 A 75-year-old Hispanic female with chronic, severe symptoms of dryness has been visiting my office fairly regularly. She complains of an eight out of 10 level of pain, photophobia and lacrimation, which does appear to be out of proportion to her physical symptoms (see image below). We tried a variety of treatments including non-preserved artificial tears, ointments, nighttime goggles, steroids, Restasis, plugs and lid repair—all to little or no avail.
A 75-year-old Hispanic female with chronic, severe symptoms of dryness has been visiting my office fairly regularly. She complains of an eight out of 10 level of pain, photophobia and lacrimation, which does appear to be out of proportion to her physical symptoms (see image below). We tried a variety of treatments including non-preserved artificial tears, ointments, nighttime goggles, steroids, Restasis, plugs and lid repair—all to little or no avail.
Understanding Dry Eye
Certainly treating dry eye disease (DED) is not an uncommonly encountered clinical situation. DED, or keratoconjunctivitis sicca, is in fact one of the most frequent complaints that eye care practitioners face in their practices, and is a major public health issue due to its negative affect on a patients’ daily lives.1,2 As eye care practitioners, we are fortunate that commercially available over-the-counter and prescription products are both safe and effective for the majority of patients. However, what else can be done for a recalcitrant dry eye problem in a post-menopausal female, such as my patient?
Age, female gender, and menopause are well-documented risk factors for DED. Sex steroid hormones have been shown to be important for both lacrimal gland and meibomian gland function (MGD).3 David Sullivan, M.D., and colleagues at Harvard University hypothesized that female gender and androgen deficiency were major factors in the pathogenesis of both aqueous deficient and evaporative dry eye in Sjögrens syndrome.4
According to the Canadian Dry Eye Epidemiology Study (CANDEES), the majority of those affected by dry eye are women.4 The researchers concluded that the topical application of androgen would be a safe and efficacious treatment.4
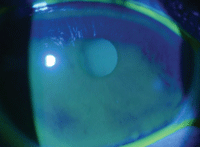
Initial patient presentation shows reduced tear break up but no corneal staining.
A subsequent study led by Debra Schaumberg, O.D., M.P.H., surveyed 39,876 women in the United States who were diagnosed with dry eye syndrome and participated in the Women’s Health Study. They found the prevalence of dry eye increased with age—from 5.7% among women under the age of 50 to 9.8% among women 75 and older. The age-adjusted prevalence was 7.8%, or 3.23 million women, over the age of 50 in the United States.5
In 1998, William Mathers, M.D., and colleagues from the University of Iowa were the first to demonstrate that tear production is correlated with serum prolactin and sex hormone levels prior to and during menopause.6 Cengaver Tamer, M.D., studied the androgen levels of patients with non-autoimmune dry eye, either with or without MGD, compared to a control group. He found that androgen levels of the patients with MGD was significantly depleted compared to the other groups.7
The Treatment
After consulting with my resident and other colleagues, I prescribed 3% testosterone cream to be applied to the upper eyelids twice a day. This cream was compounded at a local specialty pharmacy. Testosterone cream in various formulations has been anecdotally reported as safe and effective in post-menopausal dry eye patients, although large scientific studies have not been conducted.
New Research
Charles Connor, Ph.D., O.D., and Charles Haine, O.D., M.S., from the Southern College of Optometry have developed and studied the use of testosterone cream in DED. Over the years, it has been demonstrated to improve Schirmer scores and subjective symptoms on the Ocular Surface Disease Index (OSDI), as well as increase contact lens wearing time by both increasing tear production and improving meibomian gland secretions. Dr. Connor studied 10 contact lens intolerant female patients, with an average age of 53.5 years, who were treated with 5% transdermal testosterone cream twice daily for three weeks. After treatment, the average contact lens wearing time increased from one hour to 10.5 hours.8,9
In a presentation at the American Academy of Optometry meeting in 2002, Dr. Connor presented work on 20 subjects: five males and 15 females, ages 17 to 71.10 They were divided into two groups: those that applied transdermal cream without testosterone, and those that applied transdermal cream supplemented with 2.5% testosterone. Those that used the testosterone cream showed improved tear break up, Schirmer scores and prolonged contact lens wearing time. The greatest benefit was seen in post-menopausal females, while men had the least benefit.10
Transdermal testosterone promotes increased tear production and meibomian gland secretion, thereby reducing dry eye symptoms.10 Although testosterone is a steroid, it has been shown not to cause an elevation in intraocular pressure after longterm use.11 Argentis Pharmaceuticals acquired three of their patents in 2008 and are currently awaiting FDA approval.12
The Conclusion
Two weeks after initiating treatment, our patient reported a significant improvement in her symptoms. For the first time since I met her, she wasn’t wearing sunglasses when I entered the exam room.
The work of Drs. Connor and Haine, along with anecdotal reports discussed in the literature and amongst colleagues, suggests that transdermal testosterone cream is a viable addition to our toolbox, particularly when existing therapies may not be successful for some patients. However, at this time, it is not FDA approved and patients should be counseled about any off-label use. Long term effects are unknown, especially as they relate to the agent’s conversion to testosterone and estrogen in patients with a medical history of breast or prostate cancer.
1. Schaumberg DA, Sullivan DA, Buring JE, Dana MR. Prevalence of dry eye syndrome among US women. Am J Ophthalmol. 2003 Aug;136(2):318-26.
2. Miljanoviæ B, Dana R, Sullivan DA, Schaumberg DA. Impact of dry eye syndrome on vision-related quality of life. Am J Ophthalmol. 2007 Mar;143(3): 409-15.
3. Sullivan DA, Yamagami H, Liu M, et al. Sex steroids, the meibomian gland and evaporative dry eye. Adv Exp Med Biol. 2002;506(Pt A):389-99.
4. Sullivan DA, Wickham A, Rocha EM, et al. Androgens and dry eye in Sjogrens’s Syndrome. Ann N Y Acad Sci. 2002 Jun;966:211-22.
5. Schaumberg DA, Sullivan DA, Buring JE, Dana MR. Prevalence of dry eye syndrome among US women. Am J Ophthalmol. 2003 Aug;136(2):318-26.
6. Mathers WD, Stovall D, Lane JA, et al. Menopause and tear function: the influence of prolactin and sex hormones on human tear production. Cornea. 1998 Jul;17(4):353-8.
7. Tamer C, Oksuz H, Sogut S. Androgen status of the nonautoimmune dry eye subtypes. Ophthalmic Res. 2006;38(5):280-6.
8. Connor CG. Reduction in OSDI scores suggests symptomatic relief of dry eye with 3% testosterone cream. Poster presented at the American Academy of Optometry meeting, December 9-12, 2004; Tampa, Fl.
9. Connor CG. Use of transdermal testosterone cream to treat contact lens intolerance: A case series. Poster presented at the American Academy of Optometry annual meeting, November 17-20, 2010; San Francisco, Calif.
10. Connor CG. Transdermal testosterone delivery for the treatment of dry eye. Poster presented at the American Academy of Optometry annual meeting, 2002; Orlando, Fl.
11. Connor CG, Jones M. Long term observation of patients using transdermal testosterone cream for the treatment of dry eye. Poster presented at the American Academy of Optometry annual meeting, December 8-11, 2005; San Diego, Calif.


