Presbyopic patients often believe that the gradual loss of near vision represents a visual impairment that will degrade the quality of their lives. In actuality, the inevitable loss of accommodative power in human visual systems begins as early as infancy, with virtually everyone fully realizing its adverse effects by 50 years of age.
According to 2010 U.S. Census, there are approximately 100 million people over the age of 50 living in the United States—which provides only a glimpse of the global influence of this ocular condition.1 Already in 2005, presbyopia was estimated to impact 1.04 billion people worldwide, with 410 million people classified as visually impaired due to lack of adequate near corrections.2 The projected magnitude of this phenomenon underlies the attention devoted to pursuing innovative surgical approaches to manage this treatable condition.
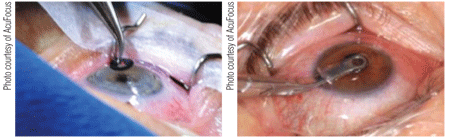
1, 2. Flap technique for inlay placement (left) and pocket techniques (right).
The total power of a human eye is determined by the relationship between cornea, crystalline lens, and the axial globe length. Since the first two elements are relatively modifiable via surgical interventions, it is easy to understand why refractive procedures—including those for presybyopia—are typically of either lens-based or cornea-based approaches. Lens-based methods include clear lens exchange, and cataractous lens extraction followed by multifocal intraocular lens (IOL) insertion. Reduced stereoacuity in monovision modality and compromised contrast sensitivity in multifocal modality may hinder post-operative patient satisfaction.
Current cornea-based management options typically result in alteration of corneal curvatures, such as monovision LASIK/PRK, PresbyLASIK and conductive keratoplasty. However, postoperative risks of optical and visual disturbances, reduced uncorrected distance vision, irreversible structural changes, regression of treatment effects and possible corneal ectasia have limited clinical applications of these surgical procedures.
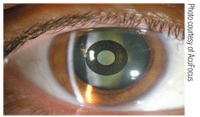
3. Mild nuclear sclerosis easily seen upon clinical examination even after KAMRA implantation.
Femtosecond Laser and Corneal Inlays
First introduced by Jose Barraquer in 1949, refractive addition surgery describes the placement of a synthetic lenticule on the cornea after debridement to alter the anterior curvature after re-epithelialization. Known today as corneal onlay, this procedure was introduced as aphakic or myopic management—although issues with epithelial healing and biocompatibility restricted its applications.
Advances in femtosecond laser platform and biocompatible material now offer intrastromal inlays as an alternative to current cornea-based vision correction techniques, while significantly reducing issues with epithelial remodeling and nutrient permeability as compared to onlays and early inlays respectively.3 Adequate corneal nutrient supply, such as oxygen from tear film and glucose from aqueous humor, is essential to prevent tissue opacification and necrotic responses. Hence, an ideal corneal inlay would be a thin material with high porosity and water content in order to facilitate the navigation of nutrients and metabolic byproducts through corneal layers.4,5
Femtosecond laser operates via the principles of tissue photodisruption where intrastromal cavitations bubbles are formed at pre-programmed depth in the target tissue. These bubbles coalesce into a cleavage plane and allow for a controlled manual dissection. Resultant surgical outcomes improve due to smoother and more stable tissue interfaces, reduced forward light scatter and potentially better overall wound healing response.6 In addition to creating more biomechanically stable LASIK flaps, corneal pockets can also be made to house corneal inlays (figure 1 and 2). A keyhole-shaped infrared blocker, inserted within the laser docking cone, outlines the area where stromal corneal pocket is to be created.
Maximal preservation of nerve plexus and peripheral biomechanical properties—which may offer patients a faster recovery and more intact corneal sensitivity—are some of the advantages of the pocket technique. Flap-related complications like striae are also reduced. Nonetheless, creation of a flap will allow concurrent treatment of ammetropia and presbyopia as laser ablation can be combined with inlay implantation. This treatment approach called “sim-LASIK” is gaining popularity outside of the United States.7
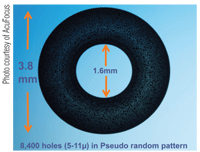
4. KAMRA inlay.
A Further Look: Corneal Inlays
Although many inlay models have received CE marks in Europe for the purposes of treating presbyopia, the FDA currently labels the inlays as investigational devices. Corneal inlays typically are implanted in the non-dominant eye to minimize impact to binocular uncorrected distance vision. They aim to improve retinal qualities of near range objects in one of three ways: providing pinhole effects (KAMRA, AcuFocus); steepening anterior corneal curvature (Vue+, Revision Optics); or increasing overall refractive index (Flexivue, Presbia).
