 Scleral lenses have allowed a number of our irregular cornea patients to see the world in a manner that may have previously been impossible. Because these lenses vault the cornea, they create a wholly new refractive surface—freeing the clinician from the constraints of the patient’s corneal anatomy. Scleral lenses also provide a stable visual experience; unlike traditional small-diameter GP lenses, they do not move with each blink.
Scleral lenses have allowed a number of our irregular cornea patients to see the world in a manner that may have previously been impossible. Because these lenses vault the cornea, they create a wholly new refractive surface—freeing the clinician from the constraints of the patient’s corneal anatomy. Scleral lenses also provide a stable visual experience; unlike traditional small-diameter GP lenses, they do not move with each blink.
We have used sclerals on a number of normal corneas and have prevented patients from dropping out of lens wear. Patients with high levels of ametropia (specifically those with high levels of astigmatism), who are dissatisfied with the stability of their vision, have done quite well with this design. We have also used this modality to allow patients to re-enter lens wear following years of discontinuation.
But, as with any lens choice, we must consider the disadvantages of the modality along with its advantages so that we can exercise caution when prescribing these lenses. Because this lens is meant to clear the cornea entirely, an ideal fit must provide both adequate central and limbal clearance.
|

| |
|
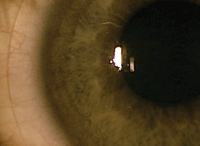
Fig. 1. The ideal lens/eye relationship. Also shown is a schematic showing an ideal scleral landing zone relationship with the eye.
| ||
As a result, the lens should rest solely on the conjunctiva and underlying sclera via its scleral landing zone. It is thus critical to respect the interaction between the lens and the conjunctiva—that may very well be what makes the difference between a successful and an unsuccessful fit.
A Perfect Fit
To achieve the ideal fitting relationship, the landing zone must be parallel to the conjunctival surface. This distributes the weight of the lens evenly across a large surface, reducing the burden on smaller areas of conjunctiva (Figure 1).
The challenge arises when the landing zone is not parallel to the conjunctiva, as this concentrates additional pressure upon localized areas of tissue. This produces excessive stress on those ‘hot spots,’ kicking off a familiar chain of events that we know all too well—discomfort » dissatisfaction » dropout.
To avoid this, we must address two clinical challenges when fitting scleral lenses: landing zone impingement and compression.
 |
|
|
|
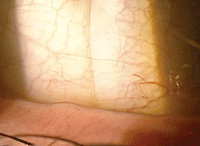
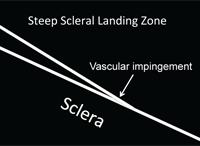
Fig. 2. A clinical photo of impingement. Also shown is a schematic showing a scleral landing zone that is causing impingement.
|
||
Using a slit lamp, you can see the pressure that the lens is placing on the conjunctiva. It will be revealed by the appearance of conjunctival blanching under and adjacent to the edge of the lens, at the distal portion of the landing zone (Figure 2).
This complication is a direct result of the scleral landing zone of the lens being steeper than the scleral profile. To resolve this particular challenge, flatten the scleral landing zone. This will allow the lens to more evenly distribute its weight over the conjunctiva, which in turn reduces the localized pressure that causes the conjunctival blanching beneath the edge of the lens.
Because of the obvious pressure on the vascular supply in the underlying conjunctiva, it is important to resolve this fitting challenge as soon as it’s seen. Additionally, these patients typically experience significantly higher amounts of debris and clouding under the lens than normal and, as such, require more frequent removal and rinsing of the lens.
Compression results when the proximal portion of the lens’s landing zone produces excessive pressure on the bulbar conjunctiva. When initially placed on the eye, patients may experience significant lens awareness; however, this will decrease as the lens settles on the eye.
|

| |
|
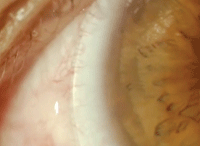
Fig. 3. A clinical photo of compression. Also shown is a schematic showing a scleral landing zone that is causing compression.
| ||
Compression may also result in bulbar hyperemia due to the area of excessive pressure.
As with impingement, this too can be seen at the slit lamp. The appearance of conjunctival blanching in an area under the proximal scleral landing zone is a clear sign of compression (Figure 3).
In effect, compression is the converse of impingement: when the scleral landing zone is flatter than the scleral profile, compression results; if the landing is steeper, impingement does. So, it should come as no surprise that the approach to resolution of compression is the opposite of that needed for impingement: steepen the scleral landing zone to achieve a more even lens distribution over the conjunctiva.
It is important to keep these considerations in mind when designing scleral lenses for patients, as it will help to ensure the best possible fit, comfort and visual outcome.
These strategies help provide those patients who would benefit from this design the greatest chance of doing so, and will also help to keep individuals in contact lenses who may have otherwise considered discontinuing lens wear. Ensuring your patients are experiencing an ideal lens-to-eye relationship will ultimately help derail dropouts.


