 New techniques and advances in imaging technologies have been a topic of great interest as of late, particularly improvements in optical coherence tomography (OCT) and confocal microscopy (CM) for the anterior segment. Of course, one key consideration for any new technology is its clinical practicality. This month, we’ll unravel the intricacies of these technologies, and consider how they are being employed as tools for both patient care and clinical research.
New techniques and advances in imaging technologies have been a topic of great interest as of late, particularly improvements in optical coherence tomography (OCT) and confocal microscopy (CM) for the anterior segment. Of course, one key consideration for any new technology is its clinical practicality. This month, we’ll unravel the intricacies of these technologies, and consider how they are being employed as tools for both patient care and clinical research.
Optical Coherence Tomography
The OCT of today comes in two basic formats: time-domain (TD-OCT) and spectral domain (SD-OCT). TD-OCT employs a technology that captures image scans serially according to depth, and uses them to reconstruct an image of the scanned tissue. On the other hand, SD-OCT separates reflective signals according to wavelength, and can collect scans for subsequent tissue re-construction in parallel. The result of these distinctions is that SD-OCT devices can collect scans as much as 100 times faster than TD-OCT devices, thus allowing for greatly improved image clarity and detail.1 Because the overall design of the SD-based devices is simpler, they also are generally less expensive.
Though traditionally used for vitreoretinal evaluation, recent OCT advancements allow for anterior segment imaging as well. An example of an emerging application for OCT is in the diagnosis of keratoconus. In its early stages, keratoconus can often go undetected. OCT has the ability to identify those individuals with early corneal thinning or other changes in corneal shape.2 Detection before the appearance of significant changes—including alterations in visual acuity—can allow for early intervention, and also can help identify patients who may be at greater risk for complications from LASIK surgery. By comparing images captured over time, it is possible to follow the progression of corneal thinning with measures comparable or superior to more traditional ultrasound pachymetry.

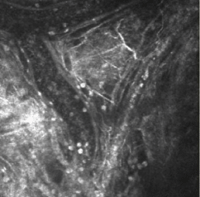
In vivo imaging of conjunctival blood vessels before (left) and after (right) allergen challenge. White cells are clearly visible following challenge, and some of these can be see migrating out of vessels into extravascular space.
One of the newer experimental applications of OCT is in dry eye assessment, where it can be used to measure tear film volume by means of tear meniscus height.3 The noninvasive nature of OCT confers a substantial advantage over other tear film assessments. Schirmer’s testing and most other methods of evaluation are disruptive to the ocular surface, potentially skewing the results. Not so with OCT.
In addition, treatment protocols for other anterior segment conditions—such as corneal scars or dystrophies, corneal transplants and anterior segment malignancies—have all benefitted from advances in OCT imaging technologies.
OCT also has become an essential tool in anterior chamber biometry, whether used to help better fit IOLs or to obtain more accurate angle measurements. Unlike ultrasound-based methods, there is no need for direct contact with the ocular surface using OCT. These measures are completed very rapidly, minimizing motion artifacts.
Confocal Microscopy
While the use of OCT for imaging the retina and anterior segment continues to expand, another methodology—confocal microscopy—has also made the move from the back to the front of the eye, becoming a standard technique for assessment of the conjunctival and corneal surface.4 CM employs standard light sources to image the cornea, or uses laser scanning technology (similar to that used for retinal imaging) to view the cornea, conjunctiva, lid margins and lacrimal glands. This noninvasive, high-resolution imaging can be used to identify and track ocular infections, assess corneal defects and monitor epithelial health in conditions, such as dry eye or chronic allergy.
When compared to traditional slit lamp imaging, confocal microscopes can provide a higher magnification and depth of view, which allows for visual diagnosis of conditions caused by Acanthamoeba or Fusarium infections. This is significant because diagnostic confirmation via culturing can take several weeks. CM also can be used to assess and monitor therapeutic efficacy for these and other infections, such as herpes keratitis.5
Looking Ahead
Several recent studies have explored the use of corneal imaging with CM as a means to track and diagnose diabetic retinopathy by longitudinal assessment of corneal nerve morphology.6 A number of these reports have been able to correlate changes in the corneal nerve fibers with other metrics of diabetic neuropathy such as quantitative sensory testing and nerve conduction velocities. At the same time, these studies highlight a major challenge in the use of CM for research: There is a need for more reliable methods to capture images of the same regions of the ocular surface––especially when studies involve dynamic events, such as changes in nerve morphology or inflammation.
The use of CM imaging has become particularly useful in studies of new treatments for ocular surface disorders. The real-time aspect of this imaging allows researchers to directly assess the efficacy of new therapies in terms of macrophage and lymphocyte infiltration into the conjunctiva as well as in measuring changes in epithelial integrity.7 The ability to track these ocular surface changes likely will pave the way for studies that can help identify the therapies that may be best suited to treat the earliest stages of dry eye and allergic conjunctivitis.
The very latest technological advancements typically are found in experimental settings, and the same goes for the newest methodologies in assessing and monitoring dry eye disease. Researchers at our company, Ora, Inc., have been addressing the sometimes baffling assortment of metrics used in diagnosing dry eye by focusing on new, objective criteria in combination with patient subpopulation analysis.8
One example of this is our computer-based imaging method, which is used to define and track dry eye signs and symptoms.9 These studies are designed to bring new therapeutics to market. They represent a merging of the best of both worlds in the development of new ocular therapies: the latest in image capture and analysis techniques with more traditional clinical research methods.
Dr. Abelson is the founder and scientific advisor for Ora, Inc. Dr. McLaughlin is an employee of Ora, Inc.
1. Grover S, Murthy RK, Brar VS, Chalam SK. Comparison of retinal thickness in normal eyes using stratus and spectralis optical coherence tomography. Invest Ophthalmol Vis Sci. 2010 May;51(5):2644-7.
2. Ramos JLB, Li Y, Huang D. Clinical and research applications of anterior segment optical coherence tomography—a review. Clin Experiment Ophthalmol. 2009 Jan;37(1):81-9.
3. Ibrahim OMA, Dogru M, Takano Y, et al. Application of Visante optical coherence tomography tear meniscus height measurement in the diagnosis of dry eye disease. Ophthalmology. 2010 Oct;117(10):1923-9.
4. Niederer RL, McGhee CNJ. Clinical in vivo confocal microscopy of the human cornea in health and disease. Prog Retinal Eye Res. 2010 Jan;29(1):30-58.
5. Hillenaar T, van Cleynenbreugel H, Verjans GM, et al. Monitoring the inflammatory process in herpetic stromal keratitis: the role of in vivo confocal microscopy. Ophthalmology. 2012 Jun;119(6):1102-10.
6. Edwards K, Pritchard N, Vagenas D, et al. Utility of corneal confocal microscopy for assessing mild diabetic neuropathy: baseline findings of the LANDMark study. Clin Exp Optom 2012 May;95(3):348-54.
7. Angjeli E, Lane KJ, Contractor M, et al. Use of in vivo confocal microscopy to assess allergic inflammation following conjunctival allergen challenge. J Allergy Clin Immunol. 2012;129(2):AB189.
8. Abelson R, Lane KJ, Angjeli E, et al. Measurement of ocular surface protection under natural blink conditions. Clin Ophthalmol. 2011 Sep;5:1349-57.
9. Abelson R, Lane KJ, Rodriguez J, et al. Validation and verification of the OPI 2.0 System. Clin Ophthalmol. 2012;6:613-22.