The specific mechanism of action influences the depth of placement as inlays designed to steepen corneal curvature are inserted more anteriorly. Since centration is critical to postoperative success, each inlay is meticulously placed on the first Purkinje image; the clinical belief is that the first Purkinje image is the best reference point for visual axis.
• Pinhole effect inlay. KAMRA is an example of a small aperture inlay and is perhaps the furthest along the clinical trial process amongst current generation of inlays. It is a small, donut-shaped disc made of polyvinylidine fluoride (PVDF) and nano-carbon particles (figure 3). PVDF has been used in ophthalmic material, such as IOL haptics, which has demonstrated history of good tissue biocompatibility. KAMRA has a total diameter of 3.8mm with a center aperture of 1.6mm. Its thickness measures 5µm and has a minimum insertion depth of 170µm to avoid potential impact to anterior corneal contour.

5. Depth of focus simulation with 4mm pupil (left). Depth of focus simulation with 1.6mm pupil (right).
The opaque annulus is incorporated with black carbon particles and has 8,400 perforations of various sizes distributed in random arrangement. This is designed to counter diffraction issues under mesopic settings and yet allow nutrient flow and approximately 10% additional light transmission beyond those passing through the center aperture (figure 4). KAMRA inlay is estimated to provide presbyopic corrective equivalence of up to +2.00D.8
The small aperture provides a pinhole effect in increasing depth of focus by permitting central image rays to project onto retina while obscuring the transmission of peripheral light rays. Because peripheral rays create larger blur circles at the retinal plane, improved depth of focus and image resolution will occur when only central incident rays are transmitted (figure 5).
Just as in photography, decreasing the size of aperture will increase the depth of field being viewed through a camera. However, there is a size limitation to an aperture stop smaller than which the increase in diffraction and decrease in light transmission will impair image quality observed. KAMRA’s aperture size of 1.6mm was determined via computer modeling to offer the best balance in depth of field, light transmission and diffraction.9 In addition to its reversibility, given ease of removal as all inlays, the potential advantage of a KAMRA inlay is its maintenance of distance vision since pinhole inlays do not alter refractive state of a treated eye.
In a two-year study, Orang Seyeddain, M.D., and colleagues found a mean improvement from J6 preoperatively to J1 in binocular uncorrected near acuity (UNVA) in 32 emmetropic presbyopic subjects, with 96.9% reported UNVA of J3 or better in the implanted eyes.10 No significant change in uncorrected distance acuity (UDVA) was found at 24 months; the implanted eye retained a mean UDVA of 20/20.10 Long-term results, released by Omer Yilmaz, M.D., and colleagues in 2011, confirmed similar visual outcome and also good corneal tolerance to KAMRA inlays after a follow-up duration of four years.11 Mean UNVA was J1 in 22 participants with 96% reading J3 or better; UDVA in all eyes was 20/40 or better.11 The small decrease in both UNVA and UDVA in five eyes was suspected to be caused by age-related cataract progression. Two patients elected to undergo cataract removal and both reported a final UNVA of J1 or better with retainment of KAMRA inlays. Finally, four explantations were performed in this series due to issues related to two microkeratome flaps and two post-operative refractive shifts. All four subjects returned to within +/- 1D of their pre-operative refractive status with no loss of corrected distance or near acuity.11
• Center-near effect inlay. Currently at the end of its Phase II of Investigational Device Exemption (US IDE) trial, the 2mm Vue+ is the smallest of the inlay designs. It is slightly larger than its predecessor, the PresbyLens, by 0.5mm to allow for a bigger near optical zone. The intention in the small diameter is to deliver the least amount of interference to the distance vision after its implantation (figure 6).
