It may come as a surprise to most of you that orthokeratology (ortho-k) officially turns 50 on October 13, 2012—the date in 1962 when George Jessen, O.D., gave his controversial lecture, “Orthofocus Techniques,” at the meeting of the International Society of Contact Lens Specialists in Chicago.1 At the same conference, Newton Wesley, O.D., M.D., Sc.D., suggested the alternative word “orthokeratology” be used to describe the technique, which Ronald Kerns, O.D., later defined as “the reduction, modification or elimination of a refractive error by the programmed application of contact lenses.”2 Because the early techniques were unsuccessful, interest in ortho-k waned by the mid-1980s, when conventional contact lenses started to really come into their own.
Science has markedly evolved since the early 1990s with the development of CNC lathes, advanced reverse-geometry lenses, high-Dk rigid gas-permeable (RGP) materials that allow for overnight wear of the lenses, and most importantly, highly accurate and repeatable corneal topography instruments.
Modern ortho-k is a scientifically validated, FDA-approved method of correcting low to moderate myopic refractive errors—up to -4.00D, and in some instances, up to -8.00D. The design of ortho-k lenses has evolved to include treatment for astigmatism and low degrees of hypermetropia and presbyopia. We are also seeing strong indicators that ortho-k can play an important role in myopia control.3-5
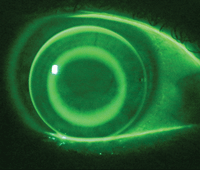
1a. Fluorescein pattern of an ideal fitting reverse-geometry lens for ortho-k.
Jerome Legerton O.D., M.S., M.B.A., has published a comprehensive review of the current options for myopia control.6 There are no published studies on the optimal time to introduce myopia control treatment, or the time (years) that the treatment needs to be maintained to have a positive long-term effect. The common rule is that the practitioner, with the clinical knowledge of family history and refractive progression, will consult the parents and child to decide when to fit.
The current practice brings up questions of safety and efficacy, as well as the importance of total compliance in order to minimize the risks of corneal infection. However, in the area of myopia control, ortho-k could conceivably become “optometry’s fluoride,” my terminology for the chance to do something positive for our myopic patients. Why, then, is this procedure not more prevalent in the optometric community?
Several external factors, such as the apprehension of taking on a new procedure, lack of formal instruction, the risk of adverse outcomes, learning new and challenging concepts (such as sag fitting) and the accurate interpretation of corneal topography maps may hinder the eye care professional. From personal conversations with fellow optometrists who are thinking about starting ortho-k, the main stumbling block appears to be a misconception as to how the procedure actually works.
In this article, I will sort through some of the myths surrounding modern orthokeratology.
Myth Busting
Myth #1: Ortho-k works by compression on the central cornea.
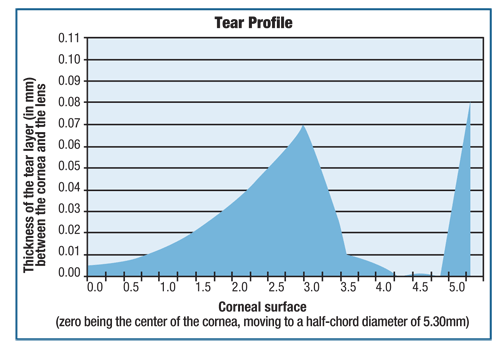
1b. The tear layer profile for a five-zone ortho-k lens showing apical clearance. Note that the TLT shows 5um of apical clearance at the center, moving to a maximum value at the BOZD (3.00mm). The reverse and alignment curve clearances make up the rest of the profile.
Dr. Jessen’s original concept was to fit lenses very flat with respect to the flat –K reading and, by applying apical bearing and pressure to the cornea, induce corneal flattening. Many optometrists find it somewhat unethical to fit a lens with this in mind. However, this is not how modern ortho-k lenses work. The base curve is definitely much flatter than the flat-K; however, the incorporation of the reverse curve allows the designer to lift the lens so that it does not come into contact with the apical corneal surface.
The reasons for this are simple. In 1977, Tommy Hayashi O.D., Ph.D., proved that if there was no apical clearance present in a contact lens fit, the “tear layer squeeze film” forces, combined with lid forces, would drag the lens off center (usually superiorly) until some form of apical clearance was re-established.7 This would lead to equilibrium between the post-lens tear layer squeeze film forces, lid forces and the surface tension around the lens edge.8
Similarly, if a reverse-geometry lens exhibits apical touch, then the lens will de-center and cause central corneal staining due to lens abrasion of the epithelium and distortion of the post-wear corneal topography.9 The ideal ortho-k lens is always well-centered and must be fitted with at least 5µm to 10µm of apical clearance (figure 1).
