There is an expressed need today to create new evidence-based standards of practice to manage the development of refractive error around the globe. Due to the growing prevalence and the far-reaching economic impact and sequelae of myopia, the primary emphasis has been on what some call myopia control, which may only be a subset of the greater field of refractive therapy.1,2 While the bulk of the work concentrates on myopia, some of the strategies also appear to have value in regulating the development of hyperopia and astigmatism.3,4
A group has been formed with the purpose to gather all evidence relating to myopia control in an effort to establish a recommended standard of care and educate practitioners. The ultimate mission is to reduce the incidence and prevalence of myopia through timely intervention by eye care practitioners worldwide. Under the leadership of Richard Anderson, O.D., the group is working to generate a document entitled, “Evidence-Based Clinical Practice Guideline for Juvenile Myopia.”
Pick Your Clinical Strategy
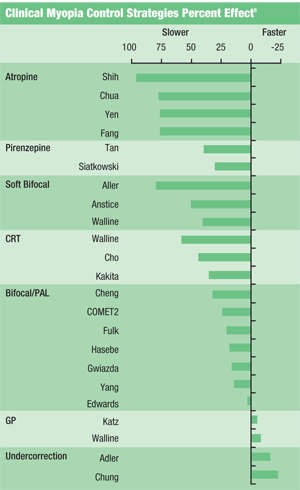
1. Literature summary of the effects of clinical strategies on the progression of myopia, summarized by Dr. Walline, but formatted from most positive to most negative.
Jeffery Walline, O.D., Ph.D., compiled a useful table for reporting the results of a number of randomized, controlled and published studies investigating the impact of clinical strategies for myopia control (figure 1).5 This table shows that the strategies which appear to have value are the use of muscarinic antagonists, bifocal soft lenses and corneal refractive therapy. Single-vision spectacle, bifocal spectacle, progressive addition spectacle, single-vision rigid gas-permeable and single-vision hydrogel contact lenses have all failed to show significant ability to regulate myopia development. Myopia development may be exacerbated or accelerated by under-correction and GP lenses.
Because the current standard of prescribing single vision spectacle lenses may be contraindicated as being neither protective or preventive, there is an interest to define a new standard of care. In fact, a recent study concluded that 0.01% atropine appears to be as effective as the previously prescribed 1%, while eliminating the side effects of long-term use of the higher concentration.6 The discovery unveils a new treatment option for patients with emerging myopia.
Peri-Form and Peri-Focus Lenses
There are two related contact lens strategies at the center of the myopia control discussion. Peri-form results from reshaping the cornea following corneal refractive therapy for myopia. The peri-form cornea is oblate, rather than the normal prolate corneal shape (figure 2). The mid-periphery of the cornea has a shorter radius of curvature than the central or apical radius. A close examination of the topography of post-treatment peri-form corneas demonstrates an increase in the spherical aberration of the eye compared to the pre-treatment measure of spherical aberration.7,8
Peri-form myopia control can be addressed through an increase in positive spherical aberration or from the relative myopic peripheral defocus resulting from the post-treatment cornea. There may be other mechanisms involved in the apparent positive effect in regulating the development of myopia from corneal refractive therapy.
There is evidence that supports a correlation between peri-form treatment and the regulation of myopia. Three independent reported longitudinal studies by Pauline Cho, Ph.D., Dr. Walline and Tetsuhiko Kakita, M.D., share the same conclusions of reduced vitreous chamber depth growth in eyes undergoing corneal refractive therapy compared to control groups wearing conventional spectacle or contact lenses.9-11 In each case, the standard deviation of the corneal reshaping group is relatively high, indicating that some eyes enjoy better control of the growth than others. The mean growth in the corneal reshaping groups remained significantly lower than the control groups; however, some eyes did show myopia progression.
Dr. Kakita further observed that the control of growth was greater the higher the initial refractive error. This raises concerns for the effectiveness of current corneal reshaping lenses for eyes with low or emerging myopia. William Meyers, Ph.D, and I have described lens design requirements for forming the peripheral cornea of an eye with emerging myopia without changing the central cornea.12 Causation, along with the precision of the treatment for all eyes, has not been established.
