
Are we providing the best contact lens care for our medical patients? A number of contact lens wearers suffer from various conditions that may hinder their ability to wear contacts, including dry eye, ocular allergies and even glaucoma. But with these so ubiquitous in eye care practices, it is often difficult to separate such patients from our “healthy” contact lens wearers.
When we do, we tend to sideline their contact lens-wearing goals, thinking that’s an acceptable sacrifice for the greater good of restoring ocular health. Sometimes, perhaps. But not universally.
We also have patients we like to call “silent sufferers.” These are our contact lens wearers who don’t want to admit to having any type of medical condition. Oftentimes, they perceive this as an issue that may even prevent them from wearing contact lenses in the future. Take the time to identify any chronic or urgent underlying condition that will impact their corneal health—and, in so doing, you’ll keep them in their contact lenses long term.
Do You Promote Urgent Care?
Too many times a patient visits their local urgent care facility to receive eye care, only to be given nothing more than an eye patch for a corneal insult. Of course, these patients are best cared for by their eye care professional, who can treat the issue using a bandage—be it a contact lens or a biologically active substance.
These patients are often very loyal to our practices, just typically unaware that they are supposed to see us for their urgent conditions.
Most patients know to come to us for vision exams, contact lens evaluations and medical treatment for various conditions. But, most do not know that we provide urgent care as well—and it’s our job to let them know that we do. Giving your patients this urgent medical care can serve to both distinguish your practice and further strengthen patient loyalty. This area of our practices may prove to offer the most growth potential in the near future.

| |
| Fig. 1. Have patients fill out an informed consent before conducting medical procedures. |
While developing a medical model and offering this service may take some internal changes (e.g., understanding medical billing and educating your staff), it can be extremely rewarding. The medical treatment and procedures you will perform will provide the patient with the highest quality of care. Prior to conducting any medical procedure, it is important to have the patient sign an informed consent form. Figure 1 shows an example of one used in Dr. Miller’s office.
As eye care professionals, we’re no strangers to patients with various types of ocular surface disease. Patients who present with advanced conditions, such as recurrent corneal erosions, are typically treated with the use of bandage soft contact lenses. In some cases, however, they will need special biological therapies to encourage corneal healing. Both of these options can help relieve pain and promote healing in patients with trauma to the cornea.
Bandage Contact Lenses
Corneal abrasions are one of the most common uses for these lenses in primary eye care. In the presence of an abrasion, bandage contact lenses shield the highly-enervated corneal surface from the constant mechanical irritation of the eyelids. This offers patients a high level of comfort almost immediately upon lens insertion, and allows patients to return to normal function by controlling the pain.1
|
|
|
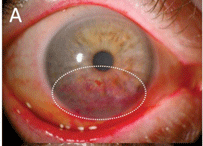
Fig. 2a. Exposure keratopathy before treatment with Prokera.
|
Unfortunately, not every insurance carrier will pay for this care. As such, it is necessary to first contact the patient’s insurer to determine which services (e.g., the fitting, the lens, replacement of lost lenses, etc.), if any, are covered. Then, have them sign an ABN before moving forward with any treatment.
Amniotic Membranes
Prokera (Bio-Tissue) is an FDA class II medical device comprised of an amniotic membrane suspended between two plastic rings. The company describes it as a “biologic corneal bandage” that helps reduce inflammation and stimulate healing.
The therapy uses a cryopreserved amniotic membrane as a novel alternative to traditional bandage treatment options. These devices are capable of treating many common corneal conditions, such as recurrent corneal erosions, corneal ulcers and ocular surface disease. They do so by promoting active healing.
|
|
|
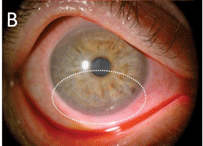
Fig. 2b. The same eye post-treatment.
|
Amniotic membranes naturally promote epithelialization, suppress inflammation, and inhibit scarring and anti-microbial agents—without the harmful side effects found in topical and oral medications. These devices have been instrumental in the proper healing of many patients.
Patients who suffer from chronic ocular surface disease need our help. Whether you are treating these patients with bandage contact lenses during an acute episode or amniotic membranes when appropriate, taking the initiative to actively diagnose and treat these patients is an important part of the healing process.
Using the aforementioned options to manage these conditions may allow the patient to return to comfortable full-time lens wear sooner and more comfortably. Taking the “extra steps” to improve the health and comfort of these individuals may prove valuable in preventing contact lens dropouts and further enhance patient loyalty.
|
It'll Take More Than a Bandage
|
|
A 57-year-old female with history of penetrating kerotaplasty OU and
chronic recurrent corneal erosion presented with complaints of another
painful red eye. She couldn’t remember any recent incident or trauma to
her eye, and her only ocular therapy at the time was Pred Forte 1% QD.
She had been treated multiple times with a bandage contact lens.
We discussed the use of an amniotic membrane, explaining how it differs from simply putting on a contact lens. She consented and the amniotic membrane was applied. Her recurrent corneal erosions healed in approximately one week, and then the device was removed. She is now six months post-treatment without recurrence. |
A special thank you to Walt Whitley, OD, MBA, and Rachèle M. Rivière,
MBA, Associate Brand Director, Prokera, for their assistance with this
article.
1.Buglisi JA, Knoop KJ, Levsky ME, Euwema M. Experience
with bandage contact lenses for the treatment of corneal abrasions in a
combat environment. Mil Med. 2007 Apr;172(4):411-3.


