Traditionally, discoveries in medicine take years, even decades, to conclude. However, in just two years, the International Workshop on Meibomian Gland Dysfunction was able to develop a better understanding of the meibomian glands as they relate to dry eye. The study involved the clinical research of 50 international experts that began in November 2008, and continued with a review of outlines and the drafting of reports following the Association for Research in Vision and Ophthalmology (ARVO) meeting in May 2009. After reviewing the literature and combining the findings with evidence-based research, the final draft of the MGD workshop was completed in April 2010.1
Definition
Meibomian gland dysfunction, or MGD, is the leading cause of dry eye syndrome (DES). The term “meibomian gland dysfunction” evolved in the mid-1980s. Since then, other terms such as posterior blepharitis, meibomian gland disease, meibomianitis, meibomitis and meibomian keratoconjunctivitis have been termed by clinicians to describe MGD and lid disease.
Although literature has referred to posterior blepharitis and MGD interchangeably, the two are not synonymous. MGD is strictly a term used to describe an obstruction within the glands themselves and changes in the secretion of meibum from the gland. By altering the tear’s composition, the patient may experience symptoms of dry eye, irritation and discomfort.1 Posterior blepharitis is defined by inflammation of the posterior lid margin. Early gland dysfunction may not show signs of blepharitis as the inflammation is not always present.1
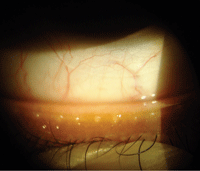
Clogged meibomian glands in a contact lens patient complaining of intolerance. (Photo: Mile Brujic, O.D., and Jason Miller, O.D., M.B.A.)
Etiology
MGD has been a clinical condition for more than 100 years. The Report of the International Workshop of MGD points out significant evidence as to the causes of gland dysfunction, but systemic and ocular contributions remain unknown.1 We know that MGD contributes to a subset of DES called evaporative dry eye. MGD is extremely prevalent, but the exact rate of occurrence varies widely because it often goes undiagnosed. MGD has been found to be higher in Asian populations—as high as 60% suffer from dry eye.1 In comparison, predominance of dry eye in whites varies from 3.5% to 19.9%.1
Systemic factors contributing to MGD include hormonal deficiency, menopause, aging, Sjögren’s, psoriasis, rosacea, hypertension and benign prostatic hyperplasia (BPH). Medications interfering with meibomian gland production include anti-androgens, BPH medications, post-menopausal therapy, antihistamines, antidepressants and retinoids.1
Anatomy, Physiology and Pathology of MGD
Meibomian glands are large sebaceous glands located in the upper and lower tarsal plates. The majority reside in the upper lids. Once the lipids and proteins are made from these glands, they are secreted into the tear film, thus preventing evaporation.
Unlike most sebaceous glands, meibomian glands do not have contact with the hair follicle. These glands are densely innervated and controlled by androgens, estrogens, progestins, retinoic acid, growth factors and possibly neurotransmitters. The process by which they produce polar and non-polar lipids is not completely understood. What we do understand is that the mechanism of action is a holocrine process. A muscular contraction occurs during lid movement, which delivers the meibum to the ocular surface.3

Fluorescein staining due to dry eyes prior to a contact lens fit. (Photo: Keshia S. Elder, O.D., M.S.)
MGD is primarily caused by a chronic duct obstruction with thickening meibum. The epithelium of the duct then begins to hyperkeratinize, which leads to dysfunction. The blockage of the gland is altered by several endogenous and exogenous factors, such as age, sex, hormonal changes and topical medications. The gland interference may lead to telangiectasia, gland drop out, meibocyte atrophy and low meibum secretion.1
Diagnosis of MGD
Diagnostic and treatment modalities for DES are becoming more sophisticated. Many times clinicians can make a diagnosis based on the patient’s symptoms alone. This can be difficult because often the symptoms do not match the clinical appearance.
The patient complains of burning, irritated eyes that seem worse in the morning, at the end of the day or after long hours of computer use. He or she may also complain of fluctuating vision upon blinking.
MGD is separated into two categories based on meibum secretion: low-delivery and high-delivery states. Low-delivery states are further divided into hyposecretory and obstructive subcategories. Hyposecretory occurs when the glands produce less amounts of meibum, but are not fully obstructed. Obstructive MGD refers to terminal duct obstruction, where no meibum is produced. High-delivery or hypersecretory MGD is characterized by large amounts of lipid release which can be visible on gland expression upon examination.
Multiple tests can be performed to assess the patient’s dry eye and the presence of MGD:
• Lid exam. First, lid examination may show significant blepharitis with inspissation in meibomian glands, and neovascularization of the lid margin may be present depending on the severity of the condition.
