 One of the most common complaints that contact lens wearers have is discomfort during lens wear. Many studies have shown that more than half of all dropouts stem from contact lens discomfort.1 Maximizing comfort is the main approach to keep patients happy in their contact lenses. Here, we will review some strategies for maximizing comfort and successful contact lens wear in patients who require gas-permeable (GP) and other specialty contact lenses.
One of the most common complaints that contact lens wearers have is discomfort during lens wear. Many studies have shown that more than half of all dropouts stem from contact lens discomfort.1 Maximizing comfort is the main approach to keep patients happy in their contact lenses. Here, we will review some strategies for maximizing comfort and successful contact lens wear in patients who require gas-permeable (GP) and other specialty contact lenses.
Gas-Permeable Strategies
GP lenses are invaluable in providing a stable visual experience for those with high amounts of astigmatism. For presbyopes, they can offer a greater range of clear vision, which enables us to maximize both distance and near vision for our patients. Additionally, GP lenses have the unique ability to mask irregularities of a diseased or irregular corneal surface.
For some patients, GP lens use is the only effective way to maximize visual function. So, strategies that maximize comfort with this design are necessary when fitting some more challenging prescriptions. Most often, patients have difficulty with excessive movement of the lens. In such cases, conventional wisdom suggests steepening the base curve to tighten the fit and minimizing excessive movement.
For patients with compromised tear films, a plasma treatment may be warranted. Plasma treatment of the GP lens modifies the superficial layer and generates a hydrophilic surface that promotes enhanced wettability. Plasma-treated GP lenses will create a reduced wetting angle as well and can potentially increase comfort during wear. Don’t use abrasive cleaners; they can remove the plasma treatment. Additionally, repeated use of laboratory cleaners will soften the treated surface and therefore should be avoided as well.2
Hybrid Contact Lens Technology
There have been many technological advances in the contact lens industry. The hybrid technology platform is an excellent example of how material science can offer those with unique visual needs the ability to wear contact lenses successfully. The two commercially available hybrid lenses are the Softperm (CIBA Vision) and the SynergEyes lens. Both designs work well. The SynergEyes design increases oxygen delivery to the cornea through the GP portion of the lens. There were no previous high-Dk hybrid lenses on the market due to “the difficulty in bonding hydrophilic skirts to high-Dk rigid materials.”3 The bond developed by the polymer chemists at SynergEyes is “approximately 10 times stronger than previous hybrid lenses.”³ The unique hybrid platform and design allows the contact lens practitioner to provide the benefits of GP optics in a lens that, because of its soft skirt, usually provides new wearers less lens awareness.
A study comparing hybrid technology lenses to soft toric contact lenses found that the subjects preferred soft toric lenses 56% of the time with regard to comfort, but the hybrid lenses provided significantly better visual acuity.4 This study went on to reveal that, of seven previous GP wearers, five (71.4%) preferred the hybrid lens technology.
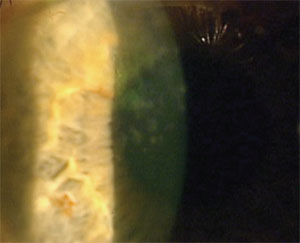
In this patient, the corneal
irregularities located superior nasally on the left cornea are
secondary to previous PTK for Salzmann’s nodular degeneration.
Certain patients will not tolerate GP lens designs. In cases where a patient would benefit from the optics that a GP delivers, but cannot wear the lenses because of discomfort, consider hybrid lens technology. The soft skirt surrounding the GP center will create less lens and edge awareness.
Scleral Contact Lenses
When fitting GP lenses, larger-diameter contact lenses may be considered a viable option. It is not uncommon to order GP lenses with a diameter greater than 10mm. For those with corneas difficult to fit with traditional GP lenses, a large-diameter lens may be warranted. Many designs can be utilized, including corneal-scleral, semi-scleral, mini-scleral or scleral contact lenses. These specialty lenses are utilized for their ability to mask irregularities, but because of their large diameter, they are, in certain situations, better tolerated than traditional small-diameter GP lenses. Scleral lenses vault the cornea, and much of the lens bears on the sclera vs. the cornea. These lenses are indicated in patients whose corneal irregularities stem from:
• Keratoconus.
