For years, practitioners have known that thicker soft lenses have the ability to mask some corneal astigmatism. While lenses made from stiffer materials than HEMA-based hydrogels (e.g., the CSI lens of the past or first-generation silicone hydrogels with a high modulus of elasticity) may work for patients with low corneal astigmatism, they rarely were successful for any patient manifesting significant amounts of astigmatism, irregular astigmatism or keratoconus.
To manage keratoconus, practitioners have tried using toric soft lenses. But, exempting patients in the early stages of disease, the results generally have been poor. The mainstay of keratoconus management has thus been through the use of rigid gas-permeable (GP) lenses, which provide outstanding vision. But keratoconic patients consistently reveal that the discomfort with GP lenses––although tolerated––is a significant detriment to quality of life.
Piggyback systems, as well as the hybrid-type lenses that combine a rigid lens center with a soft periphery (e.g., SynergEyes’ ClearKone or SynergEyes KC), can improve comfort, although to varying degrees. While both are helpful in improving vision and comfort, the hybrid lenses may result in tighter fits despite our best efforts, which sometimes can facilitate the development of corneal neovascularization.
Wouldn’t it be nice to have a single, non-hybrid soft lens that could provide improved comfort over the above-mentioned modalities and still correct the patient’s vision to a degree competitive with GP lenses? Let’s look at several lenses that strive to play this role.
Flexlens Tri-curve Keratoconus and Flexlens Piggyback
To address the need for significantly increased lens thickness, Flexlens Tri-curve Keratoconus (X-Cel Contacts) is a hydrogel lens that has been available for several years. The lens is available in both 49% or 59% water hioxifilcon, in 55% methalfilcon and, more recently, in the newest customizable Definitive material by Contamac (60Dk, 74% silicone hydrogel) to offset the reduced oxygen transmission associated with thick hydrogels.
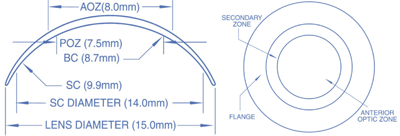
1. Flexlens Tri-curve lens for keratoconus.
The Tri-curve lens incorporates two peripheral curves and has a center thickness ranging from 0.40mm to 0.65mm thick (figure 1). A flat secondary curve (1.2mm to 1.8mm) and a peripheral scleral curve (2.2mm to 2.8mm) are used to aid alignment. Toric powers have not yet been offered with this lens design.
These lenses are best for keratoconic patients with moderate amounts of irregular astigmatism. Patients with significant residual astigmatism, however, will still need a piggyback design.
The Flexlens Piggyback design uses a soft lens with a central cut-out depression to keep a GP lens securely centered over the cornea. This is a notable advantage over other piggyback systems in which GP lenses ride low (figure 2). A wide range of parameters for the soft lens base and the anterior cut-out are available to accommodate GP lenses of varying diameters. The soft lens base is now available as a monthly replacement lens.
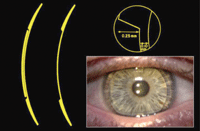
2. FlexLens piggyback lens with cut-out. Note good centration of GP over pupil zone.
NovaKone
NovaKone (Alden Optical) is a relatively new lens that uses increased thickness as a tool to control corneal irregularity. The optical zone of this soft lens functions much like a GP, which helps to neutralize irregular corneal astigmatism. The big advantage, however, is that it also allows for the essential correction of residual astigmatism. Rotational stability for the toric application comes from the company’s dual elliptical stabilization design (see figure 3 and table 1).
The lens is made of Benz G4X 54% hioxifilcon D and comes in a standard 15.0mm diameter. An 18-lens diagnostic set, which contains a wide range of base curves and fitting curves (flatter curves for the corneal regions outside of the cone), is necessary to fit this lens. These lenses contain significant amounts of minus power and varying thicknesses.
Thickness control with the NovaKone lens is critical to its success. It is designated as the “IT factor,” which stands for increased thickness, and ranges from thinnest (0) to thickest (4) in incremental steps. Steeper curves for advanced cones are naturally provided in the diagnostic set, along with several IT factors to help correct the irregular corneal astigmatism. This is gauged not only by the level of visual acuity obtained through spherocylindrical over-refraction (SCOR) performed during the spherical test lens, but also by assessing the quality of the front surface of the lens with an “over-K” measurement. As long as the clinician observes good quality of the over-K mires with the test lens (despite the amount of astigmatism measured), we know that the test lens has achieved regular astigmatism and a SCOR should result in good visual acuity.
