We are problem solvers. Some problems sneak up on us, while others we suspect but can only diagnose after extensive testing. However, presbyopia is no surprise, and is a condition that will affect everyone. Currently, one quarter of the U.S. population is on the verge or in the throws of presbyopia.1 In this article, I will draw from science and art to offer tips in managing the growing presbyopic population.
Many patients are unprepared for the focusing frustration that will inevitably befall them. This limitation can lead to contact lens dropout. It’s easier for the uninformed myopic presbyope to simply wear glasses and remove them for near tasks than to fuss with their single vision contact lenses.
So, the first step in managing the presbyopic contact lens patient is to inform them of what to expect before symptoms develop. Let them in on the secret: You have the contact lens tools to solve the problem (see “Sample Presentation to the Incipient Presbyope”)!
Thinking Ahead
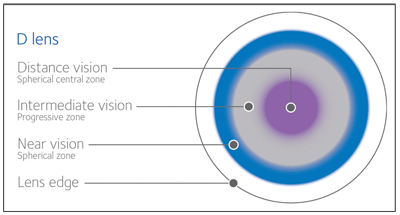
1. Biofinity multifocal D lens design.
When the day arrives that your contact lens-wearing patient presents with near symptoms, what do you do? Historically, we simply push plus in the non-dominant eye and the problem is solved. While an easy solution, this does set up both the practitioner and the patient for further problems down the line.
In these instances, when the patient returns to the office a year later, we find ourselves employing the same approach. In fact, this cycle is repeated until the patient is in full-blown monovision.
As the disparity between the eyes gradually increases, additional problems begin to arise: issues with night driving, blur at the computer distance and problems with depth perception. For example, I commonly hear patients complain about hitting their bumper when pulling into the garage. The problem here is that patients do not actively seek help until they have run into this or a similar scenario. Instead, we—as practitioners—should think ahead and think about multifocals.
Most of today’s multifocal lenses employ optics that have both distance and near light entering the pupil at the same time, known as simultaneous vision. The patient’s brain is required to choose which light to pay attention to for any given task. The greater the difference between the distance and near power, the more they compete with one another. This potential conflict means that the more advanced the presbyope is, the more challenging it will be to fit the patient with multifocal contact lenses. Patients are considerably easier to fit when they require low add powers. As they progress in presbyopia, they can be gradually eased into higher add powers over time.
The lesson here is simple: Don’t delay––fit the presbyope with a multifocal design early in the process. Today’s designs allow for very good distance vision, particularly when employing low adds. While the process may require a little more cost and effort up front, in comparison to simply adding +0.50D in the non-dominant eye, the multifocal approach is a great investment in your patient’s contact lens-wearing future.
Multifocals vs. Monovision
2. Biofinity multifocal N lens design.
Undoubtedly, some practitioners will argue that, in their clinical experience, patients prefer monovision over multifocal contact lenses. However, science tells us otherwise. Studies and surveys consistently find that seven out of 10 presbyopes prefer multifocals over monovision.2-5
This is not to say that monovision doesn’t have its benefits. In cases of advanced presbyopia, it is often necessary to introduce a bit of monovision into our multifocal approach (i.e., pushing plus in the non-dominant eye or unequal adds) to achieve the desired visual outcome.
 New Rules of the Game
New Rules of the Game
Once you have committed to fitting multifocal contact lenses as your primary form of presbyopic correction, it is imperative to begin the process by having a one-on-one session with your patient to set proper expectations. During this meeting, your goal is to explain that, while many single vision patients meet their visual needs with one or maybe two corrective tools (e.g., single vision contact lenses and perhaps a pair of back-up glasses), presbyopia is best managed by employing multiple tools.
I would recommend presenting this give-and-take mentality to the patient by using what I have dubbed the “Sandwich Approach.” The Sandwich Approach opens with a positive statement, followed by the “meat” of the message and ends with an optimistic closing statement.
