 The cornea’s many defense mechanisms and regenerative capabilities make it one of the eye’s most resilient structures. So it’s all the more distressing when patients present with a chronic, non-healing corneal defect due to trauma, infection or a degenerative process.
The cornea’s many defense mechanisms and regenerative capabilities make it one of the eye’s most resilient structures. So it’s all the more distressing when patients present with a chronic, non-healing corneal defect due to trauma, infection or a degenerative process.
The January column discussed diagnostic techniques and medical therapies suitable for such cases. Now, let’s consider a few interventional therapies to manage non-healing defects.
Bandage Contact Lenses
The first and certainly most common option is the bandage contact lens. Reviewing the original work by Donnenfeld (which showed equal healing efficacy for patching vs. bandage lenses) reveals that bandage lens use has increased dramatically in a variety of settings, and has become the norm for many.1
A few aspects of bandage contact lenses are worthy of comment. Of particular note: most clinicians do not use these lenses for a prolonged period of time, tending to treat the eye only until the process has concluded and then removing the lens in the immediate post-closure phase.
This may inadvertently limit the benefit of the intervention—keeping the lens in place for an extended period of time after the wound is healed can be very helpful in mediating against recrudescence in patients with persistent defects.
Depending on etiology, most patients are maintained on non-preserved agents (e.g., topical cyclosporine, NPATs, bland unguents), low-dose oral doxycycline and a low-dose antibiotic. The lens is maintained anywhere from two to six weeks or longer, based on lesion severity and clinical presentation.
Another unusual aspect of bandage contact lens therapy is that, in some patients, it simply does not work. The patient may report increased comfort, but the wound does not show any significant gain. In these patients, I recommend the use of a tight pressure patch; the contact of the mucous membrane to the wound will typically accelerate wound healing if there is no sign of active infection. An antibiotic ointment is placed beneath the patch for coverage in the treatment period. The patient should be seen either daily or on alternating days to remove and re-patch if needed.
This technique is an important adjunct to epithelial wound management. It offers clinicians an excellent additional treatment option when bandage contact lenses fail, or if for some reason the bandage contact lens is not a good option.
Amniotic Membrane
While use of an amniotic membrane is relatively new in its current format, it has been available for some time in surgical applications. Because the tissue comes from fetal amnion, it is a remarkable nutritional supplement that can promote healing in corneal wounds of all types. Also, it can be used across the entire spectrum of causative disease states, including herpes, microbial keratitis, severe Sjögren’s syndrome, neurotrophic cornea and others.
The first applications required that the membrane be sutured into position on the bulbar conjunctiva to maintain its position on the corneal surface. This procedure was used infrequently, and was obviously limited by the surgical intervention and tissue placement stability.
 | |
|
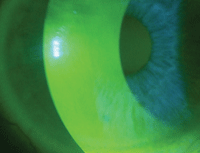
Fig. 1. ProKera, post-treatment day 3. Photo: Mile Brujic, OD
|
Two products provide fetal amniotic tissue in an easy-to-apply design that does not require suturing: ProKera (Bio-Tissue) and Ambio (IOP Ophthalmics). The former uses a symblepharon ring with amnion stretched over the device. The latter consists of an amnion patch with a large contact lens placed over it to maintain its position.
Due to recent advances in application, amniotic membrane is relatively simple to offer in clinical practice and can be done without OR access. Because ProKera is maintained with an anti-infective cocktail, it must be prepped for eye placement by thoroughly rinsing the material and ring with sterile saline; the lens can then be inserted and evaluated at the slit-lamp to check for centration. If the lens decenters, reposition it with blunt forceps.
To achieve comfortable placement of the ring, tape the lid closed temporally to decrease movement and blink (which causes discomfort). This should be done by placing the tape on the temporal half of the lid and maintaining a small opening nasally such that any necessary topical therapy can be applied to the ocular surface through the opening. This will include antibiotics, antivirals and immunomodulators.
The best way to immobilize the lid is to use Tegaderm tape (3M), which provides an easy remedy to the lid positioning issues and will provide comfort for the patient while allowing instillation of medical therapy.
The Ambio membrane is different than the ProKera in its primary presentation and need for hydration. Once this is accomplished, Ambio is applied to the eye and a contact lens larger than the corneal diameter is placed over the membrane.
Most patients can expect improvement in approximately three to five days, and the lid can be opened on subsequent follow-up visits. The clinician can observe the status of the cornea during treatment by simply removing the Tegaderm and then replacing it at the end of the examination.
Tarsorrhaphy
The next level of treatment, which goes beyond topical interventional methods, is surgical in nature. Tarsorrhaphy is the primary procedure performed when presented with a non-healing corneal insult.
The procedure is typically successful because it decreases surface area and evaporative loss of tears. This accomplishes two things: it increases tear volume and provides a mucous membrane tissue—much like patching—to contribute nutrition to the epithelial wound modulation.
Temporary tarsorrhaphy, a more recent development, can be performed in-office without suturing. This is an excellent way to produce lid closure and decrease surface evaporative problems. This technique simultaneously allows a reversible outcome and the opportunity to heal the eye without permanent lid cicatrization. It is accomplished by using cyanoacrylate glue, typically obtained from a dental surgical supply house. It comes in single-unit sterile applicators.
To perform the procedure, hold the lids closed while gently applying an extremely small amount of glue to the lashes of both lids, not lid margin. Once the glue is in place, maintain closure for approximately 30 seconds. After the final application of materials, the lashes will be temporarily glued together, providing a nonsurgical tarsorrhaphy.
This technique can be used in all categories of epithelial defects discussed in the January column. It is most effective in cases of neurotrophia and corneal melt secondary to autoimmune disease and herpetic corneal wounds.
If nonsurgical tarsorrhaphy is successful, and there is a need for a more permanent closure, the standard surgical tarsorrhaphy can provide permanent closure of the lid margins to maintain the function of the globe.
This is usually done in such a fashion that the visual axis is supported with a palpebral opening, and either the pupil margin or the mid-iris is the point at which the lid closure is completed. The glue spontaneously extrudes or breaks at approximately seven to 14 days. This allows for either re-application if necessary, or the discontinuation of treatment, which makes it ideal for patients with temporary or transient epithelial wound defect problems.
If the patient does not respond well or if the clinician elects to terminate therapy, simply cut the lashes at the base posterior to the glue position and the lid can easily be opened.
Conjunctival Flap Surgery
This is reserved for patients who have been managed through all the levels already discussed yet continue to fail, with loss of the globe as possible outcome. These are patients in which penetrating keratoplasty is not an option. In cases such as this, a conjunctival flap is created with a limbal-based hinge and simply draped over the cornea and then sutured into position.
As this technique will obviously compromise visual performance, it should only be used as an end-stage treatment to salvage the globe. This is a rarely used but extremely effective technique for managing non-responsive epithelial defects. In particular, patients presenting with defects secondary to chemical burns with melting, who are incapable of grafts or do not wish to undergo surgical procedure due to age or infirmity, will benefit from this procedure. But, be aware that conjunctival flaps often will erode or retract.
The challenges we face in hastening epithelial wound healing may seem daunting, but if one implements a structured approach to both diagnosis and intervention, success will typically follow.
1. Donnenfeld ED, Selkin BA, Perry HD, et al. Controlled evaluation of a bandage contact lens and a topical nonsteroidal anti-inflammatory drug in treating traumatic corneal abrasions. Ophthalmology. 1995 Jun;102(6):979-84.