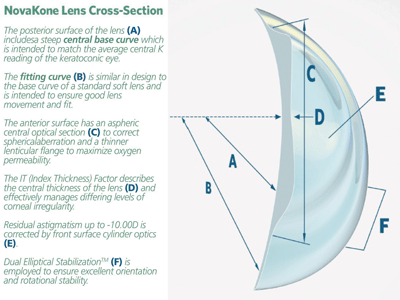
3. NovaKone uses increased thickness as a tool to control corneal irregularity.
This astigmatism is then incorporated into the rotationally stabilized toric lens design. (Be sure to compensate for rotation as you would normally do with any toric lens, assuming good lens movement and centration is observed.) There are two laser marks on the lens’s horizontal axis that aid in toric rotational measurement. You may have to repeat this process with more than one IT factor to determine the best lens. It is not uncommon to find that higher IT factors can achieve better acuity with less additional toric refractive correction. That said, the clinician should still attempt to use the lowest level of IT thickness that produces a satisfactory visual outcome.
The fitting technique is a four-step process, from the inside out:
1. Determine the central base curve. Use the supplied initial lens selection table that recommends the base curve/fitting curve combination based on average Ks (or Sim Ks if using topography) for the central 3mm to 4mm zone. This test lens is applied, filled with high molecular weight fluorescein, and evaluated to achieve an acceptable lens that demonstrates neither excessive bearing over the cone nor excessive apical clearance (figure 4).
2. Determine lens thickness (IT factor). Use the lowest IT factor that produces regular mires verified by over-keratometry or topography. If irregularity is observed, switch to a higher IT factor. (Smaller, central cones usually can be treated successfully with lower IT factors, while larger, decentered cones will often require much higher IT factors.)
3. Determine the total lens power needed. Compensate for vertex distance, as well as rotation, when adding the SCOR to your spherical test lens.
4. Determine the para-central fitting curve. Typical soft lens fitting characteristics should be observed. Excessive lens movement or edge lift requires use of a steeper fitting curve, while little to no movement or edge impingement requires a change to a flatter fitting curve.
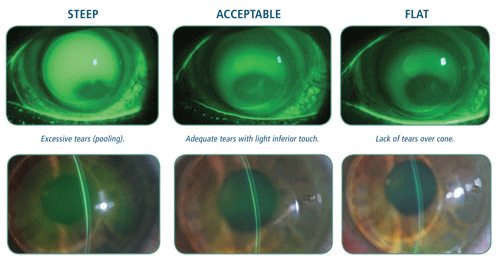
4. Fitting evaluation of NovaKone using high molecular weight sodium fluorescein.
Kerasoft IC
The Kerasoft IC is distributed through Bausch + Lomb and several authorized manufacturing labs, such as ABB Concise, Art Optical and Metro Optics. These lenses are used for all stages of keratoconus, pellucid marginal degeneration, post-LASIK ectasia and other irregular astigmatic conditions.
Practitioners who want to fit either the NovaKone or Kerasoft IC must first complete the online certification process.
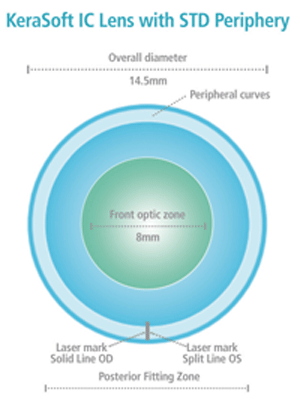
5. Kerasoft IC lens.
The aspheric Kerasoft IC lens is made from Definitive silicone hydrogel material (74% water, 60Dk) that is designed for quarterly replacement. Fitting employs an eight-lens diagnostic set, with standard 14.5mm diameter (others available), plano power and a range of base curves (7.80mm to 8.60mm, with others available). Most lenses in the set have a standard periphery, but the flatter base curves also include lenses with flat and steep peripheries for unusual fitting circumstances. It is a lean set, but one that is very useful in its intelligent design. Powers are available from +20.00D to -20.00D, with cylinder from 0.50D to 12.00D in 0.25D increments at any axis (figures 5 and 6).
The fitting process with the Kerasoft IC follows a rigid protocol, known as the MoRoCCo VA system. Initial lens design for keratoconus involves first looking at the patient’s corneal shape, which can vary from steep central cones to low, decentered cones that require different base curves––depending on the severity of the cone. Pellucid corneas often need flatter base curves, and may require additional peripheral modification of the flat superior and steep inferior zones. Post-surgical corneas will need steeper peripheries. Use of the “corneal shape recognition” and “profile” charts can help select an initial lens for evaluation.