Earl Smith, O.D., Ph.D., and colleagues used an animal study to support the clinical observations of reduced axial length growth and reduced progression of myopia in patients who have continued in programs of overnight corneal reshaping.13 Research using foveal ablation and peripheral defocus demonstrates promise for a peri-focus strategy, where the peripheral defocus is controlled by the optics of spectacle or contact lenses.
The first peri-focus spectacle lens study reported weak, yet positive, results in controlling the development of myopia and suggested the need for further investigation.14 Another early peri-focus contact lens study also reported weak, but positive, results in controlling the development of myopia.15 Dr. Smith recently reported concern for the peripheral defocus model alone, and suggested that concern for the foveal optics may also be an issue.16 The role of spherical aberration may also be an important element, along with peripheral defocus.
Even so, clinicians have an opportunity to prescribe peri-focus contact lenses in the form of distance-center multifocal contact lenses. They should pay particular attention to understanding the lens designs of current multifocal lenses. Many of the lenses available today are center-near multifocal designs. These would not have the optics that approximate the peri-focus lenses indicated for correcting peripheral hyperopic defocus. The intention, as taught by the proponents of peripheral defocus is to have central optics that focus axial light onto the fovea, while having peripheral optics which focus off axis light in front of the retina.17 Hence, a distance center multifocal is required to meet this intended strategy; a center-near multifocal would do the exact opposite and would be contraindicated.
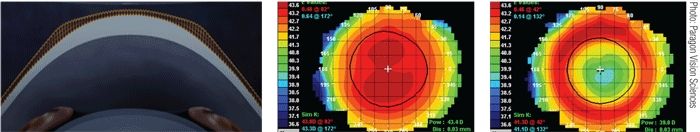
2. Change in shape and optics of anterior cornea from prolate to oblate with corneal refractive therapy.
The role of measuring the peripheral refraction is a key element of modulating peripheral focus. Auto-refractors can be harnessed to measure the peripheral refraction (figure 3). Keep in mind that if you have 10 eyes with 3.00D of myopia, each may have a different peripheral refraction. The peripheral refraction is a function of the shape of the globe and the crystalline lens. Change in shape and optics of anterior cornea from prolate to oblate with corneal refractive therapy.ystalline lens. The equatorial diameter can be larger or smaller while the axial length may be the same. Often, myopic eyes are more prolate, which is understandable because they have a smaller equatorial diameter but a longer axial length. This prolate shape can cause the resultant peripheral hyperopic defocus. Hyperopic eyes are known to be less prolate, or more round, when comparing the equatorial diameter to the length.
The peripheral crystalline lens geometry also contributes to peripheral defocus. A crystalline lens that decreases in power peripherally will contribute to the peripheral hyperopic defocus. Because each eye can be unique, there will not be one peri-focus lens design and one add power capable of providing the same peripheral focus relative to the peripheral retinal location and/or crystalline lens geometry for all eyes.
3. IProfiler Plus (Carl Zeiss Vision) combination instrument can measure on axis spherical aberration, off-axis peripheral refraction and corneal topography for peri-form and peri-focus refractive therapy clinical intervention.
The region of primary concern for peripheral refraction is about 30º from the fovea. A peripheral refraction can be conducted with an auto-refractor and by creating eccentric fixation targets that are 30º nasal and temporal from the straight-ahead fixation of the instrument. In this manner, a central refraction can be conducted in the conventional manner and then a 30º nasal refraction and a 30º temporal refraction would follow. The comparison of the values will give an estimate of the peripheral defocus for the individual eye. It is easier to have patients turn their heads to allow their eyes to point straight at the eccentric fixation targets.
This procedure also can be conducted with a contact lens in place. There is value in measuring the central refraction and higher order aberrations with contact lenses. This will allow testing different brands of single vision lenses for the desired lens-eye spherical aberration. Then a peripheral refraction can be measured in the nasal and temporal 30º fields to measure the peripheral defocus. The same procedure can be conducted with a distance center multifocal lens in place (figure 4). Each eye may require a different optical design to achieve a desired spherical aberration and/or a desired peripheral focus.
