 |
Since treating corneal infections is the focus of this edition, it seemed like a good time to talk about the new antibiotics. Wait—there aren’t any to talk about! So, I guess this column will focus on the status of antibacterial agents by answering some questions surrounding this topic.
Can current antibacterial agents manage today’s infections?
Infectious diseases are still the third leading cause of deaths in the United States and the second leading cause of death worldwide.1 According to a 2013 report by the Centers for Disease Control and Prevention (CDC), more than two million people are infected with resistant strains annually, and more than 23,000 die from these infections.2 In 2013, The World Health Organization (WHO) issued a report on priority medicines, stating that the lack of effective antibiotics poses a significant threat to global health and will require the involvement of many different organizations to respond.3 Just a year later, the WHO issued its first global report on antibiotic resistance, further emphasizing that antimicrobial resistance is a serious threat that “is no longer a prediction for the future, it is happening right now in every region of the world and has the potential to affect anyone, of any age, in any country.”4
| Table 1. Antibiotics Approved in the United States, 1983–20115 | |
|
| Number of Antibiotics Approved |
| 1983-1987 | 16 |
| 1988-1992 | 14 |
| 1993-1997 | 10 |
| 1998-2002 | 7 |
| 2003-2007 | 5 |
| 2008-2011 | 2 |
Is there a shortage of new antibiotics?
Only four new classes of antibiotics have been introduced in the past 40 years.5 The US Food and Drug Administration (FDA) approved only two antibiotics in the past five years, which represents a drop off of 88% in approvals since the mid 1980s.6 Table 1 summarizes the approval of antibacterial agents in the United States over the past several decades.5
According to the WHO, antimicrobial resistance is one of the three greatest threats to human health.4 Of the drugs in the pipeline today, very few appear beneficial over existing drugs, and few appear to target the “ESKAPE” pathogens: Enterococcus faecium, Staphylococcus aureus, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa, and Enterobacter species. This acronym was so named after the organisms currently causing most of hospital infection in the United States and because they escape being managed by currently approved antibiotics.7
Many of the new drugs coming out lack a novel mechanism and are merely a new generation of an existing antibiotic—in other words, a follow-up drug.8 Therefore, even most drugs that have been developed recently are not significantly improved or better than what we already have.
Why is there a shortage of research and development?
Drug development is costly; pharmaceutical companies spend, on average, $5 billion in research, development and clinical trials for each drug they bring to market.6 Additionally, approximately 80% of drugs fail to make it through safety and efficacy studies.6 Therefore, each drug that makes it to market needs to be highly profitable to help recoup these extensive costs.
Economically, the return on investment (ROI) for antibiotics is poor for many reasons, including:
1. Antibiotics are typically taken for a short period of time, and they typically cure the disease. Pharmaceutical companies are far more attracted to the development of drugs that need to be taken for chronic conditions such as hypertension, hyperlidemia, etc.
2. The rapid development of drug resistance shortens the clinical lifespan.
3. New antibacterial drugs often have a short patent life.
All of these situations reduce the ROI for new drugs, making their development an unattractive financial venture.
Added to the financial concerns, developing an antibacterial drug is often more challenging than developing other classes of drugs. An antibacterial drug has to be effective against many pathogens, be able to treat a variety of infections and have effectivity at different sites within the body.9
There are also ethical concerns about clinical trials that compare the investigative drug to an existing drug. If there is a high level of resistance to the comparator drug, randomizing patients to receive that therapy is ethically questionable.10,11
While there is still a push for pharmaceutical companies to develop new antibiotics, at the same time there is a competing initiative to limit their use because of increasing resistance.8 These concerns ultimately highlight the underlying paradox of antibacterial drug research and development: as the antimicrobial resistance increases dramatically, there is a marked decline in the number of antibiotics in the development pipeline.
What is the status of the antibacterial pipeline?
