As with any field, innovation and change in eye care is happening constantly—and these days it’s occurring at breakneck speed. Ongoing studies, as well as plans for future research, are the cornerstone to advances in all areas of clinical care. Without novel ideas, stagnation and decline are inevitable.
While no single report can capture the scope of findings presented in the thousands of papers and posters offered during the recent Association for Research in Vision and Ophthalmology’s (ARVO) meeting in Denver, Colo., here we present 20 intriguing findings related to cornea and contact lens topics from the many abstracts presented. The research shared at this year’s meeting will undoubtedly help in developing new strategies for diagnosing ocular health and visual problems, directing new treatment plans and ultimately improving patient care.
1. Photo-responsive contact lens may help patients suffering from iris damage or congenital defects. Patients with diminished iris function often experience photophobia, glare and poor vision when exposed to excessive light. For those with congenital or trauma-induced iris damage, commercial artificial irises provide aesthetic improvement but don’t address iris function.
To solve this issue, researchers from the University of Chicago developed a photo-responsive contact lens that mimics the natural iris’s response to light using DEA, a photochromic material, within a biocompatible polymer matrix. Because DEA changes its opacity when exposed to blue light, the contact lens is able to control the amount of light entering the eye using rapid and reversible activation by blue light to alleviate the adverse symptoms of decreased iris function. Biocompatibility was demonstrated by cell culture experimentation and minimal DEA leaching was observed.
Program #6102. Designing a Photo-Responsive Contact Lens. ARVO 2015.
2. Time between appointments impacts daily disposable overnight wear and reuse. Researchers attempted to quantify predictors for wearing daily disposable lenses overnight and reusing them over time by evaluating data on silicone hydrogel daily disposable lenses from the 1-Day Acuvue or 1-Day Acuvue Moist Performance Overview (TEMPO) Registry. Factors included age, gender, compliance as rated by the wearer and eye care practitioner (ECP), and self-report of habitual overnight wear of contact lenses. Lens reuse was predicted both through self-reporting by the patient and based on ECP assessment of compliance and baseline measures. Both daily disposable lens overnight wear and reuse were found to increase significantly in correlation with longer time since refitting, suggesting that ECPs must retrain patients when refitting daily disposables in regards to proper wear and care.
Program #6086. Predictors for Misuse of Daily Disposable Lenses in a Large Post-market Surveillance Registry—The TEMPO Registry. ARVO 2015.
3. MMP-9 increase during early contact lens wear may signal oncoming dry eye disease. This University of New South Wales team investigated how levels of a marker of inflammation in tears known as matrix metalloproteinase-9 (MMP-9) changed as a function of contact lens wear. In previous studies, altered morphology and poorer function of meibomian glands was identified in contact lens wearers and previous lens wearers. The mechanism for this remains unclear, but inflammation is thought to present as an etiological component of eyelid tissue change, as it is known to accompany dry eye disease and contribute to its propagation.
In the current study, total MMP-9 concentration was established using sandwich enzyme-linked immnunosorbent assay. Researchers found that MMP-9 increases during the early years of contact lens wear, parallel to the onset of morphological change in the meibomian gland. This may be an indication of an inflammatory mechanism in meibomian gland dropout in contact lens wearers.
Program #333. Potential Role for Matrix Metalloproteinase-9 in Meibomian Gland Changes in Contact Lens Wearers. ARVO 2015.
4. Drug-delivering nanowafer could treat dry eye. Scientists from the Baylor College of Medicine in Texas compared the effects of treatment with dexamethasone in a controlled-release nanowafer (DEX-NW) system or eye drops in a murine desiccating stress model of dry eye, as the condition is believed to be a steroid-responsive ocular surface inflammatory disease. The DEX-NW system was placed on the bulbar conjunctiva on days one and three of the study and proved equally as effective in treating dry eye as topical dexamethasone drops instilled twice daily for five days. This suggests the DEX-NW system has potential for delivery of other drugs to the ocular surface.
