|
Due to recent improvements in technology, scleral lenses are used more than ever to manage patients with irregular corneas, including presentations of keratoconus and other corneal ectasias. In moderate-to-advanced cases of keratoconus, a scleral lens may be required to help with lens centration.
Scleral lenses also accommodate corneas that are too steep to fit with corneal GP lenses or those that may have failed with other modalities.1 Vaulting the cornea minimizes risk of central scarring that can result from a poorly fitting corneal lens.
Although scleral lenses are a wonderful option, it is important to keep in mind the associated risks that may present with its use. There is still a large amount of evidence-based research necessary to determine the long-term side effects of scleral lens wear. The question is, however, should all patients be fit with scleral lenses? Is this arguably the new standard of care for this condition?
As part of the 2015 Gas Permeable (GP) lens annual report, 180 doctors were asked about their GP lens prescribing habits, reporting that though the majority of their fits were spherical lenses, one in five lens fits were achieved using scleral lenses (Table 1). Additional results reported scleral lenses were prescribed almost as often as corneal GP designs, with 50% of total fits being corneal GP designs and 44.7% of total fits being sclerals.
Interest in vaulting strategies also continues to represent an area of increasing current and future growth over traditional corneal GP lenses for patients with keratoconus. Trailing behind was the use of intralimbals, hybrids, custom soft and piggyback lens designs.2
Let’s now consider a few modalities to better understand their roles.
Small Diameter GPs
Gas permeable contact lenses continue to be the most commonly used contact lens type in keratoconus management.3,4 GP contact lenses mask irregular astigmatism to provide a more uniform anterior refractive surface. They also provide good tear exchange, but may be initially uncomfortable due to lid interaction with the edge of the lens. In mild cases, soft contact lens or spectacle wear may suffice; however, as the condition progresses, GP lenses are generally required to correct the irregular astigmatism. Often, a corneal GP lens is used unless centration or comfort is compromised, or another lens modality proves more useful.
Three types of fitting relationship exist for corneal GP lenses: apical clearance, apical touch and three-point touch. Apical clearance provides central vault over the apex of the cornea with support of the lens bearing on the paracentral cornea. This strategy is not commonly used due to reports of reduced visual acuity and risk for dimple veiling. This condition results from bubbles entering underneath the lens that lead to excessive tear pooling that compresses against the cornea to create divots. These bubbles can result in glare or reduced vision.
Apical touch places all lens support on the apex of the cornea, creating a zone of bearing on fluorescein assessment. Patients report good visual acuity; however, there may be an increased risk of corneal scarring with flat fitting lenses. One study demonstrates similar wearing comfort with both apical touch and apical clearance lens fitting methods.5 The three-point touch fitting method allows the contact lens to bear lightly on the apex of the cornea, with heavier bearing on the paracentral cornea. This technique is associated with good visual acuity.
Hybrids
SynergEyes Ultrahealth is a hybrid lens specifically designed for keratoconic patients. When fit properly, these lenses vault the corneal apex to inhibit movement, minimizing mechanical interactions that could lead to scarring. These lenses also provide adequate oxygen supply to the cornea.
With hybrid lenses, there is a tear pump under the lens as evidenced by the loss of sodium fluorescein underneath the lens over time.6 The beauty of hybrid lenses is that the GP center offers optimized vision, while the soft silicone hydrogel skirt centers the lens over the cornea to allow for longer-lasting comfort. Also, the GP center delivers a UVA and UVB blocker to protect eyes from the sun. Hybrids are suitable as a first-line therapy for mild-to-moderate keratoconic patients.
Piggyback Lenses
Piggyback systems consist of a corneal GP lens fit over a highly oxygen permeable, low-powered soft contact lens. Low-powered lenses are typically used due to their marginal 20% contribution of marked lens power towards the optics of the lens system.7 However, now that several other options exist to manage corneal GP lens intolerance, piggyback lenses are not often used, though they can be a good option for centration and stabilization of GP lenses. They also provide added comfort for those suffering from corneal GP lens discomfort by minimizing mechanical eyelid interaction with the GP lens edge. For those who exhibit 3 and 9 o’clock corneal staining, a piggyback soft lens may be the best solution to provide protection to the cornea.
In summary, it is important to look at all the available options and decide when each is best for a given patient, taking into account both the severity of the condition and financial circumstances. In some cases, it may still be best to stick to traditional treatment methods.
