 |
Many patients with inflamed, dry post-surgical eyes also often present with copious mucus. Doctors spend hours, and significant amounts of money, altering contact lens materials and fits in an attempt to ameliorate symptoms of blurred vision caused by a buildup of mucin on or under lenses—often without success, leaving patients frustrated and unhappy. What to do? Perhaps the answer to this dilemma lies in targeting the root of the problem—why this is happening—rather than addressing the issue after the fact.
Goblet cells (which produce mucus) are located throughout our bodies, including the airways and gut as well as our bulbar and palpebral conjunctivae. Goblet cells are vital to maintaining homeostasis of the ocular surface by providing a defense system and lubrication for the surface epithelia. The mucous layer secreted by the goblet cells is essential for clearing away external pathogens and allergens. Goblet cells also secrete cytokines and modulate dendritic cells.1 In effect, mucus is a friend, not foe, to the ocular surface.
When goblet cells are dysfunctional, however, they can cause significant pathogenesis. In the eye, secretion is induced by stimulation of the afferent nerves in the cornea and conjunctiva, causing a reflex neural arc of the efferent sympathetic and parasympathetic nerves surrounding the goblet cells.2 A key common feature of goblet cell upregulation, regardless of the initiating event (i.e., dryness, allergy or another disease state), is inflammation and the presence of inflammatory regulators. In some patients, such as scleral lens wearers, this overproduction can have adverse consequences.
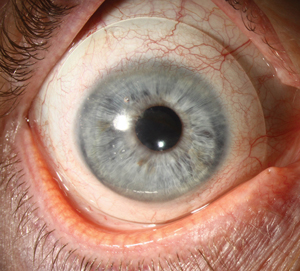 | |
| Fig. 1. A wide, tangential-aligned peripheral scleral landing area will help prevent mucin buildup under the lens. |
Achieving Balance
Scleral contact lenses are often indicated for severe dry eye states, including Sjogren’s syndrome, ocular cicatricial pemphigoid, Stevens-Johnson syndrome and neurotrophic keratitis. However, because these and other conditions produce a chronic inflammatory state of the ocular surface that can lead to mucus buildup, many scleral patients complain of “foggy” vision within minutes to hours following lens application. Thus, it is vital to achieve the right balance between mucus levels and the lens. This can be done in one of several ways:
1. Address all dry eye-related conditions. This includes improving lid hygiene, lubricating the ocular surface with preservative-free products and prescribing nutritional supplements (i.e., omega fatty acids).
2. Address any lens fit-related issues. Instill fluorescein to see if there are any leaks under the lens. Make sure the landing area is wide and tangential to the sclera—avoid focal impingement of the conjunctiva (Figure 1). Limit the central vault to 200 μm to 250μm and make sure there is clearance over the limbus.
3. Always order scleral lenses in the most highly wettable materials available. Do not have the patient continually remove the lens and clean it throughout the day (as much as they are tempted to do so). Lens removal will further drive the overproduction problem by inducing a “mucus fishing syndrome” effect. Instead, use saline vials (0.9% sodium chloride inhalation) to “squirt” the mucus out from under the lens. Conditioning solution or lubricant can be used on a plunger to “squeegee” the front surface of the lens and remove deposits. Mucus production will likely downregulate in two to four weeks, once the inflammatory status of the eye improves.
Consider adding an immunomodulator—such as a steroid—for a short course during scleral lens adaptation if mucus is a problem. Use a mucus-eliminating chemical cleaner weekly to keep the lens surface clean and free of scrubbing induced scratches.
Above all, be sure to educate patients on the fact that mucus is a sign of their disease state and not a result of a poor contact lens fit. Steps should be taken for goblet cell protection, rather than mucus elimination. With proper protection, mucus production will decrease.
1. Garcia-Posadas L, Contreras-Ruiz L, Soriano-Romani L, et al. Conjunctival Goblet Cell Function: Effect of Contact Lens Wear and Cytokines. Eye Contact Lens. 2015 May 19. [Epub ahead of print]
2. Dartt, D. A. 2004. Control of mucin production by ocular surface epithelial cells. Exp. Eye Res. 78:173–185


