We have known about the presence of higher-order aberrations in the eye since the 1950s, but it was only in the last decade that they were primarily identified as spherical aberration.1-3 More recently, however, the significant role of non-rotationally symmetrical aberrations, such as coma and trefoil, has been studied and identified as a major contributing factor to the less than ideal optical performance of the human eye.4 Using the Shack-Hartmann based wavefront sensors, measurements over the last decade have opened the door to identifying the magnitude and form of higher-order wavefront aberrations in preoperative, physiological populations.5,6
We performed an initial inspection of the average distribution of higher-order wavefront aberrations across a large population requiring vision correction, generated from a series of clinical studies conducted under an identical protocol by our group. It shows a distinct deviation from zero for the spherical aberration Zernike term, while all other Zernike terms have an average close to zero—a value expected of a biological optical system attempting to optimize itself across a population (figure 1). This agrees with previous populations reported in the literature.6
These data suggest that an appropriate aspheric surface designed to correct the spherical aberration of the eye would significantly reduce the higher-order wavefront aberration of the eye if it were incorporated into a contact lens.
Spherical Aberration and Image Quality
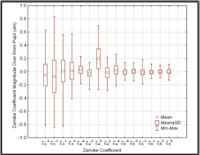
1. Mean values for the higher-order wavefront aberration Zernike coefficients in the total study population.
Spherical aberration can have a significant impact on overall image quality—both the contrast and resolution of an optical system. Reducing the magnitude of spherical aberration in the eye can give the patient better image quality at distance and has the potential of giving the practitioner a clearer refractive endpoint when determining the best sphere power lens. Interestingly, when spherical aberration is present, the sphere power that gives the best resolution (acuity) does not necessarily give the optimal contrast at the retina and may increase the presence of halos around small bright lights. Optimizing the contrast and presence of halos by changing the sphere power will typically result in a slight reduction of resolution (figure 2).
Adding an appropriate amount of negative spherical aberration to a soft contact lens to correct the population average would significantly reduce the magnitude of the higher-order aberrations of most patients—with a presumed improvement in retinal image quality, particularly under low light conditions where large pupil sizes are most prevalent. Indeed, while there is a wide range of spherical aberration values across our patient population, 92% are positive in nature (figure 3).
In order to better understand how a population of eyes could benefit from spherical aberration correction, clinical eye models were created in commercially available optical design software (Zemax) to match the biometry and ocular aberrations of each individual patient’s eyes. These models were used to theoretically predict the retinal image quality with spherical and aspheric contact lens designs.
In this study, 446 of 1,333 eyes from our available population dataset were used; all had refractive and corneal cylinder less than or equal to -0.75D with a 6mm pupil diameter. Using the same soft contact lens design as a basis, two lens designs were tested with each of the 446 individual eye models—one soft lens with aspheric optics designed to correct the population average spherical aberration value and a similar design that incorporated spherical optics with no intended spherical aberration correction. Each eye was corrected with the appropriate spherical power to minimize their optical defocus.
Keep in mind that the spherical lens designs inherently demonstrated spherical aberration due to their highly curved spherical surfaces—negative spherical aberration for negative power lenses and positive spherical aberration for positive power lenses, in proportion to their back vertex power. Spherical lenses with a power of -5.00D inherently have a similar magnitude of negative spherical aberration over a 6mm pupil as aspheric contact lenses designed to correct the positive spherical aberration average of the myopic patient population.7

2. LogMAR chart images captured using a CCD camera with optics designed to mimic the human eye in power, length and magnification.
Predicted logMAR visual acuity was calculated using a novel pattern-matching metric to simulate retinal image quality in Zemax.8 A predicted logMAR acuity value was determined for each of the aspheric and spherical optic soft lens designs for each of the selected eyes over a 6mm pupil size (figure 4).
Designing A New Lens
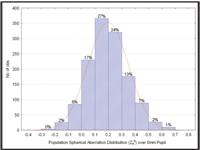
3. Population spherical aberration distribution for the study population of 1,333 eyes.
The addition of aspheric surfaces to induce the appropriate amount of negative spherical aberration to correct the population average positive spherical aberration shows an improvement for many of the eyes. But the next question is how much further improvement could be achieved if spherical aberration was optimized for each eye? Realistically, this would require a lens designed for each patient’s eye—a customized spherical lens to maximize retinal image quality, with spherical aberration optimized as well.
To answer this question, a further modeling study was conducted using the same 446 eyes and the same basic lens designs. In this case, the sphere was iterated so that the residual defocus was essentially zero (i.e., less than 0.25D), and the spherical aberration was optimized to leave the eye with zero residual spherical aberration over a 6mm pupil diameter (figure 5). While both sphere-only and spherical abberation optimization show an improvement over the previous model results, it is clear that there is an overall benefit in retinal image quality quantified as predicted logMAR visual acuity for those eyes with their spherical aberration fully corrected.
