Perhaps because it’s both commonplace and chronic, dry eye presents a seemingly never-ending series of challenges: the “easy” cases are hard, and the hard cases can be maddening. Some patients who should respond to routine therapy simply don’t, while others have symptoms far out of proportion with their signs and general medical history. And even effective therapies can be stymied by noncompliance.
While much is known about ocular surface disease, it still remains a complex condition with many causes and potential treatment options. Often, the approach to management involves as much art as science. For this reason, we asked several dry eye experts to weigh in on how they would diagnose and treat the following recalcitrant cases.
 |
Case 1:
Long-Suffering Sjögren’s Patient
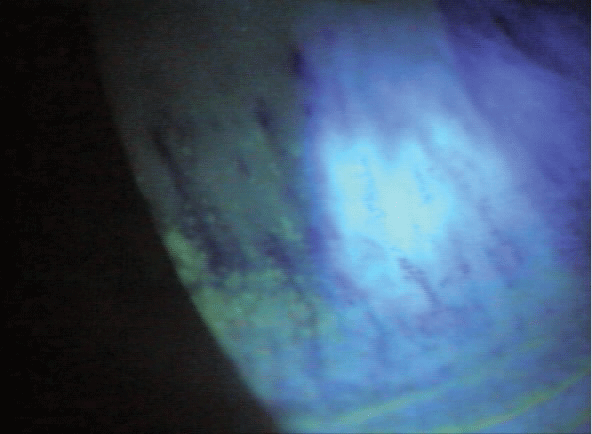
![]() In addition to over-the-counter drops for dry eye, she was currently using a topical fluoroquinolone and a formulated vancomycin drop for a lingering corneal infection, as well as Restasis (Allergan) to increase tear production. However, nothing seemed to be providing relief from severe irritation and photophobia symptoms, which had become debilitating.A 67-year-old female with a five-year history of Sjögren’s syndrome presented complaining of extreme discomfort and light sensitivity. Visits to numerous eye care practitioners, including a cornea specialty group, didn’t provide significant relief.
In addition to over-the-counter drops for dry eye, she was currently using a topical fluoroquinolone and a formulated vancomycin drop for a lingering corneal infection, as well as Restasis (Allergan) to increase tear production. However, nothing seemed to be providing relief from severe irritation and photophobia symptoms, which had become debilitating.A 67-year-old female with a five-year history of Sjögren’s syndrome presented complaining of extreme discomfort and light sensitivity. Visits to numerous eye care practitioners, including a cornea specialty group, didn’t provide significant relief.
Her noninvasive tear film break-up time was three seconds, with significant areas of corneal staining, suggesting tear instability. In addition, meibography revealed significant gland truncation and some gland loss, while diagnostic meibomian gland expression showed nearly all glands blocked, with minimal expression of thick, opaque meibum. The patient’s tear prism was noted as barely present; interferometry confirmed a deficient lipid layer.
A slit-lamp exam revealed a dense band of staining with areas of indolent corneal ulceration and haze across the right cornea below the midline. The left eye had no ulceration but did exhibit dense staining in a similar inferior-midline pattern. Careful examination of lid/globe apposition showed a significant gap on closure, while testing of Bell’s phenomenon showed that it was essentially absent in both eyes.
What’s the best course of treatment for this patient?
Dr. Karpecki: The ocular surface exposure from poor eyelid apposition is perhaps the number one reason the patient is having so many problems, Dr. Karpecki notes. Overnight bland ointments and sleep shields would likely help with the nocturnal lagophthalmos.
To address the existing issues, the first step is to heal the corneal ulcer and protect the ocular surface integrity, Dr. Karpecki says. Given the length of time the patient used vancomycin without improvement, the issue may be toxic keratitis, a Mooren’s ulcer or an ulcer related to a systemic disease such as a peripheral ulcerative keratitis (PUK) from rheumatoid arthritis or another autoimmune condition associated with Sjögren’s syndrome.
Ultimately, determining the degree of pain would help with the diagnosis. “I’d contact her rheumatologist and ensure that the specialist assesses the systemic disease, as a PUK could be a systemic manifestation,” Dr. Karpecki explains.
|
Contributors
Chuck H. Aldridge, OD , is head of Aldridge Eye Institute in North Carolina.
Mile Brujic, OD, practices full-scope optometry with special interest in contact lenses, anterior segment disease management and glaucoma as part of the Premier Vision Group in Ohio.
|
Using an oral secretagogue such as Evoxac (Daiichi Sankyo) 30mg BID to TID for the dry mouth that is likely present could also help the dry eyes, Dr. Karpecki suggests, adding that he would continue with an antibiotic but discontinue the vancomycin due to its potential toxicity and amount of time used.
