 If ever a topic could instantly generate debate, and perhaps a little fear in the hearts of optometrists, it is steroids. In a recent “Controversies in Care” online webinar, panelists Joseph Shovlin, O.D., and William Potter, O.D., with additional contributions from Paul Karpecki, O.D., tackled this thorny issue—delving into the pros and cons of steroid use in patients with corneal compromise (e.g., inflammation or marginal keratitis), the effectiveness of steroid-antibiotic regimens and the impact of the SCUT trial.
If ever a topic could instantly generate debate, and perhaps a little fear in the hearts of optometrists, it is steroids. In a recent “Controversies in Care” online webinar, panelists Joseph Shovlin, O.D., and William Potter, O.D., with additional contributions from Paul Karpecki, O.D., tackled this thorny issue—delving into the pros and cons of steroid use in patients with corneal compromise (e.g., inflammation or marginal keratitis), the effectiveness of steroid-antibiotic regimens and the impact of the SCUT trial.
To kick off the night, audience members were asked how often they prescribe topical steroids. The results showed that a good percentage regularly do: 7% said never, 30% fewer than five times a month, 47% more than five times but less than 20 times a month, and 17% said more than 20 times a month.
“From a medical standpoint, I’ve never seen anyone get faulted for not using a steroid, only for using a steroid inappropriately,” said Dr. Shovlin.
Corneal Inflammatory Events
Dr. Shovlin started the night’s conversation by mentioning the increasingly frequent occurrence of corneal inflammatory events (CIEs).
“With silicone hydrogel lenses, dryness seems to be a pretty common issue,” added Dr. Potter. “When dryness is involved, you certainly get a sequestering of dirt and germs and toxins, and that makes these events a little bit more likely.”
He then mentioned that confocal microscopy can show an up-regulated immune system in the corneas of silicone hydrogel wearers. While its clinical impact is yet to be determined, this does show that immune systems react to the silicone hydrogel modality, he said.
Dr. Shovlin noted that the relative risk is tenfold if using an MPDS vs. a peroxide-based system. More interesting, he said, is what’s growing in the lens case; work by his group found two gram-negative bugs—Stenotrophomonas and Achromobacter. Dr. Shovlin and colleagues then took those isolates and exposed them to Opti-Free Replenish (Alcon), Revitalens (AMO) and Biotrue (Bausch + Lomb).1 They recorded a significant log reduction in those organisms initially, but after six hours the bugs regrew in Opti-Free Replenish. Therefore, the ideal procedure is to follow lens care basics of rubbing and rinsing, and adhering to a lens case replacement schedule.
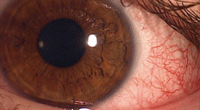
Corneal inflammatory event.
In response to an audience question on whether practitioners are seeing the same results with Opti-Free PureMoist (Alcon), Dr. Shovlin said reports are mixed but the re-addition of EDTA (previously in Opti-Free Express), may “soften” the cell membrane in gram-negative bugs and allow the disinfectants to be more robust.
How best to treat CIEs? Dr. Potter said he uses a short course of topical ciprofloxacin, and a soft steroid q.i.d. for the first week and b.i.d. for the second week, because the duration of the infection—if it is an infection at all—is much shorter than the inflammatory process. Dr. Shovlin’s go-to treatment is a combination of tobramycin and dexamethasone q.i.d., and he successfully gets patients back in lenses within seven to 10 days.
The SCUT Trial
Steroids are not as clinically effective in bacterial keratitis as initially thought, but also not as bad as once considered—that’s the takeaway from the SCUT trial, said Dr. Shovlin. Therefore, there may be a role for steroids in certain cases (i.e., a central corneal ulcer) but not as a matter of routine. The study also found that steroids should not be used in Nocardia infections, and that MIC values do correlate with clinical results. He stressed that this guidance has limitations, and there are always outliers and exceptions.
