Much has been written about how to succeed in multifocal contact lens correction of presbyopia. The emphasis, understandably, is usually on the lens design parameters and how to customize them for your patients. Knowing which lens to use in a particular case is extremely important, which is why we need to make sure we ask the right questions and conduct a thorough preliminary examination.
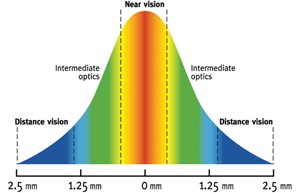
Representative center-near simultaneous image multifocal lens design.
We are all familiar with the attributes of a desirable multifocal contact lens candidate: a healthy and wet ocular surface, normal pupil size, a refractive error within certain parameters, proper motivation and realistic expectations.1
What about patients who do not meet some, or any, of these criteria? Should we simply abandon these patients and consider them lost causes? That would certainly be a mistake. In this article we will explore these issues and ways to make successes out of what we would typically consider questionable prospects.
Ocular Health Screening
First, let’s discuss ocular health status. Generally speaking, a compromised eye is not a good environment in which to insert any contact lens, let alone one that must correct a multitude of refractive errors. There are certain exceptions to this, though. In our initial examination, we must assess the patient’s lids and lashes, tear film, cornea and conjunctiva. If blepharitis is present, it must first be cleared up, otherwise there could be problems with debris under the lens, or even Staphylococcus-related inflammation or infection.2 Similarly, if Demodex proliferates, this overpopulation needs to be eradicated before the contact lens fitting. Left untreated, this ectoparasite can cause inflammation and pustules. Medications such as oral ivermectin3 and localized treatments like tea tree oil have been used for treatment.
Pay special attention to the meibomian glands, lid wiper and tear film quality. Meibomian gland obstruction needs to be treated via warm compresses and/or expression. The importance of the lid wiper in external ocular health cannot be forgotten.4 Lid wiper epitheliopathy (LWE) needs to be addressed and remedies found. LWE can manifest as ocular dryness and may be accompanied by keratitis, although some patients are asymptomatic. If an incomplete blink is involved, behavior modification can help, as can lubricants.5
Also, the tear film integrity is vitally important, as in all contact lens wearers. If there is debris in the tear meniscus, or if the meniscus is scant, we must find a remedy. Do not forget to check the tear film break-up time to ensure the ocular surface is sufficently lubricated to withstand the introduction of a contact lens into its environment. Lubricants and the other standard measures used for meibomian gland dysfunction can help return the system to normal.
Check the cornea for signs of epithelial basement membrane dystrophy, vascularization, superficial punctate keratopathy and frank keratitis. The cause of any epithelial disruption needs to found and treated.
Finally, it is also important to examine the conjunctiva. Both the bulbar conjunctiva and tarsal conjunctiva need to be evaluated—yes, you must evert the upper lid. The cause of any injection of the bulbar conjunctiva, or papillary/follicular reaction of the tarsus, should be found and appropriate measures taken.6
Suffice to say that any prospective multifocal wearer deserves at least as much screening and pre-fitting care as a wearer of spherical or toric lenses, if not more. Dry eye often develops independently but concurrently as these patients reach their 40s.
Refractive & Lifestyle Factors
Once we are satisfied that the status of the ocular surface is suitable for contact lens wear, we can begin to consider the other aspects of presbyopic contact lens fitting. The list of possible “problem” patients includes those individuals with minimal distance refractive error but high add powers, younger patients with high adds, post-refractive surgery presbyopes, those with high astigmatism, older patients and patients with unrealistic expectations. Let’s begin with the latter patient type.
Any discussion of presbyopic correction strategies, either spectacle or contact lens approaches, needs to cover what these applications both can and cannot do. There are always trade-offs with any form of vision correction. Patients who expect their vision to be perfect at all distances will be disappointed. Simultaneous-image contact lenses use merged optics, which means that in order to get distance, intermediate and near vision in one lens there will necessarily be some compromise. Usually, either distance or near vision ends up slightly suffering, but still remains viable for most activities. Translating bifocals generally require the forgoing of intermediate vision, in exchange providing good distance and near acuity. So, it is important to first discuss the patients’ needs and priorities, both for their work and leisure activities, and then pick the lens design most suited to the task.
Older patients can pose a challenge for a number of reasons. Many older individuals have relatively small pupils in ambient light. This type of patient may have difficulty getting the most out of simultaneous image designs. The same is true of patients with very large pupils. Thankfully for these patients, there are translating designs available. Older patients also tend to have decreased tear film volume and stability. Lubricants can supplement the warm compress regimen, and can be used before, during and after lens wear. Often, older patients can have flaccid lids, which might affect lens movement and translation. In these patients lens design choice is important—a simultaneous image lens may be the better option.
Representative translating design bifocal contact lens.
There is also the option of using an oculoplastics surgeon to improve lid performance prior to attemping contact lens fitting.