It should be noted that several patents have been issued that claim the use of contact lenses and spectacle lenses for myopia progression control. The order and supply of lenses for this purpose could infringe the issued patents as the lenses and methods of prescribing are specified and claimed.18-21
The Importance of Outdoor Activity

4. Center distance multifocal contact lenses are a form of peri-focus lens design for myopia control. Customized design and visual axis registration may be required to optimize refractive therapy.
Lisa Jones, O.D., Ph.D., and colleagues reported a correlation of decreased myopia with increased outdoor activity.22 The protective relationship is significant and supports the importance of recommending outdoor daytime activity when consulting with parents about their children before myopic onset.
Remember that correlation and causation may not be the same. There may be continued work to study the finite elements of the multifactorial phenomenon of outdoor vs. indoor activity and lifestyle (i.e., the roles of the higher light level alone, ultraviolet light, physical activity and ocular motility, accommodation, gaze, saccades and vergence, and near-centered task differential between activities).
Historically, the role of form deprivation—where the peripheral retina of test eyes was occulted—resulted in the rapid development of myopia with concomitant increased vitreous chamber depth. Early animal studies by Christine Wildoset, O.D., Ph.D., and colleagues, as well as recent studies by Dr. Smith and colleagues, reported the ability to modulate eye growth by regulating the retinal luminance in indoor studies.23,24 This discovery is consistent with the above mentioned outdoor activity correlation and may suggest a mechanism for the role of outdoor activity in regulating myopia as increased light passing into the eye.
Donald Mutti, O.D., Ph.D., and colleagues reported myopic patients were found to have lower vitamin D intake and vitamin D blood serum levels than those without myopia.25 Research is being conducted to evaluate whether there is a connection between outdoor activity and vitamin D blood serum levels, as well as to connecting vitamin D with ocular growth.
Indications for Contemporary Clinical Practice
Generally, myopia is a nuisance and reduces the quality of life of our patients. Specifically, higher myopia is associated with secondary ocular disease. The earlier the onset, the higher the myopia is forecast to become.26 For this reason, we should intervene early and consult with parents and patients with myopia. Literature reinforces the following recommendations: increased outdoor daytime activity, increased vitamin D intake, atropine 0.01%, corneal refractive therapy, and peri-focus contact lenses.
At the 2012 Global Specialty Lens Symposium, panelists responded that they believed it was proper to recommend corneal refractive therapy or center distance contact lenses for patients who were progressing in myopia—that it may do good and it would do no harm.16 What we clearly see is that the standard of care for prescribing single-vision spectacle lenses to myopic patients holds no value in protecting or preventing progression. Today, our patients can turn to the web to learn about wholistic approaches to regulating the myopia of their children. At a minimum, we should offer our patients basic education on the importance of outdoor daytime activity and vitamin D. There is mounting evidence to support treatment plans including the prescription of muscarinic antagonists and the prescription of peri-form or peri-focus contact lenses.
Dr. Legerton is an author, lecturer, inventor and consultant to the ophthalmic industry. He is a cofounder of SynergEyes and Innovega, and has 32 issued U.S. patents for contact lens technology including SynergEyes, Paragon CRT, myopia progression control, presbyopic laser refractive surgery, and novel multifocal contact lenses. His most recent patent is assigned to Innovega for the iOptik contact lens enabled wearable computer. He has no financial interest in the technology discussed as all patents are assigned royalty free.
1. Vitale S, Sperduto RD, Ferris FL 3rd. Increased prevalence of myopia in the United States between 1971-1972 and 1999-2004. Arch Ophthalmol. 2009 Dec;127(12):1632-9.
2. Rein DB, Zhang P, Wirth KE, et al. The economic burden of major adult visual disorders in the United States. Arch Ophthalmol. 2006;124(12):1754-60.
3. Aller T. Manipulation of retinal defocus to stimulate axial elongation in hyperopia. Optometry Vis Sci. 2010 Jan;88:395-403.
4. Legerton JA, Meyers WE. Methods and therapeutic optical devices for the regulation of astigmatism. US Patent 8128223; March 6, 2012.
