 In last month’s column, I discussed how how sometimes a corneal transplant is better served in a toric lens than a spherical lens. This is usually the case when the corneal astigmatism is fairly regular and continuous from the donor to the host cornea. However, because this is not typically the case—and there are extreme cases where astigmatism levels are high and the donor and host cornea are very different—it may be best to immediately fit the sclera instead.
In last month’s column, I discussed how how sometimes a corneal transplant is better served in a toric lens than a spherical lens. This is usually the case when the corneal astigmatism is fairly regular and continuous from the donor to the host cornea. However, because this is not typically the case—and there are extreme cases where astigmatism levels are high and the donor and host cornea are very different—it may be best to immediately fit the sclera instead.
A Case Study
This case involves a 33-year-old male who presented for a left contact lens fitting. He had a history of keratoconus and had perviously undergone a full-thickness corneal transplant. While the transplant healed properly, his vision was poor. Several GP lens fitting attempts made by another provider were unsuccessful. His right eye still had keratoconus and he was using a standard keratoconus design, corneal GP lens.
His uncorrected vision in the left eye was 20/600. With a refraction of -2.75 -8.00D x 4, his left eye vision was corrected to 20/60. Corneal topography revealed 18.00D of highly regular corneal astigmatism (see figure 1). Even more telling were the mires, which demonstrated a dramatic difference between the transplant and the host tissue (see figure 2). The previous fitter has attempted fitting him with 10mm to 11.5 mm GP lenses, all of which demonstrated significant inferior edge lift. My first thought was to try a toric corneal GP to try to reduce the inferior edge lift. An initial lens was ordered in base curves of 48.00mm x 56.00mm with powers of -9.75D and -17.75D.
Upon dispensing the toric GP, it was evident that there was still a significant degree of edge lift inferiorly and the lens was still very unstable—not due to the astigmatism of the graft, but rather the significant curve change at the donor-host interface.
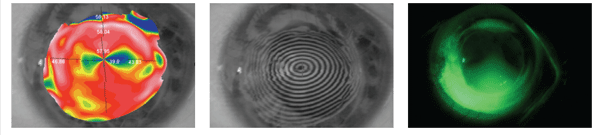
1. Corneal topography demonstrates 18.00D of fairly regular astigmatism.
2. Corneal mires indicate dramatic change in curvature from graft to host.
3. Mini-scleral lens fit on this patient.
We discussed the options again, including the use of other types of contact lenses (such as hybrids and sclerals), laser vision correction or relaxing incisions for the astigmatism. We decided on a larger diameter lens that was fitted to the sclera, thus taking the irregularity of the astigmatism and the interface out of play. After trial fitting a variety of semi- and mini-scleral lenses, we ordered him the DigiForm Scleral (Truform Optics) from the “N” series in a base curve of 7.10mm, power of -10.75D and diameter of 15.0mm with no fenestration in Boston XO2 material (see figure 3).
With the mini-scleral lens, his left eye measured 20/20. After teaching him the proper care and handling, the lens was dispensed. He returned two weeks later for follow-up and said he was very happy with his vision and comfort and was wearing the lens up to 14 hours a day every day. Evaluating the lens after several hours of wear, it was clear that it was tight in the periphery. I reordered the lens with a flatter edge profile. Nevertheless, he was so happy with the comfort in his left eye that he requested a similar refitting for his right eye.
While in last month’s case, the patient was initially referred for a scleral lens fitting but was better served with a toric corneal lens, this case proved to be the opposite. Certainly, there are certainly cases where toric corneal lenses are beneficial for post-graft patients, but this typically occurs where astigmatism is continuous from the graft through the host. Unfortunately, a significant percentage of post PK patients have issues with curvature change at the donor-host interface and this poses a problem for corneal lenses and stability. In this example, by vaulting over the entire cornea and simply fitting the sclera, we avoid the issues of corneal astigmatism and curve change from the donor to the host tissue that caused such instability in the corneal lens fits.


