Even though it is not yet FDA-approved, each day in my busy practice, patients are asking me about corneal collagen crosslinking for their keratoconus. Several studies have suggested that collagen corneal crosslinking on keratoconic eyes after intrastromal corneal ring implantation had an additive effect in improving best-corrected visual acuity and reducing steep keratometry measurements.
Keratoconus is a noninflammatory, self-limiting disease in which the cornea becomes progressively thinner, more distorted and steeper in curvature, usually beginning in adolescence. The abnormal curvature causes changes in the cornea’s refractive power in both myopia and astigmatism. It is typically bilateral but asymmetric. The prevalence is between 50 and 230 per 100,000 and a reported annual incidence of 2/100,000.1
In early keratoconus, patients can be corrected with glasses, but as the disease progresses, contact lenses are needed to reduce distortion and provide better vision. When patients are no longer able to wear contact lenses, surgical procedures such as penetrating keratoplasty or deep anterior lamellar keratoplasty have been used to restore vision. Although surgical procedures have improved over time, limitations can include immunologic rejection, graft failure, side effects from chronic topical steroids and high post-operative astigmatism.
More recently Intacs (Addition Technology) and corneal collagen crosslinking have been used to treat patients with keratoconus and other corneal ectasias. In this article, I will introduce the novel approach of combining the two procedures.
The History of Intacs
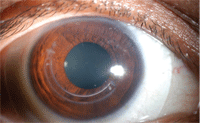
Intac post removal with scleral contact lens.
Intacs are arclike, polymethylmethacrylate (PMMA) instrastromal corneal ring (ISCR) segments that are surgically inserted into the deep corneal stroma.2 The FDA first approved Intacs in 1999 for the surgical treatment of mild myopia (-1.00D to -3.00D). Intacs act as a passive spacing element that separates corneal lamellae. The arc length of the anterior corneal surface is shortened, which flattens the central cornea. Thus, the prolate shape of the cornea is maintained over the central optical zone. Since 2004, Intacs have been FDA approved to treat keratoconus in the United States. Intacs come in many different sizes and there are potentially many different combinations that can be used to flatten the central cornea and reduce astigmatism.3 Outside of the United States, Ferrara rings (Mediphacos) and Bisantis segments (Optikon 2000) are also available. In cross-section, Intacs are hexagonal, Ferrara rings are triangular and Bisantis segments are oval.
The surgical procedure involves creation of corneal tunnels at about 70% of the corneal depth, creating a corneal pocket on each side of the incision, inserting Intacs segments in the respective corneal tunnels and then suturing the incision sites.2 The segments are separated by approximately 2.0mm. These pockets have been typically created using a mechanical spreader; however, femtosecond laser has been used recently to create channels instead.4,5
Several advantages of using femtosecond lasers include more rapid channel creation, more precise channel creation and easier channel creation, and centration. In addition, there is less risk for epithelial defects during channel creation, lower risk for posterior corneal perforation and reduced risk of infectious keratitis due to the absence of a foreign element being placed in the cornea. The femtosecond laser shows a better reduction in average keratometry, spherical equivalent, best-corrected visual acuity, uncorrected visual acuity and surface asymmetry index—versus the mechanical spreader.6
 Patients with keratoconus tend to have an inferior cone with steepening and flattening of the superior cornea. If double ISCR segments are inserted, the cornea is flattened both inferiorly and superiorly, which does not address the issue of asymmetric astigmatism. However if a single ISCR is inserted, the cornea is flattened inferiorly and steepened superiorly. This may benefit patients with keratoconus to improve uncorrected visual acuity and best spectacle-corrected visual acuity.7,8 It can also reduce irregular astigmatism.9
Patients with keratoconus tend to have an inferior cone with steepening and flattening of the superior cornea. If double ISCR segments are inserted, the cornea is flattened both inferiorly and superiorly, which does not address the issue of asymmetric astigmatism. However if a single ISCR is inserted, the cornea is flattened inferiorly and steepened superiorly. This may benefit patients with keratoconus to improve uncorrected visual acuity and best spectacle-corrected visual acuity.7,8 It can also reduce irregular astigmatism.9
What is CXL?
Investigations into the possibility of inducing crosslinking in the corneal stroma as a conservative treatment for keratoconus began in the mid-1990s. Eberhard Spoerl, Ph.D., and Theo Seiler, M.D., Ph.D., showed that the biomechanical behavior of the cornea could be altered by irradiation using ultraviolet light with photosensitizers and by aldehyde reactions.10 Crosslinking is used frequently within the polymer industry to harden materials and within bioengineering to stabilize tissue. Drs. Spoerl and Seiler treated porcine corneas with glutaraldehyde, Karnovsky’s solution (glutaraldehayde and paraformaldehyde) or riboflavin and UV-irradiation. These treatments caused increased corneal stiffness. Riboflavin is a water soluable non-toxic photosensitizer made of vitamin B2. It can penetrate easily into the corneal stroma in the absence of the corneal epithelium.