As reported by the CDC in 2011, only five major pharmaceutical companies had active antibacterial discovery programs in place.12 In a 2009 European report entitled The Bacterial Challenge: Time to React, researchers found that only 15 antibiotics out of the 167 being developed had a new mechanism of action to potentially address the multidrug resistance challenge.12
Currently, there are 37 new antibiotics in the pipeline, and given that only roughly 60% of drugs that ever reach Phase 3 trials will receive FDA approval, the pipeline is not sufficient for the rising health care needs.13 Right now, 11 of the 37 drugs are in Phase 1 trials, 13 are in Phase 2 trials and 13 are in Phase 3 trials. Eleven are expected to have activity against ESKAPE pathogens and an additional four possibly may be effective.2
According to one study, in the last 40 years only two novel classes of antibiotics have been brought to market—and both were discovered before 1987.14 Today, the greatest threat is multi-drug resistant gram negative organisms. Unfortunately, most large pharmaceutical companies have closed (or greatly reduced) their antibacterial research units. Now, a large portion of research in this field is occurring in academia or in smaller biotech companies.14
As for the few drugs that are new, researchers evaluated the characteristics of the new antibiotics approved from 2010 to 2015. There were eight approved, with only one having a new mechanism of action. Half of the drugs were for the same condition—acute bacterial skin infections. Three of the eight showed activity against the ESKAPE pathogens. One drug demonstrated activity against Clostridium difficile, one of the CDC’s greatest-threat pathogens. None of the drugs studied demonstrated superior outcomes on patient survivability over what is currently available. At the very least, the data did show that the FDA is approving new antibiotics efficiently.15
| Bacteria: Up Close and Personal |
| These “ESKAPE” pathogens are not managed by currently approved antibiotics: |
 |
| Colonial growth pattern displayed by Providencia alcalifaciens bacteria, belonging to the family Enterobacteriaceae. Photo: CDC |
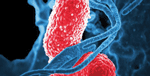 |
| A digitally-colorized SEM showing Klebsiella pneumoniae interacting with white blood cells (blue). Photo: David Dorward, PhD; NIAID |
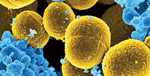 |
| Staphylococcus aureus escaping white blood cells. Photo: Frank DeLeo, NIAID |
 |
| Pseudomonas aeruginosa. Photo: Janice Haney Carr; CDC |
What is being done to address the problem?
Research suggests 20% to 50% of antibiotics prescribed in United States acute care hospitals are not needed or not appropriate.16 In 2014, the CDC recommended that all acute care hospitals implement Antibiotic Stewardship programs. These stewardship programs promote judicious use of antibacterial agents, increase the correct prescribing and prophylaxis use of antimicrobials and overall improve patient safety.16
The increase in resistance to the antimicrobials available to practitioners has led to numerous initiatives, these stewardship programs among them. But this alone cannot fix the problem; researchers need to develop new drugs.5 To address the barriers to developing antibiotic drugs, several efforts are underway, including: public-private partnerships (PPP), modified regulatory processes, outside-the-box reimbursement plans, and an increase in government investment.11
In 2012, President Obama signed the Generating Antibiotic Incentives Now (GAIN) Act into law. This legislation extends the market exclusivity of certain antibiotics that treat serious or life-threatening diseases. It also grants those drugs priority review status so they can undergo an expedited FDA approval process. Under the GAIN act, the FDA must maintain a list of pathogens that have the potential to pose a significant public health risk and update it every five years. The FDA must also provide clinical trial guidance on the development of drugs that target specific bacteria.17
Eight drugs have been approved since the initiative launched—but not in areas of greatest need such as treatment for C. diff. and drug-resistant Neisseria gonorrhoeae.13
Of the 37 antibiotics currently in development, roughly 24 are qualified infectious disease products (QIDPs). All drugs approved since 2014 have been QIDP.13
There are several other legislative proposals in play that will help with the drug approval process. For example, the Antibiotic Development to Advance Patient Treatment (ADAPT) Act has been referred to the US House of Representatives, which, if passed, will speed up the FDA approval process for antibiotics, antifungals or biological products for the treatment of a serious infection.13
At the 69th World Health Assembly this past May, the WHO announced the formation of a public-private partnership, the Global Antibiotic Research and Development (GARD) Partnership.18 It was created by the Drugs for Neglected Diseases Initiative, in conjunction with WHO, to develop new antibiotics to meet the challenges of resistance and to promote conservation but equitable access. GARD is now in the start-up phase and is receiving seed money from various organizations throughout Europe. Hopefully, such a partnership will allow the development of products that the pharmaceutical industry may pass on due to lack of profitability.18
In 2010 the Infectious Diseases Society of America launched the Bad Bugs No Drugs – 10 x ’20 initiative, which aimed to have 10 new systemic antibacterial drugs developed by 2020.7 An interim report on the 10 x ’20 initiative suggests there is progress, but the pace of research and development needs to speed up if it is going to reach its goal by 2020.19
In 2009 a transatlantic task force was created to focus on bolstering the antibacterial pipeline, strengthening infection control interventions and promoting antimicrobial stewardship in human and veterinary settings.6
With so much global attention on this antibacterial shortage, hopefully these unified efforts will garner a sufficient stockpile of antibacterial agents to manage the serious infections of today and tomorrow.
