Contact lens fitters need to design lenses that provide the best possible comfort for the wearer, allow the patient to attain his best acuity, and keep the eyes healthy. We need to design a clean, wet, moving lens and put it on a clean, wet eye. The tools available to us make this relatively easy for most “normal” corneas. With corneal topography, new highly permeable and wettable materials, and many great lens designs, we can satisfy virtually all of our patients who are legitimate candidates for contact lenses.
The fitting criteria for surgically altered corneas are the same as for the normal cornea. Ideally, the lens will have slight apical clearance with areas of light touch in the mid-periphery at 3- and 9-o’clock, and will have unobstructed vertical movement with each blink. Generally, this is easy to achieve on a standard, with-the-rule cornea; however, there is a significant challenge to achieve these fitting characteristics on surgically altered corneas. The goal is the same, but safe compromise frequently will be necessary. As a general rule, it is best to begin with the simplest lens design that you believe will satisfy the needs of the patient.
For the purposes of this article, we will concentrate on fitting gas-permeable (GP) lens options, including moderately large corneal lenses and scleral lenses.
A Demographic Apart
According to the American Academy of Ophthalmology, there were approximately 41,000 corneal transplants and 700,000 refractive surgeries performed in 2008.1 In my experience, almost all corneal transplant patients have irregular corneas and require specially designed GP lenses. If you include the high number of radial keratometry (RK) patients, we could have hundreds of thousands of people who need specialized fitting to achieve their best possible acuity.
The examination procedure should consist of the same steps as any other contact lens patient, including corneal topography (CT). CT provides information that leads the contact lens fitter to the initial diagnostic lens and provides valuable information to estimate the degree of success presented by each contact lens fitting option. At the completion of this initial exam, the patient should be educated about the benefits and limitations of each contact lens option, or even if spectacles might be a more suitable option to provide clear vision.
Lenses available to treat these irregular corneas include (but may not be limited to):
• Standard soft lenses.
• Standard spherical GP lenses.
• Large-diameter GP lenses (10.5mm to 13.0mm; average 11.2mm to 11.5mm).
• Aspheric GP lenses.
• GP lenses with either steep or flat peripheral curves.
• Reverse-geometry GP lenses.
• Toric lenses.
• Piggyback systems.
• Scleral GP lenses.
• Hybrid lenses (combination of GP and soft materials).
Multiple Sets of Lenses
The best available tools for fitting these patients are multiple sets of diagnostic lenses and the best topographer is the diagnostic lens. Post-surgical corneas that are relatively normal frequently can be fit from topography. A post-surgical cornea that is prolate (e.g., steepest in the center and flattest toward the periphery) is the easiest on which to achieve the apical clearance with light 3- to 9-o’clock touch and vertical movement. At times, a toric or aspheric lens may be necessary to attain this ideal fit. Virtually every other cornea requires diagnostic lens fitting.
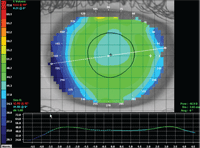
1. This topography image of a post-LASIK patient’s cornea shows minimal flattening from center to mid-periphery nasally, but a significant difference center to temporal side.
The basic diagnostic GP lenses that a fitter of irregular corneas should have available include:
• Large-diameter, large optic zone lenses for post-penetrating keratoplasty patients and other abnormal corneas.
• Reverse-geometry lenses in two diameters, ranging from 10.0mm to 11.0mm.
• Back or bitoric set. Sphere power effect set works well.
• Aspheric lenses, prolate and possibly oblate lenses.
• Scleral lenses in two diameters, ranging from 15.0mm to 19.0mm.
• Lenses designed specifically for keratoconus (useful for corneal ectasia post-LASIK). Include two different diameters, ranging from 8.6mm to 9.8mm.
It is unnecessary to have all of the above diagnostic sets at your immediate disposal, as many labs have “loaner” sets available. You can select your initial diagnostic lens a number of ways. Many topographers allow you to select from a number of lens designs and parameters to create a simulated fluorescein pattern. Manipulate the parameters until this simulated pattern looks the way you like, and then place a diagnostic lens that closely approximates the lens in the topographer on the eye. Evaluate the fluorescein pattern, and, if it is similar to the topographer’s version, over-refract to determine the exact powers and order the lens. If the topographer’s simulated fluorescein pattern is not similar to the actual pattern, make changes to your diagnostic lenses until you have the desired fit, again over-refract, and order your lens.
If you do not have access to a corneal topographer or your topographer does not allow you to “design” lenses, you will need to do everything with diagnostic lenses only. In cases where the topography is so irregular that you cannot determine a good starting point, just put a lens on the eye, evaluate the fluorescein pattern and make lens changes until you have the best initial fit.
