Today’s contact lens practitioner has an increasing number of astigmatic options in the toolbox. Yet, it can be difficult to decide whether to pick the gas-permeable (GP) or the soft lens option. In many situations, this is a case-by-case decision. This article offers eight representative cases—some with two different scenarios—to help guide practitioners as they make similar decisions in their daily practice.
Case Study #1: Low Refractive Cylinder (0.75D to 1D)
Patient A: spherical soft lens wearer; Patient B: spectacle lens wearer.
Practitioners worldwide have routinely bypassed the correction of low levels of refractive astigmatism (≥ 0.75D).1 In fact, the number of individuals who are fit into astigmatic-correcting lenses is approximately only half of those who could potentially benefit from such a lens.2-4 This is often the result of the perceived complexity, time, and expense of soft toric lenses.
These low refractive patients are often good candidates for soft toric lenses, especially if they have been wearing spherical soft lenses or even spectacles. Several studies in which low astigmatic patients were fit in both spherical and toric soft lenses found that toric lenses resulted in a significant improvement in vision.4,5
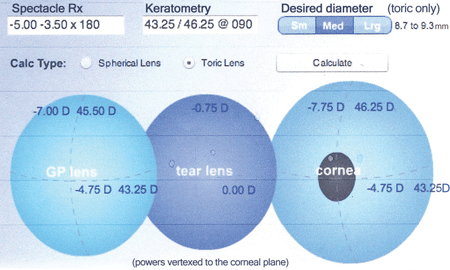
1. The GPLI Toric and Spherical Lens Calculator: Bitoric Design.
The best recommended method is to provide a “Coke-Pepsi” test: Allow your patient to try both modalities, or at least test their vision with and without astigmatic correction in the phoropter, before making the final decision.
Case Study #2: Significant Residual Cylinder
Patient A: -3.50, -1.00x180, 43/45; Patient B: -3.50, -2.25x180, 43/44.
Patients exhibiting ≥ 0.75D of residual astigmatism—i.e., not corrected with a spherical GP lens—often benefit from soft torics, especially if their refractive cylinder is in the customary range of standard designs (0.75D to 2.50D).6 In particular, silicone-hydrogel frequent replacement and disposable toric lenses are recommended; there are currently at least 12 such designs.7 These designs all meet the corneal oxygen requirements under open-eye conditions and also dehydrate at a slower rate than their hydrogel counterparts.8,9
Historically, front surface toric rigid GP lenses have been used in many of these cases; however, problems of decentration, vision instability and reduced comfort often occur. This is, in part, due to the greater thickness of these prism-ballasted lenses.
In the case of Patient B, a bitoric GP lens design is an alternative if a soft toric lens rotates excessively and results in unsatisfactory vision.
Case Study #3: Critical Vision Demands
Patient A: soft toric lens wearer; Patient B: new lens wearer.
Consider GP lenses for all individuals who have critical distance vision requirements. This is because GP lenses can mold the front surface of the eye, thereby eliminating anterior corneal astigmatism. They can also provide outstanding optical quality, which has resulted in better visual performance as compared to soft lenses.10-12
Initial comfort can be improved by a positive, proactive presentation, the use of a topical anesthetic immediately prior to initial lens application, and by ordering the lenses empirically so that the patient’s initial experience is visually encouraging.13,14
Secondary options include either a hybrid or a semi-scleral design; the latter has recently been found to result in wear and comfort comparable to soft torics, yet offers better subjective quality of vision.15
Case Study #4: Low Spherical Error/High Cylinder
Patient: -0.75, -2.75x180
These individuals often benefit from a bitoric GP lens design, particularly if their corneal cylinder is at least 2.50D.6 These designs are not complicated, plus there are several easy-to-use empirical guides and calculators available, such as the Mandell-Moore Guide, the GPLI Toric and Spherical Lens Calculator (figure 1) and Newman’s GP Toric Guide. All of these resources are available online at the GP Lens Institute (
www.gpli.info).