Program #321. Nanowafer Drug Delivery for Restoration of Healthy Ocular Surface in Dry Eye Conditions. ARVO 2015.
5. Androgens may play a more significant role in dry eye disease than previously thought. Researchers from Croatia have discovered a statistical connection between dry skin and dry eyes as part of a study aimed at determining whether one is linked to the other. Patients were screened for dry eye symptoms and asked to describe their facial skin with regards to dryness or oiliness. A sebumeter was also used to objectively determine the amount of oil produced by each patient’s skin. Findings indicated that subjects without dry eye symptoms self-reported oilier skin than those with dry eye symptoms, and sebumometry scores were found to be higher in subjects without dry eye symptoms compared with those with dry eye symptoms.
The researchers surmised from the results that since both skin and eyes play a significant role in dehydration prevention, there may be a single regulator for this function. Additionally, since androgens play a role in sebum secretion, it’s likely that androgens play a much more significant role in dry eye that previously thought.
Program #4442. Dry Eye and Dry Skin—Is there a Connection? ARVO 2015.
6. Novel antibodies may aid in earlier diagnosis of Sjögren’s syndrome. Traditionally, Sjögren’s syndrome (SS) is diagnosed based on the presence of certain autoantibodies including antinuclear antibodies, anti-Ro/SSA and anti-La/SSB antibodies, rheumatoid factor and thyroid antibodies. However, three new autoantibodies—secretory protein-1 (SP-1), carbonic anhydrase-6 (CA-6), and parotid secretory protein (PSP)—examined by researchers at the University of Pennsylvania may aid in earlier diagnosis of the immune system disorder. Researchers examined 68 dry eye patients using the Sjö kit: 22 tested positive for the novel SS autoantibodies (32.4%) while four tested positive for traditional autoantibodies (5.9%). Of the three novel autoantibodies, CA-6 was the most prevalent. There was no significant correlation between ocular surface exam signs and the presence of novel autoantibodies, however. The researchers concluded that further examination of patients who are positive for novel SS antibodies is needed to help determine the value of these antibodies in early detection of SS in dry eye patients.
Program #344. Novel Sjögren’s Syndrome Antibodies in Dry Eye Patients. ARVO 2015.
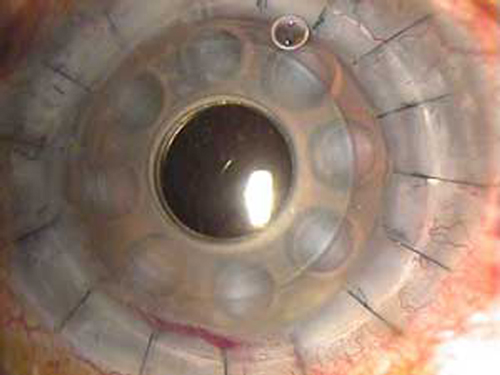 | |
| Glare is a common side effect of artificial corneas; however, a new modification could prevent this. Photo: Elyse L. Chaglasian, OD |
7. Back plate modification can reduce the glare effect experienced by patients with artificial corneas. Patients frequently report significant glare following Boston Keratoprosthesis (Boston KPro) surgery, in which an artificial cornea is implanted as a last treatment option for patients with recalcitrant or endstage corneal disease. Use of an opaque contact lens is helpful but movement of the lens can limit its ability; thus, an alternative method is needed. Researchers at the Massachusetts Eye and Ear Infirmary and Case Western Reserve University found that use of a newer titanium back plate in the Boston KPro device provides better glare protection compared with the older PMMA counterpart. No difference in glare was noted between pseudophakic and aphakic KPros with this modification, suggesting it may be an effective way to reduce glare.
Program #1121. Glare Reduction Strategies for Keratoprosthesis. ARVO 2015.