5. Walline J, Lindsley K, Vedula S, et al. Interventions to slow progression of myopia in children. Cochrane Database Syst Rev. 2011 Dec 7;(12):CD004916.
6. Chia A, Chua WH, Cheung YB, et al. Atropine for the treatment of childhood myopia: safety and efficacy of 0.5%, 0.1% and 0.01% doses (Atropine for the Treatment of Myopia 2). Ophthalmology. 2012 Feb;119(2):347-54.
7. Joslin CE, Wu SM, McMahon TT, Shahidi M. Higher-order wavefront aberrations in corneal refractive therapy. Optom Vis Sci. 2003 Dec:80(12):805-11.
8. Asbell PA. Corneal refractive therapy and the corneal surface. Eye Contact Lens. 2004 Oct:30(4):236-7; discussion 242-3.
9. Cho P, Cheung SW, Edwards M. The longitudinal orthokeratology research in children (LORIC) in Hong Kong: a pilot study on refractive changes and myopia control. Curr Eye Res. 2005 Jan;30(1):71-80.
10. Walline JJ, Jones LA, Sinnott LT. Corneal reshaping and myopia progression. Br J Ophthalmol. 2009 Sep;93(9):1181-5.
11. Kakita T, Hiraoka T, Oshika T. Influence of overnight orthokeratology on axial length elongation in childhood myopia. Invest Ophthalmol Vis Sci. 2011 Jan;10.1167/iovs.10-5485.
12. Legerton, JA, Meyers WE. Systems and methods for the regulation of emerging myopia. U.S. Patent Application 20110153012; December 17, 2009.
13. Smith EL III, Ramamirtham R, Qiao-Grider Y, et al. Effects of foveal ablation on emmetropization and form-deprivation myopia. Invest Ophthalmol Vis Sci. 2007 Sep;48(9):3914-22.
14. Sankaridurg P, Donovan L, Varnas S, et al. Spectacle lenses designed to reduce progression of myopia: 12-month results. Optom Vis Sci. 2010 Sep;87(9):631-41.
15. Sankaridurg P, Holden B, Smith E, et al. Decrease in rate of myopia progression with a contact lens designed to reduce relative peripheral hyperopia: one-year results. Invest Ophthalmol Vis Sci. 2011 Dec 9;52(13):9362-7.
16. Walline J, Mutti D, Smith E. Competing theories on myopia control. Presented at the Global Lens Specialty Symposium, Las Vegas, Nevada.
17. Smith EL. Prentice Award Lecture 2010: a case for peripheral optical treatment strategies for myopia. Optom Vis Sci. 2011 Sep;88(9):1029-44.
18. Aller T. Myopia progression control using bifocal contact lenses. U.S. Patent 6752499; June 22, 2004.
19. Smith EL III, Greeman N Jr, Ho A, Holden BA. Methods and apparatuses for altering curvature of field and positions of peripheral off axis focal positions. U.S. Patent 7025460 B2; April 11, 2006.
20. Legerton J. Method and apparatus for reducing or eliminating the progression of myopia. U.S. Patent 7401922; July 22, 2008.
21. Phillips JR. Contact lens and method for prevention of myopia progression. U.S. Patent 7997725; August 16, 2011.
22. Jones LA, Sinnott LT, Mutti DO, et al. Parental history of myopia, sports and outdoor activities, and future myopia. Invest Ophthalmol Vis Sci. 2007 Aug;48(8):3524-32.
23. Padmanabhan V, Shih J, Wildsoet CF. Constant light rearing disrupts compensation to imposed- but not induced-hyperopia and facilitates compensation to imposed myopia in chicks. Vision Res. 2007 Jun;47(14):1855-68.
24. Smith EL III, Hung L, Huang J. Protective effects of high ambient lighting on the development of form-deprivation myopia in rhesus monkeys. Invest Ophthalmol Vis Sci. 2012 Jan 25;53(1):421-8.
25. Mutti DO, Marks AR. Blood levels of vitamin D in teens and young adults with myopia. Optom Vis Sci. 2011 Mar;88(3):377-82.
26. Thorn F, Gwiazda J, Held R. Myopia progression is specified by a double exponential growth function. Optom Vis Sci. 2005;82:286-97.