Empirical fitting of bitoric lenses has been found to be as successful as diagnostic fitting, and has resulted in greater patient satisfaction when compared to soft toric lenses.10,16 A recent study found that 14 out of 19, or 74% of high astigmatic subjects who wore both soft toric and back surface GP toric lenses preferred the vision of the GP lenses and preferred to stay in them, even though most of the subjects entered the study wearing soft toric lenses.10,11,14,19 The researchers concluded that GP toric lenses should be considered as an option for all high astigmatic patients as they are preferable in day-to-day critical vision activities, notably reading and computer use.
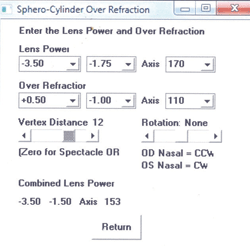
2. The AOA cross cylinder calculator recommendation based on a sphero-cylindrical over-refraction over a soft toric lens.
The biggest challenge presented with soft toric lenses is not only the high cylindrical component of the refraction, but also that the cylindrical component is predominant. For an individual with -3.00D of cylinder, 5˚ of rotation results in approximately 0.50D of over-refractive cylinder, and this increases approximately 0.50D for every additional 5˚ of rotation (i.e., -1.00D at 10˚, -2.00D at 20˚, etc.).17 This is also significant at lower cylinder levels, as 10˚ of rotation results in an over-refractive cylinder of 0.75D with a patient exhibiting -2.25D of refractive cylinder and 0.92D if they exhibit -2.75D of cylinder.18
Several calculators are available to assist in determining the soft toric cylinder amount and axis if a sphero-cylindrical over-refraction results from lens rotation on the eye (figure 2).19 Custom soft toric lenses are an option if GP lenses are not successful or desired. The fact that these lathe-cut designs can be manufactured in a 60Dk silicone-hydrogel material (e.g., Definitive from Contamac; available from Art Optical, ABB Concise, Metro Optics and Unilens) with up to 5.00D of cylinder correction and any axis is beneficial. The downside is that these lenses are more expensive than their hydrogel counterparts, and are only replaced quarterly.20
Case Study #5: Against-the-Rule Cylinder
Patient: 44.25/43 @ 090/-5.00 -1.50x090
Individuals exhibiting against-the-rule (ATR) astigmatism often benefit from a soft toric lens design. Upon blinking, GP lenses tend to follow the steeper corneal meridian on the eye; therefore, they tend to move laterally on an ATR cornea, which can result in fluctuating or blurry vision. Either one of the several newly introduced semi-scleral lens designs for healthy eyes or a hybrid design are recommended when a soft toric lens is not successful.
Case Study #6: Oblique Cylinder
 Patient A: refractive axis; Patient B: over-refraction with soft toric lenses
Patient A: refractive axis; Patient B: over-refraction with soft toric lenses
Individuals with oblique cylinder axes benefit visually from a GP lens design. Patients with healthy corneas who exhibit an oblique cylindrical correction or those with irregular astigmatism (i.e., keratoconus or post-surgical etiology) are both ideal candidates. The latter patients benefit from the ability of a GP lens to mold the front surface of the cornea into a sphere, which greatly reduces the irregularity and improves the quality of vision.
Also keep in mind that oblique axes incorporated into soft toric lens designs often result in rotation-induced reduced vision due to complex lid-lens interactions.21,22 If GP lenses are not successful, a second option is to fit the patient in either a hybrid or a semi-scleral design.
Case Study #7: Occasional Wear
Daily disposable toric lenses are the obvious option for astigmatic individuals who plan to wear their lenses only on occasion. Although the parameter range is limited and these lenses are not currently available as silicone hydrogels, they are a noteworthy alternative for the astigmatic athlete or individual with low refractive error who wears lenses only for critical distance vision tasks, such as night-time driving (see “How Do Daily Disposable Torics Impact Prescribing Habits?”).
