 How important are contact lens wearers to your practice? In the changing face of health care, contact lenses are vitally important to most optometry practices. Advanced contact lens materials, designs and solution systems have improved our ability to provide a comfortable contact lens wearing experience, but a careful corneal evaluation can identify potential complications along with specific treatment regimens for contact lens candidates. A detailed corneal assessment—before, during and after the initiation of contact lens wear—is essential to preventing contact lens dropouts.
How important are contact lens wearers to your practice? In the changing face of health care, contact lenses are vitally important to most optometry practices. Advanced contact lens materials, designs and solution systems have improved our ability to provide a comfortable contact lens wearing experience, but a careful corneal evaluation can identify potential complications along with specific treatment regimens for contact lens candidates. A detailed corneal assessment—before, during and after the initiation of contact lens wear—is essential to preventing contact lens dropouts.
Contact lens discomfort is often used as a broad term, but in this month’s column, we will evaluate underlying ocular surface disease as a potential cause of lens intolerance. In particular, dry eyes and lid margin disease—blepharitis and meibomian gland disease (MGD)—are both important conditions to identify for eye care practitioners who are interested in maximizing patient comfort with contact lens wear. Both conditions have the ability to slowly erode a contact lens practice. Further complicating matters, contact lens wear will interfere with the normal tear film and can cause problems for those with underlying disease states.1 Therefore, a patient’s underlying conditions need to be identified in advance and addressed aggressively.
Keep in mind that there are almost as many contact lens wearers dropping out as there are new contact lens wearers being added on an annual basis.2 Remediation of these underlying conditions will give patients a greater likelihood of comfortably wearing their contact lenses.
While achieving contact lens comfort is a challenge, adopting a patient-centered proactive approach is good for both your patients and your practice.
Silent Dropouts
Don’t assume that your patients are wearing their contact lenses comfortably; they may have silently dropped out of contact lenses wear without your knowledge. It may be surprising to learn that some of the more subtle conditions can pose the biggest potential threat to continuous contact lens wear. For example, MGD can exist in a not-so-obvious form.3 In order to identify these patients, gland expression is critical. It may take 10 to 15 seconds of sustained pressure in a specific area, but when a thickened meibum or lack of fluid appears, you can tell that these glands are not functioning properly and the condition needs to be addressed.4
Patients rarely call to inform us of their contact lens discomfort or when they are about to drop out of contact lens wear. As practitioners, it is our job to actively identify these patients through detailed history and routine examinations. Subtle changes in the way you question patients about their contact lens wear can provide valuable insight into comfort concerns. For example, ask your patient what time their contact lenses start to feel uncomfortable. Then, follow up with potential reasons why their lenses may be drying out early in the day and provide suggestions on how they can improve comfort.
Dry Eye Disease
When we talk about dry eye and contact lens wear, many factors can contribute to the comfort concerns. According to the National Eye Institute’s Visual Function Questionnaire: Impact of Dry Eye on Everyday Life (IDEEL), approximately 34% of contact lens wearers discontinue use at least once, most frequently because of dry eye symptoms.5 That is one third of our contact lens population!
In 2007, the International Dry Eye Workshop Study (DEWS) defined dry eye as “a multifactorial disease of the tears and ocular surface that results in symptoms of discomfort, visual disturbance and tear film instability… It is accompanied by increased osmolarity of the tear film and inflammation of the ocular surface.”6
Whether aqueous deficiency or evaporative, dry eye leads to tear hyperosmolarity. With the introduction of new tools like the TearLab Osmolarity System, a non-invasive diagnostic test that provides a tear osmolarity measurement, practitioners can quickly assess whether dry eye exists and to what severity.7 This may prove to be an ideal indicator of dry eye disease; because tear osmolarity is consistently higher with dry eye, this too may be another tool to quantify and diagnose the condition.8
The initial treatment of dry eye depends on the severity of the diagnosed condition and may include modifying a patient’s environment (computers, ceiling fan, reduced caffeine intake, smoking cessation and identification of possible contributing medications such as antihistamines, antidepressants, antihypertensives, antidiuretics and anticholinergics); increasing fluids; prescribing certain nutrients such as omega-3 and omega-6 fatty acids; and using artifi cial tears.9 The next level of management often includes punctal plugs and topical ocular medications, such as Restasis (cyclosporine 0.05%, Allergan) and oral prescriptive products.
Eyelid Margin Disease
Common symptoms of blepharitis include burning, itching, excessive tearing, granular sensation, and scratchiness or foreign-body sensation due to crusted debris or dryness. Decreased vision or changes in visual clarity may occur due to poor tear film, eyelids stuck together and/or eyes being red or crusty upon waking.
Early identification and treatment of blepharitis begins with a careful slit lamp evaluation, followed by warm compresses and eyelid hygiene. Commercially available prepackaged lid scrubs work well for patients who prefer the convenience of such a system. Occasionally, an antibiotic ointment or an antibiotic/steroid combination ointment may help alleviate the acute eyelid disease state.
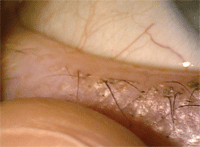 |
| It may take 10 to 15 seconds of sustained pressure in a specific area in order to express the meibum from the meibomian glands.
|
MGD can pose a major obstacle in producing a healthy tear film. The oil produced is less than ideal to coat the anterior surface of the tear layer. Treatment initially involves warm compresses, but when insufficient, topical and oral agents may be prescribed.
Comparing the Cases
Consider these two patients. One presents with lid rim redness, intermittent blur during contact lens wear, some flakes (crusties) and watery eyes. These are all new symptoms and an examination reveals anterior blepharitis, no mites, but a very low tear meniscus.
The second patient presents with chronic dry eye. She is unable to wear her contact lenses for extended periods of time and uses artificial tears throughout the day. She would love to wear contact lenses again; she has tried punctal occlusion and nighttime gel with no success. This patient has also been experiencing foreign body sensation for the past several months. An examination reveals very low tear film break-up time, meibomian gland dysfunction and scalloped lid margins with collarettes.
The management of these patients will differ by the severity of their treatment plans. The first patient with blepharitis may need to be treated with an antibiotic such as Azasite (azithromycin, Merck), while the second patient will need a more aggressive course of action with an antibiotic/steroid combination treatment such as Tobradex ST (tobramycin/dexamethasone, Alcon) or Zylet (loteprednol/tobramycin, Bausch + Lomb). Both patients need to have their underlying conditions resolved before they can resume successful contact lens wear.
Ocular surface disease requires a multifactorial approach when dealing with contact lens wearers. Contact lens wear can complicate these conditions. Initial treatments are aimed at controlling the underlying disease state, then attempting to return to successful contact lens wear.
1. Lonsberry BB. Dry eye in the office. Rev Optom. 2008 Feb:145(2):52-7.
2. Young G, Veys J, Pritchard N, Coleman S. A multi-centre study of lapsed contact lens wearers. Ophthalmic Physiol Opt. 2002
Nov;22(6):516-27.
Additional references available at www.reviewofcontactlenses.com.