Gregor Wollensak, M.D., and colleagues were the first to develop and introduce corneal collagen crosslinking (CXL) in 2003.11 In patients with preoperative progressive keratoconus, CXL appeared to halt the progression of corneal ectasia.11 CXL causes flattening of keratometry measurements and improvements of uncorrected and best-corrected visual acuity.11,12 Untreated eyes had further steepening of keratometry readings and worsening of best-corrected visual acuity.13
The treatment procedure for CXL starts by applying a topical anesthetic, then removing 7mm of the central corneal epithelium to allow a uniform diffusion of riboflavin into the stroma.14 A riboflavin 0.1 % solution is then applied prior to UVA irradiation to act as a photosensitizer and a UV blocker.14 Homogenous UV irradiance of 3mW/cm2 and wavelength of 370nm is used for 30 minutes to irradiate the cornea. An antibiotic ointment is applied post-treatment until the cornea has reepithelialized.11
Crosslinking can also be performed without epithelial debridement (C3R). Studies are currently being done to determine if the epithelium should be partially or completely removed during the crosslinking procedure. Leaving the epithelium intact allows for a shorter and more comfortable procedure and postoperative healing. The risk of infection may also be reduced. However, C3R may make the procedure longer since it may take more time to get enough riboflavin into the corneal stroma.

Epithelial erosion over Intac with CXL.
However, epithelial debridement may be needed in order to achieve stromal saturation of riboflavin during the procedure.11 Different techniques are currently being explored to make the epithelium more permeable. These can range from scratching the epithelium to chemically treating the epithelium with topical anesthetics or preservatives in order to facilitate the large riboflavin molecule to go through the epithelium more readily.
General C3R is a safe and effective procedure. Since 85% to 90% of UVA radiation is absorbed in the anterior 400μm of the cornea, CXL is not recommended for patients with corneas thinner than 400μm.14
Combining Intacs and CXL
A recent study compared inferior-segment Intacs without corneal collagen cross-linking (Intacs-only) with inferior segment Intacs placement combined with corneal collagen crosslinking (Intacs with C3R).15 The Intacs with C3R group had significantly less astigmatism than the Intacs-only group. Both steep keratometry and average topographic keratomety measurements were significantly reduced in the Intacs with C3R group. In addition, the lower-upper (L-U) ratio—a topographic measure of the degree of keratoconus—was examined. This ratio was significantly reduced in the Intacs with C3R group.15
A different study examined 25 eyes—of which 17 eyes with bilateral keratoconus had Intacs implantation with subsequent corneal cross-linking treatment.3 The Intacs with CXL group had significant improvements in uncorrected (1.9 Snellen lines) and best-corrected (1.7 Snellen lines) visual acuity. Spherical visual acuity was improved, cylinder was reduced and mean keratometry values were reduced after Intacs and CXL treatment. Thus, it seems that Intacs with CXL is an effective procedure in keratoconic eyes that improves the effect of Intacs; it is as an enhancement or stabilizing procedure.

Riboflavin (yellow) in corneal stroma with intact epithelium.
Choosing the Right Patient
Candidate selection is important when selecting a patient for Intacs with corneal collagen crosslinking. Patient expectation is a key component to success; it is important to keep our patients informed of the latest technologies.
Patients currently recommended for Intacs are individuals who are contact lens intolerant and have mild to moderate keratoconus with a clear visual axis, maximum steep keratometry readings in the range of 55.00D to 57.00D and a minimum corneal thickness of at least 450μ over the area where the Intacs will be inserted.17-20 Best-corrected visual acuity greater than 20/32(-2), astigmatism less than 3.50D and spherical myopia greater than 1.75D predict better results.19
The predictive factor for success in post-Intac keratoconic eyes is two-fold: relatively low mean keratometry values—less than or equal to 53.00D—and a relatively low spherical equivalent. Intacs improved visual acuity, the quality of corneal topography and significantly reduced the spherical equivalent. It is suggested that, in advanced keratoconus with mean K readings more than or equal to 55.00D, a poor outcome is indicated.20
The failure rate, or percentage of eyes with continued progression after C3R, was determined to be 7.6%.21 Risk factors for failure include age older than 35, entering best-corrected visual acuity with spectacles better than 20/25 and a maximum keratometry reading greater than 58.00D.21 Thus, younger patients with flatter keratometry measurements would be better candidates for this procedure.
Postoperative Findings
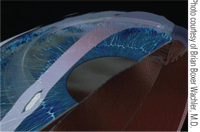
Cross-sectional graphic of cornea with Intacs in deep stroma.
