At the same time, the industry is experiencing less than 2% annual net growth. Even though more than four million new patients are dispensed their first contact lenses each year, we seem to be taking one step back for each step forward, as a nearly equal number of existing wearers discontinue.
Do Poor Fits Lead to Dropouts?
One must wonder if there is some correlation between the low made-to-order market share and the high dropout rate.
Making millions of one product design is a manufacturer’s dream; making one of a million is their nightmare. Most would agree that the major cast-molded soft lens manufacturers have executed with excellence in their material and surface modification science, low stock-keeping unit design strategies and low-cost manufacturing. They have also made it incredibly easy for eye care practitioners to prescribe their lenses. The manufacturers provide in-office inventories that enable same-day dispensing, and they use direct-to-consumer advertising to raise awareness of contact lenses generally and their brands in particular. Despite these excellent marketing and manufacturing techniques, the industry’s lackluster growth leaves much to be desired.
| |
| |
|
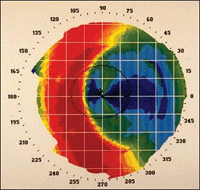
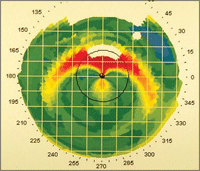
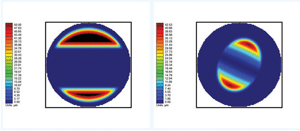
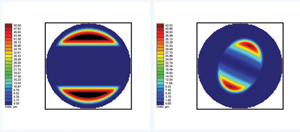
Fig.1. Two topographic images showing post-treatment corneas with overnight reshaping lenses which were not centered.
|
Add to this phenomenological overview the reality that third-party reimbursement entities structure fees for contact lens evaluations and lenses by category and pricing. It appears that these entities treat all lenses the same—as though they are all low-cost, cast-molded lenses. Additionally, they treat customized soft lenses as though they carry the same chair time and lens cost basis as low-cost, cast-molded lenses to both the practitioner and patient alike.
Patient fees for customized lenses are greater than those for production lenses purchased through fulfillment businesses. The fees from practitioners for customized lenses are also significantly greater than what is paid to them by third-party plans. These disparities create issues for patients and practitioners.
Lack of patient knowledge about customized lens alternatives requires eye care practitioners to spend extra time in consultation and patient education. For the busy practitioner, this can be painful chair time. The innocent naïveté of consumers constrains our opportunity to better serve them with customized soft lenses. These market forces discourage practitioners from providing their patients with the best possible solution when patients could benefit from customized lenses.
Practice patterns must respect market forces. As a result, the customized lens opportunity must be orchestrated through efforts to drive unnecessary cost out of the delivery. The three tenets of supply chain management for customized lenses are:
(1) greater efficiency in manufacturing
(2) technology-driven prescribing
(3) delegation of information gathering and task completion to ancillary personnel
A number of factors are allowing customized lens manufacturers to produce quarterly replacement lenses, and in some cases, monthly replacement lenses on a competitive basis: numerically controlled lathes, auto-loading robotics, and low-cost latheable conventional hydrogel, silicone hydrogel and base curve molded buttons. It is hoped and forecast that manufacturers will continue to drive down the costs. Economies of scale may also result in lower cost of lenses, as the segment of customized soft lenses expands to its potential to serve the percentage of wearers who are expected to need them.
Moving from Art to Science
One attribute of our rapidly transforming profession is the addition of imaging, sensing and automated measuring devices. Many practitioners have enjoyed the adoption of corneal topography to assist their rigid lens parameter selection. Topography software for contact lenses—which is compatible with many brands of topographers—has been distributed for customized lenses. For example, the Paragon CRT software suggests the starting lens for corneal refractive therapy and has demonstrated final lens accuracy of about 80%.2
Following lens fitting, videokeratographic images are useful in identifying a well or poorly fit lens (Figure 1).
Customized soft lens fitting can also be enhanced by technology. The advent of anterior segment OCT software, and now what is referred to as “fringe topography,” where a fringe pattern is projected onto the ocular surface after instillation of sodium fluorescein. This technology is used with the Eye Surface Profiler (Eaglet Eye), or ESP for short, which provides a means of understanding full ocular contour out to a chord diameter of 20mm. These data provide a means of correlating soft lens design with known ocular contour.
|
|
|
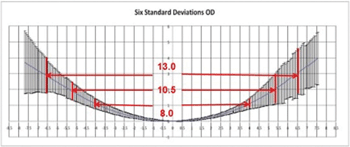
Fig. 2. Ocular contour plot in a single meridian of normal eyes showing geometric diversity to six standard deviations.
|
For instance, using a fringe topographer to gather a normal distribution of contours circumferentially in a population of normal eyes, Figure 2 demonstrates six standard deviations of the measures of the horizontal meridian of all right eyes. These data illustrate the significant difference in the sagittal depth of eyes at the chord where soft lenses make scleral contact.
