 Corneal epitheliopathies can be complicated to manage, since they arise from a multitude of different causes that are often difficult to resolve. Many times, the pattern of the affected cornea can help make the diagnosis, though some atypical presentations can be confounding. Symptoms of corneal epitheliopathies can include grittiness, burning, dryness, watering, photophobia and blurry vision. Therapeutic options include lubricants, Restasis (cyclosporine, Allergan), topical steroids, punctal occlusion, contact lenses, tarsorrhaphy and limbal stem cell transplants.
Corneal epitheliopathies can be complicated to manage, since they arise from a multitude of different causes that are often difficult to resolve. Many times, the pattern of the affected cornea can help make the diagnosis, though some atypical presentations can be confounding. Symptoms of corneal epitheliopathies can include grittiness, burning, dryness, watering, photophobia and blurry vision. Therapeutic options include lubricants, Restasis (cyclosporine, Allergan), topical steroids, punctal occlusion, contact lenses, tarsorrhaphy and limbal stem cell transplants.
Scleral lenses, an increasingly popular treatment option, can benefit patients with chronic corneal epitheliopathy and related symptoms by keeping the fluid reservoir in contact with the corneal surface, and by providing the superior optics of gas-permeable lenses for vision correction. This month’s column spotlights a case in which an unusual type of corneal epitheliopathy defies other treatment options but benefits greatly from a scleral GP lens.
A Case Study
A 37-year-old black male was referred for a contact lens fitting by his corneal specialist. He had previously seen several eye care providers for symptoms of photophobia, blurry vision and chronic irritation. Over the course of these visits, he had been diagnosed with dry eye and treated with lubricants, Restasis, punctal occlusion and topical steroids. All of these treatments had provided only minimal improvement; he still suffered, and continued to wear sunglasses indoors and two pairs of sunglasses when outside. His vision had deteriorated to the point that he felt unsafe driving.
The corneal specialist had diagnosed him with a corneal epitheliopathy; however, at this time the specific etiology was undetermined. Prior to any surgical intervention, it was recommended that he consider scleral lenses.
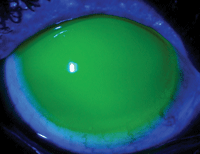
1a. Scleral lens fit O.D.
At examination, his uncorrected acuity was 20/60 O.U. A refraction did not improve his vision. Slit lamp exam revealed 2+ bulbar conjunctival and limbal injection, and 2 to 3+ whorl-like corneal staining. Within the densest areas of staining, there were small, elevated concentrations of epithelium. The palpebral conjunctiva was also 2+ injected O.U., but all other internal and external finding were normal.
After discussing his options, the patient consented to a trial of scleral lenses. A lens was placed on each eye and he could report some immediate improvement in his ocular comfort. With an over-refraction, he was capable of seeing nearly 20/20 in each eye. He was fitted and the following Jupiter lenses in Boston XO material with standard peripheral curves were ordered: 46.00mm base curve, -1.75D power and 15.6mm diameter O.D.; 46.00mm base curve, -2.00D power and 15.6mm diameter O.S.
Analysis
The reason for this particular choice of lenses was twofold. First, because of his chronic photophobia and sensitive eyes, it would have been difficult to use a lens with a larger diameter. The Jupiter design on an essentially normal corneal shape would provide a good tear reservoir centrally, where the bulk of the epitheliopathy was located.
Secondly, the lens fit provided full corneal vaulting and good centration (figures 1a and 1b). The visual acuity with the lenses was 20/20 in each eye. The patient still reported a degree of photosensitivity, but the feeling of irritation was alleviated and he was generally pleased with the comfort and thrilled with his vision. He was able to function indoors without sunglasses, and outdoors with just one pair. He continues to wear the lenses full time.
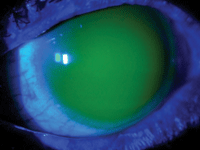
1b. Scleral Lens fit O.S.
Whorl-like corneal epitheliopathy can be seen in patients with certain specific systemic diseases such as incontinentia pigmenti, keratoconus with GP lens wear, limbal stem cell deficiencies or post-penetrating keratoplasty.1-3 Depending on the severity of the epithelial disease, a variety of therapies can be effective. In many cases, however, vision can be restored, improvements in the health of the epithelium and symptomatic relief can all be achieved with the simple use of a scleral GP lens.4
1. Selvadurai D, Salomão DR, Baratz KH. Corneal abnormalities in incontinentia pigmenti: histopathological and confocal correlations. Cornea. 2008 Aug;27(7):833-6.
2. Somodi S, Hahnel C, Slowik C, et al. Confocal in vivo microscopy and confocal laser-scanning fluorescence microscopy in keratoconus. Ger J Ophthalmol. 1996 Nov;5(6):518-25.
3. Ozbek Z, Raber IM. Successful management of aniridic ocular surface disease with long-term bandage contact lens wear. Cornea. 2006 Feb;25(2):245-7.
4. Rosenthal P, Croteau A. Fluid-ventilated, gas-permeable scleral contact lens is an effective option for managing severe ocular surface disease and many corneal disorders that would otherwise require penetrating keratoplasty. Eye Contact Lens. 2005 May;31(3):130-4.