“The questions it raises is in the subgroup analysis, since different strains of Pseudomonas might respond differently,” added Dr. Potter. “Next time around, the authors are going to look harder at the subgroups, especially the bacterial strains, which might give a better guide as to whether it is worthwhile to use steroids or not.”
Audience members were then asked when they are inclined to add steroids to a bacterial corneal ulcer. Only 3% would do so at the onset of the diagnosis, 30% at the 24-hour point with some initial improvement (as recommended by the SCUT trial), 35% only after 72 hours and the culture and sensitivity results are in, and 32% would not if the patient is showing improvement without steroids.
Interestingly, following the release of SCUT, 47% of those polled said the results had no impact on their prescribing patterns for bacterial corneal ulcers, while 27% would be more likely and 26% would be less likely to do so.
EKC Management
Because these patients often present while actively using steroids, the decision can be out of the clinician’s hands. Dr. Potter is more reluctant to start steroids in EKC unless he sees the three indicators: central infiltrate interfering with vision, intractable pain and the presence of a pseudomembrane. In the absence of those, he treats without steroids, but follow-up is vital; infiltrates develop seven days after the onset of initial symptoms and supportive care is not really going to address the discomfort. Dr. Shovlin stressed that although you cannot be punished for not using steroids, if you see any of the three indicators, steroids are the most effective way to alleviate the patient’s symptoms.
The audience agreed. A majority (47%) would use topical steroids only for pain, central infiltrates and/or pseudomembranes and 26% would wait to see how the disease progresses, while 18% said they would always use topical steroids for EKC and 8% said they would never prescribe steroids as it prolongs the clinical course.
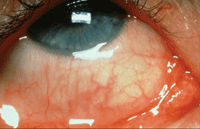
Allergic conjunctivitis.
Which steroid should you use? Dr. Potter would usually opt for soft steroids—fluorometholone or loteprednol—but for more severe cases or in the presence of a pseudomembrane, he would put patients on Pred Forte (prednisolone acetate, Allergan). He said he would remove the pseudomembrane if possible.
Intraocular Pressure
Dr. Potter brought up the classic 1963 study by Armaly that found that a third of normal patients and 90% of glaucoma patients respond to steroid use with a greater than 6mm Hg rise in intraocular pressure. The takeaway here, he said, is that prednisone has better penetration and may be more potent in raising intraocular pressure. In uveitis, for example, the regimen would not be q.i.d., but rather q2h or qh.
“Identifying a steroid response is not the most terrible thing that can happen,” he added. “You have really done your patient a favor by identifying them as a potential glaucoma patient in future years.”
In response to an audience question on treatment of steroid responders, Dr. Shovlin said he typically uses a steroid like Durezol (difluprednate, Alcon) initially, so there is potential for some impressive pressure spikes. He usually adds a topical aqueous suppressant when not contraindicated. However, he did warn that it is sometimes quite frustrating to get insurance coverage for some of these treatments.
Allergy
Last but not least, Dr. Potter gave three factors that would prompt him to use steroids in an allergic conjunctivitis patient: (1) work or school performance being disrupted significantly, (2) a high Rx contact lens such as a keratoconus patient, and (3) when making a clinical distinction between a histamine-mediated process vs. an eosinophil-type process. “We have to make sure we are dealing with allergy. It works on a higher order cascade effect—it is the echelon of therapy,” said Dr. Shovlin.
Dr. Potter added a cautionary note: Steroids should improve allergies almost immediately, so if you do not see a change, reconsider the diagnosis.
A special thank you to our active audience who participated throughout the evening. We welcome you to join us for future conversations. To learn more about this event, go to www.reviewofcontactlenses.com/controversies-in-care.
1. Kilvington S, Shovlin J, Nikolic M. Characterization Of bacteria from contact lens storage cases Of corneal infiltrative event patients. Poster presented at ARVO; May 6-9, 2012, Ft. Lauderdale, Fla.


