During a recent contact lens examination, I asked my patient for information regarding her current contact lens prescription. She happily handed me a box of daily disposables that had expired four years earlier. There were still lenses remaining. As a patient, she was excited at the money she had saved by stretching out her prescription over this extended time period. As a clinician, I instantly imagined everything that could have gone wrong.
Unfortunately, this scenario is an all too familiar one. Despite the introduction of products such as daily disposable lenses and “all in one” multipurpose solutions, compliance remains a metaphorical elephant in the room. Historically, compliance with contact lens wear has been estimated to range from 40% to 70% among adult wearers.1 These rates of noncompliance are likely greatly underestimated due to the methodology used to ascertain actual compliance. In support of this argument, recent studies in the US and abroad suggest that optimal compliance with practitioner recommended daily lens wear is closer to 1% for all soft lens wearers.2,3
Several factors have been proposed as contributors to noncompliance. These include cost, regimen complexity, frequency and duration of use, and the nature of the condition.4 The last of these, which includes asymptomatic lens wear, can fuel patient misconceptions regarding the safe wear and care of contact lenses. While patient education and attitudes are paramount in achieving compliant contact lens use, successful patient education continues to fall short and truly effective strategies to change behavior appear to be non-existent.
Compliance with Lens Wear and Care Regimens
Noncompliance has been shown to occur with most, if not all, steps involved with lens wear and care regimens. Evaluation of adherence to standard of care contact lens practices indicates that the average lens wearer only performs 50% or fewer of the steps correctly.3 This includes complying with recommended lens replacement frequencies, sleeping in lenses prescribed for daily wear, inappropriate use of cleaning and disinfection solutions, failing to rub and rinse lenses, and poor hand and lens case hygiene.
Frequent replacement lenses account for the majority of the soft lens market. Amongst all frequent replacement modalities, two-week disposable lenses have consistently been shown to carry the highest rate of noncompliance, with an average wearing period 2.6x longer than the recommended replacement frequency.5 For many, cost is the primary concern. Not surprisingly, stretching lenses to reduce cost is a major contributor driving this noncompliant behavior.
| |
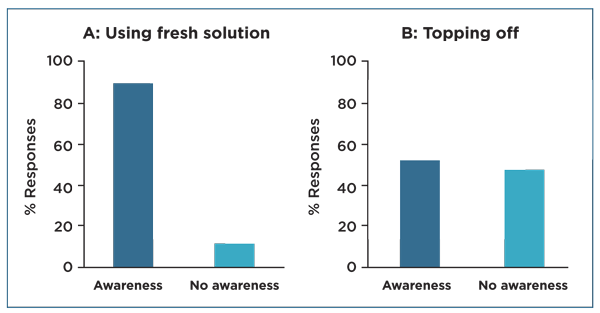
| Fig 1. Solution IQ. Respondents correctly identified the need to use fresh solution daily (A), but demonstrated reduced awareness of risk with topping off (B). Adapted from Robertson et al.3 |
However, a recent study of 1,000 lens wearers in Japan indicates that patient misconceptions about lens safety also play a role. In this study, more than 60% of lens wearers cited “no harm in extending the duration of use” as the most common reason for noncompliance with recommended replacement schedules.6 But is noncompliance with lens replacement schedules a risk factor for lens-related complications? Work by Dumbleton and colleagues indicate that it is. In their study of 501 contact lens wearers, they reported that the rate of contact lens-related adverse events was higher for patients who wore their lenses for longer than the recommended replacement interval and for those who failed to rub and rinse their lenses during cleaning.5
While daily disposable lenses that eliminate the need for care solutions and lens storage cases have the highest rate of replacement frequency compliance, they do not eliminate risk completely. Epidemiological studies from the UK have confirmed that inappropriate use of this modality can result in severe corneal infection and suggest that the incidence may be the same, if not higher, than with other frequent replacement modalities.7
In addition to replacing lenses at prescribed intervals, correct use of care solutions and exposure to water remain problematic. Following the 2006 outbreak of Fusarium keratitis, solution re-use or “topping off” was identified as a risk factor for lens-related microbial keratitis.8 A survey of established lens wearers in the Dallas-Fort Worth area also identified topping off solutions in the lens case as a key area where patient education is lacking (Figure 1).3
In this study, approximately 90% of established lens wearers correctly recognized the importance of using fresh cleaning solution daily and, more importantly, reported routinely using fresh solution. The disappointing and unsettling finding, however, was that half of the lens wearers queried failed to understand the need for discarding the used solution already present in the lens case, prior to adding new. Re-using old solution creates a one-two punch—both lowering disinfection efficacy and providing a moist environment that fosters growth of the case’s microbial inhabitants.
