 |
This 18-year-old male has an ocular history of congenital Marfan’s syndrome and Axenfeld-Rieger syndrome with bilateral dislocated lenses and iris hypoplasia. At age nine he suffered a large retinal tear, underwent a pars plana vitrectomy (PPV) repair and subsequently developed aphakic glaucoma. In the right eye, he was treated for lattice degeneration with a 360-degree laser, providing him good vision in that eye at 20/30.
Prednisolone was prescribed, which improved but did not resolve the granuloma. Surgical resection was discussed, but because he would need to be without the comfort-giving scleral device until healed, he opted for impression technology using an elevation-specific scleral design. An impression of the ocular surface was obtained using a polyvinylsiloxane mold and a custom scleral device was designed to shield and cover the granuloma. A few months later, the granuloma had completely resolved.
Recently, he developed a choroidal neovascular membrane in the right eye and began treatments with Avastin (bevacizumab, Genentech). He subsequently developed a non-clearing vitreal hemorrhage requiring PPV. Unfortunately, he developed a worsening anterior staphyloma and was referred for a patch graft consult and vision assessment.
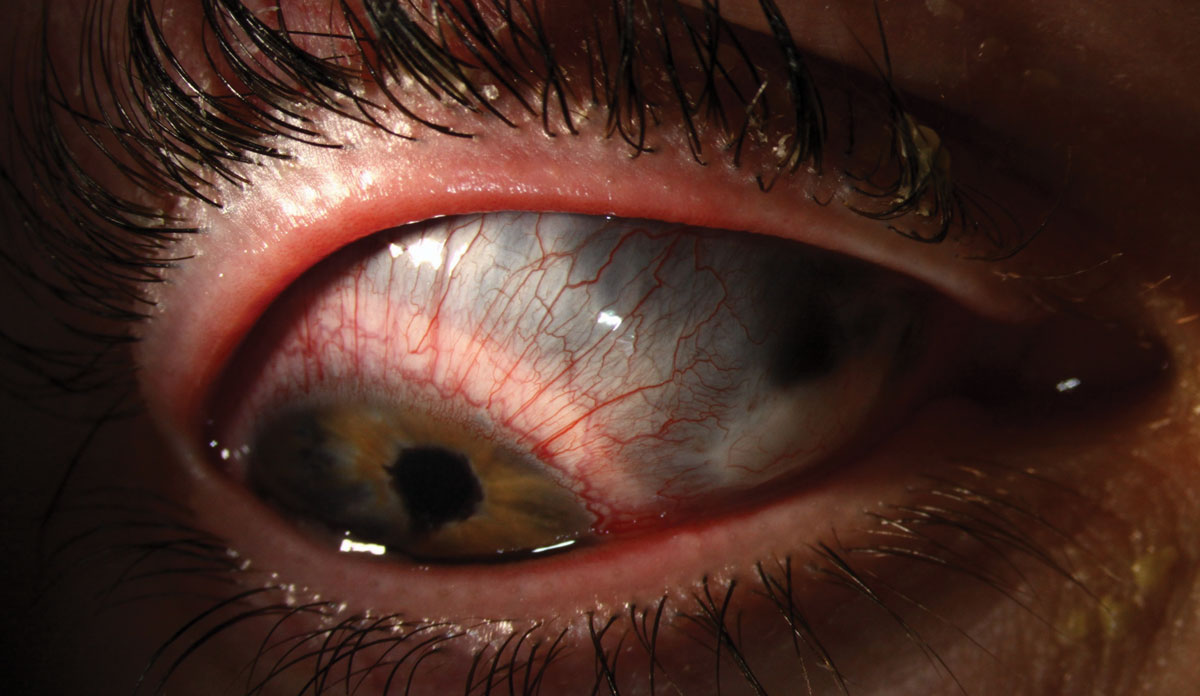
Staphylomas result from intraocular pressure pushing the uvea into an ectatic sclera.1 This causes the sclera to have a bluish or even blackish appearance as the underlying pigmented tissue becomes visible through the thinning scleral tissue. While posterior staphylomas are generally congenital, anterior staphylomas develop in response to trauma, such as surgery, or infection, as with fungal ulcers.1,2 Anterior staphylomas are generally located over the ciliary body (ciliary staphyloma) or between the ciliary body and the limbus (intercalary staphyloma).
Although reinforcement surgery with a scleral patch graft is the usual course of action in staphyloma, it was contraindicated in this case because of the size of the thinned area and the risk of intraocular bleeding. Surprisingly, however, he pinholed to his baseline visual acuity. Refraction yielded lower plus power with a significant increase in astigmatism, providing him 20/80 vision.
While a contact lens correction, including the option of a scleral lens fit, would likely yield better optics, it is contraindicated in this case secondary to the risk of perforation. Safety goggles were prescribed.
 |
| Click photo to enlarge. |
1. (Corneal) Staphyloma, Anterior. Am J Neuroradiol. www.ajnr.org/ajnr-case-collections-diagnosis/corneal-staphyloma-anterior. Accessed January 30, 2019. 2. Grieser EJ, Tuli SS, Chabi A, et al. Blueberry eye: acquired total anterior staphyloma after a fungal corneal ulcer. Cornea. 2009;28(2):231-2. |


