 |
A 12-year-old male was referred with a history of chronic blepharoconjunctivitis, stating that his eyes are intermittently red and painful. His parents noticed a “globule” next to his right temporal cornea. His previous doctor treated him with Tobradex, which would improve his symptoms, but his discomfort returned upon cessation.
His history is significant for Jacobsen syndrome (chromosome 11 deletion disorder, affecting about 1 in 100,000), which causes heart disease, frequent infections, facial/skeletal abnormalities, GI tract problems, kidney malfunction and developmental delays. He did not have a history of atopic disease.
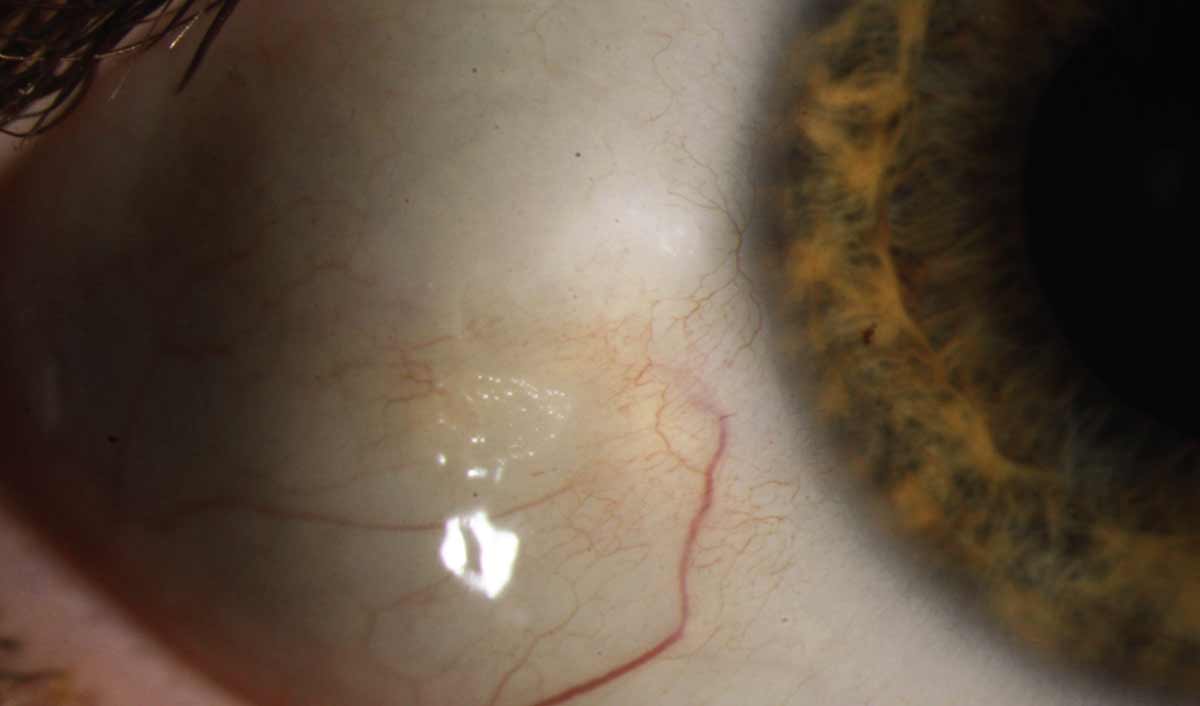
He was noted to have 20/20 vision in each eye. He had mild inspissation of all meibomian glands as well as significant lagophthalmos. His corneas were clear centrally with anterior stromal scarring at the nasal limbus in the right eye, with adjacent conjunctival hyperemia. A Bitot spot was noted on the temporal conjunctiva of the right eye.
Our patient was diagnosed with conjunctival xerosis; serum vitamin A levels were ordered. He was started on prednisone drops TID with a one-month taper. He was recommended ointment and occlusion at bedtime and preservative-free lubrication during the day.
A Bitot spot is a superficial buildup of keratin and loss of goblet cells on the conjunctiva, located in the exposure zone. They are classically associated with vitamin A deficiency; however, they may be associated with other vitamin deficiencies and exposure patterns. Our patient did not have vitamin A deficiency, but did improve with decreased exposure and intense lubrication.
 |
|
Click image to enlarge. |
A recent case series reported Bitot-like spots with lab-confirmed normal serum vitamin A levels. They found the spots indistinguishable both clinically and histopathologically from classic Bitot spots. These spots were noted to occur in a range of anterior segment pathologies, including aniridia, WAGR syndrome, Axenfeld–Rieger syndrome, and blepharokeratoconjunctivitis. Vitamin A deficiency–related Bitot is more likely to be bilateral, while other causes may have unilateral presentations.
Vitamin A serum workup is essential, since low levels could lead to nyctalopia, corneal ulceration or keratomalacia. Treatment of exposure-related conjunctival xerosis includes steroid/antibiotic bursts, lubricating drops/ ointments, amniotic membrane, bandage soft/ scleral lenses, tape/surgical tarsorrhaphy and moisture chamber goggles.