| Case Report: How Allergy Can Influence the Course of Keratoconus Case in Point. A 14-year-old Hispanic male presented to the clinic with reduced vision in his right eye that was uncorrectable to 20/20 with spectacle lenses. He reported wearing spectacle correction for myopia since age five, but had noticed the degradation in vision quality in the last two years. Patient history indicated he had been diagnosed with keratoconus at his previous comprehensive eye examination and noted a habit of eye rubbing due to ocular itching with no history of contact lens wear. The patient’s systemic history was unremarkable, as was his family’s systemic and ocular medical history. He denied taking any medications or having allergies to medications. The patient presented with the following spectacle correction: OD: -3.75 -7.75 x 013 with DVA 20/500, PH 20/100 and VVA RS200 OS: -400 DS with DVA 20/20-2 and NVA RS20-2
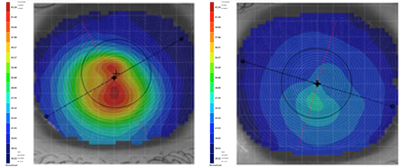
Corneal topography revealed an asymmetric bowtie with irregular astigmatism and inferior steepening present in both eyes. The overall presentation was worse in the right eye vs. the left (Figure 1). Mire distortion was evident during the patient’s corneal topography evaluation. His best-corrected spectacle distance visual acuity in the right eye was 20/150 and 20/20+2 in the left eye. Pinhole did not improve his vision in the right eye. Additionally, a biomicroscopy examination revealed the presence of Fleischer’s ring in his right cornea and Vogt’s striae in both. No other slit lamp findings commonly associated with keratoconus like stromal thinning, apical scarring or Munson’s sign were noted. No signs of ocular allergy were noted. An examination of the remainder of the anterior segment was unremarkable. The patient was fit using a corneal GP lens from a fitting set that was designed based on the Collaborative Longitudinal Evaluation of Keratoconus study. The diagnostic lenses used were a tricurve design with an overall diameter of 8.8mm with base curve radii ranging from 7.18mm to 4.50mm and variable optic zone diameters that decrease in size as the base curve steepens. The contact lens powers are variable to provide low minus over-refractions for most of the mild-to-moderate keratoconic patients.12 The secondary curve is 8.50mm for each lens, based on corneal curvatures beyond the cone being similar to the corneal curvatures of patients without keratoconus.12 The center thickness for all lenses is 0.14mm. One drop of proparacaine 0.5% ophthalmic solution was instilled in each eye to alleviate initial lens awareness during the contact lens fitting. Over-the-counter Alaway (ketotifen, Bausch + Lomb) was also prescribed for use twice a day in both eyes. No ocular allergy signs were noted at the time of the exam, though allergy drops were recommended for prophylactic use to minimize future rubbing. Preservative-free artificial tears were also prescribed to be taken as necessary. Results. After a few follow-up visits and minor adjustments to the peripheral curves, the patient’s contact lenses were finalized. Fluorescein pattern assessment demonstrated fluffy central apical touch, with mid-peripheral pooling in the right eye (Figure 2). No bubbles were noted underneath the lens. The lens decentered slightly inferiorly, but was picked up with a blink. There was 360 degrees of average peripheral edge clearance when the lens was centered on the eye. There was minimal lens movement on blink; however, movement was not a concern due to lack of corneal staining. The left lens demonstrated an alignment fit centrally with pooling noted superiorly at the edge of the optic zone but decentered slightly inferior temporally. The lens provided adequate movement on blink, and peripheral edge clearance was minimal at 9 o’clock and average at 3, 6 and 12 o’clock. |
1. Segal O, Barkana Y, Hourovitz D, et al. Scleral contact lenses may help where other modalities fail. Cornea. May 2003;22(4):308-310.
2. Bennett ES. GP Annual Report 2015. Contact Lens Spectrum. 2015;30(October 2015):24-27, 29-31.
3. Zadnik K, Barr JT, Edrington TB, et al. Baseline findings in the Collaborative Longitudinal Evaluation of Keratoconus (CLEK) Study. Invest Ophthalmol Vis Sci. Dec 1998;39(13):2537-2546.
4. Lim N, Vogt U. Characteristics and functional outcomes of 130 patients with keratoconus attending a specialist contact lens clinic. Eye (Lond). Jan 2002;16(1):54-59.
5. Edrington TB, Gundel RE, Libassi DP, et al. Variables affecting rigid contact lens comfort in the collaborative longitudinal evaluation of keratoconus (CLEK) study. Optom Vis Sci. Mar 2004;81(3):182-188.
6. Lee KL, Nguyen DP, Edrington TB, Weissman BA. Calculated in situ tear oxygen tension under hybrid contact lenses. Eye Contact Lens. Mar 2015;41(2):111-116.
7. Michaud L, Brazeau D, Corbeil ME, Forcier P, Bernard PJ. Contribution of soft lenses of various powers to the optics of a piggy-back system on regular corneas. Cont Lens Anterior Eye. Dec 2013;36(6):318-323.
8. Krachmer JH, Feder RS, Belin MW. Keratoconus and related noninflammatory corneal thinning disorders. Surv Ophthalmol. Jan-Feb 1984;28(4):293-322.
9.Cristina Kenney M, Brown DJ. The cascade hypothesis of keratoconus. Cont Lens Anterior Eye. Sep 2003;26(3):139-146.
10. Vazirani J, Basu S. Keratoconus: current perspectives. Clinical Ophthalmology. 2013;7:2019-2030.
11.Nowak DM, Gajecka M. The genetics of keratoconus. Middle East African Journal of Ophthalmology. Jan 2011;18(1):2-6.
12. Rabinowitz YS. Keratoconus. Surv Ophthalmol. Jan-Feb 1998:42(4):297-319.
13. Lema I, Duran JA. Inflammatory molecules in the tears of patients with keratoconus. Ophthalmology. Apr 2005;112(4):654-659.
14. Sharma N, Rao K, Maharana PK, Vajpayee RB. Ocular allergy and keratoconus. Indian J Ophthalmol. Aug 2013;61(8):407-409.