However, a number of eyes still show a significant potential for improvement in retinal image quality, with predicted logMAR acuity poorer than 20/20. While this is not surprising given that the pupil size is 6mm and we are essentially predicting logMAR acuity under low illumination conditions, this result clearly shows the impact of the residual higher-order wavefront aberrations other than sphere, cylinder and spherical aberration. Coma and trefoil play a significant role in retinal image quality under large pupil conditions, and ideally, correction of these terms should contract the spread of the population distribution for predicted logMAR visual acuity under 6mm pupil conditions toward the preferred end of the graph.
Correcting Higher-Order Aberrations
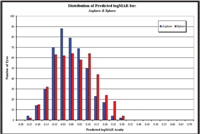
4. As a population, the eyes demonstrated better image quality by theoretically predicted logMAR acuity with the aspheric optics lens compared to the spherical optics lens.
Additional modeling with the 446-eye sample, correcting sphere and cylinder, spherical aberration, coma and trefoil represents the optimum soft contact lens optical correction. Higher-order aberrations other than these (i.e., other 4th order aberrations such as secondary astigmatism and 5th or 6th order aberrations) are impacted by lens decentration and rotation to a level that the typical movements of a soft lens on eye may nullify the gains of correcting them.9 Conversely, correction of coma and trefoil still provide a benefit to retinal image quality even when decentered or rotated by amounts typically seen with well fitting soft contact lenses.
All 446 eyes were corrected with the same lens design: correction of sphere and astigmatism; sphere, astigmatism and spherical aberration; and sphere, cylinder, spherical aberration, coma and trefoil. Again, the metric of choice for retinal image quality was predicted logMAR acuity generated for a 6mm pupil size, representing low illumination conditions. Figure 6 illustrates the improvement in retinal image quality with correction of sphere and cylinder only, spherical aberration in addition to sphere and cylinder, and finally, the significant improvement in predicted logMAR acuity when coma and trefoil are also corrected. Note that the majority of eyes have shifted to the left of the graph, indicating a significant improvement in low illumination, large pupil retinal image quality when all significant lower- and higher-order aberrations were corrected.
Aspheric Surfaces Lenses
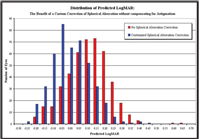
5. The distributions for the 446 eyes, optimized for sphere only in one case, and for sphere and spherical aberration in the other case.
Generating the appropriate aspheric surfaces to correct spherical aberration is relatively straightforward for either lathe cut or cast molded lenses with today’s sophisticated CNC-controlled diamond point turning. The difficulty lies in ensuring that the tools, molds and ultimately, lenses have the correct spherical aberration values. Traditional lensometers are inadequate to measure the spherical aberration of a lens, even if measurements are performed across a variety of apertures, because a single measure of the continuously changing surface is not sufficient to ensure the correct optics.10 The recent introduction of high-resolution wavefront sensors provides the ability to measure the spherical aberration value of the hydrated contact lens along with all lower- order and higher-order aberrations. Post-measurement processing of the wavefront data can also provide the power profile of rotationally symmetric contact lenses, which provides a more clinically intuitive method to fully characterize the spherical aberration correction in a finished lens with aspheric optics (figure 7).11
The Challenges
Correction of sphere and the population average spherical aberration can be performed in a rotationally symmetric lens design using today’s disposable lens manufacturing platforms and fitting paradigms. Indeed, several companies currently provide lenses that attempt to partially or fully correct the population average spherical aberration. Similarly, a lens that fully corrects the sphere and spherical aberration of the eye could be produced using the same lens design, with spherical aberration being an additional parameter used by the clinician to select the appropriate lens. To custom correct the spherical aberration—or for that matter, the astigmatism, coma or trefoil of the eye—requires a lens with non-rotationally symmetric optical surfaces. All these aberrations require the lens to be rotationally oriented on the eye, and so, much like today’s lenses designed to correct astigmatism, an optically customized contact lens would require a prism-ballast, peri-ballast or other form of thickness variation to ensure stable on-eye orientation. Naturally, for either of these last two lens options, the clinician would need to use a diagnostic aberrometer to identify the spherical aberration and/or other higher-order aberrations for the individual eye undergoing correction.
The question that arises is how to provide a wavefront aberration-correcting soft contact lens in today’s paradigm of affordable frequent replacement and disposable lenses. These lenses need to be customized to an individual eye, yet the physiological needs of patients and demands of clinicians make it necessary to provide up to a year’s supply of weekly to monthly replacement lenses at any one time. Figure 8 demonstrates one proposed model for order and delivery of a wavefront aberration-correcting soft lens customized to an individual eye.
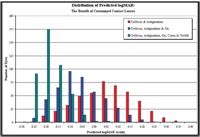
6. Predicted logMAR acuity values with 6mm pupils for customized lens designs with spherical optics to correct defocus and astigmatism only; aspheric optics to correct defocus, astigmatism and spherical aberration; and fully customized optical surfaces to correct defocus, astigmatism, coma, trefoil and spherical aberration.