• The positive opening: “I know you enjoy the many benefits of contact lenses, but have recently started to have difficulty with your close vision. I have great news. As I mentioned to you last year, we have a contact lens design that can solve your near vision problems. It’s called a multifocal contact lens.”

3. Biofinity multifocal fitting guide.
• The meat in the middle: “When correcting this problem––be it with glasses or contact lenses––there is always a bit of give and take. For example, with glasses you will need to hold your head in a particular position and look through a specific part of the lens to see clearly. With most contact lenses, you don’t have that limitation. However, you may find that in a dimly lit restaurant, you may need to hold the menu under a light or put on a pair of magnifiers in order to see adequately.”
• The optimistic ending: “Having said that, I do believe that I can meet most of your needs most of the time with multifocal contact lenses. Shall we get started?”
The Basics of Lens Selection
Virtually all of the multifocal contact lens fitting guides recommend that the distance power selection be based on the most plus power equivalent sphere refractive finding. For example, a patient with a distance refraction of -3.00-0.75 x 180, or an equivalent sphere of -3.37D, should be fit with a -3.25D lens. Don’t forget to take vertex distance into account for refractive errors over 4.00D. When refracting, take precautions against over-minusing. Pushing plus reduces the disparity between distance and near powers, making it easier for the brain to adapt to multifocal optics.
What about the add power? Add power is selected based on the manufacturer’s fitting guide. The fitting guides are based on the spectacle add. As with the distance Rx, when determining the add, you should give the patient just enough power to provide clear near vision, but no more. Keep the interval between distance and near power as tight as possible.
Perhaps the most common mistake practitioners make when fitting multifocal contact lenses is to deviate from the fitting guide. These guides have been developed based on the manufacturer’s experience with hundreds of patients during clinical studies undertaken during design development. Take advantage of this experience and follow the guide.
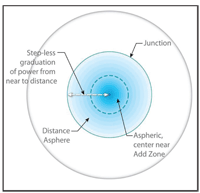
4. Optics of the Duette Multifocal.
Adjusting the Fitting Guide
Several manufacturers have recently updated their fitting guides in response to additional data gathered since releasing their lenses to the market.
• Bausch + Lomb has updated its fitting guide for both the PureVision multifocal lenses and its parent lens, the Soflens Multifocal. Based on years of clinical experience in the field, they have modified their recommended initial lens selection for patients with spectacle add powers of +1.50D or +1.75D. Instead of fitting a low add on one eye and a high add on the other, fit both eyes with high adds, but add -0.25D or -0.50D to the distance power, if needed, to enhance distance vision.
• Ciba Vision’s Air Optix Multifocal fitting guide has also been recently revised. Rather than prescribing unequal adds during initial lens selection for the +1.75D and +2.00D spectacle add patient, it now recommends that equal add powers be selected in all add ranges.
• CooperVision released its Biofinity Multifocal on June 15. This lens employs the same optical approach found in CooperVision’s Proclear and Frequency 55 Multifocal designs. The “D” lens has a central spherical zone dedicated to distance vision, surrounded by a progressive intermediate zone with an outer spherical zone dedicated to near vision (figure 1). The “N” lens has the optics inverted: a central near zone surrounded by a progressive intermediate zone, but an outer zone dedicated to distance vision (figure 2).
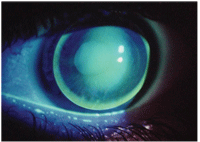
5. High eccentricity posterior aspheric GP multifocal.
The Biofinity Multifocal is CooperVision’s first foray into the silicone hydrogel market with a multifocal design. The comfilcon A material is the same one used in the spherical and toric Biofinity products.Like Bausch + Lomb and Ciba Vision, CooperVision has analyzed lens performance and modified its fitting guide. Recognizing that many practitioners have had success fitting low add patients with a “D” design in each eye, the fitting guide now recommends this approach be employed when fitting patients with adds up to +1.50D. Those patients with higher add requirements should be fit with an “N” lens on the non-dominant eye (figure 3).
