 Sometimes we, as practitioners, get so busy in our daily routines that we forget to stop and think of other possible options for our patients. Today, GP lens manufacturers have increasing capabilities with their lathes and software to make lenses more customized than in the past. This month’s column describes a patient that, more than likely, would have been dissuaded from contact lens wear by the vast majority of providers––but, with a little creativity, turned into a happy, successful lens wearer.
Sometimes we, as practitioners, get so busy in our daily routines that we forget to stop and think of other possible options for our patients. Today, GP lens manufacturers have increasing capabilities with their lathes and software to make lenses more customized than in the past. This month’s column describes a patient that, more than likely, would have been dissuaded from contact lens wear by the vast majority of providers––but, with a little creativity, turned into a happy, successful lens wearer.
J.J. is a 58-year-old female who was referred to the contact lens service because she had an interest in contact lens wear. She reported having worn “hard” lenses many years ago, but had stopped due to dryness and discomfort. She now only wore distance correction glasses, removing them to read.
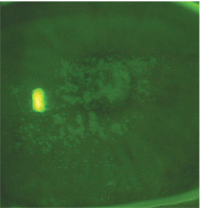
1. Corneal staining in the right eye.
She reported having dry eyes, used lubricating drops two to three times a day, had no other ocular or systemic history and had no other complaints other than the dryness and the desire for contact lenses.
Her corrected visual acuity measured 20/25-1 at distance O.U., and 20/40 uncorrected at near O.U. All entrance testing was normal. Refraction yielded a prescription of -3.00–3.00 x 178 in the right eye and -2.75–3.25 x 5 in the left eye, correcting to 20/25 in each eye. Her near add was measured to be +2.25D. Slit lamp examination revealed 1-2+ superficial punctate keratitis (SPK) O.U. (figure 1). There was minimal injection of the conjunctiva and minimal evidence of lens changes. Fundus examination was unremarkable.
At this point, given her significant astigmatic prescription, presbyopia and dry eyes—to the point of having obvious corneal staining—my initial thought was that wearing contact lenses would not be possible. But stepping back to assess the situation, I thought about how I would manage her if she presented to me for treatment of her dry eyes. I would certainly consider all the treatment options, one of which could be scleral GP lenses. The more I considered the option of fitting her in scleral lenses—the potential benefits for her dry eyes and good vision correction—the more I thought this option had room to succeed. The only consideration would be how to account for near vision. Right now, J.J. only used her glasses for distance. It would not be that helpful to go from wearing glasses only for distance to using reading glasses.
At this point, I decided to contact one of the labs that I order scleral lenses from to ask if they could put a front surface add power on their scleral lens. The technician replied, “yes.” I offered this option to J.J., and she eagerly accepted the idea of fitting her in scleral bifocal GPs.
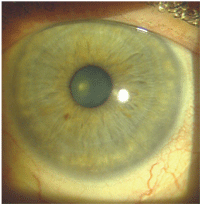
2. Scleral lens in the right eye.
The best attempt at keratometry through the corneal irregularity revealed Ks in the 43.00D to 46.00D range in each eye. A fitting was undertaken with a 15.0mm diameter lens, with the goal to have full corneal clearance. I chose a 15.0mm lens over something larger to try to ensure good centration for the bifocal. Larger diameter lenses, in my experience, have an increased tendency to ride just slightly low, which might create vision problems with the bifocal.
The final lens fit in each eye resulted in good centration, approximately 100µ of corneal clearance at the shallowest point and good scleral alignment (see figures 2 and 3). The lenses were ordered with the distance prescription in each eye, with a 2.0mm zone of +2.25D add in the center of each lens for near. The lenses were dispensed and the vision with the lenses was 20/20 O.U. at distance and 20/25 O.U. at near. J.J. had no problems mastering the insertion and removal process, and the care regimen was carefully explained to her. Because these lenses were corneal vaulting, fluid ventilated lenses, they were not fenestrated and required filling with non-preserved saline solution at insertion. At the two-week follow-up visit, J.J. reported using the lenses up to 12 hours a day with good comfort, good vision and no problems.
This case brings out a few worthwhile points. First, scleral lenses can be useful for dry eye patients––even those without pathologic dry eye. Choosing those patients carefully can produce good results in situations that would otherwise be hopeless for contact lens wear. Second, multifocal optics can be cut on many lens designs, even those not specifically advertised, by simply asking your lab. You may find this true even with some of your current lenses. When faced with a scenario that seems like a no-win situation, take a step back, think outside the box for a minute and you may turn that no-win situation into a win-win for you and your patient.

3. Approximately 100µ of apical corneal vault in the right eye.


