The concept of a protective eye bandage originated in the first century A.D., when Celsus reportedly applied a honey-soaked linen to the site of a pterygium removal to prevent symblepharon development.1,2 Bandage soft contact lenses were first used in the 1970s following the development of hydroxyethyl methacrylate (HEMA) by Otto Wichterle.2 With the recent advances in material technology, today’s bandage contact lenses provide the same benefits as their predecessors—but with enhanced convenience, improved healing and increased corneal health.
 Bandage Lens Basics
Bandage Lens Basics
By definition, a bandage contact lens protects the cornea. Many different lens types can be utilized to accomplish this goal (see tables 1 and 2); however, because of their high oxygen permeability and FDA approval for extended wear, silicone hydrogel soft contact lenses are currently most practitioners’ first choice.
Bandage lenses protect the cornea not only from potential exterior sources of injury, but also from a patient’s own eyelids. The shearing effect created by the lids during the blink can inhibit re-epithelialization and cause pain. Use of a bandage lens facilitates corneal healing in a pain-free environment.
Depending on the patient’s ocular condition, he or she may wear their therapeutic lenses for a period of days to years. They may be utilized for daily or extended wear (see table 2). Because there is generally an underlying disease process precipitating the need for a therapeutic lens, extra caution must be taken to clean and disinfect the lens after wear, keeping in mind that silicone hydrogel lenses tend to deposit lipids more readily than HEMA lenses (see image 1). That said, the addition of a digital rubbing step is necessary for lenses that are used more than once.
It is critical to perform frequent follow-ups for bandage contact lens patients. One reason is that a bandage lens fit, by design, demonstrates less movement than a traditional soft lens fit. The theory is to provide increased patient comfort while preventing the healing epithelial cells from sloughing off due to any mechanical trauma of the lens itself.3 In addition, it is important for the practitioner to be vigilant regarding the detection of signs of microbial keratitis. The compromised cornea—especially when wearing lenses in an extended wear modality—is at particular risk for infection.4
 Indications
Indications
Bandage contact lenses are indicated for many different reasons, including: protecting the eyes, increasing comfort, facilitating healing and sealing wound leaks. We’ll explore these indications, and others, in more detail in the following paragraphs.
• Protection. Corneal protection is needed in the case of several conditions, including: entropion, trichiasis, tarsal scars, recurrent corneal erosion, post-surgical ptosis and surgical sutures or exposed suture knots.
Recurrent erosions are a typical sequella of epithelial basement membrane (basal lamina) trauma or are secondary to anterior basement membrane dystrophy, anterior basement membrane degeneration or stromal dystrophy. A bandage contact lens is the second line of treatment, after hyperosmotic drops and/or ointment fail.2,5 An added benefit is the enhanced vision provided by the smooth refracting surface of the contact lens, as opposed to an irregular anterior corneal surface.5 Hypertonic saline drops should continue to be utilized concurrently with the lenses.
• Pain relief. The mitigation of corneal pain is another important indication for therapeutic contact lenses. The conditions most in need of this therapy include bullous keratopathy; epithelial erosion and abrasion; filamentary keratitis; and postoperative penetrating keratoplasty.
In bullous keratopathy, endothelial failure results in corneal edema, which in turn creates epithelial blisters that rupture, causing pain, foreign body sensation, and photophobia. A bandage contact lens reinforces the damaged tissues and protects the nerve endings from the abrasive actions of the eyelids. Patients who are awaiting a conjunctival flap or cornea transplant may be fitted with therapeutic lenses for up to 30 days at a time.2
Until recently, pressure patching was the standard of care for treating large epithelial abrasions (see figure 2). With this treatment, the caveat was to refrain from patching contact lens wearers or injuries caused by presumed vegetative matter or false fingernails. The utilization of a bandage contact lens provides protection and healing for all three of these conditions, and it has now supplanted patching as the standard of care. The authors of the Wills Eye Manual caution, however, that prophylactic topical antibiotics should be used concurrently and that daily follow-up care is mandatory.6
The other advantage of bandage contact lenses over patching is the ability to continue to install topical ophthalmic medications. This is particularly important after a corneal abrasion, erosion, or corneal refractive surgery, which necessitate the frequent installation of antibiotics and/or artificial tears. Some reports caution against the installation of cycloplegic agents (which reduce the pain associated with a corneal abrasion/erosion or after corneal refractive surgery) in bandage CL wearers. The dilating drops can cause the bandage lenses to dry out and become less comfortable, especially overnight, with the end result a potentially decreased healing response.7 On the other hand, bandage contact lenses can be utilized—by design—as vehicles for drug delivery, but the exact way to ensure a consistent dosage is still under investigation.