Remember to avoid the temptation to prescribe the spherical equivalent power in a spherical daily disposable lens. It is also important to note that daily disposable lenses, along with GPs and daily wear soft lenses, have the lowest incidence of infection.24
Case Study #8: Young Progressive Myope
Patient A: low cylinder (1.00D); Patient B: high cylinder (2.00D)
Several recent studies have found that the design of overnight orthokeratology lenses is responsible for slowing down myopia progression and also exhibits a significant effect on axial length growth.25-28 This appears to be consistent with recent research that the peripheral retina plays an important role in myopia progression, and designs that do not result in peripheral retinal hyperopia appear to essentially serve as a “stop sign” for eye growth.29
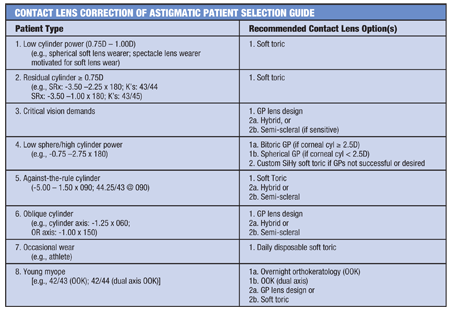 Spectacles, soft lenses and conventional GP lenses appear to exhibit little to no effect on myopia progression.25,26,30 In fact, some of these lens designs actually encourage myopia, particularly if they have increased minus power in the periphery of the lens.31
Spectacles, soft lenses and conventional GP lenses appear to exhibit little to no effect on myopia progression.25,26,30 In fact, some of these lens designs actually encourage myopia, particularly if they have increased minus power in the periphery of the lens.31
For higher astigmatic patients, the use of meridional differences in elevation (e.g., Paragon CRT Dual Axis, Paragon Vision Sciences) can result in reducing the astigmatism in the central treatment zone.32 Alternatively, spherical GP lenses or soft toric designs can be used with these patients to increase self-esteem and quality of life, relative to only spectacle wear.33
It is clear that we have many options when fitting even our astigmatic patients. Picking the right lens can help achieve the ideal patient vision and overall satisfaction. The good news is that both GP and soft lens options are readily available, are increasing in parameters and are an easy fit.
Dr. Bennett is currently assistant dean for Student Services and Alumni Relations at the University of Missouri-St. Louis College of Optometry. He is also executive director of the Gas Permeable Lens Institute, the educational division of the Contact Lens Manufacturers Association.
1. Efron N, Morgan PB, Helland M, et al. Soft toric contact lens prescribing in different countries. Cont Lens Anterior Eye. 2011 Feb;34(1):36-8.
2. Young G, Sulley A, Hunt C. Prevalence of astigmatism in relation to soft contact lens fitting. Eye Contact Lens. 2011 Jan;37(1):20-5.
3. Nichols JJ. Contact Lenses 2012. CL Spectrum. 2013 Jan. Available at:
www.clspectrum.com/articleviewer.aspx?articleID=107853. Accessed February 2013.
4. Dabkowski JA, Roach MP, Begley C. Soft toric versus spherical contact lenses in myopes with low astigmatism. Int Contact Lens Clin. 1992 Nov;19(11):252-6.
5. Richdale K, Berntsen DA, Mack CJ, et al. Visual acuity with spherical and toric soft lenses in low- to moderate- astigmatic eyes. Optom Vis Sci. 2007 Oct;84(10):969-75.
6. Bennett ES, Layfield KA, Lam D, et al. Correction of astigmatism. In: Bennett ES, Henry VA. Clinical Manual of Contact Lenses. 4th ed. Philadelphia: Lippincott Williams & Wilkins, 2009.
7. Thompson TT. Tyler’s Quarterly Soft Contact Lens Parameter Guide. 2012;30(1):11-5.
8. Brennan NA. Corneal oxygenation during toric contact lens wear. Poster presented at the American Academy of Optometry annual meeting, October 22, 2008; Anaheim, Calif.
9. Quinn TG. Soft toric advances and fitting trends. CL Spectrum. 2009;24(3). Available at:
www.clspectrum.com/articleviewer.aspx?articleid=102649. Accessed February 2013.
10. Michaud L, Barriault C, Dionne A, Karwatsky P. Empirical fitting of soft or rigid gas-permeable contact lenses for the correction of moderate to severe refractive astigmatism: a comparative study. Optometry. 2009 Jul;80(7):375-83.(15)
11. Fonn D, Gauthier CA, Pritchard N. Patient preferences and comparative ocular responses to rigid and soft lenses. Optom Vis Sci. 1995 Dec;72(12):857-63.
12. Johnson TJ, Schnider C. Clinical performance and patient preference for hydrogel versus RGP lenses. Int Contact Lens Clin. 1991 Jul-Aug;18(7-8):130-5.
