 Gas-permeable lenses circulate fluid under the lens by the vertical movement with the blink. There is rapid turnover of the tears under the lens. When the Dk of lenses was negligible, these tears provided an important source of oxygen. But as Dk and diameter have increased, lens movement has decreased.
Gas-permeable lenses circulate fluid under the lens by the vertical movement with the blink. There is rapid turnover of the tears under the lens. When the Dk of lenses was negligible, these tears provided an important source of oxygen. But as Dk and diameter have increased, lens movement has decreased.
Large diameter GP lenses, such as intra-limbal, minisclerals and sclerals, present an interesting challenge to solution selection because of this change in fluid dynamics.
Fluid Dynamics
Large diameter lenses move fluid under the lens with a diaphragm movement, rather than by a vertical movement. The change in fluid dynamics creates two situations:
1. Solution in the bowl of the lens is “trapped” under the lens. It is pumped out relatively slowly—the solution will be in contact with the cornea for a longer period of time.
2. Tears and solutions stagnate under the lens causing an increase in tear viscosity. This will result in mucous rolling and debris formation, which in turn will stick to the back of the lens and to the cornea.
Taking Care with Solutions
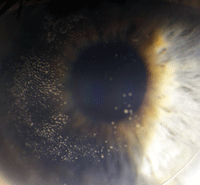
Mucous plaque formation.
Conditioning solutions are both wetting agents and cushioning solutions. In large diameter lenses, the viscosity agent may cause visual blur, which can last up to several hours, since the thick solution is not quickly removed by the tear pump. Since solution exchange occurs at a much slower rate, the preservative in many disinfecting solutions may result in significant solution-induced corneal toxicity.
Beyond blur on insertion, a highly viscous solution will further slow fluid exchange and increase mucus formation. It has been long known that stagnating tears increase in viscosity and result in mucus clumping. Hydroxy-propyl-methyl-cellulose (HPMC), a viscosity agent found in many lubricating and conditioning solutions, will further aggravate this situation. Interestingly, the diaphragm movement of the lens, as well as the central retinal artery pulse, will roll this mucus into rows. Mucous rolls will likely cause the patient complaint of foggy vision and the need to remove the lens several times per day. If the wettability of either the cornea or lens decreases, mucus may become adherent to the posterior lens surface.
Mucous plaque formation will cause discomfort. Eventually the lens will not be able to be inserted without pain and the plaque must be removed from back surface of the lens (see image below).
Cleaning the Lens
When dealing with large diameter GP lenses, the following tips minimize solution/cleaning related complications:
• Since it is necessary to use solution to fill the bowl of the lens upon insertion to avoid trapped bubbles under the lens, a low viscosity/preservative-free agent will have better initial patient acceptance and eventual decreased mucus formation.
• Saline will not effectively wet the surface of the lens and non-wetting areas may result; however, preservative-free/buffer-free saline (0.9% sodium chloride respiratory therapy vials) may be used to fill the bowl. (For more information, see “Going Off Label,” Lens Care Update, Review of Cornea & Contact Lenses, March 2011.)
• Instruct the patient to diligently clean the inside of the lens.
• If the patient experiences heavy mucus formation, the lens may need to be removed and cleaned during the day. This is particularly true for corneal graft patients who may experience higher mucus formation rates.
• Progent (Menicon) is highly effective at removing mucous plaque formation and is now available for home use. A monthly application is recommended.
Extremely large GP designs have many benefits. For some irregular corneas they have become nearly essential. With these new designs, however, must come a new understanding of the importance of fluid dynamics and the solutions we use.


