Rigid contact lens polishing units are still commonly found in contact lens practices (figure 1). Yet, they are headed toward obsolescence. It is not because the rigid lens modality is dying. Prescribing rigid lenses is still important, especially in a practice like mine with many keratoconus and other irregular cornea patients. Instead, changes in our industry are making the disadvantages of rigid lens polishing apparent.
In-office polishing is rooted in the good intentions of reducing accumulated surface deposits to extend the life of the rigid lens, sort of like refinishing wood flooring to give it life anew. This deep cleaning is designed to remove deposits more effectively than digitally rubbing with an abrasive cleaner. But lens polishing has a dark side.
Concern for the Optics
First, with the newer “no-polish” computer numerical controlled (CNC) lathes, like the Optoform 80 (Ametek, Inc.), rigid lenses are generated with such high accuracy and precision that polishing can harm their optics. For example, interferometry shows how polishing a rigid lens can induce aberrations (figure 2). I even once observed a center-add rigid bifocal lens have the add segment accidentally polished off, causing the patient loss of near vision.

1. Rigid lens polishing unit.
Even though it may seem like polishing is helping the patient by removing deposits, it may actually work against your goal of offering the best quality of vision. While a new lens is often the best treatment, an alternative to polishing is using Progent (Menicon), a protein remover that uses sodium hypochlorite and potassium bromide to chemically clean the lenses.
Watch for Plasma Treatment
Second, more rigid lenses today have plasma treatment. Plasma treatment is intended to reduce deposits from accumulating, reduce bacterial adhesion and increase lens wetting. Abrasive cleaners such as Boston Original and Boston Advance (Bausch + Lomb) can remove the plasma treatment. Instead, use non-abrasive cleaners such as Boston Simplus (Bausch + Lomb), Opti-Free GP (Alcon) or Optimum (Lobob).
Lens polishing can also remove plasma treatment. To illustrate this effect, I had five identically lathed rigid lenses (HDS 100 material, Paragon Vision Sciences) with the contact angle measured before and after plasma treatment. After having the lenses plasma treated at SynergEyes, Inc., the contact angle was measured. Then after polishing, the contact angle was measured again (see “Contact angle before plasma treatment, after plasma treatment and after polishing”).

2. Interferometry of a rigid lens before polishing (left) and after polishing (right). Note the polish-induced aberrations.
I found that plasma treatment dramatically improved lens wetting; subsequent polishing returned the lenses to their wettability state prior to plasma treatment. Indiscriminate lens polishing on plasma-treated rigid lenses negates the benefits of plasma treatment.
Perils of Lens Polishing
Third, lens polishing is inefficient. Many ancillary personnel confide that they are uncomfortable polishing lenses, even those supposedly trained to do it. There is the fear of breaking the lens, having the lens spin off or losing the lens down the drain.
All too often, the doctor ends up polishing the lenses. But, the doctor is not always available when the patient comes in asking to have their lenses polished. This can disrupt the schedule and cause delays, especially if the patient has no back-up contact lenses or eyewear.
Also, keep in mind that most practices do not charge enough to cover the doctor’s time for lens polishing. In most cases, the doctor operates more productively and efficiently examining patients. Pulling the doctor away from direct patient care toward lens polishing is not and should not be the doctor’s core competency. Therefore, a patient coming in to have their lenses polished creates an unnecessary operation, which is often unpredictable in timing and can throw a wrench into busy practice operations.

3. Wettability of rigid lens with plasma treatment before polishing (left) and after polishing (right).
Replacement Schedules
Finally, polishing lenses can decrease the frequency of purchasing new lenses if patients mistakenly believe that polishing makes the lenses perform like new. Reduced practice profitability limits your ability to reinvest in new technology, and sustain or even grow practice operations, and can threaten your ability to give employees cost-of-living adjustments to their compensation.
In this fragile economy, where there is still widespread consumer appeal to save money, take the time to educate your patients that insist on lens polishing. Explain to them that that polishing today’s advanced rigid lenses can compromise optical quality, lens wettability and their overall wearing experience.
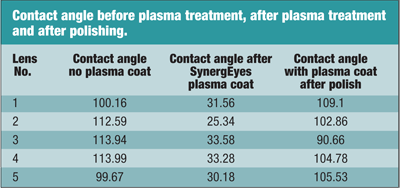
All lenses were made with the following parameters: 7.80 BC, -3.00 D, 9.2 Diam, 0.120 CT.
Dr. Chou is in private practice at EyeLux Optometry in San Diego and is the co-developer of EyeDock.com, an online clinical reference guide for contact lens practitioners. He graciously acknowledges William Meyers, Ph.D., vice president of Science & Technology at Paragon Vision Sciences, for providing the test lenses, and Ramazan Benrashid, Ph.D., vice president of R&D of SynergEyes, for providing plasma treatment, measuring wetting angle, and interferometry of the lenses for this article.


