 We complain about and cite poor compliance as a major risk factor for contact lens infections. Yet, in some of our own practices, we routinely make common compliance mistakes.
We complain about and cite poor compliance as a major risk factor for contact lens infections. Yet, in some of our own practices, we routinely make common compliance mistakes.
The Importance of Hand Washing
Bacteria and viruses are commonly transmitted through the hands of health care workers. Hand washing is the single most important intervention to prevent the spread of disease. Keep in mind, I mean hand washing by all office employees. Numerous infectious outbreaks have been traced to contaminated hands of healthcare workers, including reports of epidemic keratoconjunctivitis.1
In spite of these concerns, compliance with hand washing guidelines remains a problem in most health care settings. Even in controlled study conditions, the hand washing rate usually does not exceed 40%.2 A number of factors are associated with low rates of compliance, including the lack of availability of sinks, skin irritation with repeat exposure, high work volume and low perceived risk.2
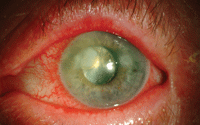
Compliance in our own practices can help prevent serious infections.
Washing hands for 15 seconds achieves a microbial kill of 100.6 – 1.1 and for 30 seconds 101.8-2.8.3 Unfortunately, however, many individuals wash their hands for less than 10 seconds, which may not achieve a satisfactory microbial kill rate.
According to the Centers for Disease Control and Prevention, using solutions that contain 60% to 70% alcohol are most effective on gram-positive, gram-negative and spore-forming bacteria, as well as fungi and viruses.4 Hand disinfectant should be used regularly throughout the practice, but use standard hand washing when handling contact lenses.
Contact Lens Hygiene
It is vital to properly clean and store reusable contact lenses. The American National Standards Institute last updated the criteria for in-office disinfection of contact lenses in October 1999. However, the changing lens material and care product market leaves the practitioner with questions on how to clean, disinfect and store current non-disposable diagnostic lenses.
• Gas-permeable (GP) lenses are fairly easy to clean and disinfect. Start by using a GP-approved cleaner or polish for a wash. Soak in ophthalmic-grade hydrogen peroxide for 10 minutes. Rinse with saline and store dry. Finally, lubricate with conditioning solution prior to insertion.
• For soft lenses, autoclaving is the only 100%-effective disinfection method. However, most practitioners use multipurpose solutions to disinfect and store lenses. If a multipurpose solution is used, follow the manufacturer’s recommendations on rubbing, rinsing and solution replacement (usually every 30 days).
The Role of Tap Water
The use of water with contact lenses is significantly linked to microbial keratitis infections, specifically Acanthamoeba. During the past decade, the Environmental Protection Agency has downregulated control of Acanthamoeba in the U.S. tap water supply. They have cited that the critical point identification for the presentation of Acanthamoeba in contact lens wearers is personal hygiene, not drinking water.5 Therefore, regulating Acanthamoeba will not reduce health risk for the general population.
However, numerous studies have shown that direct contact with water—including tap water, swimming pools, hot tubs and showers—is the primary point of contamination and subsequent infection with the organism.6-9
The lesson: Hands should be thoroughly dried before handling lenses. When rinsing cleaner from GP lenses, switch to sterile saline or multipurpose solution.
Being ever vigilant about our own compliance habits will ensure patient safety in our own practices.
1. Larson EL, Bryan JL, Adler LM, Blane C. A multifaceted approach to changing handwashing behavior. Am J Infect Control. 1997;25:3-10.
2. Larson E, Killien M. Factors influencing handwashing behavior of patient care personnel. Am J Infect Control. 1982;10:93-9.
3. Rofter M. Hand washing and hand disinfection. In: Mayhall CG, ed. Hospital epidemiology and infection control. 1st ed. Baltimore, MD: Williams and Wilkins. 1996:1052-68.
4. The U.S. Centers for Disease Control and Prevention. Available at: www.cdc.gov (accessed April 2012).
5. EPA. Health effects support document for Acanthamoeba. 2003. Available at:
http://nepis.epa.gov/Exe/ZyNET.exe/20003KD0.TXT?ZyActionD=ZyDocument&Client=EPA&Index=2000+Thru+2005&Docs=&Query=FNAME%3D20003KD0.TXT%20or%20(%20epa%20or%20water%20or%20standard%20or%20Acanthamoeba)&Time=&EndTime=&SearchMethod=1&TocRestrict=n&Toc=&TocEntry=&QField=&QFieldYear=&QFieldMonth=&QFieldDay=&UseQField=&IntQFieldOp=1&ExtQFieldOp=1&XmlQuery=&File=D%3A%5Czyfiles%5CIndex%20Data%5C00thru05%5CTxt%5C00000007%5C20003KD0.txt&User=ANONYMOUS&Password=anonymous&SortMethod=h%7C-&MaximumDocuments=10&FuzzyDegree=0&ImageQuality=r75g8/r75g8/x150y150g16/i425&Display=p%7Cf&DefSeekPage=x&SearchBack=ZyActionL&Back=ZyActionS&BackDesc=Results%20page&MaximumPages=1&ZyEntry=1&SeekPage=x&ZyPURL (accessed April 2012).
6. Anger C, Lally JM. Acanthamoeba: a review of its potential to cause keratitis, current lens care solution disinfection standards and methodologies, and strategies to reduce patient risk. Eye Contact Lens. 2008 Sep;34(5):247-53.
7. Mubareka S, Alfa M, Harding G, et al. Acanthaemoeba species keratitis in a soft contact lens wearer molecularly linked to well water. Can J Infect Dis Med Microbial. 2006 Mar-Apr;17(2):120-2.
8. Caumo K, Rott MB. Acanthamoeba T3, T4 and T5 in swimming-pool waters from Southern Brazil. Acta Trop. 2011 Mar;117(3):233-5.
9. Bonilla-Lemus P, Ramírez-Bautista GA, Zamora-Munõz C, et al. Acanthamoeba spp. In domestic tap water in houses of contact lens wearers in the metropolitan area of Mexico City. Exp Parasitol. 2010 Sep;126(1):54-8.


