 From 2005 to 2006, Fusarium keratitis gained notoriety when a fungal infection outbreak was associated with a certain contact lens solution. Though the incidence of fungal keratitis has since decreased, certain studies suggest that infection rates may once again spike due to an increase in the contact lens-wearing population and the rising trend of using multipurpose solutions, which have been shown to be less effective than peroxide systems.1
From 2005 to 2006, Fusarium keratitis gained notoriety when a fungal infection outbreak was associated with a certain contact lens solution. Though the incidence of fungal keratitis has since decreased, certain studies suggest that infection rates may once again spike due to an increase in the contact lens-wearing population and the rising trend of using multipurpose solutions, which have been shown to be less effective than peroxide systems.1
The truth is that Fusarium cases continue to persist and, without proper knowledge of the disease and its signs and symptoms, an outbreak could very well occur again. If nothing else, the outbreak of fungal keratitis taught us that early detection and patient compliance are key aspects of prevention. It is vitally important that we learn from history rather than make the same mistakes. Today, years after the epidemic, we seek to re-emphasize the notions that enforcing contact lens compliance and awareness of the signs and symptoms of all diseases— even the most rare—is crucial in maintaining a patient’s health.
In this column, we will focus on what you, as the eye care practitioner, can do to prevent your contact-lens wearing patients from exposing themselves to fungal infections.
Who Does Fungal Keratitis Affect?
For contact lens users, fungal keratitis is a rare, but real concern. An estimated 30 million people in the United States wear soft contact lenses; cases of contact lens-related fungal keratitis has been estimated to range from approximately four in 10,000 for daily wear to 20 in 10,000 for extended wear.2 Fungal keratitis is a condition more prevalent in warm climates—in the U.S., up to 35% of microbial keratitis cases are fungal keratitis in the Southern states, compared to only 1% in New York.3,4
Fusarium has been deemed among the most common of filamentus fungi in the United States.5 However, yeast and filamentous fungi are the two groups mainly responsible for infection. Candida is the most common pathogen in the yeast group and usually affects corneas compromised by topical steroids or ocular surface dysfunction.
Fungal keratitis can occur when patients come into contact with plant matter—particularly in cases when the patient’s immune system has been compromised or is battling chronic ocular surface issues. Patients at greatest risk for fungal keratitis are those who live in warm, humid environments and who do not maintain proper contact lens care.
Identifying the Culprit
The key to diagnosis is to proceed quickly, and to maintain a high level of suspicion. The longer it takes to reach an accurate conclusion, the greater the possibility for the disease to become rampant. An eye care practitioner should be acutely aware of what fungal keratitis looks like, so as to act fast and appropriately when combatting the aggressive infection.
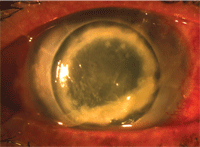 |
| A fungal keratitus case in the setting of a corneal transplant. Notice the purulent infiltrate along the margins of the cornea, as well as marked conjunctival hyperemia.
|
We do want to stress that fungal keratitis may resemble advanced bacterial keratitis, and there is also the distinct possibility of co-infection/poly-microbial events that include bacterial infection.
The Importance of Compliance
Preventing fungal keratitis takes dedication and cannot be done effectively without proper contact lens care, which may not always be an easy task. Patients must constantly be reminded that noncompliance puts them at risk for potentially devastating ocular infection.
There are ways to minimize safety concerns. The American Optometric Association outlines the following steps:6
1. Always wash your hands before handling contact lenses.
2. Carefully and regularly clean contact lenses, following the directions outlined by your eye care practitioner. If recommended, rub the contact lens with fingers and rinse thoroughly before soaking lenses overnight; the multipurpose solution should completely cover the lens.
3. Store lenses in a proper lens storage case and replace the case every three months. Clean the case after each use, and keep it open and dry between cleanings.
4. Use only products recommended by your eye care practitioner to clean and disinfect your lenses. Saline solution and rewetting drops are not designed to disinfect lenses.
5. Only fresh solution should be used to clean and store contact lenses. Never re-use old solution. Contact lens solution must be changed according to the manufacturer’s recommendations, even if the lenses are not used daily.
Most importantly, discuss prevention with patients and stress good ocular hygiene, proper safety precautions and general awareness, particularly when outdoors. The odds of contracting fungal keratitis, or any other type of keratitis, are greatly increased when the contact lens user is not compliant; lens hygiene remains the most valuable tool to prevent cases of keratitis.
In addition to stressing compliance and hygiene, as well as being acutely aware of what fungal keratitis looks like upon onset, eye care practitioners should be aware of their patient’s lifestyle. Fungus is found in soil and vegetable matter, so stress caution and general awareness for patients who may work outdoors, especially in warmer climates. By discussing work and hobbies, such as gardening, you can better determine risk and plan accordingly.
Keeping the lines of communication open between you and your patient is a vital step in assessing the situation appropriately. In our next column, we will discuss what happens if a patient does contract this dangerous infection.
1. Tuli SS, Iyer SA, Driebe WT, Jr. Fungal keratitis and contact lenses: an old enemy unrecognized or a new nemesis on the block? Eye Contact Lens. 2007 Nov;33(6 Pt 2):415-7; discussion 424-5.
2. Schein OD, Glynn RJ, Poggio EC, et al. The relative risk of ulcerative keratitis among users of daily-wear and extended-wear soft contact lenses. A case-control study. Microbial Keratitis Study Group. N Engl J Med. 1989 Sep;321(12):773-8.
3. Liesegang TJ, Forster RK. Spectrum of microbial keratitis in South Florida. Am J Ophthalmol. 1980 Jul;90(1):38-47.
4. Asbell P, Stenson S. Ulcerative keratitis. Survey of 30 years’ laboratory experience. Arch Ophthalmol. 1982 Jan;100(1):77-80.
5. Embong Z, Wan Hitam WH, Yean CY, et al. Specific detection of fungal pathogens by 18S rRNA gene PCR in microbial keratitis. BMC Ophthalmol. 2008 Apr;8:7.
6. Clinical Guidance Regarding Fungal Keratitis Associated with Contact Lens Wear. American Optometric Association.
Available at: www.aoa.org/x5185.xml (accessed August 2011)


