 |  |
The advent of soft disposable contact lenses permanently altered the contact lens landscape, resulting in the steady decline of corneal gas permeable (GP) lens fitting. At one point, it was even opined that GP lenses would be rendered obsolete.1 Although this prediction has not come to fruition entirely, GP lenses are increasingly relegated to patients with complex prescriptions or high vision demands. Additionally, specialty designs such as custom soft toric, hybrid and scleral lenses are now widely available and steadily growing in popularity. Consequently, corneal GP lenses are often overlooked as a first choice for our patients.
Research shows GP lenses can provide superior vision quality compared with soft lenses.2 Their smooth refracting surface in combination with the post-lens tear layer delivers crisp, stable optics, especially for patients with corneal astigmatism. Despite this advantage, practitioners are still hesitant to fit GP lenses. Let’s address a few reservations practitioners may have.
Increased Chair Time
In a survey of contact lens fitters in the United Kingdom, GP lens fitting was perceived to require more technical skill and chair time than soft lenses.3 When a diagnostic fitting set is used, multiple diagnostic lenses may be assessed to find the appropriate lens-to-cornea relationship. An over-refraction is then required to determine the final power of the contact lens to be ordered. While this fitting method may involve more chair time on the initial visit, fewer modifications should be required after ordering the initial contact lens. To choose an initial diagnostic lens, fitting calculators are available from resources such as the Gas Permeable Lens Institute, EyeDock and the GP laboratories themselves.
An alternative method to fitting GP lenses that can potentially save chair time is empirically ordering an initial lens. Laboratories can design lenses using only keratometry readings and a subjective refraction, although additional measurements such as corneal topography, horizontal visible iris diameter and pupil size can improve the precision of the initial lens design. The power of empirically ordered GP lenses is typically accurate, allowing for great initial vision to provide the “wow effect” that is especially critical for new wearers. To fine-tune the lens fit, usually only small adjustments are required. This approach also reduces the hassle of verifying, disinfecting and maintaining diagnostic lens sets.
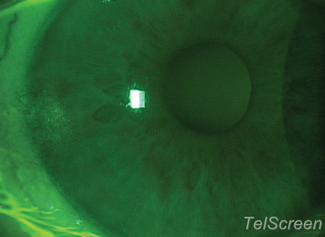 |
| Here is a look at three and nine o’clock corneal staining with mild pannus. Photo: Gaddie Vision Center |
Comfort
Discomfort is the leading cause of contact lens discontinuation across all modalities.4,5 Therefore, it should come as no surprise that practitioners may be apprehensive about the initial comfort level of a GP lens. The smaller diameter allows for greater movement on the eye and interaction of the lens edge with the eyelids, creating the sensation of lens awareness. Although the majority of contact lens wearers prefer the initial comfort of a soft contact lens, it does not mean they cannot be successful with GP lenses.6
The first step towards achieving optimal comfort begins before the lens is placed on the eye. Proper education about the adaptation process is paramount to the success of a new GP wearer. One study of neophyte GP wearers suggests the first 10 to 15 days are a good predictor of successful adaptation.7 Patients must understand that lens awareness will dissipate over time. A helpful analogy is to compare a GP lens to a new dress shoe and a soft contact lens to a slipper. New dress shoes must be broken in before they are comfortable, while slippers start out comfortable, but gradually break down over time. It is also helpful to be confident when presenting GP lenses. A positive attitude may be just enough for the patient to persist through the first few days of lens awareness.
With GP lenses, centration and lid interaction are important factors that contribute to the initial comfort. Fortunately, advances in automation have allowed modern GP lenses to be manufactured thinner with improved back surface geometry and more consistent edges.8 When the upper lid is at or below the superior limbus, a lid-attached fit using a slightly larger lens (9.2mm to 9.8mm) is recommended. If the upper lid is positioned higher, an inter-palpebral fit with a smaller diameter (<9.0mm) lens is preferred.
Lastly, for the neophyte GP wearer, research shows using a topical anesthetic at the initial dispensing appointment improves initial comfort and perception of adaptation. This also helps the practitioner evaluate the lens on eye without excessive tearing or blinking. Initial use of topical anesthetic can also improve the rate of satisfaction over the course of one month, reducing the risk of dropout.9
Adverse Events
Like any contact lens, there are risks associated with GP lens wear; however, complications are typically mechanical in nature.10 One of the most common complications induced by GP lens wear is corneal dessication. The vertical movement of the lens during the blinking motion can disrupt the adjacent tear film, causing dehydration of the peripheral cornea. This leads to punctate staining of the cornea both nasally and temporally, referred to as three and nine o’clock staining. In severe cases of dessication, dellen formation or vascularized limbal keratitis can occur. It has been been reported that up to 90% of GP wearers will present with signs of dessication, although improvements in lens design, such as peripheral curve and diameter changes, may reduce this to closer to 30%.11,12 When symptomatic, patients report dryness and redness, which can be typically managed with topical lubrication.
