ODs Rally for FTC Contact Lens Rule Workshop
More than a year after proposing changes to the Contact Lens Rule, the Federal Trade Commission (FTC) is answering pushback from the American Optometric Association (AOA), lawmakers, practitioners and other advocates with a public Contact Lens Rule Workshop on March 7 in Washington, DC. The gathering, designed to discuss contact lens marketplace competition, consumer access, prescription release and portability, and other contact lens-related subjects, will feature panelists, public comments and feedback.
A persistent advocate for contact lens patient health and safety, the AOA says it will be an active participant in the upcoming workshop.
“During the past year, the AOA and our supporters have underscored that our regulatory agencies should take a closer look at those online contact lens retailers who are breaking the current laws instead of supporting more unnecessary bureaucracy,” says Christopher J. Quinn, OD, AOA president. “AOA will carry this message forward and has been working quickly to prepare for this workshop.”
Among the proposed changes is a mandate that eye care practitioners maintain a signed agreement of prescription dispensation for contact lens patients for three years.
“I can’t help but feel the FTC proposed paperwork mandate is somehow a diversionary tactic supported by companies like 1800-Contacts, designed to keep organized optometry away from working on the real issue of protecting patients from unscrupulous business tactics,” says Justin Bazan, OD, of Park Slope Eye. “I understand the FTC is focused on ensuring a competitive marketplace, but it cannot be done without also safeguarding the eyes of our patients.”
The change would drive a wedge in the doctor-patient relationship and have a huge impact on the bottom line. The FTC estimates it would cost the industry roughly $10.5 million, while the AOA cites a study that suggests an unacceptable burden for ODs, with potential costs to a one-doctor, one-support staff practice as high as $18,795 in the initial year, if finalized.
To rally the profession, the AOA has issued a call to action to ensure at least one OD from each state attends the meeting to create a united front, according to Dr. Quinn.
“One thing that is critical is that we mobilize to ensure that the optometric profession’s full perspective and range of expertise is included in every aspect of the discussion,” Dr. Quinn says. “Those who want to undermine optometry and patient care will be there in force, and optometry needs to have a stronger presence.”
“There will be strict limits on participation, and not every doctor will gain recognition during the limited times for open discussion,” Dr. Quinn adds. “But an engaged, nationally representative group of doctors on hand will deliver a powerful message to the FTC.”
“This workshop absolutely requires a strong showing from organized optometry,” says Dr. Bazan. “As an optometrist, I feel it’s a duty to my profession to, at a minimum, let the FTC know how I feel.”
Depression and Anxiety Show Dry Eye Correlation
A recent study found a correlation between dry eye and non-ocular comorbidities such as anxiety and depression.1 This suggests that, for some patients, dry eye symptoms may stem from a condition unrelated to ocular surface health. For practitioners, this could explain why some dry eye cases do not respond to topical dry eye treatment.
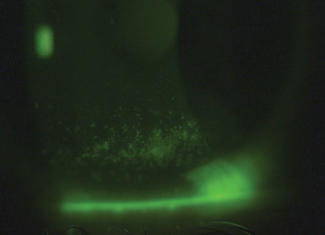 |
| Depression and anxiety may be associated with dry eye, similar to other systemic conditions like Sjögren’s. Photo: Chandra Mickles, OD |
“It’s a great point to note that ocular pain and depression/anxiety are correlated with non-ocular pain,” says Bill Potter, OD, chief of Optometry and Contact Lens Services at Millennium Eye Care in West Freehold, NJ. “Perceptions of pain and associated mental health issues vary tremendously by age, culture, sex and more. Some of it is due to induced biochemical changes and some is due to the way that we are hard-wired.”
Researchers used the Pearson correlation coefficient to evaluate the association of dry eye symptoms and neuropathic-like ocular pain features, chronic pain conditions, depression and anxiety in 233 patients.
Coming into the study, about 40% of patients had mild or greater dry eye symptoms and 12% had severe symptoms per the Dry Eye Questionnaire. The patient population was predominantly female to counterbalance a previous study that looked at a mostly male population. However, results were consistent between both studies, showing notable correlation between dry eye symptoms and neuropathic-like ocular pain (burning and sensitivity to wind, light and temperature), non-ocular pain conditions (arthritic pain, back pain and headaches), depression and anxiety. According to the study, the results indicate “the link between dry eye symptoms and pain elsewhere in the body is robust,” and suggest that “optometrists need to redefine dry eye and separate those who have ocular surface dryness from those whose dry eye symptoms are driven by somatosensory dysfunction such as neuropathy.”
“Dry eye with systemic comorbidity is a classic example of how we need an integrated approach, mental health and systemic pain control included,” says Dr. Potter. “Although there is a trend toward optometrists doing more traditional primary medical care, we can’t do it all. Teamwork with other specialists is key.”
While dry eye therapies target tear function, inflammation and ocular surface anatomy, patients with both dry eye symptoms and non-ocular pain conditions may benefit more from treatments that focus on reducing the excitability of somatosensory function, the study says.
For future studies, Dr. Potter suggests identifying psychological or systemic pathophysiologic profiles that would indicate patients at greater risk for progression.
1. Chang VS, Rose TP, Karp CL, et al. Neuropathic-like ocular pain and nonocular comorbidities correlate with dry eye symptoms.Eye & Contact Lens. December 7, 2017. [Epub ahead of print].
| In Brief Rosen R. Amniotic membrane grafts to reduce pterygium recurrence. Cornea. 2018;37(2):189-93. • A new meta-analysis reveals that standard corneal collagen crosslinking (epithelium-off CXL) was more effective in decreasing the maximum keratometry than transepithelial CXL in patients with keratoconus. The researchers evaluated three studies with a total of 244 eyes—111 in the standard CXL group and 133 in the transepithelial CXL group. They found a mean keratometry difference of 1.05D at least 12 months post-procedure, in favor of standard CXL. At the same time, transepithelial CXL provided slightly better corrected distance visual acuity. Both had similar safety. Li W, Wang B. Efficacy and safety of transepithelial corneal collagen crosslinking surgery versus standard corneal collagen crosslinking surgery for keratoconus: a meta-analysis of randomized controlled trials. BMC Ophthalmol. December 28, 2017. [Epub]. • Italian researchers recently discovered obstructive sleep apnea (OSA) was 10 to 20 times more prevalent in study patients with keratoconus compared with the rate found within the general population. After studying 50 patients diagnosed with keratoconus using home overnight polysomnography, they found 38% had OSA—a mild form in roughly half of study participants. They did not find any statistically significant differences in corneal parameters or keratoconus severity between patients with and without OSA and patients with different degrees of OSA severity. Pedrotti E, Demasi CL, Fasolo. Obstructive sleep apnea assessed by overnight polysomnography in patients with keratoconus. Cornea. January 9, 2018. [Epub ahead of print]. |


