gland Dysfunction reported that “it is believed that meibomian gland dysfunction may well be the leading cause of dry eye disease throughout the world.”12 A 2012 report further confirmed this paradigm shift by indicating that 86% of all dry eye disease patients demonstrated signs of MGD.13 It is therefore apparent that understanding the contribution of the lipid layer, as well as the function and dysfunction of the meibomian glands, is important in the diagnosis and treatment of dry eye.
It has been reported that the thinning or loss of the nanometer thick lipid coating at the surface of the tears leads to increased evaporation of the aqueous portion of the tears resulting in dry areas.14 Majd A. Isreb, M.D., and colleagues noted that lipid layer thicknesses (LLT) of 60nm or less correlated with fluorescein break-up time and Schirmer’s test scores indicative of dry eye; LLT of greater than 120nm have low to no likelihood of having dry eye.15
The Tear Structure
Given that the lipid layer has an important influence on the tear, understanding the structure of this portion of the tear structure is critical. This thin layer of lipid, usually 50nm to 100nm, is not a single homogeneous layer. It is believed that there is a layer of polar lipids overlying the aqueous layer of the tears, and a second layer of non-polar, hydrophobic lipids facing the air.16,17
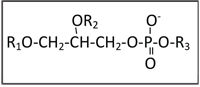
1. The general structure of phospholipids, where R1 and R2 are saturated or unsaturated fatty acids, and R3 is numerous polyols, aminoalcohols and complex O and N groups.
The precise composition of these tear film lipids continues to be debated. While the non-polar fraction is reported to contain cholesterol esters and mono, di- and tri-glycerides, the polar fractions forming the interface between hydrophobic and hydrophilic domains are more interesting. It is in this layer that phospholipids play an important role.
Igor Butovich, Ph.D., and Thomas James Millar, Ph.D., reported that the levels of phospholipids in the tears were dependent on the animal species—rabbits and koala bears, for example, and other animals with long inter-blink intervals show much higher levels of phospholipids.18
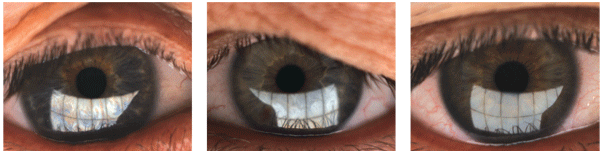
2. Good right overlay. 3. Average left overlay. 4. Bad right overlay.
What are Phospholipids?
Phospholipids are a class of molecules that are important in the body. Members of this class make up the important structures forming the bi-layer of the cell wall.19 These molecules help form the structure of the tears (figure 1).
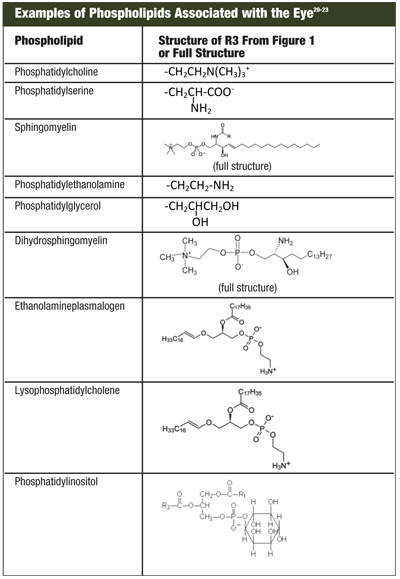
Research into identifying and understanding the role of phospholipids present in tears has seen mixed results. “Examples of Phospholipids Associated with the Eye” shows some of the phospholipids identified in tears. Phospholipids have basically two types: zwitterionic and anionic. All the compounds contain a negative charge on the oxygen attached to the phosphorous group. If the polar group at R3 contains a positive charge, such as phosphatidylcholine, then the overall net charge of the system is neutral. These are called zwitterionic phospholipids. Phospholipids that have polar groups at R3 that contain a polar group containing no charge such as phosphatidylglycerol, or have a net negative charge such as phosphatidylserine, are defined as anionic phospholipids.
We now understand that not all phospholipid structures are equally important in providing a thicker, more stable lipid layer in the tear.
