 Blepharitis and meibomian gland disease are significant causes of contact lens discomfort and inflammation, and as such, these conditions must be identified and addressed prior to contact lens fitting. In ocular surface disease sufferers, specific lens cleaning regimens may help improve comfort and enhance the lens wearing experience.
Blepharitis and meibomian gland disease are significant causes of contact lens discomfort and inflammation, and as such, these conditions must be identified and addressed prior to contact lens fitting. In ocular surface disease sufferers, specific lens cleaning regimens may help improve comfort and enhance the lens wearing experience.
Recognize the Signs
In lid margin disease, inspissated meibomian glands, lid margin telangiectasias, collarettes and decreased tear break-up time are typical findings. Ten percent of the population may have rosacea, and up to 50% of rosacea patients will have concomitant ocular findings. The ocular findings, however, may precede the generalized facial symptoms by many years.1 In contact lens wearers, toxins produced by the lid margin bacteria are adsorbed into the lens, likely causing increased symptoms and staphylococcal marginal keratitis complaints.2
Lid Disease Treatment
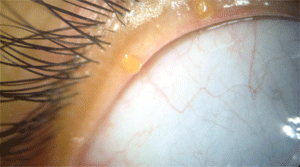
Capped meibomian glands may lead to dryness.
For hygiene-based treatment of lid margin disease, it is important to recommend products that are compatible with the lid and ocular surface. Baby shampoo is often recommended to cleanse the eyelid margins, but it can be harsh if not diluted, which may cause excessive drying of the periorbital area. Products with a foam pump, such as OcuSoft foaming eyelid cleanser (Cynacon/OcuSoft) and Thera- Tears SteriLid Eyelid Cleanser (Advanced Vision Research), may be easier for patients to use. They aim not to cause drying or flaking of the periorbital area or burning upon application, which enhances patient compliance.
Hot compresses are useful, but they are sometimes difficult for patients to apply, which leads to eventual noncompliance. I recommend that the patient apply hot compresses for five minutes two or three times a day, depending on the severity of the lid disease. A wet washcloth may be ineffective, because it does not hold heat for five minutes. Various techniques can be used to apply hot compresses. One clean, inexpensive, reusable and effective option is to put dry rice in a small sock and heat the sock in the microwave until it is warm; patients should be cautioned to avoid overheating the compress, as this can cause skin burns. For patients who prefer to avoid a homemade technique, there are commercial hot pack products, such as OCuSOFT Goggles with reusable heating elements.
Patients who do not respond to this line of therapy, particularly those with ocular rosacea, may require such medications as doxycycline (oral), azithromycin (topical or oral) or nutritional supplements (e.g., omega-3 fatty acids, oral flax seed oil) to modify the lipid component of the tear film and increase break-up time.3 Short bursts of topical antibiotic-steroid ointment are effective in ameliorating lid disease.
Effective Lens Cleaning
Contact lens cleaning is another issue that must be addressed in patients with lid disease in order to ensure contact lens wearing success. Ideally, patients must remove debris, toxins and pathogens from their lenses nightly. This can be done either through the use of daily disposable contact lenses or with specific cleaning techniques. For our patients who cannot wear daily disposable lenses, we recommend a digital rub with a preservative-free alcohol-based cleaner—such as Sereine Extra Strength Cleaner (Optikem Care System)—for superior pathogen and deposit control before soaking in a multipurpose solution.4,5
First Things First
Patients with lid and ocular surface disease can effectively wear contact lenses as long as their conditions are diagnosed in a timely fashion and specific attention is paid to treatment and proper cleaning routines.
1. Scheinfeld N, Berk T. A review of the diagnosis and treatment of rosacea. Postgrad Med. 2010 Jan;122(1):139-43.
2. Knop E, Knop N. Meibomian glands: part IV. Functional interactions in the pathogenesis of meibomian gland dysfunction (MGD). Ophthalmologe. 2009 Nov;106(11):980-7.
3. Alikhan A, Kurek L, Feldman SR. The role of tetracyclines in rosacea. Am J Clin Dermatol. 2010;11(2):79-87.
4. 510(k) Summary of Safety and Effectiveness. Available at: www.accessdata.fda.gov/cdrh_docs/pdf7/K071203.pdf. (Accessed February 2010).
5. Ghajar M, Houlsby RD, Chavez G. Microbiological evaluation of MiraFlow. J Am Optom Assoc. 1989 Aug;60(8):592-5.