When comanaging patients with Intacs, several complications can occur. Although rare, intraoperative complications occurred in 2% of eyes in a European multicenter study of intrastromal corneal ring segments in 2001.22 Complications included two incisional gapes, removal of one intrastromal corneal ring due to a non-healing incision and a single channel infection. Epithelial cysts at the incision site and a diffuse haze under the stromal tunnel medial and lateral to the segments may also be present. These findings didn’t affect visual outcome.
Foreign body sensation and photophobia may occur after intrastromal ring segments.22 Glare may be present in the first two months, but typically, all visual symptoms resolve by 12 months. Corneal thinning may occur infrequently over the ring segments.22,23 Rarely, corneal melting and severe corneal infiltration may occur.24 Infectious keratitis following intrastromal ring segments is rarely reported. Infection may occur as a result of a loose stitch or a wound gape due to migration of the segment to the site of the wound.25-29
Postoperative CXL
In a 2003 study by Drs. Wollensak and Spoerl, postoperative CXL healing was generally unremarkable with the exception of slight transient stromal edema until corneal reepitheliazation.11 There was no corneal scarring, persistent corneal epithelial defects or changes in endothelial cell density. Corneal and lens transparency were not altered and there was no evidence of cataract formation. Retinal damage was not observed with CXL, nor did it affect contact lenses wear postoperatively.
There are several findings to be aware of when comanaging CXL. Stromal haze has been reported after CXL treatment.28 The stromal haze developed between the second and third postoperative months and was resistant to topical steroids. Stromal haze was unchanged at postoperative month six and did not impair best-corrected visual acuity postoperatively. Confocal analysis preoperatively of these two patients showed reticular hypo-reflective microstriae. Postoperative confocal analysis demonstrated an increase in keratocyte population at 170-200μm.
An alternate study demonstrated that 14 of 163 eyes developed significant stromal haze after C3R.29 This haze impaired uncorrected visual acuity and best-corrected visual acuity. However corneas were thinner prior to CXL in the haze group—420μm compared with 478μm in the control group. The haze may be associated with the depth of the crosslinking procedure and the amount of keratocyte loss.14,28 Patients with advanced keratoconus are at higher risk of haze development due to thinner corneas and steeper corneal curvatures.28
Another finding after C3R is a thin stromal demarcation line over the entire cornea at a depth of approximately 300μm.21 The demarcation line is visible beginning two weeks after treatment and does not cause any changes in the corneal endothelium, the lens or intraocular pressure. The stromal demarcation line may be due to changes in the refractive index between the untreated and treated cornea or may be due to the reflection properties of treated and untreated corneas.28 Sterile infiltrates and central stromal scars may be present in patients after CXL.21
It is truly rewarding to be able to counsel and treat patients with their complicated corneal conditions. In my experience, contact lens wear has been successful after Intacs and CXL. Contact lenses combined with Intacs have been demonstrated to be effective in postponing penetrating keratoplasty, even in patients with advanced keratoconus.30
The combined procedure may be able to delay or avoid corneal grafts in keratoconus patients. It may also be able to create a cornea more receptive to contact lenses and improve the functional refraction with contact lenses.
After the combined procedure, the refractive error of the patient needs to be addressed and a refraction for glasses or contact lenses should be performed. Keep in mind that the curvature of the cornea may change and repeated refractions and contact lens adjustments need to be performed.
Melissa Barnett, O.D., is a senior optometrist at the UC Davis Medical Center in Sacramento, where she performs primary and medical eye examinations and fits contact lenses, including specialty contact lenses, in addition to teaching optics and contact lenses to ophthalmology residents. She lectures and has been published on topics including dry eye, anterior segment disease, contact lenses and creating a healthy balance between work and home life for women in optometry.
1. Kennedy RH, Bourne WM, Dyer JA. A 48-year clinical and epidemiologic study of keratoconus. Am J Ophthalmol. 1986 Mar;101(3):267-73.
2. Colin J, Malet FJ. Intacs for the correction of keratoconus: Two-year follow-up. J Cataract Refract Surg. 2007 Jan:33(1):69-74.
3. Rabinowitz YS. Intacs for keratoconus. Int Ophthalmol Clin. 2006;46:91-103.
4. Carrasquillo KG, Rand J, Talamo JH. Intacs for keratoconus and post-LASIK ectasia: Mechanical versus femtosecond laser-assisted channel creation. Cornea. 2007 Sep;26(8):956-62.
5. Ertan A, Colin J. Intracorneal rings for keratoconus and keratectasia. J Cataract Refract Surg. 2007 Jul:33(7):1303-14.
6. Rabinowitz YS, Li X, Ignacio TS, et al. Intacs inserts using the femtosecond laser compared to the mechanical spreader in the treatment of keratoconus. J Refract Surg. 2006 Oct;22(8):764-71.
