 Although soft contact lenses have eclipsed gas permeables in popularity and in the public consciousness, over three million people in the United States alone currently wear GP lenses.1
Although soft contact lenses have eclipsed gas permeables in popularity and in the public consciousness, over three million people in the United States alone currently wear GP lenses.1
It is a modality with many unique strengths that, when paired with the proper encouragement, stands to gain rather than diminish in prominence. GP lenses provide crisp, clear vision for a wider variety of patients than do soft lenses. Advances with newer, larger diameter designs have significantly improved lens comfort and stability.
These improvements have given practitioners the opportunity to select a GP lens option as the first choice for many contact lens patients.
However, to set the stage for success, it is important to discuss some common concerns that patients may report—or, worse, not report to you but worry about nonetheless.
1. Comfort
“My friend tried hard contact lenses and they said they hurt. A lot.”
One of the main reasons GP lenses are not commonly prescribed or worn is their reputation for discomfort. Practitioners and patients alike tend to share the same fear that reduced comfort will lead to patient dissatisfaction with the experience.
Prospective contact lens patients may have asked their friends and family about the different contact lenses they have used in the past. It is not uncommon for patients to request a type of lens recommended by someone they know and trust.
Patients especially tend to remember which lenses they do not want to try; unfortunately, GP lenses get a bad rap for discomfort.
One of the best ways to reduce discomfort is to use anesthesia when fitting GP lenses by instilling one drop of topical anesthetic before applying the lens to the eye.
Using this technique, many patients are often so impressed with the vision achieved with their new lens that the feeling of lens awareness becomes less of an issue.2
It is important to inform the patient that the lens will not feel quite as good as the initial dispensing, and their eyes will get used to this type of lens the more often they wear it.
Another way to increase the comfort of GP lenses is the use of topical nonsteroidal anti-inflammatory drops. NSAIDs reduce prostaglandins, which effectively reduces pain.6,7
A typical dosing regimen involves instilling one drop of NSAID 30 minutes, 15 minutes and right before GP dispensing, and then one drop one hour after insertion.6 Repeat this regimen for three to five days until gas permeable lens wear adaptation is complete.7
Another useful tip is to discuss the GP wear and adaptation experience with the patient before the lens is applied to the eye, so they know exactly what to expect.
 | |
|
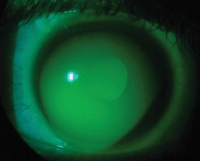
Figure 1. Corneo-scleral lens vaulting the central cornea and eliminating inferior standoff.
|
A common statement from the practitioner can be, “This type of lens will be similar to a new watch or a new ring. At first, you’ll notice it’s there, but the more and more you wear it, the less you’ll feel it. At some point, you even forget you have it on.”
Patient education is very important in the success of GP lens wearers.
“I wore hard contact lenses in 1970s and they were really uncomfortable. What’s changed since then?”
Patients that have worn “hard” lenses in the past may have been wearing PMMA or early RGP lenses, but it is hard to pinpoint exactly which type of lens they wore, as both were frequently used. Recent advances in lens materials, such as the fluorosilicone acrylates, allow much more oxygen transmissibility than previously available materials.3
GP lenses are now available in ultra-thin designs with aspheric peripheries, which aid in comfort as well.4 Be sure to inform patients that newer lens materials deliver much more oxygen to their eye, and the design of these lenses is much thinner and more comfortable than their old lenses.
2. Stability
“Sometimes when I’m riding my bike, one of my lenses pops off or feels really unstable!”
Some of the smaller, corneal GP lenses may dislodge if a patient moves their eye in an extreme left/right gaze, plays sports, etc.
Lens dislodgement can occur with some of the smaller diameter lenses, especially if there is any inferior standoff. This is especially true in GP wearers who have irregular astigmatism or more challenging fits.
If the patient wishes to remain in a corneal GP design, increasing the diameter of the lens or changing the peripheries of the lens may aid in centration.
The larger diameter lenses are much less likely to dislodge than the corneal GP lenses due to decreased lid interaction and the ability to completely vault the cornea and rest on the sclera/conjunctiva (figure 1).
Corneal-scleral, mini-scleral and scleral lens designs are great options for patients with complaints of lens dislodgment. Newer designs are becoming easier to fit, which gives the practitioner more confidence when fitting patients in GP lenses.
3. Price
“So, Doc, you’re telling me the price of one GP contact lens is $__. But I only pay $__ for a box of my current soft contact lenses. And what if I don’t like them or they don’t work?”
Another major concern for patients is the cost of GP lenses. Oftentimes, they experience sticker shock at the initial price of the lens, and typically have reservations about the success of the lens fit.
Although the initial price of GP lenses may be more expensive, the long-term cost actually can work out to be less with this modality.
Because GP lenses are far more durable and resistant to deposits than soft lenses, many patients are able to successfully wear the same pair for one year or longer. In fact, 47% of patients who wear GP lenses replace their lenses after two to three years.1
Working with a lab that has a good warranty program is essential in building trust with your GP patients.5 If patients are worried about the success of the lens—and committing their money to it—some communication of the cost should be addressed.
“I understand your concern about the cost of the lens, but this lens has a great warranty,” you might say. “We can make any changes necessary in a short period of time to get the most accurate prescription and fit. At the end of the trial period, if you still do not like the lenses, we can return them for a full or partial refund and go back to your original lenses.”
Addressing the issue of returning the lens and going back to what the patient was already wearing gives the patient more confidence in taking the leap and trying a GP lens, as there is little to no risk involved.
Practitioners should not be apprehensive about GP lenses, but we should be aware of the concerns that may arise with any type of contact lens. Knowing the pros and cons of soft, GP and hybrid lenses will allow us to make the best selection for each patient.
By addressing and managing concerns with GP lenses, most patients will be able to achieve crisp, comfortable vision while maintaining ocular health.
1. Nichols J. Contact Lenses 2012. Contact Lens Spectrum. Jan 1, 2013.
2. Bennett ES, Smythe J, Henry VA, et al. The effect of topical anesthetic use on initial patient satisfaction and overall success with rigid gas permeable contact lenses. Optom Vis Sci 1998;75:800-805.
3. Brennan NA, Efron N, Holden BA. (1986), Oxygen permeability of hard gas permeable contact lens materials. Clinical and Experimental Optometry, 69: 82–89.
4. Schnider CM. Anesthetic and RGPs: crossing the controversial line. Rev Optom 1996;133:41-43.
5. Jedlicka J. Make the most of everybody’s time. Review of Cornea and Contact Lenses. May 5, 2013.
6. Gordon A, et al. The effect of diclofenac sodium on initial adaptation to RGP lenses: a pilot study. J Am Optom Assoc. 1999:70;509-512.
7. Bennet E, et al. Clinical manual of contact lenses. Philadelphia: Lippincott Williams and Wilkins. 2009; 113-114.