• Trauma.
• A history of penetrating keratoplasty or refractive surgery.
• Stevens-Johnson syndrome.
• Neurotrophic keratitis.
• Severe dry eye syndrome.
Hydroxypropyl Cellulose Inserts
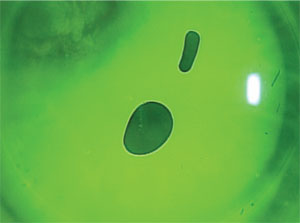
This fluorescein pattern
is that of a hybrid contact lens fit shortly after lens insertion. The
air bubbles noted here resolved after the lens was on the eye for about
20 minutes.
With the variety of soft contact lens options and care systems available, practitioners can usually change either one or both to maximize contact lens comfort. But, for those wearing specialty contact lenses, the situation becomes significantly more difficult because lens options may be more limited. In these cases, a lacrimal insert may improve comfort.
Hydroxypropyl cellulose inserts (commercially available as Lacriserts by Aton Pharma) are placed in the lower fornix, and over the course of a day, they dissolve demulcents into the tear film. With contact lens wearers, it’s important to place the insert in the eye after the contact lens. If the insert is placed in the eye before the lens, it will likely be displaced upon lens insertion.
In a recent registry of more than 500 patients who used hydroxypropyl cellulose inserts for 30 days, there was a 21.3% improvement in the ocular surface disease index. A subset of 86 patients in the study wore contact lenses, and in this group, there were measurable improvements in many areas—including a 23.2% improvement in OSDI scores.6
A Case in Point
“Molly,” a 42-year-old female, had phototherapeutic keratectomy (PTK) in her left eye to treat Salzmann nodular degeneration 10 years ago. She is relatively new to the area and visited an ophthalmologist to see if she could undergo PTK again to improve her vision. The ophthalmologist didn’t think that another surgical procedure was prudent at this point and referred her to our office for a contact lens fitting.
Molly’s best-corrected visual acuity was 20/60 O.S. She reported trying GP lenses in the past with poor success because she was “never able to get used to the lens.” The patient was fit with a hybrid lens technology with the following parameters: 7.4mm (GP) / 8.4mm (Soft Skirt) / -2.00D. Molly’s resultant visual acuity was 20/20-. The patient was extremely happy with the vision, but she could only wear the contact lens for four to six hours before she had significant comfort issues. Rewetting drops were used three to four times a day for only temporary relief. We recommended hydroxypropyl cellulose inserts to be utilized daily with lens wear, and she noticed significant improvement in comfort. Molly can now wear her contact lenses all day with minimal rewetting drop use.
The authors would like to thank Michael Johnson, Art Optical, for his help with this month’s column.
1. Young G, Veys J, Pritchard N, Coleman S. A multi-centre study of lapsed contact lens wearers. Ophthalmic Physiol Opt. 2002 Nov;22(6):516-27.
2. Pamphlet. Practitioner Q&A Plasma Treated GP Lenses. Art Optical Contact Lens, Inc.
3. Chou B. Rigid optics with soft lens comfort. Cont Lens Spect. 2006 July. Available at: www.clspectrum.com/article.aspx?article=13066. (Accessed January 2010).
4. Lipson MJ, Musch DC. Synergeyes versus soft toric lenses: vision-related quality of life. Optom Vis Sci. 2007 July:(7:593-7.
5. Hong X, Himebaugh N, Thibos LN. On-eye evaluation of optical performance of rigid and soft contact lenses. Optom Vis Sci. 2001 Dec;78(12):872-80.
6. Lacrisert (hydroxypropylcellulose ophthalmic inserts) significantly improves symptoms of dry eye syndrome (DES) and patient quality of life. Poster presented at: ARVO Annual Meeting; May 3-7, 2009, Ft. Lauderdale, FL. Program 4660.


