 As I wrote in my last column, nodular corneal degenerations can often be difficult to manage. The symptoms of discomfort and decreased vision can vary greatly, and also can be associated with other conditions, such as chronic ocular surface inflammation and irritation.1 Patients with nodular degenerations often will seek surgical treatment if their symptoms are persistent.
As I wrote in my last column, nodular corneal degenerations can often be difficult to manage. The symptoms of discomfort and decreased vision can vary greatly, and also can be associated with other conditions, such as chronic ocular surface inflammation and irritation.1 Patients with nodular degenerations often will seek surgical treatment if their symptoms are persistent.
In the June 2012 column, I discussed the case of a 33-year-old white female who presented with severe corneal nodular degeneration leading to significant vision loss but who only suffered minor discomfort from the symptoms. The patient has been managed successfully for many years now by piggybacking a gas-permeable (GP) lens over a bandage soft lens. However, if symptoms of discomfort, photophobia and irritation become predominant, sometimes another approach can work better.
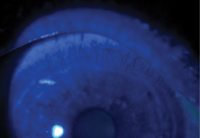
1. Limbal injection at the superior limbus indicates ocular surface inflammation.
A Case Study
EH, a 43-year-old white female, was recently referred for a possible contact lens fitting for Salzmann’s nodular corneal degeneration. She had been diagnosed with this condition 20 years ago, and had undergone multiple attempts to treat it with bandage lenses, corneal scrapings and phototherapeutic keratectomy (PTK).
The most recent PTK was done bilaterally less than six months prior to this evaluation. Her chief complaints were light sensitivity, blurry vision and a chronic scratchy sensation.
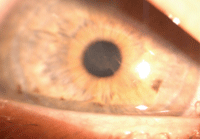
2. Fragile, irregular epithelium in the visual axis.
Her entering acuity without correction was 20/60-2 O.D. and 20/70 O.S. The slit lamp exam revealed an ocular surface mostly free of nodules, though there was ocular surface inflammation (figure 1), as well as areas of fragile, irregular epithelium (figure 2).
At this stage, because so many procedures had already been done on her corneal surface with only fair results, both she and her corneal specialist were determined to forgo any further surgical intervention. After reviewing her past history and discussing her options, I agreed that scleral lenses might be of benefit. This option could significantly improve her vision, and hopefully reduce her symptoms by covering the sensitive corneal epithelium. EH consented and we fitted her with a pair of msd Mini-Scleral Design lenses (Blanchard Labs). To bring her right eye to 20/20 vision, I fitted a 4.40 Sag, 18.0mm, increased profile lens with a power of +1.25D (figures 3 and 4). To achieve 20/20 vision in her left eye, I fitted a 4.60 Sag, 18.0mm, standard profile lens with a power of +0.50D.
After the lenses were ordered and dispensed, I made slight adjustments to the refraction and edge profile over the next few visits. In the end, EH was able to wear her scleral lenses for more than 10 hours a day with good vision. Her symptoms were not fully resolved, but she did notice a difference. Her vision improved and she was satisfied to continue wearing the lenses as her primary mode of vision correction.
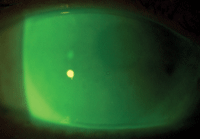
3. Scleral lens with full corneal vault, avoiding contact with raised corneal nodules.
Discussion
Fitting Salzmann’s corneal nodular degeneration in scleral lenses can be an excellent way of correcting vision and providing the best possible comfort in many cases. In fact, scleral lenses have proven effective for a vast array of corneal degenerations and ocular surface diseases.2,3
One difficulty in fitting Salzmann’s corneal degeneration patients with scleral lenses is that the nodules are focal elevations on the ocular surface. Scleral lenses often settle by 100µm or more.4 Ensuring sufficient vault at the time of fitting will allow for that settling to occur without the lens bearing down on these fragile nodules, which would likely lead to a worsening of the symptoms. The nodules are often in the peripheral cornea, making it all the more complex to get sufficient vault to avoid contact with the elevated nodules either at fitting or after lens settling has occurred. In general, larger-diameter sclerals are preferred to allow for a larger corneal chamber and one with sufficient vault all the way to and beyond the limbus.
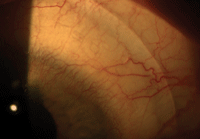
4. A well contoured landing zone of a scleral lens. Notice the superior corneal inflammation.
Nodular corneal degenerations can be difficult to manage. As demonstrated in these last two columns, GP lenses have a significant role in managing these conditions by restoring vision and—to a certain extent—improving symptoms. Whether you choose to go the direction of a larger, vaulting GP lens or something that rides on the cornea (with or without piggybacking) will depend on your patients’ individual presentations.
1. Farjo AA, Halperin GI, Syed N, et al. Salzmann’s nodular corneal degeneration clinical characteristics and surgical outcomes. Cornea. 2006 Jan;25(1):11-5.
2. Romero-Rangel T, Stavrou P, Cotter J, et al. Gas-permeable scleral contact lens therapy in ocular surface disease. Am J Ophthalmol. 2000 Jul;130(1):25-32.
3. Cotter JM, Rosenthal P. Scleral contact lenses. J Am Optom Assoc. 1998 Jan;69(1):33-40.
4. Caroline P, Andre M. Scleral lens settling. CL Spectrum. 2012 May;27:56.


