 Fitting patients with diagnostic hard or gas permeable lenses was almost a necessity when both of these modalities first became available on the market. Practitioners relied on diagnostic lens sets and would routinely fit the patient with several lens options in-office to determine the appropriate fit and power for each patient. The process was tedious—for those on both sides of the slit lamp.
Fitting patients with diagnostic hard or gas permeable lenses was almost a necessity when both of these modalities first became available on the market. Practitioners relied on diagnostic lens sets and would routinely fit the patient with several lens options in-office to determine the appropriate fit and power for each patient. The process was tedious—for those on both sides of the slit lamp.
It has been a great boon to GP lens practice that nowadays most labs can simply create a lens based on the patient’s keratometry values and refraction. Even more complex lenses, such as bitorics and GP multifocals, can be ordered empirically—eliminating the need for a diagnostic fit.1
 | |
|
Fig. 1. Diagnostic GP lens being cleaned with Optimum. Notice the foamy lather it creates.
|
Empirical fitting offers the potential to reduce the chair time of every patient. “Think of it as ordering a custom diagnostic lens for every patient,” says Doug Benoit, OD.1 While empirical fitting works very well in most cases, certain patient scenarios will still require diagnostic lens fitting.
This technique is particularly helpful in observing the lens-to-cornea relationship and lid interaction.2 These fits can be especially useful for patients who present with irregular corneal astigmatism due to keratoconus, pellucid marginal degeneration or corneal surgery (e.g., transplant, RK, LASIK).
And because lens/eye dynamics are also compromised by ocular surface disease, such patients can benefit from diagnostic lens fitting as well. Scleral lenses are almost always fit using a diagnostic lens kit, due to factors such as total corneal clearance, scleral contour and lens settling.
Maintenance
Diagnostic lenses can be stored either wet or dry. Wet diagnostic lenses have excellent wetting capabilities and are ready for immediate use—there’s no need to clean or condition them before use. Keep in mind, however, that when lenses are stored wet they must have their solution replaced every 30 days to ensure appropriate disinfection.3 Because this can be a time-consuming process, storing diagnostic lenses dry is the standard practice for most doctors.
 |
||
|
Fig. 2. The use of Biotrue during the contact lens conditioning step can aid in the wetting of a GP lens.
|
||
Such lenses need to be cleaned and conditioned before being applied to a patient’s eye. The lenses should be cleaned with an approved GP lens cleaner, such as Boston Simplus/Original/Advanced (Bausch + Lomb) or Optimum (Lobob). Cleaning the lenses thoroughly ensures a smooth surface free of debris, so spend at least 30 seconds cleaning the lens (Figure 1).
Once cleaned, it will need to be conditioned; this will ensure the lens wets well. GP conditioning agents such as Boston Conditioning solution and Boston Simplus work very well for this purpose. Additionally, an off-label use of Biotrue can aid in wetting. Biotrue contains hyaluronan, which binds to the lens surface and can help stubborn, non-wetting GP lenses (Figure 2). Adding Biotrue to the conditioning process may help GP lenses to wet more easily.
Following the trial fitting, the lenses must be cleaned and disinfected. The CDC suggests using ophthalmic grade hydrogen peroxide 3% to disinfect rigid lenses. According to the CDC, “Contact lenses used in trial fittings should be disinfected after each fitting by using a hydrogen peroxide contact lens disinfecting system for 10 minutes.”3-4
Once the lenses have been successfully disinfected, they should be stored dry. Be sure to take extra care to ensure all liquid is removed from the lens case, as well as the lens itself. If there is even one drop of liquid, the lens may bind to the case, potentially causing the lens to break as it is being removed from the case when reused at a later date.
Topical Anesthetics
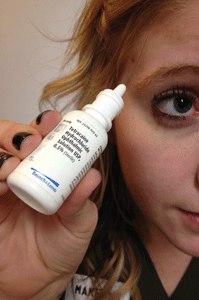
The use of a topical anesthetic may be helpful during a diagnostic GP fitting. If a patient has never worn GP lenses, instill one drop of anesthetic in each eye prior to applying the lens (Figure 3).5 This helps to increase patient comfort during the fitting process—especially if they will be trying multiple lenses. A topical anesthetic can also help to inhibit excessive tearing, which will make the evaluation of the fit significantly easier.
While most practitioners will agree that topical anesthetic is useful when fitting corneal lenses, how do they feel about using it when fitting scleral lenses? Sclerals are very comfortable and already feel much better than corneal GP lenses. So, is it really even necessary to use a topical anesthetic?
|
|
|
|
|
Fig. 3. The use of a topical anesthetic during diagnostic GP fitting can aid in patient comfort.
|
The debate on this topic is split; unfortunately, there is no clear-cut answer. Some practitioners will argue that a scleral lens is so comfortable that there is no need for any topical anesthetic. Others, by contrast, maintain that instilling a topical anesthetic is still useful for scleral lens fittings—especially in patients who have never worn any type of contact lens in the past, rigid or soft.
Personally, I agree with using anesthetic during a scleral lens fit. Many patients presenting with irregular corneas have never previously worn contact lenses, so they exhibit some apprehension about wearing any type of contact lens. Additionally, because scleral lenses are quite large when compared to a corneal GP lens, patients begin to feel even more nervous when they see the larger lenses.
In my experience, I have found that using topical anesthetic on all my GP diagnostic fittings has worked quite well. This technique allows me to quickly apply and remove several different lenses until I find the appropriate fit, while the patient remains very comfortable during this process.
While the trend favoring empirical fitting continues to expand every day, diagnostic lens fitting is still important in any practice—especially in patients with irregular corneas. Exercising proper care for the diagnostic lenses and using a topical anesthetic during the fitting process can help you become successful with all of your diagnostic fits!
|
Hyper-Dk Lens Care
|
|
For lens materials with Dk
values over 100, such as Boston XO (Bausch + Lomb), Boston XO2 (Bausch +
Lomb) and Menicon Z (Menicon), Boston Advanced may be too abrasive for
the lens surface. This can cause the material, which is softer and more
pliable, to break down faster and scratch more easily. If your patient
wears a lens made of a hyper-Dk material, consider recommending other GP
care products such as Boston Simplus or Optimum by Lobob.
|
1. Benoit, D. Empirical fitting of gp multifocals. Contact Lens Spectrum. Oct 2009.
2. Lam, D, et al. A toric gp primer. Contact Lens Spectrum. Dec 2013.
3. Ward, M. Maintaining and Disinfecting GP Diagnostic Lenses. Contact Lens Spectrum. Sep 2006.
4. http://www.cdc.gov/mmwr/preview/mmwrhtml/00000602.htm
5. Bennett ES, et al. The effect of topical anesthetic use on initial patient satisfaction and overall success with RGP contact lenses. Optom Vis Sci 1998;75(11):800-5.