An initial reaction to these data is one of amazement that a production lens of one diameter and one base curve could fit the majority of the normal population. Is it possible that the production lenses are not the best option in a significant percentage of cases? In fact, Alonso-Caneiro et al. discovered corneoscleral morphology changes after wearing soft lenses daily.3 This finding may support the notion of improper lens fitting and may reveal the role of fit as a possible ingredient in end-of-day discomfort or low-grade inflammatory response.
Kollbaum et al. reported the optical power differences of soft lenses when on the eye and when off the eye.4 Their conclusions support the existence of soft lens deformation on-eye. This stands to reason, as the mean flat keratometry value of human eyes is about 7.8mm while the mean soft lens base curve is about 8.3mm. Additionally, the power of soft lenses is not adjusted for a tear lens power. In other words, the soft lens is known to “drape” or conform (deform) to the shape of the underlying cornea. At the same time, a monocurve lens, which also has a base curve of about 8.3mm, extends onto the sclera, which has a radius of about 12.5mm, and appears to conform (deform) to a compatible lens-eye relationship.
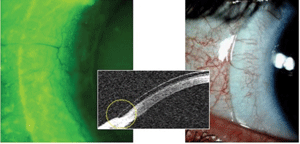
Figure 3 displays an OCT image of a soft lens that is not fully conforming to the scleral sagittal depth and volume and is impinging. Vicoh team observations of ocular contours matched with successfully fit soft lenses reveal that the majority of soft lenses are about 200µm deeper than the eye to which they are fit.
Another observation from fringe topography of human eyes reveals a zone that extends out from the limbus, which is concave away from the eye when mapped and measured at 60µm steps. Consider that most soft lenses have concave toward the eye ocular surfaces. This means a concave toward the eye ocular lens surface is mated to a concave away from the eye scleral contour. This represents a mismatch to the eyes in the normal distribution and an angle of incidence of the lens periphery that would suggest impingement. This concave away from the eye ocular contour is the rationale for the convex toward-the-eye (or posteriorly convex) landing zone used in some scleral lens design philosophies, such as that of the NormalEyes 15.5 (Paragon Vision Sciences).5
| |
|
Fig. 3. OCT image of a soft lens with conventional curvature incident on the bulbar conjunctiva.
|
There is an opportunity to use ocular contour mapping for soft lens design to reduce corneoscleral morphology changes and lens deformation. The design rationale would use clinical markers or metrics to determine the parameter values. One example is a soft lens design produced for independent laboratories by Vicoh. Four clinical metrics are used to determine four parameter values (Table 1). Manifest refraction determines lens power; flat keratometry establishes base curve; corneal diameter (horizontal visible iris diameter) provides overall lens diameter; and OCT or ESP reveals the landing zone angle.
Alternatively, a diagnostic set with base curve radii, overall diameter and landing zone angle increments can be used to select the landing zone angle by observation. The greatest chair time efficiency is achieved with clinical measurements alone rather than with diagnostic lens observations.
The first objective in ocular contour-driven soft lens design is to reduce lens deformation, which induces higher-order aberrations and confounds precision optics for peak clarity and optimum simultaneous vision optics needed for multifocal lenses. The second objective is to produce the best possible corneoscleral lens-eye relationship to reduce morphology changes and any adverse response from excessive localized mechanical interaction. The third objective is to improve the extension of lenses onto the sclera for consistency of fit over the population distributions of corneal diameter.
These three distinct objectives are met in a number of ways: the first by matching the soft lens radius more closely to the corneal radius; the second by matching the landing zone angle more closely to the corneoscleral contour; and the third by selecting an overall diameter that is respective of the corneal diameter.
|
Table 1. Clinical Metrics for Empirical Ordering of Custom Soft Lenses
| |
|
Clinical Metric
|
Lens Parameter
|
|
Manifest Refraction
|
Power
|
|
Keratometry
|
Base Curve Radius
|
|
Corneal Diameter
|
Overall Lens Diameter
|
|
Sag of Eye at Key Chord for Design
|
Landing Zone Angle
|
Information Delegation
The beauty of technology-driven prescribing is the relative independence of instrument accuracy and repeatability from the operator. For example, it doesn’t matter who operates a corneal topographer or the ESP—the results will be the same regardless. As such, ancillary personnel can gather the data needed for a custom soft lens order.