Very often, the older patient has higher add power needs as well. Patients with high adds, whether older or younger, can be a challenge. Those with a long history of spectacle wear are accustomed to their glasses providing crisp near vision, and they expect the same from the contact lens. A soft lens may not work well in such patients. Gas permeable lenses to the rescue! GP bifocals, particularly translating designs, allow for the correction of higher adds without degrading distance vision. In the case of the older patient, corneal sensitivity is often lower, so comfort may be less of a concern with GP wear than in younger patients.
For a younger patient who is attempting GP lens wear, the generally improved clarity will usually help them through the adaptation phase, and good comfort is eventually achieved through acclimation to lens wear. Gas permeable lenses also work very well for the patient who has very low myopia but needs a bifocal/multifocal.
There are certainly soft multifocal lenses that are appropriate for these patients as well, particularly early presbyopes, whose visual demands are not too taxing, or those patients who may not be willing to tolerate the lens awareness that comes with GP wear. It all comes down to patient needs and practitioner experience as to which design to fit first.
Another area where GP lenses shine is in fitting a presbyopic post-refractive surgery patient. These folks often have unusual corneal profiles. Some also have ectasia, which can complicate the fit. The gas permeable lens designs offer great flexibility in instances such as these. One can find a posterior lens design to align the corneal curvature and correct the distance vision, and then add a bifocal or multifocal on the front surface to correct the near and intermediate vision.
This same approach also works well for those patients with high corneal astigmatism. A toric, or more often bitoric, back surface can provide both a good fit and vision, while the front surface can contain the necessary presbyopic correction. For those practitioners (or patients) who are uncomfortable with a GP lens, there are some very good soft lens designs that will correct the astigmatic and presbyopic refractive errors quite well.
None of the patients mentioned above present an insurmountable problem to fitting contact lenses, even multifocal lenses. The preliminary evaluation will point out the areas that require attention before the lens is placed on the eye and should indicate which design is best suited for that patient. It is simply a matter of the practitioner being aware of all the options that exist and presenting them honestly to the patient. It also helps if the eye care professional has experience with a number of different lens designs so that they feel confident in fitting them. These challenging patients can make the day interesting, to say the least, but the successes are all the sweeter because of it.
| Say "No" to Mono?
|
||
|
|
Many studies have shown that vision and
stereopsis is far superior with bifocal/multifocal corrections than in
monovision correction.7 Since both eyes have nearly equal
acuity with multifocals, overall vision is clearer and depth perception
is more normal. Monovision limits depth perception to such an extent
that the FAA will not allow pilots to fly wearing monovision
corrections. And as presbyopia advances, monovision eventually become
less and less viable and must be abandoned. Rather than start the
patient on a path that only offers a short-term solution—and one that
comes saddled with visual compromises at that—it seems prudent to take a
long-term perspective and have patients accept that adaptation to
multifocal optics is the better way forward.
That said, there is a place for modified, or enhanced, monovsion in presbyopic contact lens correction. Most designs take into account the role of eye dominance in vision. For this reason, the end visual result can be improved by biasing our power selections in the lenses. We must not forget that, for some individuals, single vision contact lenses with reading glasses might be the best option. It is even possible to use single vision lenses for near and put on glasses over them to enhance distance vision. However, most presbyopes presenting for contact lens evaluation desire to be spectacle-free and that should remain our goal. |
|
Dr. Benoit is senior optometrist with The Eye Center of Concord, a multi-subspecialty ophthalmology group located in Concord, NH. He is a Diplomate of the Section on Cornea, Contact Lenses and Refractive Technologies of the American Academy of Optometry.
1. Benoit DP. Inflammation and contact lens wear. Rev Optom. 2012 Apr; 149(4): 54-61.
2. Stapleton F, Keay L, Jalbert I, Cole N. The epidemiology of contact lens related infiltrates. Optom Vis Sci. 2007 Apr; 84(4): 257-272.
3. Holzchuh FG, Hida RY, Moscovici, BK, et al. Clinical treatment of ocular Demodex follicularum by systemic ivermectin. Am J Ophthalmol. 2011 Jun; 151(6): 1030-1034.
4. Korb DR, Herman JP, Blackie CA, et al. Prevalence of lid wiper epitheliopathy in subjects with dry eye signs and symptoms. Cornea. 2010 Apr; 29(4): 377-383.
5. McMonnies CW. Incomplete blinking: exposure keratopathy, lid wiper Epitheliopathy, dry eye, refractive surgery, dry contact lenses. Cont Lens Anterior Eye. 2007 Mar; 30(1): 37-51.
6. Fodor E, Barabino S, Montaldo E, et al. Quantitative evaluation of ocular surface inflammation in patients with different grade of conjunctivochalasis. Curr Eye Res. 2010 Aug; 35(8): 665-669.
7. Rajagopalan AS, Bennett ES, Lakshminarayanan V. Optom Vis Sci. 2006 Aug; 83(8): 611-615.