Frequently, more than one lens design will provide the necessary fitting characteristics to ensure the patient sees well, is comfortable and maintains a healthy cornea. As a reminder, start with the least complicated lens design that you believe will meet the needs of the patient. Large-diameter lenses, as well as scleral lenses, tend to center well and provide a stable fit and stable acuity because the lenses do not move excessively on the eye.
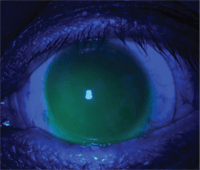
2. A corneal touch zone on a post-surgical cornea that has a “feathery” edge, as in the one above (look at the superior temporal quadrant), can be acceptable.
When topography shows a large amount of steepening in the mid-peripheral cornea, a reverse-geometry lens may be the best starting point. If the mid-peripheral cornea is similar to the central cornea, then a traditional lens may function well. The goal of a large-diameter lens fit is to have the flattest base curve that does not bear heavily on the cornea.
Figure 1 is a topography image of a post-LASIK patient whose cornea could be fit with either a spherical lens or a reverse-geometry lens. Notice that there is not a large amount of flattening from center to mid-periphery on the nasal side, but there is a significant difference center to temporal side. Curvature at apex is 41.80D, 3.5mm nasal curvature is 40.80D, and 3.5mm to the temporal side the curvature is 47.5D. It would be logical to expect a conventional GP lens to decenter to the temporal side, as that is the steepest portion of the cornea. To minimize this, either a large-diameter spherical lens or a reverse-geometry lens would be a good first choice.
When selecting a reverse-geometry lens for your patient, the base curve will approximate the flat keratometer reading and the “alignment” curve will approximate the average of the nasal and temporal cornea 3.5mm to 4.0mm from the corneal apex. The diagnostic lenses that are used for orthokeratology work well when fitting postoperative corneas with an oblate shape.
To Each Their Zone
As previously noted, scleral lenses provide good centration and stable vision due to their near lack of movement and large optical zone. Scleral lenses are less likely to “pop-off” the eye. The downside is that they are significantly more expensive and initially more difficult to handle. They can work well for most irregular corneas, regardless of the cause of the irregularity. A well-fit scleral lens should always vault the central cornea and clear the limbus.
The initial lens selection typically will be a base curve that is 1.00D steeper than the steepest K-reading. A well-fit lens will center; vault the corneal apex; complete clearance of the limbal region; avoid blanching of conjunctival vessels, which would indicate the periphery is too tight; and involve minimal or no lens movement. Also, after several hours of wear, the lens can be easily removed; there is no “suction.”
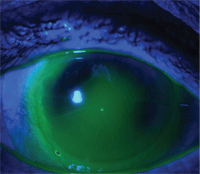
3. Excessively hard touch in the superior temporal quadrant of a corneal touch zone.
The three zones of the lens should be evaluated beginning with the corneal zone and moving out:
• Corneal zone. Use an optic section to evaluate the depth of the tear layer near the corneal apex. The tear layer should be one-fourth to three-fourths the thickness of the cornea, or 150µm to 375µm. This will vary with each lens design, but as an estimate, 1.00D of base curve change will result in 100µm of sagittal depth change when the base curve and first peripheral curve are changed the same amount.
Post-surgical corneas can be quite irregular and it is not always possible to vault the entire cornea. At times, it may be necessary to accept some corneal touch. This can be acceptable if the touch zone has a “feathery” edge (see figure 2) as opposed to a very sharp edge (see figure 3).
• Limbal zone. There should be adequate clearance of this area, which is evidenced by diffusion of fluorescein over the entire limbal area. If additional clearance is needed in this region, consider widening the optical zone or the first peripheral curve.
• Scleral zone. There should be no blanching of blood vessels or restriction of blood flow. Also, there should be no excessive edge lift. Let the lens settle on the eye for at least 30 minutes before you evaluate the fit. Further, it is wise to evaluate the lens again after three to four hours of wear before ordering the initial lens. At the three- to four-hour evaluation, assess tear flow beneath the lens and determine if the lens is “sucked on.”
Because each lab manufactures and designs their lenses differently, the information provided here serves as a general guide. When first fitting any scleral lens or any lens design that is new to you, don’t be shy about asking questions of the lab’s consultants. They are a valuable source of information and will be a great aid to your success.
1. The American Academy of Ophthalmology. http://www.aao.org/newsroom/press_kit/upload/Eye-Health-Statistics-June-2009.pdf. (Accessed December 2011).
Dr. Rinehart is a graduate of Pacific University of Optometry. He has been in private general practice in Peoria, Ariz. with primary interest in gas permeable contact lenses since 1976. He is also one of the founding members of the American Academy of Orthokeratology, and is currently on the Board of Advisors of the Rigid Gas Permeable Lens Institute.