8. Graft rejection in atopic dermatitis patients undergoing keratoplasty reduced with corticosteroid use. A retrospective study on outcomes and treatments for atopic patients undergoing keratoplasty suggests patients with atopic dermatitis have a higher potential for graft rejection, infection and post-keratoplasty atopic sclerokeratitis. Researchers at Fukouka University in Japan examined the medical records of 183 patients prescribed systemic immunosuppressants or corticosteroids during the preoperative period. Postoperative complications included four eyes with cornea graft rejection and two eyes with methicillin-resistant Staphylococcus aureus (MRSA) culture-positive from the graft and anterior chamber. No cases of post-keratoplasty atopic sclerokeratitis were observed, however. These results indicate that early treatment using immunosuppressants or corticosteroids could improve graft survival in high-risk atopic patients.
Program #1549. Treatment Outcomes of Keratoplasty with Atopic Dermatitis. ARVO 2015.
9. Previous use of glaucoma drainage device may impact graft failure rate. A small retrospective study from investigators at Wills Eye Hospital, Oxford Valley Laser Vision Center and Sidney Kimmel Medical Laser Vision Center at Thomas Jefferson Hospital in Philadelphia examined graft failure rates and endothelial cell loss after Descemet’s stripping automated endothelial keratoplasty (DSAEK) in eyes with previous glaucoma drainage devices (GDD). Researchers reviewed 25 cases in 22 eyes with prior GDDs undergoing DSAEK, and found no cases of primary graft failure. However, secondary graft failure occurred in 48% of grafts, with average time to failure 33.3+/-16.8 months over the mean follow-up period of 36.1 months. This suggests the procedure may be complicated by the presence of a prior GDD because of the frequent inability to raise the pressure in the eye adequately enough to achieve effective air tamponade. Additionally, compared to the endothelial cell count (ECC) at the time of transplantation, graft ECC decreased by 74.8+/-14% at 36 months, reaffirming the significant rate of intermediate term endothelial cell loss and secondary graft failure in eyes undergoing DSAEK with prior GDDs.
Program #1565. Three-Year Follow-up of DSAEK Failure Rates and Endothelial Cell Loss in Eyes with Glaucoma Drainage Devices. ARVO 2015.
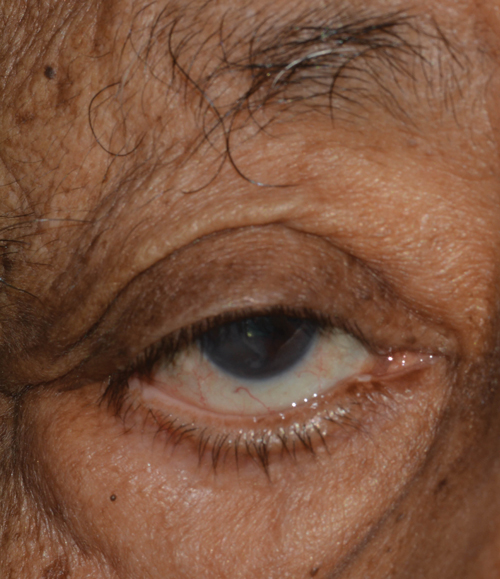 | |
| Ptosis may be an underreported side effect of topical mitomycin C therapy. |
10. Significant link between ptosis and topical mitomycin C identified. Topical mitomycin C (MMC) is a well-established primary or adjunctive therapy for ocular surface neoplasia. Adverse effects include allergic reactions, epiphora secondary to punctal stenosis and limbal stem cell deficiency. Ptosis, however, is rarely reported as a consequence (1%). Researchers from the University of Liverpool and the Oncology Service at University of California, San Francisco, suspected that the true incidence was underreported and studied the prevalence of this complication in their patients who had received topical MMC therapy. Fifty-four neoplasia patients were identified with a mean age of 62 at the time of treatment. Forty-two percent of patients receiving mitomycin application for neoplasia reported ptosis. Following retrospective chart review, researchers surmised that ptosis after topical MMC-therapy at a standard dose and regimen is vastly underreported, and that patients should be better warned of this potential adverse event.
