Dry eye is a complex disease that affects millions of people around the globe. In 2011, the American Academy of Ophthalmology estimated that over five million Americans aged 50 or older suffered from the condition.1 But of course the condition impacts other demographics as well, particularly otherwise healthy contact lens wearers at any age.
Its propensity to affect such a wide swath of patients in varying ways makes dry eye both mundane and also uniquely challenging—rarely does such a commonplace condition retain the ability to confound.
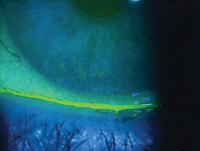
Dryness from incomplete blinks. Photo: Paul M. Karpecki, OD
This conundrum has given rise to a number of new technologies, developed to help clinicians diagnose and treat dry eye with greater precision. A plethora of diagnostic tools designed specifically for dry eye disease now exist, but which truly might offer advantages over the humble Schirmer test and slit-lamp exam in your practice?
This article will discuss the value of some emerging technologies in dry eye care to help you expand and streamline your management of the disease.
The technologies detailed below are but a few options currently available for clinicians in an effort to simplify and improve dry eye diagnosis techniques. Each of these products employs a unique manner of diagnosing and treating the condition.
Tear Interferometry
A new and noteworthy application of an already existing technology in dry eye diagnosis and treatment is the TearScience tear interferometry system. The process of tear interferometry examines changes that occur over time on the tear film. TearScience’s offering is comprised of two separate devices—the LipiView and the LipiFlow—to help clinicians in the diagnosis and treatment of dry eye.
• LipiView. The TearScience LipiView is notable in that it uses interferometry to quantify the average lipid layer thickness of a designated area of tear film, and capture the blink profile of an eye during a designated time interval. This helps to quantify the number of partial blinks vs. complete blinks.
This is clinically useful, as partial blinking that is left unnoticed is a significant contributor to the chronic nature of dry eye, according to Caroline Blackie, OD, PhD, Senior Clinical Scientist at TearScience, who practices in Burlington, Mass.
The LipiView also offers clinicians the ability to show their patients exactly what is seen during the examination. This method of educating patients can help make treating dry eye easier for eye care professionals.
“The LipiView provides the patient with a powerful educational tool to help them better understand what the lipid layer is and why blinking exercises and other in-office and at-home treatment may be critical to their recovery,” says Dr. Blackie.
• LipiFlow. TearScience’s LipiFlow system applies heat and force directly and simultaneously over the meibomian glands, relieving them of obstruction. According to Phoenix’s Arthur B. Epstein, OD, 86% of dry eye is caused by meibomian gland dysfunction (MGD) and lipid deficiency.
The LipiFlow system is unique in its ability to treat MGD. “It applies therapeutic levels of heat directly over the glands as opposed to the conventional and highly inefficient application of heat to the outside of the eyelid,” says Dr. Blackie.
LipiFlow uses heat as a means to treat MGD because it helps to liquefy any solidified secretions that may cause obstruction in the gland duct. When pressure is simultaneously added, the liquefied material is painlessly evacuated from the glands, Dr. Blackie says, significantly increasing the likelihood of normal gland function post treatment.
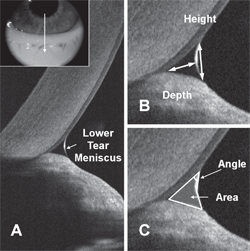
Measuring the tear meniscus with a standard resolution OCT. Photo: Yan Li, PhD, and David Huang, MD, PhD, Casey Eye Institute, Portland, OR.
Dr. Epstein is planning to incorporate the system in his new practice within the next few months, and says he couldn’t imagine not having access to this technology in a practice focused on dry eye. “When we planned our practice, we intentionally created a dry eye center specifically to incorporate this technology,” Dr. Epstein says.
“I've seen how LipiFlow provides a life-changing experience for many dry eye sufferers who have spent amazing amounts of money on therapies that are palliative at best and often don't really help much at all.” Dr. Epstein considers this system the centerpiece of a dedicated dry eye center and a potential new standard of care for managing MGD and evaporative dry eye.
