There are numerous applications for anterior segment optical coherence tomography (AS-OCT), including research and clinical applications for glaucoma, phakic IOLs, tear height, LASIK, cataract surgery, corneal transplant, pachymetry and corneal disease.1-8 AS-OCT is also used for custom design and evaluation of specialty contact lenses, especially large-diameter scleral lenses.9 Investigations of scleral shape with AS-OCT have explained how large-diameter contact lenses interact with the peripheral cornea and sclera.10,11
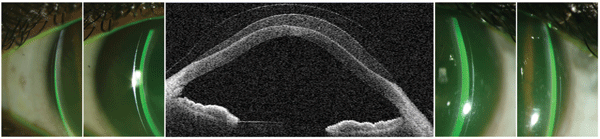
1. Horizontal AS-OCT scan with corresponding slit lamp images.
The Ideal Fit
Proper fitting of scleral lenses includes three principles: vaulting over the cornea, including the limbus (related terms are clearance, sagittal height or fluid chamber); ensuring a proper landing zone (also known as the haptic or scleral zone); and maintaining adequate tear exchange under the lens.
A well-designed lens with respect to the vault and landing zone usually will result in good tear exchange and corneal physiology. Evaluating the lens vault and landing zone is done clinically through slit lamp observation––with and without fluorescein. However, from teaching scleral lens education workshops, we know that some beginners have a very difficult time learning to estimate parameters like central and limbal corneal vault. Furthermore, manual or SIMK keratometry values are often not very useful for selecting an initial trial lens with the proper sagittal height for adequate vault during scleral lens fittings.12
Clearance, or vault, can be judged during slit lamp biomicroscopy by using the known or estimated corneal thickness and comparing that slit width to the width of the space between the lens and the cornea (figure 1). Scleral lenses typically are fit with vault equal to 25% to 100% of the corneal thickness (150µm to 600µm). The vault of a scleral lens is more dependent on the total sagittal height of the lens than the base curve, and AS-OCT is a powerful tool for calculation and observing sagittal height.11
Using the AS-OCT
While not required, correlating slit lamp observations with AS-OCT measurements can be a very valuable learning tool for the practitioner fitting specialty contact lenses. The fit relationships seen in digital images can be compared with slit lamp observations. After a few patient encounters, a novice scleral lens fitter can become very confident with judging an appropriate fit. In figure 1, the slit lamp images show that there is more corneal vault on the right side, and this is clearly the case in the horizontal scan of this severe keratoconus patient.
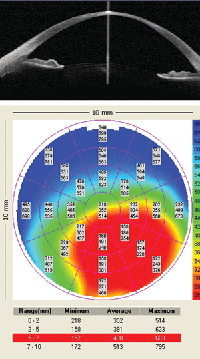
2. Visante pachymetry.
AS-OCT is especially useful for observing how parameter changes (sagittal height, base curve and diameter) affect the lens fit during a fitting or refit process. Unlike standard-size rigid gas-permeable lenses, large changes in some parameters are often required to make a significant change in the way a scleral lens fits. Caliper tools in the instrument software allow for precise eye measurements, which can then be correlated to slit lamp observations.
Even very experienced practitioners can have difficulty determining limbal clearance with the slit lamp. Human observers may not be able to detect a very thin fluorescein layer under a lens that may actually have some clearance. A scleral lens will often fit with deep (e.g., 300µm), clearance centrally, but minimal clearance or touch at the limbus. The resolution of modern AS-OCT can be as good as a few microns (see “Anterior Segment OCT Specifications”), and there are cases where imaging can confirm a patient has just enough limbal clearance to avoid starting a refit in a lens that seems to fit well otherwise.
Another use for AS-OCT is to evaluate the landing zone. Landings that are too tight or loose can result in hypoxia or bubble formation. Scleral lens design is becoming very precise and customizable with the programing capabilities of manufacturing lathes. It is now possible to design varying landing profiles in different lens quadrants. AS-OCT will likely become a very important tool in highly customizable lens designs, including custom values for corneal and limbal vault, and peripheral curve design.
Case Studies
Before fitting a diseased, traumatized or post-surgical eye, you must first conduct a very thorough evaluation of corneal integrity. AS-OCT can plot pachymetry over a large area of the cornea rather than just a single point. Here are three AS-OCT case reports:
• A 24-year-old white male presented with corneal thinning from severe atopic keratoconjunctivitis. A horizontal OCT scan and pachymetry was used to evaluate the patient (figure 2); an area of extreme thinning might alert the practitioner to arrange more frequent follow up after beginning lens wear. This patient had a remarkable improvement in acuity with a diagnostic scleral lens. However, after viewing the AS-OCT, he was concerned about his corneal health and elected not to be fit.
• A 69-year-old white male is a radiologist with a failing corneal graft. He elected to manage his failing corneal graft conservatively after AS-OCT documentation showed that scleral lens wear worsened the bullous keratopathy even though the lens fit very well (figure 3).
• Sometimes, after acute corneal hydrops, a severe keratoconus patient will have fortuitous flattening and strengthening of the cornea. A 49-year-old white female presented wearing an old, flat-fitting scleral lens at the time of acute hydrops. The AS-OCT imaging was very valuable in monitoring the healing process; she was recently refit in a new scleral lens where she achieved 20/25 acuity.
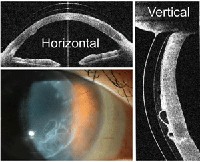
3. Epithelial bullae under scleral lens.
Digital Image Comparisons
We captured AS-OCT images for every instrument available during the Ophthalmic Photographers’ Society annual program at the American Academy of Ophthalmology meeting (see “Anterior Segment OCT Specifications”). To image a contact lens on the cornea, one individual wore a commercially available hydrogel (+13.50, 14.2mm, omafilcon A, 62% water). Images were exported from the instrument using the standard software available at the time. Some images have been minimally formatted for better side-by-side comparison. We cropped and resized in an attempt to standardize the total thickness of the cornea/soft lens, but no digital enhancements were made except some minor brightness changes. All of the six instruments we discuss have numerous scan parameters and digital output choices.