Program #1602. Prevalence of Ptosis after Topical Mitomycin C Therapy for Conjunctival Neoplasia. ARVO 2015.
11. Lid-debridement scaling could help treat Sjögren’s syndrome-related dry eye. A pilot study from investigators in Canada sought to determine the effect of lid-debridement scaling (LBS) of dry eye signs and symptoms in patients with Sjögren’s syndrome (SS). Subjects were divided into a control group and treatment group. The treatment group was evaluated pre-LBS and post-LBS with the Ocular Surface Disease Index (OSDI), ocular staining and Meibomian Gland Evaluator (MGS), and showed statistically significant improvements in OSDI along with ocular staining and meibomian gland function. Thus, this study indicates LBS may help with the management of Sjögren’s syndrome-related dry eye.
Program #2487. Effect of Lid Debridement-Scaling on Dry Eye Signs and Symptoms in Sjorgren’s Syndrome. ARVO 2015.
12. Higher prevalence of meibomian gland dysfunction in Caucasians. Researchers in Boston evaluated the prevalence of meibomian gland dysfunction (MGD) among Caucasian patients (n=168) using a standardized metric for meibomian gland function to see whether various genetic factors (i.e., skin type, eye and hair color) increase the likelihood of MGD in this population. The prevalence of MGD (characterized by 25% or fewer functional MGs) was 70.2%, while prevalence was 43% with a more conservative cutoff of four or fewer functional meibomian glands (17%). Skin type, eye color and hair color had no statistically significant impact on the likelihood of MGD in this population; nevertheless, overall prevalence of MGD in this population was substantial—70.2%—which is significantly higher than previous reports of the prevalence of MGD in Caucasian populations.
Program #2508. The Prevalence of Meibomain Gland Dysfunction in a Caucasian Clinical Population. ARVO 2015.
13. Blepharitis may cause corneal thinning. Alterations of the tear film and local inflammation, both hallmarks of blepharitis, may result in corneal thinning, reports a study from France. Researchers measured central corneal thickness of 40 eyes of 20 patients (11 men) with blepharitis; the mean age was 58.5. Forty eyes of 20 healthy patients were used as a control group; mean central thickness was 554.9µm. The researchers surmised that increased osmolarity and ocular surface inflammation are the cause of this decrease in corneal thickness.
Program #2511. Blepharitis and Thin Corneal Thickness: An Unexpected Association. ARVO 2015.
14. Focal crosslinking is a better alternative to pan-corneal crosslinking. Traditionally, pan-corneal crosslinking (CXL) is used to stabilize and reduce corneal curvature in keratoconus (KC). However, theoretical finite element models (FEM) of crosslinking in the keratoconic cornea have suggested focal treatment may lead to better postoperative central corneal symmetry, and the recent development of patterned UV systems offers an opportunity to provide focal treatment with the intention of improving vision.
This study retrospectively examined focally applied crosslinking in keratoconus patients to evaluate the potential of focal CXL to improve visual function. At six months, focal CLX subjects’ central topographies were more symmetric, exhibiting inferior flattening and superior steepening on sagittal and tangential maps as predicted by FEM models. On average, there was no significant progression of corneal steepening over the follow-up period, nor significant change in K max. For most subjects, however, the treatment area did not enclose the area of maximum corneal thinning and posterior elevation. Thus, preliminary results suggest that focal treatment may provide greater visual improvement and improved contact lens tolerance over pan-corneal crosslinking.
Program #3000. Design of Focal UVA Delivery Patterns for Cross-Linking Treatment of Keratoconus. ARVO 2015.