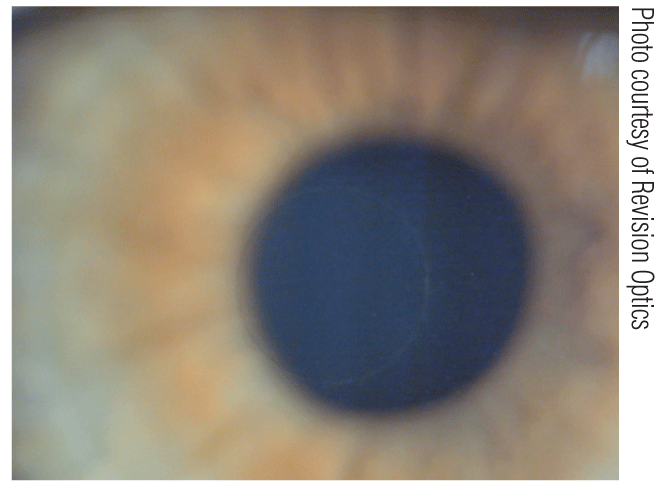
6. Vue+ inlay on slitlamp examination.
Vue+ inlay is made of micro-porous hydrogel that has the same refractive index and water content as human cornea. Thus, it does not introduce additional refractive power when implanted in the cornea. Instead, it is placed at a depth of approximately 120µm to 130µm to induce a steeper postoperative corneal profile in the non-dominant eye. This hyperprolate shift within the central 2mm area confers multifocality at corneal plane (figure 7).
Alan Lane, Ph.D., and colleagues implanted Vue+ inlays after concurrent LASIK procedure for 25 presbyopic patients with uncorrected hyperopia and found an average improvement of seven lines in UNVA, with more than 80% reading J1 or better. The improvement in UNVA reported at one month follow-up was found to be sustainable through the entire study period of six-months. Moreover, the sim-LASIK technique resulted in a mean two-line improvement in UDVA in the implanted eye, with one subject reported loss of one line in UDVA. Nonetheless, binocular UDVA remained at 20/20 or better for all participants throughout the whole study.12
• Center-distance effect inlay. The Flexivue Microlens is a hydrophilic acrylic polymer insert that is 3.2mm in diameter and approximately 20µm in thickness (figure 8). The central 1.6mm disc area is a power neutral zone, which lessens its impact to the distance vision in the eye. Meanwhile, customized powers ranging from +1.50D to +3.00D in 0.25D steps can be chosen for the area of peripheral annulus. The nomogram for add power determination depends on patients’ near demands as measured at 33cm. The refractive power is mainly generated by the higher refractive index of the inlay material. In addition, there is a central perforation of 0.5mm that permits the transfer of glucose and other nutrients to corneal tissues anterior to the implant.
A study of 43 patients found 93% of patients with UNVA of J2 or better at one year.6
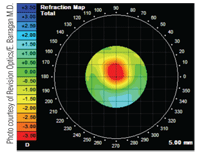
7. Central hyperprolate shift on topography after PresbyLens inlay implantation.
Femtosecond Laser and Transepithelial Vision Correction
• INTRACOR. Femtosecond laser technology delivers ultrashort pulses at near infrared wavelength in pre-planned patterns and tissue depth. This clinical ability renders a new approach in which stromal tissues can be accessed for refractive vision correction. It is now possible to perform intrastromal refractive modification without breaching epithelial integrity.