Next, Dr. Karpecki would address the need for increased lubrication of the ocular surface, then apply an amniotic membrane such as Prokera (Bio-Tissue) if the ulcer or persistent epithelial defect does not respond.
Further testing such as tear osmolarity could be illuminating as well. “I would be at a loss for how to best treat this patient without knowing her osmolarity readings, in addition to symptoms, meibomian gland expression and ocular surface staining,” Dr. Karpecki notes. Meibography and lid closure assessment or blink would also be valuable findings.
Most Sjögren’s patients have osmolarity readings above 330mOsmol/L; a patient on Restasis for a substantial period of time, however, may show significant im--provement, Dr. Karpecki says. “Given her continued symptoms, I’d predict the reading to be around 315 to 320—that is, improved on Restasis—but given the severity of the disease, additional therapies may be required.” Blocked meibomian glands in a Sjögren’s patient indicate concurrent and long-standing disease, which is typical, “but the key is the lack of apposition of the eyelids,” he says. “This finding over time will cause significant obstruction, dysfunction, dropout of the meibomian glands and exposure keratopathy.”
Assuming the osmolarity tests high, Dr. Karpecki suggests changing her artificial tears to a drop more likely to lower osmolarity, such as Blink (Abbott Medical Optics), TheraTears (Advanced Vision Research), FreshKote (Focus Laboratories) or Retaine (Ocusoft). Preservative-free versions should be used if the reading is extremely high (i.e., >330 in at least one eye). If the osmolarity reading were slightly elevated to normal on Restasis (i.e., <315), he would recommend using a lipid-based or lipid-enhanced artificial tear such as Refresh Optive Advanced, Systane Balance, Soothe XP (Bausch + Lomb) or Retaine MGD, and continuing the Restasis.
Additionally, because this level of obstruction and meibomian gland loss requires aggressive therapy, Dr. Karpecki would prescribe 50mg BID doxycycline for one to three months, then taper the doxy and begin a nutritional supplement such as HydroEye (ScienceBased Health) for long-term use.
Dr. Karpecki would also recommend a warm compress (e.g., Bruder Eye Hydrating Compress) and would place the patient on a topical anti-inflammatory/antibiotic for approximately two weeks, preferably a preservative-free option in light of the keratopathy present, and would continue the Restasis BID. If significant improvement is not noted over the next one to three months, an in-office gland expression therapy like LipiFlow could also be considered.
“Once the disease is controlled from all of these steps,” he said, “I’d have her continue the Restasis, HydroEye, the appropriate artificial tear and the Bruder Eye Hydrating Compress long-term, in addition to good systemic control of the autoimmune disease.”
Dr. Hauswirth: While agreeing with Dr. Karpecki’s initiative to tackle the corneal ulcer first, Dr. Hauswirth suggests starting treatment of the meibomian gland problem with LipiFlow or manual therapeutic gland expression in addition to oral doxycycline.
“As this is a Sjögren’s patient, we would expect that her lacrimal function is decreased, but any amount of aqueous tear production she has would be better served with improved meibomian function and a thicker meibum layer,” he explains.
In addition, he suggests adding autologous serum drops to allow growth factors and other beneficial proteins for the epithelium, and anti-inflammatories. Punctal occlusion once the inflammatory markers are reduced would also be beneficial.
Dr. Aldridge: “If this is a true infection and not a sterile ulcer,” Dr. Aldridge cautions, “Restasis is contraindicated and needs to be stopped until the infection is cleared.”
The patient is also likely suffering from aqueous deficiency—common in those with Sjögren’s—and evaporative deficiency as evidenced in the meibomian glands. In addition, “to complicate it more, there seems to be an exposure keratitis being created from the lack of lid closure,” Dr. Aldridge added.
The antibiotics unfortunately must be continued despite appearing abrasive on the ocular surface. Dr. Aldridge would consider adding an antibiotic ointment to help with lubrication. Once the infection clears, punctal plugs to increase tear volume could be inserted. The patient should then resume using Restasis.
After a few weeks, Dr. Aldridge would monitor corneal staining during a follow-up examination. If signs and symptoms don’t improve, he’d consider fitting a mini-scleral contact lens to put a reservoir of fluid against the corneal surface for most of the waking hours.
Dr. Tseng: In contrast with the others, Dr. Tseng suggests addressing the corneal infection using punctal occlusion with cautery if there is no reflex tearing. Following the procedure, He’d use a corneal bandage such as Prokera Slim to help the corneal epithelium heal. Autologous serum drops can be used later to maintain ocular surface health.