15. Subconjunctival injections for whiter eyes. Researchers from the Southwestern Eye Center, St. Bernard’s Medical Center and Ross University School of Medicine explored the possibility of an alternative method of whitening the eyes using subconjunctival injections to avoid complications associated with current, controversial techniques. Recent reports have detailed the dangers of certain eye whitening procedures that combine the removal of generous portions of the conjunctiva with cautery, laser and use of antimetabolites. In the new method, ink is injected into the subconjunctival space using a 25-gauge needle. Researchers noted the ink covered deeper scleral vessels but that superficial conjunctival vessels were still visible, suggesting the technique may be a viable, safer means of whitening the eyes.
Program #3024. Eye Whitening Using Subconjunctival Injections. ARVO 2015.
16. Thermal pulsation for MGD and clinical merit of Sjö testing validated. Researchers from the Ohio State University investigated whether the LipiFlow (TearScience) device improves subjective and objective variables relating to dry eye and MGD, and if a correlation to Sjögren’s syndrome exists. Evaporative dry eye from MGD is the most common form of dry eye, and thermal pulsation therapy using the LipFlow device is the only FDA-approved treatment.
Researchers retrospectively reviewed records of patients who received a single 12-minute session of thermal pulsation, paying particular attention to SPEED scores, preoperative lipid layer thickness, meibomian gland dropout, tear breakup time (TBUT) and meibomian gland evaluation scores (MGES). A test for Sjögren’s syndrome was also performed, and patients were retested six to eight weeks following treatment. Researchers noted a statistically significant difference between pre- and postoperative SPEED scores, TBUT and MGES, suggesting the effectiveness of a single treatment using LipiFlow. Additionally, 43% of the patients tested positive with the Sjö test compared with 26% of the controls, indicating there is a strong correlation between a positive Sjö test and MGD, indicating an autoimmune component contributing to symptoms experienced in this disease process.
Program # 3050. Evaluation of a Single Thermal Pulsation Treatment for Dry Eye and Meibomian Gland Dysfunction and Likelihood of Positive Sjo Test. ARVO 2015.
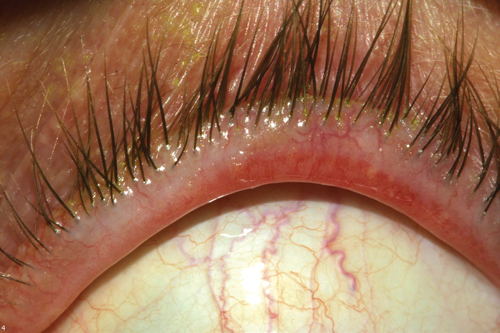 | |
| Blepharitis may cause corneal thinning, says a study from France. |
17. Dexamethasone formulation effective against blepharitis. A joint team of researchers and clinicians from Minnesota Eye Consultants and InSite Vision evaluated the safety and efficacy of a fixed combination and single agents in DuraSite (dexamethasone and azithromycin) in combination with lid hygiene using lid scrubs to treat blepharitis. Clinical signs (i.e., eyelid redness, swelling and debris) were assessed along with patient-reported satisfaction results. Patients randomized to the dexamethasone-azithromycin arm and dexamethasone arm alone experienced a statistically significant greater reduction in blepharitis scores when compared with the AzaSite and/or vehicle alone groups. Few side effects were noted. These results suggest the anti-inflammatory properties of dexamethasone formulated in the long lasting DuraSite vehicle appear to be effective in treating signs and symptoms of blepharitis for up to six months.
Program #3058. A Phase 3 Clinical Study to Evaluate the Efficacy and Safety of Fixed Combination of Azithromycin and Dexamethasone in DuraSite and Dexamethasone Alone in DuraSite in the Treatment of Blepharitis. ARVO 2015.
