 The last decade has brought a shift in the thinking of many contact lens practitioners. Ten years ago, gas-permeable lenses that landed beyond the limbus were an uncommonly used, and often unsuccessful, means of correction. Today, those same lenses are the first choice for a majority of GP lens wearers.
The last decade has brought a shift in the thinking of many contact lens practitioners. Ten years ago, gas-permeable lenses that landed beyond the limbus were an uncommonly used, and often unsuccessful, means of correction. Today, those same lenses are the first choice for a majority of GP lens wearers.
Is it time to replace our corneal GP lenses with corneoscleral, mini-scleral and scleral lenses?
A Case Study
RH, a 59-year-old white male, arrived at our office for a comprehensive eye exam and contact lens evaluation. He was referred by his wife, a long-time patient who was fit in 14.0mm corneoscleral lenses a few years prior. She had been so pleased with her lens experience that she recommended RH also be fitted in corneoscleral lenses instead of the toric GP lenses he had worn for the past 30 years.
RH presented wearing his monovision toric GP lenses—right eye for near and left eye for distance. He thought he needed an updated prescription and said that while he tolerated his GP lenses, his eyes were dry and that he used artificial tears a few times each day. His lenses were obtained elsewhere and the parameters were not known.
Visual acuity with his current GP lenses was 20/30 OD at near and 20/20-1 OS at distance. The fit of the lenses was acceptable and an over-refraction revealed mild astigmatism over each lens. The lenses were removed and refraction was calculated: -10.00 +3.75 x 117 OD and -9.75 +2.50 x87 OS, both to 20/20 vision. A slit lamp exam revealed mild conjunctival injection and limbal staining OU. All other exam findings were normal.
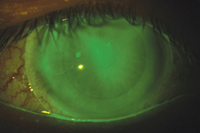
1. A SoClear corneoscleral lens OD at the dispensing visit.
We discussed the options, including staying with his current lenses or perhaps reordering them with a slight update to the prescription to better correct the astigmatism. We also discussed going to a corneoscleral or mini-scleral lens, both with and without a multifocal, as opposed to staying with monovision. Ultimately, RH opted to try the corneoscleral lenses with monovision correction.
A fitting was performed on each eye with the SoClear (Dakota Sciences) standard design lens. After trying a few lenses on each eye, a final order was placed with these parameters: 43.50mm base curve, -7.00D power, 14.2mm diameter, 0.5D steep peripheral curves and 0.33mm minimum center thickness with no fenestration OD; 44.00mm base curve, -7.75D power, 14.2mm diameter, standard peripheral curves and 0.24 minimum center thickness, with no fenestration OS.
RH returned for a dispensing visit three weeks later. The lenses were applied to the eyes and allowed to settle. Acuity measured 20/20 OD at near and 20/30+ 1 OS at distance. An over-refraction of -0.50 OS improved the left eye vision to 20/20 and a new lens was ordered. The fit looked as expected (figures 1 and 2). We dispensed the lenses and instructed the patient to begin using the new left lens upon arrival, and to return for a check-up a few weeks later.
RH returned three weeks later for follow-up. He reported improved comfort and night vision over his old GP lenses. His vision with the new lenses was 20/25 at near OD at near and 20/20 OS at distance. An over-refraction demonstrated more plus acceptance for near OD and plano at distance OS. After discussing the option of adjusting the right lens for near at the risk of losing range, RH opted to keep the current specifications.

2. A SoClear corneoscleral lens OS at the dispensing visit.
This case highlights the importance of specifying center thickness in our larger diameter lens patients. Traditionally, the lab determined this parameter. However, patients with higher degrees of astigmatism, particularly when it is regular in nature, will often need lens center thicknesses of 0.30 or greater; this increase in thickness almost never affects comfort, but does aid visual quality. I always specify center thickness on all my corneo-scleral and scleral lens orders so that I can optimize vision. In the case of RH, the right eye had more astigmatism, and therefore required a thicker lens to mask that cylinder.
Note: Because the number of practitioners that use these larger diameter designs is still relatively small, happy scleral and corneoscleral wearers (word-of-mouth referrals are key!) will tend to funnel patients your way, further building your specialty practice.
Larger diameter GP lenses can often provide better comfort, more stability and similar visual acuity as their corneal GP counterparts. While not always the solution, the use of corneoscleral, mini-scleral and scleral GP lenses is expected to rise and may eventually become the preferred mode of correction for the majority of individuals using GP lenses. In addition to our irregular cornea patients, we should consider individuals with specific visual demands or corneal configurations for larger diameter GP lenses.