 |
|
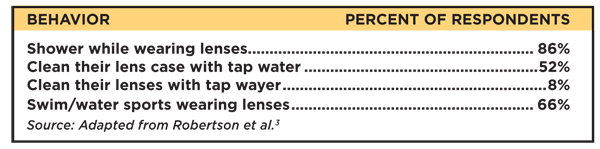
| Table 1. Behaviors Associated with Water Exposure |
Since the first reported case of Acanthamoeba keratitis (AK) in South Texas in the 1970s, water exposure during contact lens wear remains a major risk factor for infection. Although water exposure to soft lenses during wear from swimming and showering is more common than not, and many patients use tap water to rinse their lens cases on a routine basis, the overall incidence of lens-related AK remains low at around one to 33 cases per million contact lens wearers per year in developed countries. This low incidence may account in part for the lack of patient knowledge of the risks associated with water and their subsequent behaviors (Table 1).3 This represents an important area for patient education by eye care practitioners for both soft and rigid lens wearers. While Acanthamoeba infections are infrequent among this latter group, they can and do occur, and the consequences are dire.9
Don’t Forget the Lens Case
Contact lens storage cases serve as a reservoir for infectious microorganisms. Contributors to the high bacterial load include failure to replace the lens case on a routine basis and inadequate hygiene practices. In a study of over 700 lens wearers in the US, Hickson-Curran and colleagues reported a median cleaning frequency of two to three times per week, with one third of patients cleaning their lens case monthly or less often.10 Cleaning of the lens case with water has also been associated with higher rates of gram-negative contamination.11
Microbial contamination of the lens case often results in biofilm formation, the encasement of bacteria within a protective extracellular polysaccharide matrix. Currently available contact lens care solutions have limited efficacy against bacterial biofilms formed on lens surfaces and in lens cases.12,13 These heavy biofilms require mechanical removal, either through rubbing and rinsing or tissue wiping, to effectively remove them and facilitate disinfection.14
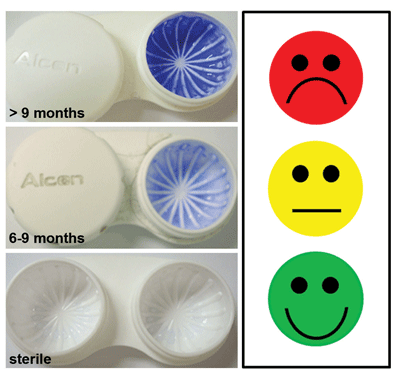
One of the biggest challenges eye care practitioners face when trying to promote cleaning and replacement of the lens storage case is the absence of visual signs of contamination. This buildup can be readily visualized by staining with crystal violet, a histologic stain that labels protein and DNA, the primary constituents of cellular debris. As shown in Figure 2, staining of lens storage cases collected across our university campus showed an increase in crystal violet staining that paralleled the age of the lens case.15 When compared against sterile, unused cases, lens cases older than six months all demonstrated some level of staining. The phenomenon was further increased after one year of use.
|
|
| Fig 2. Crystal violet staining of lens storage cases. Staining of cases was evident as early as six months. Cases older than nine months showed dramatic increases in staining intensity. Adapted from Burnham et al.15 |
Using the stoplight approach demonstrated in Figure 2, we can categorize levels of contamination as viewed by crystal violet, making it readily visible for patients and offering an ideal interventional strategy for eye care practitioners to address lens case cleaning and replacement.
Tell Patients: Compliance Matters
Proposed strategies to enhance patient compliance have included the use of both verbal and written instructions, the use of visual aids such as photographs to reinforce proper instruction, and repetition and frequent monitoring of compliance at annual and aftercare exams.16 Effective hand washing techniques should be reinforced at all visits. Regularly spaced self-review exercises on appropriate lens handling techniques have been shown to enhance lens case hygiene; however, this strategy had little effect on other aspects of lens care.17
Examination of lens case contaminants in a population of lens wearers participating in clinical research also has confirmed that patient education results in an improvement in lens case hygiene and is more effective when presented in written form as opposed to verbal instructions.11 Whether these changes persist long term and result in true behavioral modification requires further investigation.
Unfortunately, education alone isn’t likely to exert a measurable change in patient attitudes and behavior with their contact lens wear and care practices. It is well established that the majority of lens wearers exhibit noncompliant behaviors. As with other medical practices, awareness of risk factors associated with contact lens wear is not a major deterrent to poor behavior.3
Interventional approaches may be more effective. In his review of patient education and compliance, McMonnies advises that the optimal time to review wear and care procedures is during an exam for a red eye or when a patient complains of persistent irritation or discomfort during lens wear.18 He argues that a patient whom is symptomatic and receives an explanation for those symptoms may be more motivated to enhance their compliance. In support of an interventional approach, we found that patients were more likely to report replacing their lens case if they had experienced a prior contact lens-related complication.1
McMonnies also advocates the use of practice newsletters and group emails. Along these lines, emails or text messages may serve as a useful adjunct to remind patients to replace their lenses or their lens storage case. The implementation of newly designed blister packs (such as the Magic 1-day Menicon Flat Pack) as a countermeasure to poor hand hygiene may be beneficial in reducing the introduction of bacterial contaminants to the eye.19 However, even these would require a strict level of compliance with removal of the lens from the blister pack followed by direct insertion into the eye as further lens manipulation by hand would override any beneficial effect.