Regarding the meibomian gland dysfunction, Dr. Tseng suggests looking into alternate causes, such as Demodex infestation. If epilated eyelashes and cylindrical dandruff are noted, he says, the problem can be treated using a preservative-free facial cleanser like Cliradex (Bio-Tissue).
Dr. Epstein: Dr. Epstein, who submitted this case, prescribed doxycycline 50mg BID and recommended the patient begin using HydroEye, a nutritional supplement. He initially treated the exposure using a bland ointment at nighttime before switching to the EyeEco Quartz silicon sleep shield. The patient’s use of topical vancomycin was discontinued and the generic fluoroquinolone was switched to Vigamox (Alcon) for 10 days to minimize toxicity, then suspended after resolution of the ulceration was noted. Use of Restasis was continued and the patient was told to keep well hydrated.
The patient’s discomfort and photophobia improved only slightly following adoption of this regimen, so bandage lenses were fitted successfully with excellent results following discussion of risks and benefits.
The patient currently uses warm moist heat goggles (Tranquileyes by EyeEco) nightly, and meibomian gland expression using the LipiFlow system is planned for the future. The patient continues to do well on the current regimen.
 |
Case 2:
Alternatives for Noncompliance
A
66-year-old diabetic male presented with a diagnosis of dry eye. He was being treated with Systane Ultra, which he reported using “about once a day.” His dry eye severity was tested with InflammaDry (RPS), an in-office inflammatory marker test, resulting in a “strong positive” reading. The patient admitted he had problems with compliance and remembering to “use the drops.” Prescription options were discussed and the patient expressed an interest in using nonprescription options, if possible.
How would you treat this patient?
Dr. Schaeffer: The first step is to perform a complete ocular surface evaluation, says Dr. Schaeffer. Depending on slit-lamp findings and dry eye severity, treatment options include medications such as Lotemax (Bausch + Lomb) gel BID; Restasis BID or TID; lipid-based artificial tears such as Systane Balance, ointment or gels QHS; Lacrisert; meibomian gland treatment options such as expression, hot compresses, doxycycline, antibiotic/steroid drops or LipiFlow; punctal plugs and omega-3 supplementation.
Dr. Karpecki: Consider additional testing—e.g., osmolarity, meibomian gland expression (and meibography, if available), and, fluorescein dye—to quickly gauge the staining, tear meniscus height, clearance and tear film breakup time, suggests Dr. Karpecki. “Without those tests, it is difficult to determine the most appropriate treatment especially given the fact that the patient expressed an interest in non-prescription products,” he explained.
If osmolarity was found to be elevated (i.e. above 320mOsmol/L), artificial tears like TheraTears, Blink, Retaine and FreshKote have a greater propensity to lower osmolarity are more likely to achieve quicker results, he says. “My assumption, given the specifics of this case, is this patient’s osmolarity was below 320 and the meibomian glands did not show significant disease,” Dr. Karpecki says. “In that case, a tear like Systane Ultra would work well.”
Due to the level of inflammation noted, treatment options include ocular nutrition, oral doxycycline, Restasis and corticosteroids. “Given the patient’s desire to start with nonprescription options,” he says, “I agree with the nutritional treatment approach. One could then step up therapy if resolution was not achieved.”
Finally, the patient’s diabetes should be monitored, as dry eye can also be a manifestation of poorly controlled disease. For this, a letter to the endocrinologist or PCP would be prudent, he says.
Dr. Hauswirth: Because “compliance and cost are both issues that become more challenging in less symptomatic patients,” Dr. Hauswirth would first attempt to address compliance through patient counseling, focusing on the patient’s risk of progression in the presence of diabetes and a positive MMP-9 marker. “He needs to know that artificial tears in this case is not the same thing as treating it medically.”
Dr. Hauswirth advises using Lotemax gel TID for one month to address the ocular inflammation, as well as Restasis BID. “This patient may well have reduced corneal sensation due to partial neurotrophia. The improvement in the ocular surface and InflammaDry markers may be initially offset by the patient ‘noticing’ his eyes more, which is a good sign—it means we may be regenerating some of the corneal nerves,” he says. In any case, however, “his age, systemic condition and high risk of progression will make this a longer treatment regimen.”
Dr. Brujic: As the doctor who treated this patient, Dr. Brujic prescribed Systane Ultra TID, EZ tears (EyePromise, ZeaVision), a nutrition supplement containing omegas 3 and 6, vitamins A, D3 and E, and other components to enhance the tear film.
