 Picture driving down the freeway in your Mercedes Benz S-600 after a long day of treating patients.1 You didn’t get enough sleep last night and you feel fatigue start to set in. Your eyes water, you blink faster, your head starts to nod… Beep, beep, beep! A set of alarms start ringing and you’re jolted back to reality—you almost fell asleep at the wheel. Now, how did your car know this?
Picture driving down the freeway in your Mercedes Benz S-600 after a long day of treating patients.1 You didn’t get enough sleep last night and you feel fatigue start to set in. Your eyes water, you blink faster, your head starts to nod… Beep, beep, beep! A set of alarms start ringing and you’re jolted back to reality—you almost fell asleep at the wheel. Now, how did your car know this?
The answer is simple: blinks. Blinks have been shown to be a measure of fatigue, and Mercedes Benz has rightly seized on the importance of blinks by developing an attention assist driver drowsiness monitor to keep drivers from engaging in “microsleep,” a spontaneous reaction to fatigue in which our body gives us physical signs, including either an increase or decrease in blink rate, to stop what we are doing and sleep.2,3 The system is a novel safety tool as it utilizes parameters such as blink duration, delay of lid reopening and interblink interval (IBI) in order to monitor drivers’ sleepiness.4
While the eye has been studied extensively, the blink itself tends to be overlooked even though we are unintentionally observing blinks constantly throughout the day. Mercedes Benz, a company that is far and beyond the realm of ophthalmology, has realized the significance in analyzing blinks more carefully, yet eye care practitioners have yet to place the same importance on the study of blinks. A thorough understanding of the latest technologies and research concerning blinks will help eye care practitioners to better identify corneal surface problems such as dry-eye disease and meibomian gland dysfunction (MGD).
In the optometrist’s armamentarium, blink patterns are the arrows in the quiver that target the proper identification of a patient’s ocular health. The blink itself is the eye’s first and foremost defense against ocular grievances like dust and pollen. The blink muscles produce a “lid wiper” action that protects against these insults; that action itself also stimulates mucin secretions that lubricate the ocular surface.5 Though quite inconspicuous and involuntary, observing blinks can serve as an important diagnostic tool for a multitude of ocular surface conditions.
The Blink as a Therapeutic Assessment
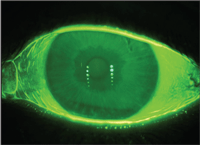
Tear film stability and corneal health are measured using fluorescein staining.
A greater understanding of blink patterns can aid in identifying patient populations and help an optometrist to better understand the full capacity of their patient’s ocular problems. For instance, patients with dry eye usually have blink patterns that exhibit variable patterns, i.e. their rates may switch between periods of rapid blinking to periods where their blink rates slow. Though these patterns change, their tear film stability usually remains the same; therefore, identifying these changing blink patterns is the key in determining the extent of their dry eye.
A recent study showed differentiation between normal and dry eye patients by utilizing various blink pattern diagnostic tools and demonstrated that dry eye subjects had twice the IBI of normals.6 Further, various types of blinks were categorized into five types: ¼ blink, ½ blink, ¾ blink, full blink and extended full blink. The two populations were significantly different in the occurrence of extended full blinks—occurring 1% and 4% of the time in dry eye and non-dry eye subjects, respectively.6
In the MGD arena, blink diagnostics also can serve as an important indicator. When a patient has a lower blink rate, they do not blink as frequently. Therefore, the distribution of secretions produced by the meibomian glands is fewer, which can impact the corneal surface. In one study, researchers observed blink patterns and rates and used these observations to split 14 subjects into two groups: normals and patients with MGD.7 The results showed that for MGD subjects, the proportion of full blinks was significantly greater than the normals. Hence, MGD patients may change their own blink patterns to incorporate more complete blinks and squeeze blinks to compensate for a lack of meibum secretions.7 This finding was determined after splitting up the two groups based on observing blinks, indicating that blinks are a vitally important diagnostic tool.
A Tool to Analyze Visual Function
In addition, optometrists should be acutely aware of a patient’s blink patterns. A long interblink interval may not only cause ocular discomfort, but also indicate problems with a patient’s visual acuity. There have been attempts over the years to accurately assess visual acuity, yet a validated test developed by Ora, which also utilizes blinks, provides a necessary measurement of visual function shown in real time.8
Known as the IVAD, this computer-based system presents the optotype Landolt C at the patient’s best-corrected visual acuity; visual acuity decay results are measured in milliseconds. To achieve accurate visual acuity information from a patient, this measurement is key. In a study using IVAD measurements to assess visual acuity, researchers demonstrated that patients with central corneal staining did not maintain their best-corrected acuity between blinks as long as patients who did not show corneal staining.9
Although blinking is a physical aspect that can easily be overlooked, it is important to keep in mind the wealth of opportunities that observing blinks can offer—from diagnosing a patient with dry eye to making sure a patient doesn’t fall asleep at the wheel. The observation of blinking behavior is a useful instrument for patient characterization and should be valued as highly as any other measure behind the optometrist’s slit lamp.
1. Mercedes Benz. S-Class Sedan. Available at:
www.mbusa.com/mercedes/vehicles/class/class-S (accessed August 2011).
2. Stern JA, Boyer D, Schroeder D. Blink rate: a possible measure of fatigue. Hum Factors. 1994 Jun;36(2):285-97.
3. Schleicher R, Galley N, Briest S, Galley L. Blinks and saccades as indicators of fatigue in sleepiness warnings: looking tired? Ergonomics. 2008 Jul;51(7):982-1010.
4. Umbehr J. Mercedes develops anti-microsleep system. MedGadget. 2006 Nov. Available at:
www.medgadget.com/2006/11/mercedes_develo_1.html (accessed August 2011).
5. Ousler GW 3rd, Hagberg KW, Schindelar M, et al. The Ocular Protection Index. Cornea. 2008 Jun;27(5):509-13.
6. White R, Rodriguez J, Lane KJ, et al. Blink patterns in normals and dry eye subjects; beyond blink rate. Invest Ophthalmol Vis Sci. 2010;51:E-abstract 3366.
7. Welch D, Contractor M, Abelson MB, et al. A single-center pilot study evaluating eyelid functionality and signs associated with dry eye in subjects suffering from Meibomian Gland Dysfunction and non-MGD subjects using the OPI 2.0 system. Invest Ophthalmol Vis Sci. 2011;52:ARVO E-Abstract 946.
8. Walker PM, Ousler III G, Workman A, et al. Visual function in normals compared to patients diagnosed with dry eye as measured by the inter-blink interval visual acuity decay (IVAD) test. Invest Ophthalmol Vis Sci. 2007;48: ARVO E-Abstract 422.
9. Ousler III G, Durham T, Brazzell K, et al. A correlation between central corneal staining and visual function in patients diagnosed with dry eye. Invest Ophthalmol Vis Sci. 2007;48:ARVO E-Abstract 410.