The MoRoCCo VA system is then employed for the fitting assessment, as follows:
• Mo (Movement) is evaluated, and up to 2mm of movement is acceptable as long as the patient is comfortable. Change the base curve radius if movement is greater than 2mm or less than 1mm, or if the patient is uncomfortable. (Be prepared to see more movement with soft keratoconic lenses than you would otherwise observe with conventional soft lenses. Increased patient comfort comes with adaptation, so patient education is important here.)
• Ro (Rotation) is assessed using the vertical laser mark, which should be at six o’clock, stable, with up to 10º of acceptable rotation. Rotation will need to be compensated. A slightly flatter base curve may improve the stability, but unstable rotation is caused by a flat fit. Stable but greater than 10º rotation implies a tight fit and the base curve should then be flattened.
• C ( Centration) should be good, but a minimal amount of decentration is acceptable if acuity is stable and clear. If vision improves immediately after the blink, then there is a tight fit. Lateral decentration with a drop on up-gaze indicates a flat fit.
Centration) should be good, but a minimal amount of decentration is acceptable if acuity is stable and clear. If vision improves immediately after the blink, then there is a tight fit. Lateral decentration with a drop on up-gaze indicates a flat fit.
• Co (Comfort) should be good, but if persistent edge awareness exists, try a steeper base curve. If there is discomfort and the lens is stationary, the lens likely is tight.
• VA (Visual Acuity) should be stable, without fluctuation between blinks. If the vision is worse after the blink, it is likely due to a flat fit. If it is clearer after the blink, a steep fit is likely. If acuity cannot be achieved after the above adjustments, this may be due to a very flat peripheral cornea. Peripheral modification may be needed, or the lens design discontinued in favor of other lens options.
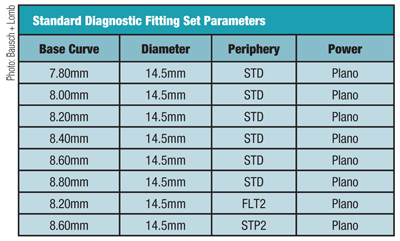

6. Eight-lens Kerasoft IC fitting set.
The periphery of the Kerasoft IC is unique in that it can be steepened or flattened, independent of the base curve. This customizable process is known as sector management control (SMC). Up to two sectors in the periphery can be modified when necessary, such as with post-graft corneas that require flatter base curves but need peripheral steepening. Also, low cones and PMD corneas may require SMC steepening of the inferior sector and possibly flattening of the superior sector. Lens sector angles (quadrants) are designated and specified as either STD or STP 1-4 or FLT 1-4 (figure 7).
The use of these new, specialized soft lens designs for keratoconus can be very rewarding. They give practitioners the ability to improve visual acuity for patients with irregular astigmatism or irregular corneal profiles that is on par with GP lenses, but with improved comfort. Good lens movement and the use of silicone hydrogel materials provide these corneas with improved metabolism, free of the risks of vascularization sometimes seen with tighter hybrid designs.
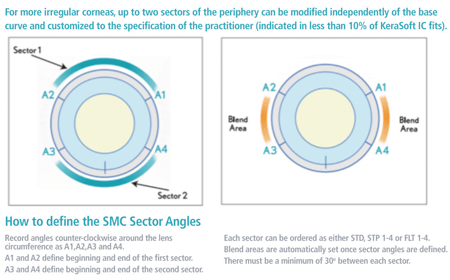
7. Kerasoft IC sector management control (SMC).
Whether using these new soft lens modalities or using scleral lenses (which also provide good acuity and comfort), the clinician now has powerful tools that can better serve these patients. Considerable time is needed to work with these patients, so schedule your appointments accordingly. And, remember to fit each lens individually, per eye.
Dr. Silbert is professor of optometry at the Pennsylvania College of Optometry at Salus University and the director of Contact Lens Programs. He is also the director of the Cornea and Specialty Contact Lens Service at The Eye Institute of Salus University. In addition to being a diplomate of the Cornea, Contact Lens and Refractive Technology Section of the American Academy of Optometry, a charter member of the Cornea & Contact Lens Section of the American Optometric Association and a former chair of the Association of Contact Lens Educators, Dr. Silbert was the principal investigator of the NIH-funded CLEK Study at PCO-Salus.