There are differences in the maximum size of the horizontal scan length for different instruments. Spectralis (Heidelberg Engineering) and Visante (Carl Zeiss Meditec) are able to capture the entire cornea and limbus in one horizontal or vertical scan of at least 15mm (figure 4). Wide scans can be useful for evaluating fit characteristics of large-diameter scleral lenses. We also imaged the edge of the soft lens and placed those scans alongside the horizontal scans. Edge design can be very important for scleral lens fitting.
The iVue (Optovue), RT-Vue (Optovue), Cirrus (Carl Zeiss Meditec) and Envisu R2300 (Bioptigen) are instruments that have smaller horizontal scan lengths. The horizontal and edge scans can still be used to image the entire cornea by making overlapping scans and stitching the images with some digital imaging software (figure 5).
Diagnosing a Poor Fit
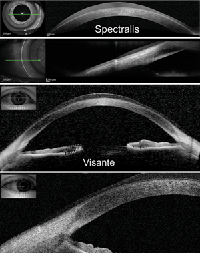
4. Large diameter scans of an individual wearing a contact lens.
AS-OCT images helped confirm that one patient’s initial 18.2mm lens did not have clearance or vault over the limbus. He developed a severe keratitis/iritis while wearing the lens. The patient was refit to a 19.0mm lens with a reverse geometry design that produced a larger sagittal depth, allowing for vaulting over the limbus that was clearly evident in the repeated AS-OCT.
Many scleral lens patients have significant eye conditions that require close monitoring, which can be done with an AS-OCT. This technology is very useful for fitting large-diameter scleral lenses, evaluating the fit and problem solving. Keep in mind that some insurance carriers will reimburse for imaging certain eye conditions using CPT code 92132: scanning computerized ophthalmic diagnostic imaging, anterior segment, with interpretation and report, unilateral or bilateral (the old 0187T code). Undoubtedly, hardware and software upgrades on current instruments and new models with advanced imaging capabilities will improve the practitioner’s ability to manage specialty contact lens patients.
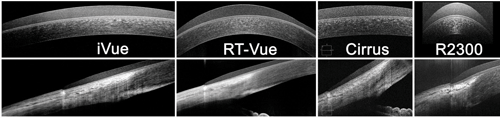
5. Smaller diameter scans of individual wearing a contact lens.
Dr. Baldwin is a clinical assistant professor at the University of North Carolina Department of Ophthalmology. He manages a specialty contact lens practice and trains optometry and ophthalmology residents and optometry externs.
Sarah Moyer is the director of ophthalmic imaging at the University of North Carolina. She is also a member of the Board of Education for the Ophthalmic Photographers’ Society and has lectured for the past several years at national OPS meetings.
1. Lee Y, Sung KR, Na JH, Sun JH. Dynamic changes in anterior segment (AS) parameters in eyes with primary angle closure (PAC) and PAC glaucoma and open-angle eyes assessed using AS optical coherence tomography. Invest Ophthalmol Vis Sci. 2012 Feb 13;53(2):693-7.
2. Güell JL, Morral M, Gris O, et al. Evaluation of Verisyse and Artiflex phakic intraocular lenses during accommodation using Visante optical coherence tomography. J Cataract Refract Surg. 2007 Aug;33(8):1398-404.
3. Czajkowski G, Kaluzny BJ, Laudencka A, et al. Tear meniscus measurement by spectral optical coherence tomography. Optom Vis Sci. 2012 Mar;89(3):336-42.
4. Hall RC, Mohamed FK, Htoon HM, et al. Laser in situ keratomileusis flap measurements: Comparison between observers and between spectral-domain and time-domain anterior segment optical coherence tomography. J Cataract Refract Surg. 2011 Mar;37(3):544-51.
5. Lyles GW, Cohen KL, Lam D. OCT-documented incision features and natural history of clear corneal incisions used for bimanual microincision cataract surgery. Cornea. 2011 Jun;30(6):681-6.
6. Moutsouris K, Dapena I, Ham L, et al. Optical coherence tomography, Scheimpflug imaging, and slit-lamp biomicroscopy in the early detection of graft detachment after Descemet membrane endothelial keratoplasty. Cornea. 2011 Dec;30(12):1369-75.
7. Ishibazawa A, Igarashi S, Hanada K, et al. Central corneal thickness measurements with Fourier-domain optical coherence tomography versus ultrasonic pachymetry and rotating Scheimpflug camera. Cornea. 2011 Jun;30(6):615-9.
8. Maeda N. Optical coherence tomography for corneal diseases. Eye Contact Lens. 2010 Sep;36(5):254-9.
9. Gemoules G. A novel method of fitting scleral lenses using high resolution optical coherence tomography. Eye Contact Lens. 2008 Mar;34(2):80-3.
10. van der Worp E. A Guide to Scleral Lens Fitting [monograph online]. Scleral Lens Education Society; 2010. Available at:
http://commons.pacificu.edu/mono/4/ (accessed March 26, 2012)
11. Achong-Coan R, Caroline P, Kinoshita B, et al. How do normal and keratoconic eyes differ in shape? Poster presented at the Global Specialty Lens Symposium, January 28, 2012, Las Vegas.
12. Schornack M, Patel S. Relationship between corneal topographic indices and scleral lens base curve. Eye Contact Lens. 2010 Nov;36(6):330-3.