1. Conly JM, Johnston BL. Where are all the new antibiotics? The new antibiotic paradox. Can J Infect Dis Med Microbiol. 2005 May;16(3):159-60.
2. Centers for Disease Control and Prevention. Antibiotic Resistance Threats in the United States, 2013. Available at www.cdc.gov/drugresistance/threat-report-2013/. Accessed August 23, 2016.
3. Kaplan W, Wirtz VJ, Mantel-Teeuwisse A, et al. Priority Medicines for Europe and the World, 2013 Update. The World Health Organization. July 9, 2013. Available at www.who.int/medicines/areas/priority_medicines/MasterDocJune28_FINAL_Web.pdf. Accessed August 23, 2016.
4. The World Health Organization. WHO’s first global report on antibiotic resistance reveals serious, worldwide threat to public health. News Release. April 30, 2014. Available at www.who.int/mediacentre/news/releases/2014/amr-report/en/. Accessed August 23, 2016.
5.Cooper MA, Shlaes D. Fix the antibiotic pipeline. Nature. 2011 Apr;472(7341):32.
6. Krans B. Few New Drugs: Why the Antibiotic Pipeline Is Running Dry. Healthline.com. 2014 July. Available at www.healthline.com/health/antibiotics/why-pipeline-running-dry. Accessed August 23, 2016.
7. Infectious Diseases Society of America. The 10 x ‘20 Initiative: pursuing a global commitment to develop 10 new antibacterial drugs by 2020. Clin Infect Dis. 2010 Apr 15;50(8):1081-3.
8. Sukkar E. Why are there so few antibiotics in the research and development pipeline? The Pharmaceutical Journal. 2013 Nov;13.
9. Piddock L. The crisis of no new antibiotics--what is the way forward? Lancet Infectious Diseases. 2012 Mar;12(3):249-53.
10. DiNubile MJ. Noninferior antibiotics: when is “not bad” “good enough”? Open Forum Infect Dis. 2016 May 25;3(3):ofw110.
11. McDonnell A, Rex JH, Goossens H. et al. Efficient delivery of investigational antibacterial agents via sustainable clinical trial networks. Clin Infect Dis. 2016 Aug 15;63 Suppl 2:S57-9.
12. Race against time to develop new antibiotics. Bulletin of the World Health Organization. 2011;89:88–9.
13. Drug development critical to combating antibiotic resistance. Healio Infectious Disease News. 2015 June. Available at www.healio.com/infectious-diseases. Accessed August 10, 2016.
14. Zorzet A. Overcoming scientific and structural bottlenecks in antibacterial discovery and development. Ups J Med Sci. 2014 May;119(2):170-5.
15. Deak D, Outterson K, Powers JH, Kesselheim AS. Progress in the fight against multidrug-resistant bacteria? A review of U.S. Food and Drug Administration-approved antibiotics, 2010-2015. Ann Intern Med. 2016 May 31. doi: 10.7326/M16-0291.
16. Centers for Disease Control and Prevention. Core Elements of Hospital Antibiotic Stewardship Programs. Available at www.cdc.gov/getsmart/healthcare/implementation/core-elements.html. Accessed August 11, 2016.
17. GAIN: How a New Law is Stimulating the Development of Antibiotics. The Pew Charitable Trusts Issue Brief. November 07, 2013. Available at www.pewtrusts.org/en/research-and-analysis/issue-briefs/2013/11/07/gain-how-a-new-law-is-stimulating-the-development-of-antibiotics. Accessed August 25, 2016.
18. Drugs for Neglected Diseases Initiative. Global Antibiotic Research & Development (Gard) Partnership. Available at www.Dndi.org/diseases-project. Accessed August 10, 2016.
19. Boucher HW, Talbot GH, Benjamin DK, et al. 10 x ‘20 Progress--development of new drugs active against gram-negative bacilli: an update from the Infectious Diseases Society of America. Clin Infect Dis. 2013 Jun;56(12):1685-94.