7. Colin J, Cochener B, Savary G, et al. Intacs inserts for treating keratoconus: one-year results. Ophthalmology. 2001 Aug;108(8):1409-14.
8. Alió JL, Artola A, Hassanein A, et al. One or 2 Intacs segments for the correction of keratoconus. J Cataract Refract Surg. 2005 May;31(5):943-53.
9. Boxer Wachler BS, Christie JP, Chandra NS, et al. Intacs for keratoconus. Ophthalmology. 2003 May;110(5):1031-40.
10. Spoerl E, Huhle M, Seiler T. Induction of cross-links in corneal tissue. Exp Eye Res. 1998 Jan;66(1):97-103.
11. Wollensak G, Spoerl E, Seiler T. Riboflavin/ultraviolet-A-induced collagen crosslinking for the treatment of keratoconus. Am J Ophthalmol. 2003 May;135(5):620-7.
12. Vinciguerra P, Albe E, Trazza S, et al. Intraoperative and postoperative effects of corneal collagen cross-linking on progressive keratoconus. Arch Ophthalmol. 2009 Oct;127(10):1258-65.
13. Wittig-Silva C, Whiting M, Lamoureux E, et al. A randomized controlled trial of corneal collagen cross-linking in progressive keratoconus: preliminary results. J Refract Surg. 2008 Sep;24(7):S720-5.
14. Spoerl E, Mrochen M, Sliney D, et al. Safety of UVA-riboflavin cross-linking of the cornea. Cornea. 2007 May;26(4):385-9.
15. Chan CC, Sharma M, Wachler BS. Effect of inferior-segment Intacs with and without C3R on keratoconus. J Cataract Refract Surg. 2007 Jan;33(1):75-80.
16. Ertan A, Karacal H, Kamburoglu G. Refractive and topographic results of transepithelial cross-linking treatment in eyes with Intacs. Cornea. 2009 Aug;28(7):719-23.
17. Colin J, Cochener B, Savary G, et al. Correcting keratoconus with intracorneal rings. J Cataract Refract Surg. 2000 Aug;26(8):1117-22.
18. Colin J, Cochener B, Savary G, et al. INTACS inserts for treating keratoconus: one-year results. Ophthalmology. 2001 Aug;108(8):1409-14.
19. Levinger S, Pokroy R. Keratoconus managed with intacs: one-year results. Arch Ophthalmol. 2005 Oct;123(10):1308-14.
20. Alió JL, Shabayek MH, Belda JI, et al. Analysis of results related to good and bad outcomes of Intacs implantation for keratoconus correction. J Cataract Refract Surg. 2006 May;32(5):756-61.
21. Koller T, Mrochen M, Seiler T. Complications and failure rates after corneal crosslinking. J Cataract Refract Surg. 2009 Aug;35(8):1358-62.
22. Ruckhofer J, Stoiber J, Alzner E, et al. One year results of European multicenter study of intrastromal corneal ring segments. Part 2: Complications, visual symtpoms, and patient satisfaction. J Cataract Refract Surg. 2001 Feb;27(2):287-96.
23. Zare MA, Hashemi H, Salari MR. Intracorneal ring segment implantation for the management of keratoconus: safety and efficacy. J Cataract Refract Surg. 2007 Nov;33(11):1886-91.
24. Chalasani R, Beltz J, Jhanji V, et al. Microbial keratitis following intracorneal ring segment implantation. Br J Ophthalmol. 2010 Aug 1 [Epub ahead of print].
25. Spoerl, Wollensak G, Seiler T. Increased resistance of cross linked cornea against enzymatic digestion. Curr Eye Res. 2004 Jul;19(4):474-6.
26. McAlister JC, Ardjomand N, Ilari L, et al. Keratitis after intracorneal ring segment insertion for keratoconus. J Cataract Refract Surg. 2006 Apr;32(4):676-8.
27. Bourcier T, Borderie V, Laroche L. Late bacterial keratitis after implantation of intrastromal corneal ring segments. J Cataract Refract Surg. 2003 Feb;29(2):407-9.
28. Mazzotta C, Balestrazzi A, Baiocchi S, et al. Stromal haze after combined riboflavin-UVA corneal collagen cross-linking in keratoconus: in vivo confocal microscopic evaluation. Clin Experiment Ophthalmol 2007 Aug;35(6):580-2.
29. Raiskup F, Hoyer A, Spoerl E. Permanent corneal haze after riboflavin-UVA-induced cross-linking in keratoconus. J Refract Surg. 2009 Sep;25(9):S824-8.
30. Uçakhan OO, Kanpolat A, Ozdemir O. Contact lens fitting for keratoconus after Intacs placement. Eye Contact Lens. 2006 Mar;32(2):75-7.