Phospholipids and Tears
There are two phospholipids predominant in tears—phosphatidylcholine and phosphatidylethanolamine—which account for 60% of the phospholipid profile of the meibomian secretions.20 Oliver Shine, Ph.D., and James McCulley, M.D., reported that low levels of phosphatidylethanolamine and sphingomyelin were associated with evaporative dry eye rather than tear insufficiency.23 They determined that chronic blepharitis patients had significantly lower amounts of anionic phosphatidylethanolamine and sphingomyelin but not the zwitterionic neutral phospholipid phosphatidylcholine.23
 Dr. Korb and colleagues investigated the effect of the polar anionic phospholipid, dimyristeroylphosphatidylglycerol and the zwitterionic phosphatidylcholine alone and combined with white mineral oil.24 We found that an anionic formulation with white mineral oil increased the lipid layer thickness from 63nm to 115nm at 60 minutes.24 In comparison, an identical formulation, but with the zwitterionic phospholipid phosphatidylcholine substituted for the anionic dimyristeroylphosphatidylglycerol resulted in a marginal increase from 63nm to 67.5nm at 60 minutes.24
Dr. Korb and colleagues investigated the effect of the polar anionic phospholipid, dimyristeroylphosphatidylglycerol and the zwitterionic phosphatidylcholine alone and combined with white mineral oil.24 We found that an anionic formulation with white mineral oil increased the lipid layer thickness from 63nm to 115nm at 60 minutes.24 In comparison, an identical formulation, but with the zwitterionic phospholipid phosphatidylcholine substituted for the anionic dimyristeroylphosphatidylglycerol resulted in a marginal increase from 63nm to 67.5nm at 60 minutes.24
Using formulations with no added mineral oil provided much lower, but similar results. The zwitterionic phosphatidylcholine showed no increase in LLT at 60 minutes compared to baseline.
Phospholipids and Dry Eye
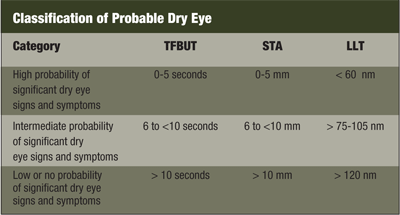
Dr. Isreb and colleagues found that LLT was correlated with measurement of tear film break-up time (TFBUT) and Schirmer test with anesthesia (STA).15 The results demonstrated the importance of the LLT (see “Classification of Probable Dry Eye”).
Only recently have emulsions been designed and marketed to target the lipid layer for the treatment of the signs and symptoms of dry eye. However, these approaches can only replace the lipids produced in the meibomian glands, not change the actual production of meibum. The Soothe (Bausch + Lomb) emulsion formula used non-phospholipid ingredients to rebuild the interface with the non-polar lipid facing the hydrophobic air and the hydrophilic aqueous portion of the tears. Results of these studies indicated that the lipid layer could be enhanced at one, five and 15 minutes from 59.6nm to 121.5nm.25
Soothe XP (Bausch + Lomb), a non-phospholipid emulsion, was compared to Systane Balance (Alcon), an anionic phospholipid emulsion, in a study by Dr. Korb and colleagues.26 Systane Balance increased LLT from baseline of 60nm to 90nm at two hours, a 50% improvement over baseline. Soothe, on the other hand, increased LLT from baseline of 60nm to 73nm at two hours, only 13nm above baseline. This difference was significant (p=0.0002), providing further support for the efficacy of anionic phospholipids in increasing LLT.
Confirming the improvement in LLT with the anionic phospholipid-based formulation, a clinical study by Gary Foulks, M.D., and colleagues reported that use of this anionic phospholipid-based formulation (Systane Balance) for one month compared to their habitual dry eye therapy showed significant improvement in TFBUT (p=0.032) and corneal staining reduction (p=<0.001).27 There were improvements in the patient’s ability to perform activities (p=0.006), a reduction of daily activity and work limitations (p=0.001, <0.001), as well as a reduction of symptom bother (<0.001), based on the Impact of Dry Eye Everyday Living (IDEEL) questionnaire.
Current evidence indicates that MGD and the resultant decrease in lipid secretions may be the primary cause of dry eye. It is now established that the lipid layer must be adequate to minimize evaporation and stabilize the tear film—to avoid dry eye or treat it when already present. Nature’s secret to the stability of the overall tear film appears to be the anionic phospholipids that provide a stable interface between non-polar lipids at the surface and the hydrophilic aqueous layer. These molecules work to enhance the lipid layer thickness resulting in reductions of key signs and symptoms of dry eye.
We now have ways to repair the lipid layer. An emulsion based on anionic phospholipids enhances the lipid layer thickness, resulting in improved overall tear stability. While not a cure for dry eye, these anionic phospholipid formulations can provide relief for many patients.
1. Craig JR. Structure and function of the preocular tear film. In: Korb DR, Craig J, Doughty M, et al. (Eds): The Tear Film: Structure Function and Clinical Examination. London: Butterworth-Heinemann;2002:18-50.
2. Lemp MA. Basic principles and classification of dry eye disorders. In: Lemp MA, Marquardt R (eds). The Dry Eye. New York: Springer-Verlag;1992:101-31.
3. Pfugfelder SC, Tseng SC, Sanabria O, et al. Evaluation of subjective assessments and objective diagnostic tests for diagnosing tear-film disorders known to cause ocular irritation. Cornea. 1998 Jan;17(1):38-56.