Picking the Right Lens
• Hybrid multifocal lenses: SynergEyes recently released its Duette Multifocal hybrid lens. As with the Duette single vision lens, the Duette Multifocal is made of a UV-blocking 130Dk rigid center with a 32% H2O2 content silicone hydrogel skirt.
The optics of the Duette Multifocal is significantly different from the original SynergEyes Multifocal. An aspheric center near add zone is surrounded by a seamless aspheric distance zone, which SynergEyes describes as a “step-less graduation of power from near to distance” (figure 4). Uniquely, this progressive optical design negates the need to select an add power. Two add zone sizes (small and large) are available, with a difference of 0.3mm between them.
To fit the Duette Multifocal, follow the same guidelines employed when fitting the Duette single vision lens with the additional step of determining the add zone size.
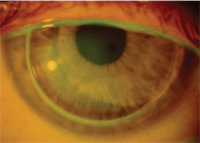
6. Front surface aspheric GP multifocal.
Once optimal movement and centration is achieved by selecting the appropriate base and skirt curves, place a small add lens on one eye and a large add lens on the other eye.
The high depth of focus provided by the aspheric optics requires certain precautions be taken to avoid over-minusing the patient. Perform a monocular over-refraction, noting best-corrected vision acuity (BVA) at distance. Then fog the patient by +1.50D. Slowly add minus to the over-refraction until the patient is able to read one or two letters on their BVA line. Then, add -0.50D for your final endpoint.
Add zone diameter is determined by which size provides the best balance of vision at distance, intermediate and near.
• Gas-permeable multifocals: GP multifocal designs have been trending toward moving more of the multifocal optics from the back surface of the lens to the front surface. Early GP multifocal designs were fabricated with a highly eccentric posterior surface, requiring them to be fit up to 4D steeper than K in some cases (figure 5). This extremely steep fitting approach often resulted in corneal shape changes that led to spectacle blur.
Subsequent designs allowed for a more aligned fitting approach, but corneal topographic changes continue to cause spectacle blur in some patients.6
• Front surface add designs: The development of lathes that allow for controlled manipulation of the anterior lens surface has led to the emergence of front surface multifocal designs. The beauty of these designs, in addition to reducing problems with spectacle blur, is the relative ease it affords when switching patients already adapted to spherical, single vision GP lenses into a multifocal. The key to success with these designs is excellent centration (figure 6). If a patient’s eye/lid anatomy results in a consistently high riding lens, pursue a design that employs a lid attachment approach.
• Combination designs: Manufacturing advances also have allowed for some multifocal designs to employ both the front and back lens surfaces to create the desired add power. When combined with the ability to create these curves in a wide array of zone sizes, GP multifocals can be customized to meet most individual patient requirements.
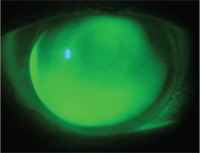
7. LASIK Near multifocal on a post-LASIK patient.
The Astigmatic Patient
Presbyopic patients with corneal astigmatism matching their vertexed spectacle cylinder are well served by GP and hybrid multifocals. The optics in these lenses can deliver impressive results.
Presbyopes with internal astigmatism are less straightforward. Some patients do quite well with toric soft multifocal designs; those who don’t are left with the option of soft toric lenses fit in a monovision modality or soft toric lenses for distance O.U., wearing readers over the lenses for near tasks.
The Post-LASIK Patient
Since its approval in 1995, more than 12 million patients have had LASIK.7 Many of these patients are now among those transitioning into presbyopia and are resistant to return to spectacle wear in order to obtain clear near vision.
Good visual performance can be elusive when fitting soft lenses on post-LASIK patients. Even with well-centered ablations, I have found the highly modified corneal shape can lead to unpredictable lens flexure and/or creation of a tear lens. To compensate for these changes, the patient may require a contact lens power that is quite different from that predicted by their spectacle refraction. Consider fitting any post-LASIK presbyope first with a single vision lens of the same material you plan to use in a multifocal design. This will give you a good starting point for distance power prior to complicating the analysis by introducing multifocal optics.