It can be easy to forget that GP lenses have an excellent safety profile with a lower rate of microbial keratitis (MK) and corneal inflammatory events (CIEs) than soft contact lenses.10,13-14 Most modern GP lenses are made with fluoro-silicone/acrylate polymers, which are highly permeable to oxygen, provide good surface wettability and lack any significant water content. These lens properties make it difficult for microorganisms to adhere to the lens. In addition to functioning as a flushing mechanism, the ability of GP lenses to facilitate tear exchange underneath the lens surface also provides a biochemical protection against microbes.15 Reducing the bacterial load helps to lower the risk of both CIEs and MK. CIEs are also caused by hypoxia; however, GP lenses are less commonly worn for extended periods than soft contact lenses.
Tear exchange also improves oxygen tension reaching the corneal surface.16 This may be part of the reason CIEs occur less frequently with GP wearers.
GP lenses have several benefits, including superior optics and an excellent safety profile. Although initial comfort may be a factor, if a patient is motivated to adapt to the lens they can be quite successful. Don’t hesitate to discuss GP lenses with your patients, including contact lens neophytes.
1. Efron N. Obituary--rigid contact lenses. Cont Lens Anterior Eye. 2010;33:245-52.
2. Michaud L, Barriault C, Dionne A, Karwatsky P. Empirical fitting of soft or rigid gas-permeable contact lenses for the correction of moderate to severe refractive astigmatism: a comparative study. Optometry. 2009;80:375-83.
3. Gill FR, Murphy PJ, Purslow C. A survey of UK practitioner attitudes to the fitting of rigid gas permeable lenses. Ophthal Physiol Opt. 2010;30:731-9.
4. Pritchard N, Fonn D, Brazeau D. Discontinuation of contact lens wear: a survey. Int Contact Lens Clin. 1999;26(6):157-62.
5. Richdale K, Sinnott LT, Skadahl E, Nichols JJ. Frequency of and factors associated with contact lens dissatisfaction and discontinuation. Cornea. 2007;26(2):168-74.
6. Fonn D, Gauthier CA, Pritchard N. Patient preferences and comparative ocular responses to rigid and soft contact lenses. Optom Vis Sci. 1995;72(12):857-63
7. Carracedo G, Martin-Gil A, Peixoto de Matos SC, et al. Symptoms and signs in rigid gas permeable lens wearers during adaptation period. Eye & Contact Lens: Science & Clinical Practice. 2016;42(2):108-14.
8. Bennett ES, Sorbara L, Kojima R. Gas-permeable lens design, fitting and evaluation. In: Bennett ES, Henry VA, eds. Clinical Manual of Contact Lenses. 4th Ed. Philadelphia, PA: Lippincott, Williams & Wilkins; 2014:112-56.
9. Bennett ES, Smythe J, Henry VA, et al. The effect of topical anesthetic use on initial patient satisfaction and overall success with rigid gas permeable contact lenses. Optom Vis Sci. 1998;75:800-5.
10. Morgan PB, Efron N, Maldonado-Codina C, Efron S. Adverse events and discontinuation with rigid and soft hyper DK contact lenses used for continuous wear. Optom Vis Sci. 2005;82:528-35.
11. Edrington TB, Barr JT. Peripheral corneal dessication. CL Spectrum. 2002;17:46.
12. Azhar J, Bennett ES, Castellano CF. Corneal dessication in today’s GP lens wearers: results. CL Spectrum. 2015;30:17.
13. Stapleton F, Keay L, Edwards K, et al. The incidence of contact lens-related microbial keratitis in Australia. Ophthalmology. 2008;115(10):1655-62.
14. Stapleton F, Keay L, Jalbert I, Cole N. The epidemiology of contact lens related infiltrates. Optom Vis Sci. 2007;84(4):257-72.
15. Fleiszig SM. The pathogenesis of contact lens-related keratitis. Optom Vis Sci. 2006;83:E866-73.
16. Weissman BA. Corneal oxygen: 2015. CL Spectrum. 2015;30:25-29, 55.