• Corneal staining. A second important observation in the evaluation of DES is the presence of corneal staining. Corneal staining with instillation of fluorescein indicates tissue damage to the cornea and dryness. According to Eric Donnenfeld, M.D., the use of these dyes can be quite beneficial to the practice. The dyes are effective because they stain damaged epithelial cells where there is a loss of mucin in the tear film.9
• Tear evaluation. Lastly, we can evaluate the amount of tears via the tear film break-up time, Schirmer’s test and corneal topography. For these cases, we can now use the TearLab osmometer (TearLab Corporation) to evaluate tear osmolarity. A recent study by Dr. Donnenfeld and colleagues reiterated the importance of using tear osmolarity testing on contact lens and refractive surgery patients. This is especially important because DES can affect surgical outcomes or pose a problem for contact lens wear.5 Topography is also useful in determining the severity of dryness by evaluating the regularity of the axial maps, as well as the placido rings, especially in pre- and post-refractive surgery cases.9
Treatment
Treatment plans are formulated depending on the quality and quantity of tears, symptoms and the presentation of the cornea. Most clinicians delegate treatment according to the severity of the case. Treatment for mild to moderate blepharitis and MGD consists of better lid hygiene and digital massaging of the lids. In severe cases, oral antibiotics should be considered and it’s important to treat the underlying pathology. Topical medications, such as antibiotic and/or combination steroid ointments, qd to b.i.d. for up to two weeks, and oral doxycycline (20mg to 50mg/day) can help improve tear film quality.9
In-office expression of the meibomian glands also provides relief for the patient. Topical antisthetic is applied to the lid margin and the eye care provider manipulates the lid with two cotton-tipped applicators—one on either side of the lid. Alternatively, a Mastrota paddle (Ocusoft) can be used. The paddle is a smooth-edged titanium paddle designed to gently express the meibum from the glands. The paddle is placed behind the tarsal plate and digital pressure is applied. This is a less expensive and less irritating option for the patient.10
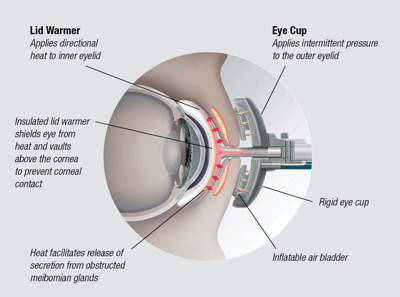
Diagram of the LipiFlow thermal pulsation system.
The FDA approved the second edition LipiFlow (TearScience) pulsation treatment in March 2012. With this system, the practitioner applies a sterile single-use combined lid warmer and eye cup to the patient’s lids. The machine generates heat and pulsation to the area. The procedure lasts for approximately 12 minutes.
Insurance currently does not cover the procedure. The machine itself can cost more than $90,000. Some centers charge around $1,500 for the treatment. Studies show that patients do well with one treatment a year and report a significant increase in patient comfort and less symptoms, particularly in comparison to the alternative of meibomian gland probing.
Information on prevalence, risk factors and how MGD affects the ocular surface is only just beginning to emerge. More than a decade ago the mechanism and etiology of this dry eye syndrome was unknown. Today there is a plethora of information regarding dry eye, easily accessible to the general public. Keep in mind that in addition to the millions of Americans who suffer from dry eye disease, an estimated 39 million have not yet been diagnosed.3 It is only a matter of time now before we solve the remaining mysteries of MGD.
1. Nichols KK. The international workshop on meibomian gland dysfunction: introduction. Invest Opthalmology Vis Sci. 2011 Mar 30;52(4):1917-21.
2. Knop E, Knop N, Millar T, et al. The international workshop on meibomian gland dysfunction: report of the subcommittee on anatomy, physiology, and pathophysiology of the meibomian gland. Invest Ophthalmol Vis Sci. 2011 Mar 30;52(4);1938-78.
3. McDonald MO. The importance of improving the ocular surface on surgical outcomes. Novel Therapeutic Regimens in Treating Ocular Surface Disease and Blepharitis. EyeWorld. 2008 Sep;(Suppl):6-7.
4. Narayanan S. Osmolarity: a diagnostic test for dry eye. Rev Optom. 2011 Jan;148(1):69-73.
5. Donnenfeld E. Goundbreaking osmolarity prevalence study. Presented at the annual meeting of the American Society of Cataract and Refractive Surgery, April 23, 2012; Chicago.
6. Kaiser P, et al. Blepharitis. In: The Will’s Eye Manual, 2nd ed. Philadelphia: Lippincott, Williams & Wilkins; 2004:58-9.
7. McCulley JP, Shine WE. Changing concepts in the diagnosis and management of blepharitis. Cornea. 2000 Sep;19(5):650-8.
8. Shimazaki J, Sakata M, Tsubota K. Ocular surface changes and discomfort in patients with meibomian gland dysfunction. Arch Ophthalmol. 1995 Oct;113(10):1266-70.
9. Caceres V. Dry eye step-by-step: how to diagnose and treat dry eye. Eye World News. 2006 Sep. Available at:
www.eyeworld.org/article.php?sid=3381 (accessed May 2012).
10. McCulley JP. A combination therapy for blepharitis and meibomianitis. Ophthalmol Manage. 2006 Sep. Available at: www.ophmanagement.com (accessed May 2012).
Dr. Knouff, is board certified by the American Board of Optometry, and is residency trained in ocular disease. She has no financial disclosures. She currently practices at Omni Eye Services in Atlanta.