Meibography
One of the newest innovations in the diagnosis of dry eye, the Keratograph 5M, comes from the German company Oculus.
A key feature of the device is its ability to conduct IR meibography, a non-contact method that uses a camera and an infrared light source to examine the meibomian glands in extensive detail, which Dr. Epstein says is “vastly superior to transillumination.” Because MGD is one of the leading causes of dry eye around the world, the device’s ability to examine the meibomian glands is an essential feature for clinicians treating the condition, he says.
The Keratograph 5M also offers clinicians non-invasive automated tear break-up time measurements. Examining tear break-up time measurements non-invasively is advantageous because it has the ability to produce accurate results more quickly and comfortably for patients.
“They are reproducible and provide unique insight into tear stability,” says Dr. Epstein, who has used the 5M in his practice for the past three months. “The 5M also offers tear meniscus height measurement, which is helpful in estimating tear volume and reserve rather than grossly estimating it.”
Much like the LipiView, the unit also offers the advantage of being able to show patients exactly what you’re seeing via its display.
“The graphical display is also very helpful in educating patients as well as observing change from treatment or over time,” Dr. Epstein adds.
The device has become a staple in Dr. Epstein’s practice. “The 5M replaces a conventional topographer, which I consider an essential instrument in its own right.“
Non-invasive Evaluation of the Tear Film
All clinicians are familiar with the clinical value of OCT for retinal disease management, but anterior segment OCT (AS-OCT) is emerging as a way to improve the diagnosis of dry eye in patients.
Other Notable Dry Eye Technologies
TearLab Osmolarity System
The TearLab Osmolarity System measures the osmolarity of human tears
to aid in the diagnosis of dry eye. Abnormal tear osmolarity is a
common feature found in patients with dry eye disease. As the osmolarity
level increases in the tears, the severity of dry eye increases.2
Intense Pulsed Light for MGD
For patients with moderate to severe dry eye, intense pulsed light
(IPL) can be used as a treatment option. Rolando Toyos, MD, founder of
the Toyos Clinic in Memphis, helped refine this technology for patients
with dry eye. IPL uses powerful bursts of light to unclog meibomian
glands and correct MGD, and is especially good for patients with
rosacea.3
Maskin Meibomian Gland Intraductal Probe
The Maskin Meibomian Gland Intraductal probe can be used to unclog
meibomian orifices. After a bandage contact lens is placed on the eye
and a topical anesthetic is administered, the probe is inserted into the
blocked glandular orifice and distal duct. The procedure generally
takes about 15 minutes in most cases.4
For diagnosing dry eye, David Huang, MD, PhD, one of the pioneering physicians and scientists who invented OCT technology in the early 1990s, suggests examining the tear meniscus with a typical OCT. “Specifically, the central-lower tear meniscus cross sectional area,” he says. “That measures tear volume like the Schirmer’s test, but it’s more repeatable than Schirmer’s, and doesn’t require putting in an anesthetic or a stain.”
“It is important to perform the meniscus scan at the same point in the blink cycle,” Dr. Huang cautions. “In a published study, we performed scans at two seconds after a blink.”
“The tear film itself can be very thin in dry eye patients, and is beyond the resolution of standard clinical OCT systems,” notes Dr. Huang.
Ultra-high resolution (1-2µm) OCT devices can measure the thickness of the tear film to confirm the presence of dry eye in patients. But for the time being, they may be too specialized to be worth the investment for clinicians.
“The problem with ultra-high resolution is that the field of view becomes very shallow,” adds Dr. Huang. “This makes scan acquisition very difficult for more common purposes, such as corneal mapping or angle imaging.”
Dr. Huang believes most clinicians would already find their standard-resolution OCT useful for dry eye diagnosis. “I think that by detecting low tear meniscus and redundant conjunctival folds (conjunctivochalasis) with OCT, clinicians can already identify the cause of irritation in most patients with complaints of dry eye symptoms.”
Another promising use for OCT is in the mapping of epithelial thickness.
“The epithelial thickness becomes more irregular in dry eye,” says Dr. Huang. “This could be useful in dry eye evaluation. But further software development and clinical validation is needed,” according to Dr. Huang.
