Ne urotrophic keratitis can be one of the more difficult corneal conditions to manage. It is a rare degenerative disease caused by an impairment of trigeminal corneal innervation, which then leads to corneal anesthesia.
urotrophic keratitis can be one of the more difficult corneal conditions to manage. It is a rare degenerative disease caused by an impairment of trigeminal corneal innervation, which then leads to corneal anesthesia.
The most common causes of neurotrophic keratitis are viral infection by either the herpes simplex or herpes zoster viruses, followed by chemical burns, physical injury and, ultimately, surgical complication.1
These cases can be difficult to manage, despite our best efforts. Many times corneal defects develop and worsen despite careful monitoring and therapeutic intervention. On the other side, watching corneas develop scarring, large and deep defects that can lead to deteriorating vision and perforation in some cases can be unattractive. In this month’s column, I will suggest an aesthetically pleasing way to manage individuals with this condition.
A Case Study
A 52-year-old white male was referred to my office for a corneal evaluation. His history was significant for the development of herpes zoster of the right branch of V1 four months prior to his visit. Lesions erupted and subsequently became infected with Staph. At the time of his presentation, he still had many open lesions on the right side of his scalp.
Approximately one month prior to his visit, he noticed issues with his right eye. He developed blurry vision, a burning sensation in the right orbit and mild photophobia. He was initially treated with artificial tears; an antibiotic drop was later added. Despite the therapy, his vision continued to deteriorate.
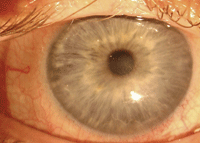
Scleral lens on neurotrophic eye (left).
His presenting acuity in the right eye was 20/100 with correction. A slit lamp examination revealed a small epithelial defect, as well as anterior stromal haze and mild tissue loss. At this point, I added prednisolone acetate 1% QID.
One week later, his eye had improved and his vision was up to 20/50 OD. He continued on this therapy and was stable for three weeks.
At a follow-up one month after his initial presentation, he reported that his eye was increasingly uncomfortable and his vision was once again deteriorating. His best-corrected acuity was 20/100 OD. He was still using the prednisolone acetate 1% QID, in addition to artificial tears and an antibiotic drop. Slit lamp examination at this visit revealed a 4mm x 1.5mm central epithelial defect just below the visual axis. Erythromycin ointment was added QID and he was scheduled to return in one week.
At the next follow-up, he reported improvement again. Vision returned to 20/60 OD and the epithelial defect measured 50% smaller than the previous visit.
The same regimen was continued; in one week, the defect was larger but the patient did not have any worsening symptoms. I decided to place a bandage soft lens on the right eye and discontinue the erythromycin ointment.
Unfortunately, he had difficulty keeping the lens in place. Over a four-week period, we tried several lenses, including an 18mm soft lens, but all the lenses had dislodged within three days of placement. Autologous serum drops were added Q2H OD.
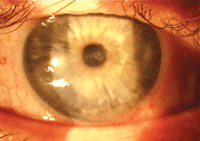
Neurotrophic eye with scleral lens removed (right). Note irregular surface but no epithelial defect.
At the next follow-up (now two months after the original visit), the patient said he did not feel that the lenses were helping, and that his vision was getting worse. He was using autologous serum drops Q2H OD., as well as prednisolone acetate 1% TID OD and ofloxacin drops TID OD. His visual acuity was now 20/300 OD. Slit lamp exam revealed a 5mm x 3mm epithelial defect, as well as irregular epithelium over the remaining cornea. The anterior stroma was developing haze.
Desperate Measures
We had reached a point of desperation. I decided to fit the eye with a scleral lens to act as a protective device for the cornea.
Based upon the shape of the unaffected eye, he was fitted with a 46.00D, 18.2mm diameter scleral lens. The lens exhibited an estimated 400µm of vault. After an evaluation for proper fit, the lens was removed, coated with a low viscosity non-preserved artificial tear, and replaced. I instructed the patient to leave the lens in place, continue all of the same drops and return in 48 hours.
He returned two days later reporting that he was tolerating the lens well, and that his vision was slowly improving—it was 20/100 OD, and the epithelial defect was 80% resolved. I removed, cleaned and replaced the lens, and instructed him to return in five days.
At the visit five days later, he reported continued improvement in comfort and vision. His vision had increased to 20/50 OD and the epithelial defect was completely closed (figure 1). The cornea still had a mild degree of haze and the epithelium was far from smooth, but improvement was obvious (figure 2).
We had him continue to use the lens on an extended basis and return weekly for removal, cleaning and replacement. I also instructed him to continue to use the autologous serum, prednisolone and ofloxacin QID.
He continued the extended wear of the scleral lens for three more weeks. After four weeks of continuous wear, we educated the patient on proper application and removal of the lens. He continues to use the lens daily, removing the lens at bedtime and inserting the lens upon waking. The epithelium has remained intact and his vision is 20/30 OD with the lens in place.
Treatment for neurotrophic keratitis has traditionally included artificial tears, antibiotic eye drops, steroid eye drops, tetracyclines, autologous serum drops, vitamin therapy, bandage lenses and tarsorrhaphy, depending on the condition and the severity.2,3 Scleral lenses—with their high degree of oxygen permeability, capability of holding a moisture chamber to the corneal surface, ability to vault over the cornea and avoid contact with the corneal surface, and large overall diameter for comfort and stability—seem to be a natural choice for treating these conditions.
1. Groos Jr EB. Neurotrophic keratitis. In: Krachmer JH, Mannis MJ, Holland EJ (eds.). Cornea: Clinical Diagnosis and Management. St. Louis: Mosby; 1997:1340.
2. Smith VA, Cook SD. Doxycycline—a role in ocular surface repair. Br J Ophthalmol. 2004 May;88(5):619-25.
3. Tsubota K, Goto E, Shimmura S, Shimazaki J. Treatment of persistent corneal epithelial defect by autologous serum application. Ophthalmology. 1999 Oct;106(10):1984-9.