Femtosecond laser system (Technolas Perfect Vision) creates a pattern of five intrastromal cylindrical rings, which alters the dynamics of corneal biomechanical forces (figure 9). The procedure, having already received CE marks in Europe since April 2009, is known as INTRACOR. A net effect of a steepening in central cornea is produced, which confers multifocality in the non-dominant eye. Presumably, the hyperprolate shift is due to progressive tissue distension as a summation between outward vector forces of intraocular pressure and the newly established equilibrium of corneal biomechanics.13
When proper pachymetric data is incorporated into each INTRACOR treatment nomogram, the five intrastromal cylindrical rings are incised without affecting the four neighboring corneal layers. The postoperative implications are avoidance of common surgical risks of infection, inflammation, irregular or delayed epithelial healing and perforation. Patients typically report initial blur immediately after the procedure due to intraoperative cavitation bubbles trapped within the five intrastromal rings. Vision improves as gas bubbles dissipate within the first day leaving only faint circular stromal lines reminiscent of the pattern seen on a multifocal lens (figure 10 and 11).14
A one year study by Luis Ruiz, M.D., and colleagues with 83 mildly hyperopic or near emmetropic presbyopes found 89.2% of eyes with UNVA of J2 or better. A two to three line decrease in UDVA due to mild postoperative myopic shift was reported in 3.6% of eyes.2 Overall stability was noted in contrast sensitivity, pachymetry, endothelial cell density and corneal biomechanical properties as measured via Ocular Response Analyzer (Reichert). Notably, aberrometry findings of positive shift in primary spherical aberration and negative shift in secondary spherical aberration corresponded to the expected clinical results of increased corneal asphericity and depth of focus.2
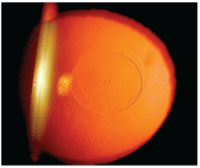
8. Flexivue Microlens within which the 0.5mm central perforation can be seen with retroillumination.
The most common patient complaint during the postoperative period was nighttime halo. All patients reported visual symptoms right after surgery, with just 3% reporting persistence of symptom at 12 months. Although INTRACOR is optimal for mild hyeropic or emmetropic presbyopes, additional photodisruptive spots may be applied to include those presbyopes with the need for mild myopic and/or astigmatic corrections in future studies. Moreover, diffractive effects of paracentral laser energy delivery and treatment regression due to biomechanical reorganization may need to be further investigated.2
Femtosecond Laser and Laser Lentotomy

9. INTRACOR 3D corneal model.
• Femtosecond Lentotomy. Although the exact mechanism of accommodation is debated, Helmholtz’s theory indicates that zonular relaxation under the state of ciliary muscle contraction leads to the evenutal steepening in lenticular curvatures. As a result, the object image plane moves into one’s punctum proximum to allow for its subsequent conjugation with the retinal plane. This doctrine supports lenticular sclerosis as being responsible for loss of accommodative ability with time. Because the ciliary muscle, lens capsule and zonules appear to retain inherent flexibility, it is sensible to presume a complete or partial return of accommodative ability if the elasticity of crystalline lens can be restored.
Ronald Krueger, M.D., and Raymond Myers, O.D., first suggested the use of laser photodisruptive incisions within crystalline lens to alter the dynamic forces between collagen fibrils in order to increase tissue elasticity.15 The principle of photodisruption was initially experimented with nanosecond laser pulses, which left undesirable optical effects from trapped residual gas bubbles and resultant lenticular opacities. However, the ultrashort pulses of femtosecond laser may deliver the necessary precision to renew interest in laser lentotomy. The accuracy and reproducibility of femtosecond laser permits the formation of incisions in multiple dimensions without disturbing neighboring tissue structures such as lens capsule; therefore, gliding planes can be created to break the molding force within the sclerotic matrix of a crystalline lens.15
Ex-vivo elasticity measurements in treated porcine eyes showed 26% increase in mechanical flexibility of the lens. In addition, early in vivo studies with rabbit models have not shown side effects such as cataract formation or optical scattering within a three month postoperative period.15 Histology studies also have not revealed collateral tissue damage in the posterior segment from infrared energy passing through the crystalline lens.16 Utilizing computer models, Valas Teuma and colleagues demonstrated an average refractive gain of +1.5D to maximum response of +3.6D with ex-vivo treated porcine lenses.17
Future Management
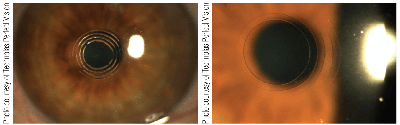
10, 11. Three hours (left) and one day (right) post-INTRACOR treatment.
The diminution of accommodative ability in a human eye appears to correspond well with age-dependent structural changes within the crystalline lens. Therefore, developing presbyopic treatment modalities that target the level of crystalline lens would seem to have sound clinical merits.
Inventive lens-based concepts such as that of femtosecond lentotomy show promising interim results although the optimal patterns and number of incisions have yet to be studied. Nevertheless, development of novel lens-based techniques may give way to a future management trend for our ever-growing presbyopic population as these procedures may provide the potential for binocular treatments while reducing iatrogenic optical disturbances from current monovision and multifocal approaches.