4. Stahl U, Wilcox M, Stapleton F. Osmolality and tear film dynamics. Clin Exp Optom. 2012 Jan;95(1):3-11.
5. Wolff E. The muco-cutaneous junction of the lid margin and distribution of the tear fluid. Trans Ophthalmol Soc UK. 1946;66:291-308.
6. Wolff E. The Anatomy of the Eye and Orbit, 4th ed. London: H.K. Lewis and Co.;1954:49.
7. Holly FJ. Formation and stability of the tear film. Int Ophthalmol Clin. 1973 Spring;13(1):73-96.
8. 2007 Report of the International Dry Eye Workshop. Ocul Surf. 2007;5(2):65-206.
9. Ophthalmic drug products for over-the-counter use; final monograph. Fed Regist. 1988; 53(43):7076-93.
10. Restasis [package insert]. Irvine, CA: Allergan, Inc; 2010 Feb.
11. Korb DR, Henriquez AS. Meibomian gland dysfunction and contact lens intolerance. J Am Optom Assoc. 1980 Mar;51(3):243-51.
12. Nichols KK, Foulks GN, Bron AJ, et al. The Report of the TFOS Workshop on Meibomian Gland Dysfunction. Invest Ophthalmol Vis Sci. 2011;52(4):1917-2085.
13. Lemp MA, Crews LA, Bron AJ, et al. Distribution of aqueous-deficient and evaporative dry eye in a clinic-based patient cohort: a retrospective study. Cornea. 2012 May;31(5);472-8.
14. Mishima S, Maurice DM. The oily layer of the tear film and evaporation from the corneal surface. Exp Eye Res. 1961 Sep;1:39-45.
15. Isreb MA, Greiner JV, Korb DR, et al. Correlation of lipid layer thickness measurements with Fluorescein tear film break-up time and Schirmer’s test. Eye. 2003 Jan;17(1):79-83.
16. Yamada M, Mochizuki H, Kawai M, et al. Decreased tear lipocalin concentration in patients with meibomium gland dysfunction. Br J Ophthalmol. 2005 Jul;89(7):803-5.
17. Millar TJ, Mudgil P, Butovich IA, Palaniappan CK. Adsorption of lipocalin to human meibomian lipid films. Invest Ophthalmol Vis Sci. 2009 Jan;50(1):140-51.
18. Butovich IA, Millar TJ. In search of a better animal model of human tear film: comparative lipiomic analysis of human and animal meibum. Invest Ophthalmol Vis Sci. 2009;50: e-abstract 2545.
19. Alberts B, Johnson A, Lewis J, et al. Molecular Biology of the Cell, 4th Edition. New York: Garland Science; 2002.
20. Greiner JV, Glonek T, Korb DR, et al. Phospholipids in gland secretion. Ophthalmic Res. 1996;28(1):44-9.
21. Dean AW, Glascow BJ. Mass spectrophoyometric identification of phospholipids in human tears and tear lipocalin. Invest Ophthalmol Vis Sci. 2012 Apr 2;53(4):1773-82.
22. Ham BM, Cole RB, Jacob JT. Identification and comparison of the polar phospholipids in normal and dry eye rabbit tears by MALDI-TOF mass spectrometry. Invest Ophthalmol Vis Sci. 2006;47(8):3330-8.
23. Shine W, McCulley JP. Keratoconjunctivitis sicca associated with meibomian secretion polar lipid abnormality. Arch Ophthalmol. 1998 Jul;116(7):849-52.
24. Korb DR, Greiner JV, Glonek T. The effects of anionic and zwitterionic phospholipids on the tear film lipid layer. Adv Exp Med Biol. 2002;506(Pt A):495-9.
25. Scaffidi RC, Korb DR. Comparison of two lipid emulsion eye drops in increasing tear film lipid layer. Eye Contact Lens. 2007 Jan;33(1):38-44.
26. Christensen MT, Blackie CA, Korb DR, et al. An evaluation of the performance of a novel lubricant eye drop. Invest Ophthalmol Vis Sci. 2010;51:e-abstract 4141.
27. Foulks G, Sindt C, Griffin J. Efficacy evaluation of a novel emulsion based, anionic phospholipid-containing artificial tear in meibomian gland dysfuntion subjects. Poster presented at the 6th Conference of the Tear Film and Ocular Surface Society, Florence, Italy; September 2010.
Dr. Korb has divided his time between the practice of optometry and research. His accomplishments include over 95 refereed publications, 35 U.S. patents, founding five research companies and naming MGD, GPC and lid wiper epitheliopathy.
Dr. Stone retired from Alcon Laboratories in 2006, after nearly 30 years in research and development of products for contact lens care and the treatment of dry eye and other ophthalmic products. He currently continues to consult in the area of ophthalmology.