So, if it’s not causing apical pressure, how does the process actually work?
The old adage that “flat lenses cause corneal flattening, steep lenses cause steepening” is loosely applicable to ortho-k lenses because elements of both fitting philosophies are inherent in the lens design. The flat base curve centrally applies a minimal degree of central compression, but due mainly to the effects of the lens thickness on lid tension. The steep reverse curve at the edge of the back optic zone creates an annulus of tension, or negative pressure, that draws fluid from the central epithelium into the mid-peripheral cornea, thereby causing central flattening and mid-peripheral steepening (figure 2).10 The combination of these two effects causes the change in anterior corneal curvature and the refractive change (figure 3).
Myth #2: Ortho-k lenses are difficult and time consuming to fit.

2. A cross-section of a reverse-geometry lens on the eye. The central compression from the lid is positive, and the tension at the back optic zone/reverse curve junction is negative. The combination of both forces causes the cornea to change shape.
This is certainly true if you believe you can fit ortho-k lenses using a keratometer. Essentially, the keratometer is now an obsolete instrument for measuring corneal shape.
Our entire history of lens design and fitting was based on the false assumption that the cornea was somehow spherical in shape centrally, and then flattened off in the periphery. Corneal topography has challenged this notion; now we understand the true aspheric nature of the corneal shape.
Keratometry readings give an indication of the sagittal radius of curvature of the cornea at a chord of 3.00mm, but give no indication as to the rate of corneal flattening (eccentricity, or e), which determines the sag height of the cornea. So, instead of having a fitting rule that says to “fit the lens X diopters flatter than K,” the new rule for fitting ortho-k lenses is: lens sag = corneal sag + apical clearance (over the common chord of contact).11
Corneal sag is determined by the values obtained from the corneal topographer. The lens designers and laboratory then determine the lens sag that best suits the corneal data using their own proprietary design algorithms.
Myth #3: All corneal topographers are created equal.
“Garbage in, garbage out” is as true today as it was when the phrase was first used in early computing language. The accuracy of a lens fit based on corneal topography data is only as good as the information supplied by the topographer. As stated previously, the aim with an ortho-k lens fit is to have an apical clearance ranging between 5µm and 10µm. So, if the topographer is only repeatable to +/-10µm, the lens can be either too flat or too steep from the outset.
All corneal topographers are accurate when measuring steel balls, but human eyes are neither perfectly spherical nor completely hardened. Therefore, it cannot be said with any scientific validity that a certain topographer is accurate in measuring corneal data. All that can be said is how repeatable the instrument is at “telling its story and sticking to it.”
 Of all the studies performed on different corneal topographers, the most repeatable instrument is the Medmont E300 (Medmont International).12 A practitioner certainly may use a less repeatable instrument, but the cost of having to determine the inaccuracies of the instrument in order to develop strategies that increase the first fit success rate can be disheartening and may lead to a loss of confidence in ortho-k.
Of all the studies performed on different corneal topographers, the most repeatable instrument is the Medmont E300 (Medmont International).12 A practitioner certainly may use a less repeatable instrument, but the cost of having to determine the inaccuracies of the instrument in order to develop strategies that increase the first fit success rate can be disheartening and may lead to a loss of confidence in ortho-k.
The success or failure of a lens absolutely depends on the practitioner’s ability to read and interpret the post-wear topography maps, with special emphasis on the difference maps. This can give an objective assessment of the refractive change achieved and, most importantly, the centration of the lens.12
Ortho-k lenses are not assessed on how good the fluorescein pattern looks, but on how well the aim of correct centration and refractive change was achieved following lens removal.
A corneal topographer that has poor repeatability will, therefore, provide less than optimal or accurate information if both the pre-fit and post-wear maps have variable quality.
Myth #4: Some lenses are inherently better than others.
Unlike corneal topographers, most ortho-k lenses were created equal. The only difference between the different lens designs is the actual fitting philosophy used by the manufacturer.
Studies have shown that the clinical outcomes are equal irrespective of the design used, so the most important thing to consider when starting with ortho-k is which design you think will work best for you; then stick with it until you master it.14
Of great advantage is the technical help offered by all the manufacturers during the critical learning curve (the first 20 cases). Also critically important are your clinical skills, including patient suitability, interpretation of the lens fit and the ability to accurately interpret the topography maps.