18. Contact lens discomfort mediated by leukotriene B4. Elevated levels of tear film components may at least partially mediate the discomfort response during lens wear, according to a study from the University of New South Wales. Researchers measured prostaglandins, leukotriene B4 and cysteinyl leukptriene (C4, D4 and E4) using enzyme immunoassay kits in both symptomatic and asymptomatic contact lens wearers. An elevated LTB4 level was detected in symptomatic wearers compared with asymptomatic wearers, but the other markers remained essentially unchanged across the two comfort groups. Lysozyme levels were slightly reduced in symptomatic wearers at the end of the day. Further investigation is needed, however, to determine any significant findings that may aid in treating patients with contact lens comfort problems.
Program #3166. Tear Film in Symptomatic and Asymptomatic Lens Wearers. ARVO 2015.
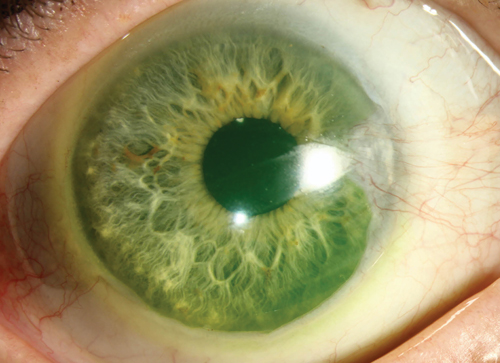 | |
| Researchers may be closing in on the ideal clearance for achieving adequate oxygen transmissibility under a scleral lens. |
19. Is 200µm ideal clearance under scleral lens? Investigators from the University of Montreal School of Optometry evaluated oxygen partial pressures under rigid gas permeable scleral lenses with different amounts of clearance in an effort to determine the ideal amount needed under a scleral lens. Researchers measured the thickness of the liquid layer beneath the contact lens using optical coherence tomography and pO2 levels at the corneal surface using a Clark electrode and an electrometer linked to a computer after five minutes of wear. As predicted, calculations of oxygen transmissibility of scleral lens systems demonstrated that an increased thickness in clearance reduces oxygen tension available to the cornea; ultimately, a clearance close to the 200µm level may help the adequate amount of oxygen reach the cornea.
Program #6074. Measuring Oxygen Tension Under Scleral Contact Lenses of Different Clearances. ARVO 2015.
20. Mechanical mapping technology could assess corneal ectasia. Scientists from the Massachusetts General Hospital and Harvard Medical School presented a non-contact in-vivo mechanical mapping of keratoconus based on Brillouin scattering with axial scans at various lateral positions. The balance between the cornea’s mechanical strength and intraocular pressure is critical to maintain normal shape—when this is disrupted, the stress can lead to progressive compensatory thinning and bulging of the cornea, or keratoectasia. In normal patients, it was observed that corneal mechanical strength decreased with depth and increased toward the periphery. Additionally, the modulus also increases with age. Thus, the Brillouin modulus was positively correlated with corneal thickness and negatively with front surface sagittal curvature.
Striking differences could be observed between normal and keratoconic corneal biomechanics. In the normal cornea, the elastic modulus gradually increases from its center to the periphery. Strong focal weakening was observed in the keratoconic eyes. Corneal stiffness seems to increase with age and may explain the high prevalence of keratoconus in earlier years. Thus, this technology seems to hold potential in assessing corneal ectasia and measuring therapeutic benefits from procedures such as collagen crosslinking.
Program #1138. 3D Corneal Elasticity Mapping in Normal and Keratoconus Patients. ARVO 2015.
While the 20 abstracts highlighted here were selected specifically for this Review of Cornea & Contact Lenses report, you are encouraged to review the many other abstracts available from this year’s ARVO conference (Available at www.arvo.org/Annual_Meeting/2015/Abstracts/2015_Session_Abstract_PDFs/). I’m sure you’ll find them fascinating. And as always, we look forward to another round of clinically relevant research to be presented next year!
Dr. Shovlin, a board-certified optometrist who practices at Northeastern Eye Institute, is the Clinical Editor of Review of Cornea & Contact Lenses and an Associate Clinical Editor of Review of Optometry. He is also President-elect of the American Academy of Optometry.