Dr. Chang is the director of the contact lens division at The Cornea and Laser Eye Institute-Hersh Vision Group in Teaneck, N.J. He completed his clinical fellowship in cornea and contact lens with a special interest in the fitting of keratoconus and post-surgical corneas. He also serves as an adjunct faculty for Pennsylvania College of Optometry at Salus University.
1. Howden L, Meyer J. Age and Sex Composition: 2010. 2010 Census Briefs. 2011 May. Available at:
www.census.gov/prod/cen2010/briefs/c2010br-03.pdf (accessed June 2011).
2. Ruiz LA, Cepeda LM, Fuentes VC. Intrastromal correction of presbyopia using a femtosecond laser system. J Refract Surg. 2009 Oct;25(10):847-54.
3. Evans MD, Xie RZ, Fabbri M, et al. Progress in the development of a synthetic corneal onlay. Invest Ophthalmol Vis Sci. 2002 Oct;43(10):3196-201.
4. Verity SM, McCulley JP, Bowman RW, et al. Outcomes of PermaVision intracorneal implants for the correction of hyperopia. Am J Ophthalmol. 2009 Jun;147(6):973-7.
5. Sweeney DF. The Max Schapero Memorial Award Lecture 2004: contact lenses on and in the cornea, what the eye needs. Optom Vis Sci. 2006 Mar;83(3):133-42.
6. Waring GO. Corneal Inlays for the treatment of Presbyopia. Int Ophthalmol Clin. 2011;51(2):51-62.
7. Low AJ. Presbyopia correction with the kamra inlay. Cat Refract Surg Today Europe. 2010 Jan. Available at:
www.bmctoday.net/crstodayeurope/2011/01/article.asp?f=presbyopia-correction-with-the-kamra-inlay (accessed June 2011).
8. Lindstrom RL. Intracorneal lens inlays. LA Insight. Available at:
www.la-sight.com/In-Development/corneal-lens-inlays.aspx (accessed June 2011).
9. Yilmaz OF, Bayraktar S, Agca A, et al. Intracorneal inlay for the surgical correction of presbyopia. J Cataract Refract Surg. 2008 Nov;34(11):1921-7.
10. Seyeddain O, Riha W, Hohensinn M, et al. Refractive surgical correction of presbyopia with the AcuFocus small aperture corneal inlay: two-year follow-up. J Refract Surg. 2010 Oct;26(10):707-15.
11. Yılmaz OF, Alagöz N, Pekel G, et al. Intracorneal inlay to correct presbyopia: long-term results. J Cataract Refract Surg. 2011 Jul;37(3):1275-81.
12. Lang AJ, Porter T, Holliday K, et al. Concurrent use of the ReVision Optics intracorneal inlay with LASIK to improve visual acuity at all distances in hyperopic presbyopes. Poster presented at the Association for Research in Vision and Ophthalmology meeting, May 1-5, 2011; Ft. Lauderdale, Fla.
13. Guedj T, Danan A, Lebuisson DA. In-vivo architectural analysis of intrastromal incisions after INTRACOR surgery using fourier-domain OCT and Scheimpflug imaging. J Emmetropia. 2011;2(2):85-91.
14. Holzer MP, Mannsfeld A, Ehmer A, Auffarth GU. Early outcomes of INTRACOR femtosecond laser treatment for presbyopia. J Refract Surg. 2009 Oct;25(10):855-61.
15. Ripken T, Oberheide U, Fromm M, et al. fs-Laser induced elasticity changes to improve presbyopic lens accommodation. Graefes Arch Clin Exp Ophthalmol. 2008 Jun;246(6):897-906.
16. Lubatschowski H, Schumacher S, Fromm M, et al. Femtosecond fentotomy: generating gliding planes inside the crystalline lens to regain accommodation ability. J Biophotonics. 2010 Jun;3(5-6):265-8.
17. Teuma V, Gray G, Edwards K, et al. Improving presbyopic eye accommodation response by softening mid-peripehery of the crystalline lens via ultra-fast laser. Poster presented at the Association for Research in Vision and Ophthalmoloy meeting, May 1-5 2011; Ft. Lauderdale, Fla.