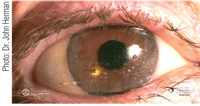
1. Therapeutic soft contact lens with 2+ surface coating.
• Healing. The use of bandage contact lenses to facilitate healing is particularly necessary for the following conditions: chronic epithelial defects, corneal ulcer, neurotrophic keratitis, neuroparalytic keratitis, chemical burns and basement membrane disease.
They also enhance healing following corneal surgery, particularly refractive surgery. They protect the cornea from exposure or from the irritation caused by rubbing the eye as the corneal wounds are healing. Therapeutic bandage contact lenses are a mainstay after photorefractive keratectomy (PRK) procedures, in which the removal of the epithelium leaves an open wound that takes about one week to heal (see figure 3). They are also valuable for the following procedures: laser-assisted in situ keratomileusis (LASIK), laser-assisted subepithelial keratomileusis (LASEK), Epi-LASIK, penetrating keratoplasty (PK) and phototherapeutic keratectomy (PTK), lamellar grafts and corneal flaps.
• Sealing. The lenses also may aid in sealing leaky wounds. Serving as a splint or sealant, the lenses can be beneficial after cataract, penetrating keratoplasty or glaucoma filtering surgery.

2. The use of therapeutic contact lenses has replaced pressure patching as the standard of care for epithelial abrasions such as the one in the image above.
• Maintenance of corneal hydration. The role of bandage contact lenses in dry eye is controversial. For patients who need to continually instill lubricating drops into their eyes, particularly after refractive surgery, the benefits of using a bandage lens can be great. Other patients who benefit are those who have significant lagophthalmos and subsequent corneal exposure. However, contact lenses are generally contraindicated for dry eye.7
• Structural stability and protection in piggyback lens fitting. Many patients benefit from the utilization of a soft and rigid lens concurrently. The rigid lens provides crisp vision, particularly for irregular corneas, and the soft bandage lens protects the cornea, preventing irritation and abrasions. Examples include elevation differences in the host/graft junction, keratoconus and in the presence of scar tissue.
Contraindications
Each clinician must assess his patient’s condition carefully to determine whether a bandage contact lens is warranted. Interestingly, many of the conditions that require bandage contact lenses (dry eye, infection, inflammation, etc.) contraindicate lens wear in general. In addition, therapeutic contact lenses should not be used in patients who are unwilling or unable to comply with the necessary treatment and follow-up.

3. The cornea, one day following PRK.
Dr. Gromacki is a diplomate in the Cornea, Contact Lens and Refractive Technologies Section of the American Academy of Optometry. She is Chief Research Optometrist at Keller Army Community Hospital, West Point, New York.
1. Arrington GE. A history of ophthalmology. MD Publishers, New York, New York, 1959.
2. Weiner BM. Therapeutic bandage lenses. In: Silbert JA, ed. Anterior Segment Complications of Contact Lens Wear. Churchill Livingstone, New York, New York, 1994; 455-471.
3. Aquavella JV. Chronic corneal edema. Am J Ophthalmol 1973;(76):201-207.
4. Thoft RA, Mobilia EF. Complications with therapeutic extended wear soft contact lenses. Int Ophthalmol Clin. 1981;(21):197.
5. Chan WE, Weissman BA. Therapeutic contact lenses. In: Bennett ES, Weismann BA, (eds). Clinical Contact Lens Practice, Lippincott Williams & Wilkins: New York, New York, 2005: 619-628.
6. Ehlers JP and Shah CP, eds. The Wills Eye Manual Fifth Edition, Wolters Kluwer Health, New York, New York, 2008:15-16.
7. Russell GE. Bandage lenses: new opportunities in practice. Contact Lens Spectrum. 2004(6).
8. Tyler Thompson TT. Tyler’s Quarterly 2011;28(3):32-52.
9. White P. 2011 Contact Lenses and Solutions Summary. In: Contact Lens Spectrum (suppl) 2011;27(7):14.


