 |
A 53-year-old white male presented with a long history of slowly increasing astigmatism in both eyes. He denied pain or redness but stated his glasses were no longer working for him.
His exam revealed 360 degrees of peripheral stromal thinning with corneal neovascularization and lipid at the leading edge. The conjunctiva/sclera was white and quiet.
He had a manifest refraction of -2.00 +5.50 x 180 OD and -3.00 +6.00 x 180 OS, yielding 20/20 vision in each eye.
Based on these findings, he was diagnosed with Terrien’s marginal degeneration (TMD), given a new prescription, counseled on the progressive nature of the disease and cautioned to wear glasses or eye protection at all times to avoid the risk of accidental perforation.
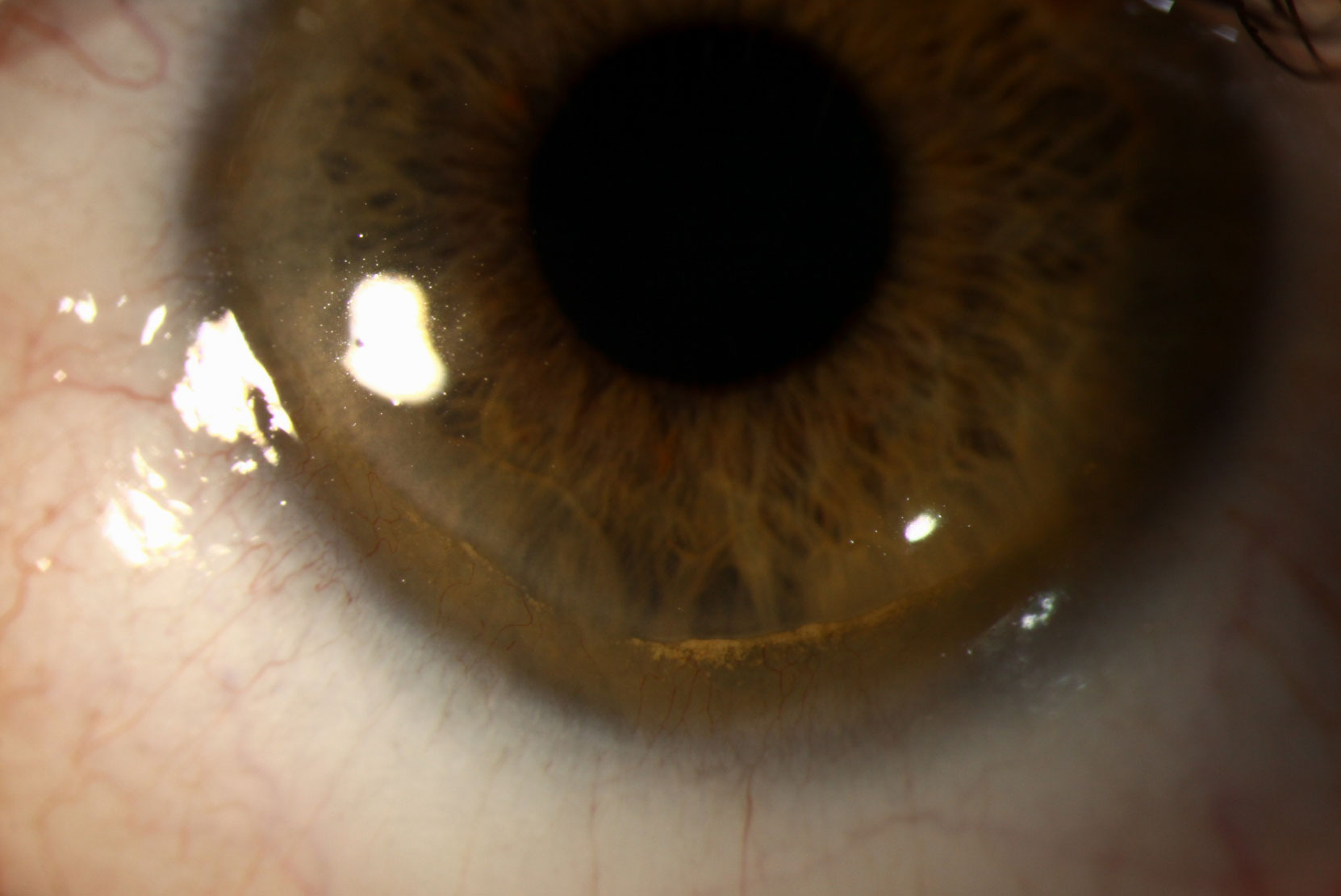 |
| Click image to enlarge. |
Disease Basics
TMD is a non-inflammatory condition that causes thinning of the peripheral/limbal cornea. It typically begins on the superior cornea and advances circumferentially. Opacification and lipid deposits form at the edge of the thinned area, and lacy pannus vessels form throughout it. While punctate epithelial erosion is possible, the epithelium generally appears intact. Spontaneous perforations are rare; however, Descemet’s membrane may rupture and cause intracorneal swelling. Progressive, high against-the-rule astigmatism is a classic refractive finding in TMD.
The condition can be differentiated from other corneal thinning disorders such as pellucid marginal degeneration (PMD) based on the location of the thinning. For TMD, thinning starts superiorly and rarely involves the inferior limbus. PMD thinning, however, starts inferiorly and only involves the cornea within 1mm to 2mm of the inferior limbus.
A complete differential diagnosis includes: dellen, collagen vascular disease, sclerokeratitis, dry eye, staphylococcal marginal keratitis and infectious corneal ulcer.
Maintaining Vision
Patients should be cautioned about the risk of traumatic perforation and given protective eyewear. Scleral lenses may be indicated if vision does not improve with glasses.