13. Bennett ES, Stulc S, Bassi CJ, et al. Effect of patient personality profile and verbal presentation on successful rigid contact lens adaptation, satisfaction and compliance. Optom Vis Sci. 1998 Jul;75(7):500-5.
14. Bennett ES, Smythe J, Henry VA, et al. Effect of topical anesthetic use on initial patient satisfaction and overall success with rigid gas permeable contact lenses. Optom Vis Sci. 1998 Nov;75(11):800-5.
15. Michaud L, Woo S, Bennett ES, et al. Clinical evaluation of a large diameter rigid gas-permeable lens for the correction of refractive astigmatism. Paper presented at the Global Specialty Lens Symposium, January 24-27, 2013; Las Vegas.
16. Pitts K, Pack L, Edmondson W, et al. Putting a bitoric RGP lens fitting guide to the test. CL Spectrum. 2001;16(10):34-40.
17. Lindsay RG. Toric contact lens fitting. In: Phillips AJ, Spreewell L. Contact Lenses. 4th ed. London: Butterworth-Heinemann; 1997:255-70.
18. Jackson JM. Back to basics: Soft lenses for astigmatism. CL Spectrum. 2012 Jun;27(6):28-32. Available at:
www.clspectrum.com/articleviewer.aspx?articleID=107074. Accessed February 2013.
19. Jackson JM. A closer look at soft toric contact lens calculators. CL Spectrum. 2012 Mar;27(3). Available at:
www.clspectrum.com/articleviewer.aspx?articleID=106749. Accessed February 2013.
20. Brujic M, Miller J. Taking stock in your astigmatic options. Rev Cornea Contact Lenses. 2012 Apr;149(3):8-9.
21. Holden BA. The principles and practice of correcting astigmatism with soft contact lenses. Aust J Optom. 1975 Aug;58(8):279-99.
22. Gundel RE. Effect of cylinder axis on rotation for a double thin zone design toric hydrogel. Int Contact lens Clin. 1989 May;16(5):141-5.
23. Stapleton F, Keay L, Edwards K, et al. The incidence of contact lens-related microbial keratitis in Australia. Ophthalmol. 2008 Oct;115(10):1655-62.
24. Miller JR. Don’t forget daily disposables when fitting astigmats. CL Spectrum. 2011;26(8). Available at:
www.clspectrum.com/articleviewer.aspx?articleid=105914. Accessed February 2013.
25. Cho P, Cheung SW, Edwards M. The longitudinal orthokeratology research in children (LORIC) in Hong Kong: a pilot study on refractive changes and myopia control. Curr Eye Res. 2005 Jan;30(1):71-80.
26. Walline JJ, Jones LA, Sinnott LT. Corneal reshaping and myopia progression. Br J Ophthalmol. 2009 Sep;93(9):1181-5.
27. Hiraoka T, Kakita T, Okamoto F, et al. Long-term effect of overnight orthokeratology on axial length elongation in childhood myopia: a 5-year follow-up study. Invest Ophthalmol Vis Sci. 2012 Jun 22;53(7):3913-9.
28. Cho P, Cheung SW. Retardation of myopia in orthokeratology (ROMIO) study: a 2-year randomized clinical trial. Invest Ophthalmol Vis Sci. 2012 Oct 11;53(11):7077-85.
29. Smith EL, III, Kee CS, Ramamirtham R, et al. Peripheral vision can influence eye growth and refractive development in infant monkeys. Invest Ophthalmol Vis Sci. 2005 Nov;46(11):3965-72.
30. Walline JJ, Jones LA, Mutti DO, Zadnik K. A randomized trial of the effects of rigid contact lenses on myopia progression. Arch Ophthalmol. 2004 Dec;122(12):1760-6.
31. Holden BA. Myopia control update. Presented at the annual Global Specialty lens Symposium; January 24-27, 2013; Las Vegas.
32. Jackson JM. Advanced corneal reshaping for astigmatism. CL Spectrum. 2013;28(2). Available at:
www.clspectrum.com/articleviewer.aspx?articleID=107948. Accessed February 2013.
33. Walline JJ, Jones LA, Sinnott L, et al. Randomized trial of the effect of contact lens wear on self-perception in children. Optom Vis Sci. 2009 Mar;86(3):222-32.