Another potentially useful strategy to promote good behavioral patterns is the use of a subscription membership system, where members pay an annual fee and receive a continuous supply of lenses throughout the year, as needed.20 The effectiveness of a subscription-based system, as recently evaluated in the Japanese market, has been shown by an increase in lens replacement frequency by members when compared to non-members and a corresponding reduction in the rate of non-severe ocular complications associated with lens wear.
As the indications for contact lenses continue to expand with the development of new designs and technologies, so too will the need for increased compliance with contact lens wear and care regimens. While some areas of lens care may benefit from increased education, new innovative strategies geared towards modification of attitudes, perceptions and behaviors to enhance compliance are needed.
1. Bui TH, Cavanagh HD, Robertson DM. Patient compliance during contact lens wear: perceptions, awareness, and behavior. Eye Contact Lens 2010;36:334-339.
2. Morgan PB. Contact lens compliance and reducing the risk of keratitis. Optician 2007:20-25.
3. Robertson DM, Cavanagh HD. Non-compliance with contact lens wear and care practices: a comparative analysis. Optom Vis Sci 2011;88:1402-1408.
4. Donshik PC, Ehlers WH, Anderson LD, Suchecki JK. Strategies to better engage, educate, and empower patient compliance and safe lens wear: compliance: what we know, what we do not know, and what we need to know. Eye Contact Lens 2007;33:430-433.
5. Dumbleton KA, Woods CA, Jones LW, Fonn D. The relationship between compliance with lens replacement and contact lens-related problems in silicone hydrogel wearers. Cont Lens Anterior Eye 2011;34:216-222.
6. Ichijima H, Shimamoto S, Ariwaka Y, Muraki K, Cavanagh HD. Compliance study of contact lens wearers in Japan, part 1: internet survey of actual circumstances of lens use. Eye Contact Lens 2014;40:169-174.
7. Dart JKG, Radford CF, Misassian D, Verma S, Stapleton F. Risk factors for microbial keratitis with contemporary contact lenses: a case-control study. Ophthalmology 2008;115:1647-1654.
8. Levy B, Heiler D, Norton S. Report on testing from an investigation of Fusarium keratitis in contact lens wearers. Eye Contact Lens 2006;32:256-261.
9. Robertson DM, McCulley JP, Cavanagh HD. Severe acanthamoeba keratitis after overnight orthokeratology. Eye Contact Lens 2007;33:121-123.
10. Hickson-Curran S, Chalmers RL, Riley C. Patient attitudes and behavior regarding hygiene and replacement of soft contact lenses and storage cases. Cont Lens Anterior Eye 2011 Jan 10;34:207-215.
11. Tilia D, Lazon de la Jara P, Zhu H, Naduvilath TJ, Holden BA. The effect of compliance on contact lens case contamination. Optom Vis Sci 2014;91:262-271.
12. Wu YT, Zhu H, Willcox M, Stapleton F. Removal of biofilm from contact lens storage cases. Invest Ophthalmol Vis Sci 2010;51:6329-6333.
13. Szczotka-Flynn LB, Imamura Y, Chandra J, Yu C, Mukherjee PK, Pearlman E, Ghannoum MA. Increased resistance of contact lens-related bacterial biofilms to antimicrobial activity of soft contact lens care solutions. Cornea 2009;28:918-926.
14. Wu YT, Zhu H, Willcox M, Stapleton F. The effectiveness of various cleaning regimens and current guidelines in contact lens case biofilm removal. Invest Ophthalmol Vis Sci 2011 April 7;52:5287-5292.
15. Burnham GW, Cavanagh HD, Robertson DM. The impact of cellular debris on Pseudomonas aeruginosa adherence to silicone hydrogel contact lenses and contact lens storage cases. Eye Contact Lens 2012;38:7-15.
16. McMonnies CW. Improving patient education and attitudes toward compliance with instructions for contact lens use. Cont Lens Anterior Eye 2011;34:241-248.
17. Yung AM, Boost MV, Cho P, Yap M. The effect of a compliance enhancement strategy (self-review) on the level of lens care compliance and contamination of contact lenses and lens care accessories. Clin Exp Optom 2007;90:190-202.
18. McMonnies CW. Improving contact lens compliance by explaining the benefits of compliant procedures. Cont Lens Anterior Eye 2011;34:249-252.
19. Nomachi M, Sakanishi K, Ichijima H, Cavanagh HD. Evaluation of diminished microbial contamination in handling of a novel daily disposable flat pack contact lens. Eye Contact Lens 2013;39:234-238.
20. Ichijima H, Shimamoto S, Ariwaka Y, Sakata H, Cavanagh HD. Innovations to improve patient compliance. Contact Lens Association of Ophthalmology 2014;Annual meeting:abstract.