Myth #5: All you need to get started is the FDA certification course.
The completion of a certification course simply means you have the right to start to learn how to fit ortho-k lenses; it does not confer clinical expertise. The best way of gaining the required knowledge is to join a professional organization that provides the training and support that is required to really get you started with confidence.
The Orthokeratology Academy of America (OAA) provides great scientific content, and its annual conference always incorporates a “boot camp” for beginners. The OAA is in the process of becoming an international body, which bodes well for the future of ortho-k.
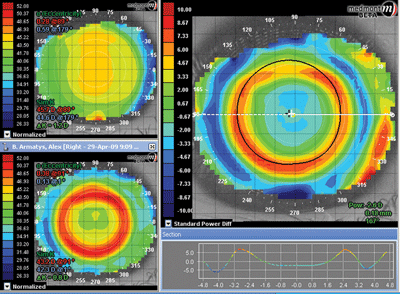
3. Corneal topography maps showing a well-centered lens and good refractive change.
Modern marketing has a tendency to oversimplify things in order to increase market penetration and usage. We see this with the misconception that ortho-k is another cookie-cutter approach to fitting a contact lenses. While in some instances, such as when dealing with an ideal corneal shape and a simple refractive error, this may be true, but it is certainly not the case in more complex fittings. When practitioners say that they have tried ortho-k and it didn’t work for them, they usually mean that they have tried the simple approach and it didn’t work, but they didn’t take the time to properly learn how to fit the lenses.
To successfully incorporate ortho-k into your practice, initially ignore the marketing, and instead concentrate on the basics. Understand the science, go to the experts for training, get good gear (trial lens sets and topographer) and, most importantly, start off with the simple, low myopia cases.
Mr. Mountford entered private practice after graduating from the Queensland University of Technology in 1975. He specializes in contact lenses for keratoconus, post-PK, pediatric aphakia, orthokeratology and the medical applications of scleral lenses. He is a fellow of the American Academy of Optometry, a founding fellow of the Cornea and Contact Lens Society of Australia and a fellow of the British Contact Lens Association.
1. Nolan J. The first orthokeratology meeting. Contacto. 1995;38(4):9-14. Reprinted in: Mountford J. Orthokeratology, Principles and Practice. New York: Butterworth-Heinemann, 2004.
2. Kerns RL. Research in orthokeratology. Part VII: examination of techniques, procedures and control. J Am Optom Assoc. 1977 Dec;48(12):1541-53.
3. Cho P, Cheung SW, Edwards M. The longitudinal orthokeratology research in children (LORIC) in Hong Kong: a pilot study on refractive changes and myopia control. Curr Eye Res. 2005 Jan;30(1):71-80.
4. Walline JJ, Jones LA, Sinnott LT. Corneal reshaping and myopia progression. Br J Ophthalmol. 2009 Sept;93(9):1181-5.
5. Kakita T, Hiraoka T, Oshika T. Influence of overnight orthokeratology on axial length elongation in childhood myopia. Invest Ophthalmol Vis Sci. 2011 Apr 6;52(5):2170-4.
6. Legerton J. Taking a wholistic approach to refractive therapy. Rev Cornea Contact Lens. 2012 Apr;149(3):19-22.
7. Hayashi TT. Mechanics of contact lens motion. PhD Thesis, School of Optometry, UC Berkeley. 1977.
8. Hayashi TT, Fatt I. Forces retaining a contact lens on the eye. Am J Optom Physiol Opt. 1980 Aug;57(8):485-507.
9. Mountford J, Ruston D, Dave T. Orthokeratology: Principles and Practice. London: Butterworth Heinemann; 2004:255-69.
10. Mountford J, Ruston D, Dave T. A model of forces acting in orthokeratology. In Orthokeratology: Principles and Practice. London, Butterworth Heinemann; 2004:269.
11. Mountford J. An analysis of the changes in corneal shape and refractive error induced by accelerated orthokeratology. Int Contact Lens Clinic. 1997;24(4):128-44.
12. Cho P, Lam A, Mountford J, Ng, L. The performance of four different corneal topographers on normal human corneas and its impact on orthokeratology lens fitting. Optom Vis Sci. 2002 Mar;79(3):175-83.
13. Mountford J, Noack D. Corneal topography and orthokeratology: post-fit assessment. Contact Lens Spectrum. 2002 Jun;17(6):43-9.
14. Tahhan N, Du Toit R, Papas E, et al. Comparison of reverse geometry designs for overnight orthokeratology. Optom Vis Sci. 2003 Dec;80(12):796-804.