If we reach a point at which higher resolution AS-OCTs become the norm, the technology will provide a non-invasive option to evaluate the tear film, which simplifies and speeds up the process of examining the tear film while keeping it free of interference by the clinician, for greater accuracy.
But this application of ultra-high resolution OCTs for diagnosing dry eye may not currently be ideal for clinicians.

A standard resolution OCT can be used to detect conjunctivochalasis in relation to dry eye symptoms. Photo: Yan Li, PhD, and David Huang, MD, PhD, Casey Eye Institute, Portland, OR.
Technology on the Horizon
The following technologies are not yet available in the US, but are expected to debut soon. Continuing the trend of unique diagnostic methods, the following emerging technologies will complement your current techniques, resulting in a simplified and more complete overall diagnosis of dry eye.
• RPS InflammaDry Detector. The clinical signs of dry eye often do not correlate with patient complaints. This can make the diagnosis of dry eye difficult for clinicians.
Research has shown the enzyme matrix metalloproteinase-9 (MMP-9), an inflammatory marker, is consistently elevated in the tears of dry eye patient.5 The InflammaDry Detector tests for elevated levels MMP-9 to aid in the objective diagnosis of dry eye.
The test is easy for clinicians to conduct and produces results quickly.
“This test is easy to administer using a small tear sample taken from the inside lining of the lower eyelid, the palpebral conjunctiva,” says Dr. Robert Sambursky, MD, co-founder and CEO of RPS. “It takes only seconds to collect the sample and run the test. Results are available in just 10 minutes, allowing a diagnosis and treatment plan to be established with the patient before they leave the office.”
The InflammaDry test has shown promise in its ability to accurately diagnose dry eye.
“In a prospective, sequential, masked, multicenter clinical trial of 206 patients, the InflammaDry test showed sensitivity of 85% and a specificity of 94%, compared to a clinical assessment of dry eye using the Ocular Surface Disease Index, Schirmer tear test, tear break-up time and keratoconjunctival staining6,” says Dr. Sambursky.
The InflammaDry test is approved for use in Canada and Europe, but is not yet available in the United State. It is still under review by the FDA.
• Nicox Dry Eye Panel. Another technology that may soon make a splash in the diagnosis of dry eye is the Nicox Dry Eye Panel. The product will specifically help to simplify and improve the testing of Sjogren’s syndrome, a cause for severe dry eye symptoms.
“The Nicox panel will help make diagnosis more specific and allow us to better target severe dry eye patients well before they become severe,” says Dr. Epstein.
The Nicox Dry Eye Panel is a proprietary “lab on a chip” that gives clinicians access to testing that would normally need to be conducted in a laboratory. The diagnostic test combines three novel biomarkers (SP-1, CA-6 and PSP) with traditional biomarkers (ANA, Ro, La and RF) to diagnose Sjogren’s syndrome at an early stage.
There is of course no “one-size-fits-all” option for diagnosing or treating dry eye—different tools will work better for different clinicians, so it’s all about what works best for you and your practice.
Generally speaking, you will be employing multiple technologies at any given time to achieve the best results, and each of the aforementioned products and techniques could improve your ability to accurately diagnosis dry eye and tailor the therapy appropriately to each presentation.
1.
http://www.aao.org/newsroom/upload/Eye-Health-Statistics-April-2011.pdf
2.
http://www.tearlab.com/pdfs/TearLab%20Clinical%20Utility%20Guide.pdf
3.
http://www.revophth.com/content/d/technology_update/c/25857/
4.
http://www.refractiveeyecare.com/2012/07/intraductal-meibomian-gland-probes/
5.Kaufman, HE. The practical detection of mmp-9 diagnoses ocular surface disease and may help prevent its complications. Cornea. 2013 Feb;32(2):211-6.
6.Sambursky, Davitt, Latkany, et al. Sensitivity and Specificity of a Point-of-Care Matrix Metalloproteinase 9 Immunoassay for Diagnosing Inflammation Related to Dry Eye. JAMA Ophthalmol. 2013;131(1):24-28.