First, the patient’s eye is measured with a trial lens in place, which, much like today’s toric lenses, has the lens orientation features of the final lens design but does not contain the customized optics of the final lens. This allows any aberrations that are induced or altered by the conformation of the lens itself to be measured by a wavefront sensor at the same time as measuring the total wavefront error of the patient’s eye. The Zernike coefficients are uploaded to a central remote server along with other necessary fitting data through a modem in the wavefront sensor computer. The lathing parameters necessary to cut the non-rotationally symmetrical front surface using a three-axis CNC lathe are calculated by the central server and downloaded into the lathe, generating the prescribed number of lenses from a single trial lens to a one-year supply. These lenses are then processed, packaged, sterilized, labeled and returned to the prescribing clinician’s office within a few days. If necessary, the process can be repeated with the new lens in-situ, to refine the wavefront aberration correction.
Lens manufacturing methods need not be limited to lathing only—a cast molding procedure similar to current disposable lenses could be used to provide the basic lens structure, the process used to create the final higher-order wavefront-correcting front surface over the optical zone of the lens. Alternatively, a laser, similar to those used for refractive surgery procedures, could be used to create the final optical zone surface as a secondary process to the current manufacturing procedures used for creating disposable prism-ballasted toric lenses.
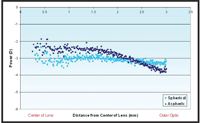
7. Power profiles of a -3.00D spherical contact lens and a -3.00D aspheric
contact lens.
What the Future Holds
New wavefront aberration diagnostic and metrology techniques and CNC-controlled diamond point-turned lathing capabilities have opened the door for manufacturers to provide lenses capable of correcting spherical aberration and other higher-order aberrations. Patients wearing these lenses will experience better retinal image quality, especially under large pupil, low illumination conditions, such as night driving or viewing a movie at the cinema.
Correction of spherical aberration is relatively straightforward in lenses designed to correct myopia or hyperopia and several manufacturers are attempting to provide such designs, usually correcting or reducing the population average value for spherical aberration. Enhancing these designs to correct astigmatism, individual spherical aberration and even coma and trefoil wavefront aberrations will require a shift in the fitting paradigm performed today. While this is technically feasible, it may be several years before the marketplace is ready for a disposable soft contact lens with optics customized to an individual eye.12,13
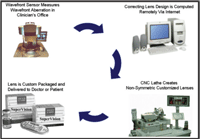
8. Schematic drawing representing a potential business model for fitting, manufacturing and delivering fully customized disposable contact lenses designed to fully correct the significant higher-order aberrations of the eye
Ian Cox is a distinguished research fellow and director of lens design, Vision Care Research and Development at Bausch + Lomb. Since 1998, Dr. Cox has been an adjunct professor at the University of Rochester, collaborating on the role of ocular aberrations in visual performance.
Amanda C. Kingston is an optical design engineer, Vision Care Research and Development at Bausch + Lomb, where she designs lenses and evaluates the optical performance based on predictive models of visual acuity. She also is a Corporate Certified Ophthalmic Assistant through JCAHPO.
1. Ivanof A. About the spherical aberration of the eye. J Opt Soc Am. 1953;46(10):901-3.
2. Jenkin TCA. Aberrations of the eye and their effect upon vision. Part II. Br J Physiol Opt.1962;20:161-201.
3. Koomen M, Tousey R, Scolnik R. The spherical aberration of the eye. J Opt Soc Am. 1949 May;39(5):370-6.
4. Howland HC, Howland B. A subjective method for the measurement of the monochromatic aberrations of the eye. J Opt Soc Am. 1977;67(11):1508-18.
5. Porter J, Guirao A, Cox IG, Williams DR. Monochromatic aberrations of the human eye in a large population. J Opt Soc Am A Image Sci Vis. 2001 Aug;18(8):1793-803.
6. Salmon T, van de Pol C. Normal-eye Zernike coefficients and root-mean-square wavefront errors. J Cataract Refract Surg. 2006;32;2064-74.
7. Dietze HH, Cox MJ. On- and off-eye spherical aberration of soft contact lenses and consequent changes of effective lens power. Optom Vis Sci. 2003 Feb;80(2);126-34.
8. Pinto C, Kingston A, Venkiteshwar M, Ludington P. Pattern recognition as a retinal image quality metric. Invest Ophthalmo Vis Sci. 2008;49:E-Abstract 995.
9. Guirao A, Williams DR, Cox IG. Effect of rotation and translation on the expected benefit of an ideal method to correct the eye’s higher order aberrations. J Opt Soc Am A Image Sci Vis. 2001 May;18(5):1003-15.
10. Collins MJ, Goode A, Davis BA, Tait A. A computer-interfaced vertometer system for contact lenses. Optom Vis Sci. 1997 Jan;74(1):59-65.
11. Vogt AKS, Bateman K, Green T, Reinde, B. Using power profiles to evaluate aspheric lenses. CL Spectrum. 2011 Jan.
12. Marsack J, Parker KE, Niu Y, et al. On-eye performance of custom wavefront guided soft contact lenses in a habitual soft lens-wearing keratoconic patient. J Refract Surg. 2007 Nov;23(9):960-4.
13. Marsack JD, Parker KE, Applegate RA. Performance of wavefront-guided soft lenses in three keratoconus subjects. Optom Vis Sci. 2008 Dec;85(12):E1172–E1178.