A reverse geometry GP lens can often provide good vision and fit performance on a post-LASIK patient.8 At least one lens design, LASIK Near (Valley Contax Inc.), offers a reverse geometry posterior lens surface to fit ablated corneas and an aspheric anterior surface for multifocal correction (figure 7).
A Final Word
Expectation setting is so important in the multifocal contact lens fitting process. It is advantageous to both open and close the fitting process by employing techniques that help the patient know what to expect.
At the multifocal lens-dispensing visit, consider sharing the following thoughts:
•Light is your friend. You will always see better in good light. If you don’t tell your patient this fact at the dispensing visit, they will be the one to tell you at their first follow-up visit. Instead, let them know you are aware of this and prepare them for it.
• These lenses are designed to work together. Binocular performance with multifocal contact lenses always outshines monocular performance. Remember to share this fact with your patient as you discourage comparing each eye’s individual performance.
In cases where unequal adds are needed to meet the visual needs of the more advanced presbyope, tell the patient that the vision will be different between each eye as you emphasize binocular viewing. Again, if you don’t tell the patient, this difference will be among the first things they will tell you upon their return.
• Fitting multifocal contact lenses is a process. Sometimes the first multifocal design selected does the trick, while at other times a slight modification is necessary to meet the visual needs of the patient. I tell patients that multifocal lenses are wonderful, sophisticated devices. However, the variables—such as pupil size, working distance, habitual light levels and the detail of the tasks they need to perform—can all impact which lens is needed. All this can only be sorted out by having the patient wear their multifocal lenses in their day-to-day environment.
So, it may take a few adjustments to get where we want to go. Just remember to prepare the patients upfront, which will ultimately allow you to maintain their confidence in your ability to ultimately achieve success.
Today’s changing patient demographics have created an urgency for us, as practitioners, to master both the science and the art of multifocal contact lens fitting. Familiarize yourself with the modern multifocal lenses we have within our reach and present them in a realistic light. Fit them early and according to the manufacturer’s fitting guides. Remember to adopt an attitude of empathy, support and patience. Then, sit back and reap the rewards of success as you find yourself meeting the needs of your presbyopic patients.
Dr. Thomas Quinn, a graduate of the Ohio State University, runs a practice in Athens, Ohio. He serves on the American Optometric Association’s Contact Lens and Cornea Section council and is an American Academy.fellow and diplomate of the cornea and contact lens section.
1. Studebaker J. Soft Multifocals: Practice Growth Opportunity. CL Spectrum. 2009 Jun. Available at:
www.clspectrum.com/article.aspx?article=103013 (accessed July 2011).
2. Situ P, Du Toit R, Fonn D, Simpson T. Successful monovision contact lens wearers refitted with bifocal contact lenses. Eye Contact Lens. 2003 Jul;29(3):181-4.
3. Richdale K, Mitchell GL, Zadnik K. Comparison of multifocal and monovision soft contact lens corrections in patients with low-astigmatic presbyopia. Optom Vis Stci. 2006 May; 83(5):266-73.
4. Johnson J, Bennett ES, Henry VA, et al. Multivision vs Monovision: A Comparative Study. Presented at the Annual Meeting of the Contact lens Association of Ophthalmologists, Las Vegas; February 2000.
5. Rajagopalan AS, Bennett ES, Lakshminarayanan V. Visual performance of subjects wearing presbyopic contact lenses. Optom Vis Sci. 2006 Aug;83(8):611-5.
6. Benoit, DP. Evolution of a GP multifocal. CL Spectrum. 2002 Oct. Available at:
www.clspectrum.com/article.aspx?article=12227 (accessed July 2011).
7. Feder BJ. As economy slows, so do laser eye surgeries. The New York Times. Apr 24, 2008. Available at:
www.nytimes.com/2008/04/24/business/24lasik.html (accessed July 2011).
8. Yu JU. Fitting Contact Lenses Post-LASIK. CL Spectrum. 2009 Nov. Available at:
www.clspectrum.com/article.aspx?article=103603 (accessed July 2011).