During a three-month follow up, the patient reported poor compliance with artificial tears but good compliance with ocular nutrition. InflammaDry testing showed a “weak positive” result, suggesting decreased inflammation. Ocular surface findings improved with minimal staining and an improved TBUT. Dr. Brujic continues to treat the patient with ocular nutrition and Systane Ultra.
 |
| Photo: Dr. John P. Herman, OD |
Case 3:
The Great Masquerader
A 78-year-old female presented complaining of significant ocular irritation, redness of the conjunctiva and epiphora in both eyes. She reported her last eye care provider diagnosed her with an aqueous deficient dry eye with a secondary reflex tearing. She was placed on a regimen of artificial tears and Restasis 0.05% BID, warm compresses and lid hygiene without improvement. Her conjunctiva was significant for redundant folds inferiorly.
Dr. Tseng: “The clinical history of this case suggests the patient has both aqueous-deficient dry eye and conjunctivochalasis, while being refractory to conventional medical treatment,” Dr. Tseng says.
Because conjunctivochalasis is a mechanical problem that eliminates the tear meniscus and the tear reservoir in the fornix, one possible solution could be to repair both using cryopreserved amniotic membrane in a surgery known as the reservoir restoration procedure. Following the procedure, if symptoms persist, Dr. Tseng suggests punctal occlusion.
Dr. Hauswirth: Application of a corticosteroid such as Lotemax gel BID or compounded Pred-Healon (prednisolone sulfate 0.25% in hyaluronic acid) two-to-three-times daily over a month’s time may alleviate some inflammation and other symptoms that result from conjunctivochalasis, Dr. Hauswirth says. Topical antihistamines or NSAIDs may also be used, but he cautions they are not as dependable in this scenario.
In the longer term, Dr. Hauswirth recommends oil-based non-preserved artificial tears, such as Refresh Optive Advanced, in combination with Restasis. “Appropriate education is critical in this scenario for the patient to understand that anti-inflammatories may only help a small amount as far as symptoms go, but may slow down the progression of the disorder,” he says.
To ultimately correct the pathology in highly symptomatic patients, however, Dr. Hauswirth advocates a surgical consultation with excision of redundant conjunctiva, which he says has been shown to help reduce inflammatory markers and restore a more normal tear reservoir.
Dr. Schaeffer: “Conjunctivo-chalasis is a very undiagnosed condition that leads to many ocular complications,” says Dr. Schaeffer. If the folds are blocking the puncta or the meibomian glands, or just irritating the eye, he agrees surgical correction will be needed. In this case, the conjunctiva folds are most likely causing the epiphora.
Because this patient also has issues with her canalicular system, Dr. Schaeffer suggests a lacrimal system irrigation to open or measure the patency of the tear drainage duct. He also would consider other options to improve tear volume.
Dr. Brujic: Unlike the others, Dr. Brujic believes surgery isn’t re-quired, despite the con-junctivo-chalasis. He suggests maintaining the Restasis BID and adding heat therapy (e.g., a Bruder Mask) in the evening to increase compliance. “Often, people just apply a warm washcloth to the eyes for a few minutes, which is in-adequate in my experience,” he says.
Also determine if the patient’s current artificial tears are suitable for her type of dry eye. For example, if she is using a store brand such as Visine, Dr. Brujic would discontinue it and instead prescribe one that is more appropriate to her condition.
He would also order further testing, specifically InflammaDry on each eye to determine if the MMP-9 levels are greater than 40ng/mL, and ask about any nutritional supplements she may be taking.
“Assuming she is not taking anything, I would start her on an appropriate ocular nutrient that would support improvement in tear film function, such as EZ tears by ZeaVision,” Dr. Brujic says.
Finally, Dr. Brujic would test her four-to-six weeks later with InflammaDry. Depending whether improvement is noted, he would either keep her on the prescribed regimen or add a topical steroid such as loteprednol gel QID for a month. He would then ask to see the patient again for further evaluation.
Dr. Shovlin: “Conjunctivo-chalasis should be distinguished from aqueous-deficient dry eye and recognized as a significant masquerader for dry eye, as they often have similar symptoms and signs,” explains Dr. Shovlin, who submitted this case. When the conjunctiva is loose enough, it can occlude the puncta and cause epiphora. Such a condition can result in mechanical irritation and conjunctival redness that affects many patients, especially those of the older population when the conjunctiva loses its firm attachment to Tenon’s membrane.
Dr. Shovlin treated the patient using Prolensa HS, a topical NSAID. However, he cautioned, some patients will need conjunctival resection and, if large areas are excised, an amniotic membrane graft may even be needed.