The measures of flat keratometry and corneal diameter can be accomplished with most modern corneal topographers. Ocular contour can be measured with an OCT or an ESP. Anticipated future advancements in OCT software will provide more nuanced measurements of corneoscleral geometry to help us better determine the appropriate landing zone angle of the lenses discussed earlier. These same data can be used for toric soft lens design. Added measurements of lid position allow for custom superior and inferior slab off dimensions (Figure 4).
Technology-driven prescribing can also help to resolve the enigma of presbyopia correction with soft lenses. It is well understood that the visual axis is nasal to the geometric center of the pupil, while the most common soft lens displacement is temporal. Chateau et al. observed a mean deviation of the geometric center of soft lenses to be more than 0.4mm temporal to the pupil center and a near equal amount inferior to the pupil center.6 These data suggest that the optical center of the average lens could approach 1.0mm from the visual axis. As such, there is a need for a visual axis-aligned multifocal that would be fit with the same precision as progressive addition spectacle lenses.
|
|
|
|
|
Fig. 4. Two toric lenses with different slab-off dimensions to conform to two different eyes with different upper/lower lid positions.
|
Pupil size and reactivity also have a population distribution and play an important role in selecting segment sizes and optics to improve simultaneous vision designs in presbyopia correction. These can also be measured clinically through a number of methods.
Customized spherical aberration correction can be used to improve the vision of the largest contact leans wearing demographic (i.e., patients between the ages of 18 and 34). The eyes of younger wearers are inclined to manifest larger pupil sizes, resulting in differences between their daytime small-pupil refraction and nighttime larger-pupil refraction due to spherical aberration. This age group also typically enjoys a greater frequency of nighttime spectator activities and greater nighttime driving hours per week. Wavefront aberrometry over the full natural pupil under scotopic conditions will demonstrate the spherical aberration of each eye. Customized lenses can be made with two or more spherical aberration levels for each lens power.7
Finally, a thin soft lens for keratoconus may also be designed using population distribution of ectasia. Schwiegerling et al. measured eyes with keratoconus that were not deformed by rigid contact lens wear. He found a population distribution that could be described by the displacement of the apex of the cone, the width of the cone and the sagittal height of the ectasia from a reference sphere.8 These data were used to design a series of soft lenses with posterior divots, which can be selected by use of corneal topography.9 The peripheral landing zone angles and overall diameters can also be selected in the same manner as soft lenses using OCT or ESP as previously described.
I believe there is a clear opportunity to expand customized lens use beyond its current confines to provide better vision, comfort and health for a significant percentage of patients who are candidates for soft lenses. The most significant missing piece has been the knowledge of ocular contour, as Otto Wichterle—the person credited with inventing the soft lens—himself believed.10 The hypothesis that a significant number of soft lens wearers drop out due to inadequacies that would be overcome by customized lenses is worth researching.
Customized lens laboratories are making great strides in their adoption of more precise manufacturing and metrology technology. Material suppliers are increasing their efficiency in button production and advancements, including base curve molded buttons. They are also supporting the laboratories by enabling technologies that include specialized surface treatments and lens tinting. In-office instrument technology can now link the eye care practitioner directly to the sophisticated apparatus of industry.
1. Andre MP, et al. The effect of corneal diameter on soft lens fitting, part 2. Contact Lens Spectrum May 2002.
2. Data on file; Paragon Vision Sciences
3. Alonso-Caneiro D, et al. Using optical coherence tomography to measure corneoscleral morphology after soft contact lens wear. Optom Vis Sci. 2012; 89(11):1619-1625
4. Kollbaum PS. Comparing the optical properties of soft contact lenses on and off the eye. Optom Vis Sci. 2013;90(9):924-936.
5. Legerton JA. It’s time to rethink mini-scleral lenses. Rev Optom. 2010 April 10.
6. Chateau N, et al. Infrared pupillometry in presbyopes fitted with soft contact lenses. Optom Vis Sci. 1996 Dec; 73(12):733-41.
7. US Patent 8,430,511. Kit of higher order aberration contact lenses and methods of use.
8. Schwiegerling J. Cone dimensions in keratoconus using Zernike polynomials. Optom Vis Sci. 1997; 74(11) 963-969.
9. US Patent 8,083,346. Contact lens for keratoconus.
10. Wichterle K, et al. Shape of the cornea and conjunctiva. Optom Vis Sci. 1991;68(3)232-5.


